Preparation Design and Armamentarium for Lithium Disilicate Restorations
Providing this restorative solution requires some adjustment in clinical technique as well as the burs used to achieve the correct margin design and reduction
Lee Ann Brady, DMD
Not only have all-ceramic indirect restorations become the mainstay of my clinical practice, 95% of my posterior restorations are made from lithium disilicate (IPS e.max® CAD/Press, Ivoclar Vivadent). I have found IPS e.max to be an incredibly versatile material, providing superior strength, fracture resistance, and esthetics. It can be used in both posterior and anterior situations and for full and partial coverage. In addition, this material can be bonded or cemented depending on the clinical circumstance.
When I made the decision to provide these restorative solutions for my patients, I had to incorporate new clinical techniques and a new armamentarium. A key area that I had to change was my preparation design and the burs that I used to achieve the correct margin design and the reduction necessary for long-term success.
Today, my practice uses procedure-based bur blocks, which has been one way that we stay efficient; for any given clinical procedure, I know which burs I need. Being equipped with a specific kit that provides me with all of the tools that I need for success saves time and staves off frustration. In my operatory, I have bur blocks always ready. My goal is to place the first bur to be used in the procedure into the handpiece, deploy it on the teeth that I will be preparing, and then move to the next bur. If a bur can be cleaned, sterilized, and reused, I will return it to my tray table. If the bur must be discarded, I will place it on my assistant’s tray table. This ensures that dull burs are not cleaned and sterilized, simply to be discovered during the next preparation.
Ready for Any Indirect Preparation
The new IPS e.max® Restorative Preparation System (Figure 1), featuring Durabraze Diamonds, is equipped with all the burs needed for any indirect preparation for IPS e.max. Durabraze diamonds are uniquely manufactured to eliminate debris accumulation, increase cutting efficiency, and extend the lifetime of the diamond.
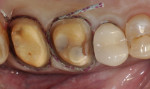
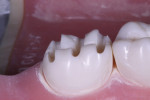
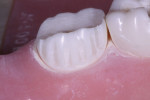
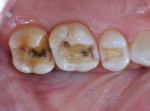
Posterior full-coverage restorations should be prepared with a modified shoulder (rounded internal line angle) margin design, a 1.5-mm occlusal reduction at the very minimum, and 1-mm axial wall reduction at the margin, with a 1.5-mm reduction in the middle and occlusal thirds of the axial walls (Figure 2). I use the WDL1.5 to create depth cuts through all of the occlusal anatomy and over the cusps (Figure 3). The coarse-grit 016 modified shoulder Peter Brasseler diamond (845KR) is then used to reduce the occlusal table of the tooth to the extent of the depth cuts. This same diamond is used on the buccal and lingual walls to create depth cuts for axial wall reduction, the gingival margin, and preparation of the interproximal surfaces (Figure 4). Occlusal reduction should be verified visually, with a reduction guide or bite-registration silicone before the preparation is completed. The entire preparation is polished, and all line angles are rounded using the fine-grit 016 modified shoulder diamond (BR8847KR). A polished surface of a prepared tooth improves the accuracy of both traditional and digital impressions, leading to a final restoration with a more precise fit and longevity.
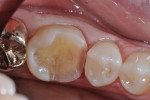
Posterior onlays follow similar preparation design principles as crowns, and the same burs can be used (Figure 5 and Figure 6). In cases in which the dentist is preparing a tooth with a short clinical crown or the patient has a limited opening, the 845KR 016 diamond can be used to create a modified shoulder margin and adequate reduction. Any cusp that is covered should have a minimum of 1.5-mm occlusal reduction. The axial walls should be reduced 1 mm at the gingival margin and 1.5 mm in the middle and occlusal thirds, including the gingival floor of an interproximal box. When no cuspal coverage is indicated and an inlay is prepared, the dentist should pay close attention to the preparation in the isthmus, which must have widths of 1 mm to 1.5 mm and a depth of at least 1 mm. The WDL1.0 is used to create adequate depth cuts through the occlusal grooves. The gingival box is prepared with a modified shoulder margin and a minimum of 1-mm axial reduction at the floor of the box. As with any all-ceramic preparations, all internal line angles should be rounded and smoothed.
The Brasseler IPS e.max bur system is perfectly designed for anterior preparations, including the uniquely designed RWEXT, RWCONV, and RWMIN labial depth cutters. Anterior full-coverage IPS e.max crowns are designed with a minimum of 1.5-mm incisal edge reduction and 1.2-mm facial minimum facial reduction with 1-mm reduction at the gingival margin (Figure 7). I use my RWDL1.5 first to place depth cuts through the incisal edge (Figure 8). I will then switch to the RWEXT depth cutter and place the incisal and middle third depth cuts by lining the shank of the diamond parallel with the incisal plane of the tooth. I then place the RWEXT parallel to the gingival third of the tooth to place the gingival depth cut. The cutting end of this unique bur can also be used to place a deep chamfer margin based on the dentist’s preference. Creating adequate lingual reduction in anterior crown preparations is challenging due to the shape of the tooth (Figure 9). The RWDL1.0 can be easily used to place 1-mm depth cuts into the lingual anatomy to ensure adequate thickness of the ceramic. I complete my facial and interproximal gross reduction with the BR6847KR diamond and the lingual reduction with a football-shaped BR6379.023. The entire preparation is rounded, refined, and polished with the BR8847KR.
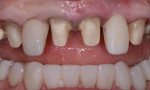
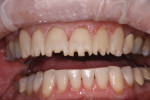
The final indirect preparation is for an anterior IPS e.max veneer (Figure 10). Anterior veneers are one of the most unique and variable tooth preparations. The preparation design for an anterior veneer is dependent on the final esthetic outcome, the color of the tooth being veneered, and the structural condition of the tooth. The facial reduction can vary from 0.3 mm at the gingival margin to 0.8 mm. Keeping the facial reduction small maximizes the amount of enamel to which the restoration will be bonded, but limits the degree of color and esthetic changes of the restoration. Conversely, the deeper the facial preparation, the greater the esthetic change the restoration can accomplish but the more dependent retention becomes on dentin adhesion. Anterior veneers can remain entirely on the facial and leave the interproximal contacts in natural tooth structure, or wrap the ceramic into the interproximal and around to the lingual line angle (Figure 11). Breaking the contacts will depend on the presence of interproximal caries, any prior Class III restorations, and a desire to extend the ceramic into the interproximal to close black triangles or alter the contour of the tooth. Interproximal preparation design can leave a wall of enamel at the lingual side of the contact or curve around to the lingual line angle in a slice preparation.
Lastly, anterior veneers can cap the incisal edge of the tooth or simply be the facial half of the incisal edge. This decision is again dictated by the expected clinical outcomes. Often, dentists are lengthening the tooth or changing the final incisal edge position with the veneer and will require ceramic at the incisal edge. Capping the incisal edge provides the ceramist with greater freedom in design of the esthetic characteristics such as incisal translucency and the appearance of dentin lobes. If dentists are maintaining incisal-edge length and position and like the incisal-edge esthetics preoperatively, they can simply place ceramic to the incisal edge and not cap it.
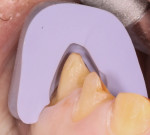
Typically, when I am preparing anterior teeth, the restorations are being used to change tooth position, tooth shape, or incisal-edge position. In these situations to ensure adequate room for the ceramic but to minimize the reduction of the natural tooth structure, the teeth are prepared from a mock-up. Preoperative models are sent to a laboratory, and a wax-up is created. A silicone matrix of the wax-up is used to create a mock-up. The teeth are spot-etched prior to preparation, and the matrix is loaded with bis-acryl provisional material and seated over the unprepared teeth. Once the bis-acryl has come to a full set, the matrix is removed, and flash beyond the free gingival margins is peeled away with a plastic instrument. Depth cuts and tooth preparation are then done using the bis-acryl mock-up.
As with a full-coverage crown, I use the RWDL1.5 to place incisal depth cuts. I perform facial depth cuts with the RWMIN, RWCONV, or RWEXT depending on the amount of facial reduction I need. Unlike crowns, veneers do not draw down the incisal edge of the tooth, but roll from the incisal/facial to the gingival/facial. I suggest that clinicians should use RW depth cutters in three facial planes—incisal, middle, and gingival—to preserve the natural enamel by following the facial curvature of the tooth.
The final removal of incisal, facial, and interproximal tooth structure is accomplished with either the 012 modified shoulder diamond or the 016, depending on the total reduction needed. The plane of the incisal reduction should follow that of the final incisal edge. To ensure gingival-embrasure esthetic results, the gingival margin on the distal and mesial should be placed more lingually than the margin at the incisal of the tooth. As with other preparations, the fine-grit diamond can then be used to round the line angles and refine and polish the prepared surfaces. Leaving a remnant of the facial depth cuts is common when preparing conservative veneers. To avoid this and ensure the accuracy of my polishing and refinement step, I use the fine diamonds in a torque reduction friction grip attachment at slow speed (20,000 rpm) so I can clearly see the surface of the preparation.
Conclusion
Taking a methodical approach and using a bur block system that includes the entire preparation armamentarium helps to ensure perfect preparations every time, with maximum efficiency. Preparation and seating appointments will be smooth, quick, and full of satisfaction for both the dentist and the patient.
Disclosure
Lee Ann Brady, DMD, has no conflicts of interest to disclose relative to this article.
About the Author
Lee Ann Brady, DMD
Private Practice
Glendale, Arizona