In-Office Whitening Treatment
An evidence-based protocol with a contemporary LED whitening lamp
The term power bleaching, or professional in-office bleaching, describes the chairside treatment of discolored dentition with high-concentration oxidizing agents by the dental professional. A variety of techniques, devices, and material choices have been used in dentistry for treating discoloration with various levels of successes. Some situations are better suited for extended treatment outside the dental office with lower concentrations of peroxide delivered in custom trays, while the presentation of a severely discolored non-vital tooth may best be treated using a classic “walking bleach” technique. This article will primarily focus on the in-office technique using a contemporary whitening lamp for achieving immediate results on multiple vital teeth.
Treatment Planning Clinical and Radiographic Examinations
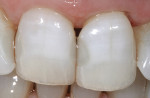
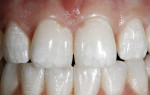
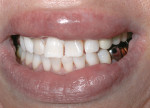
As with all dental bleaching, a comprehensive oral examination should be performed before power bleaching. Thorough clinical and radiographic examinations of the hard and soft tissues should be performed to rule out the presence of any oral pathologies or dental diseases and to determine the etiology of the stain. The clinician should make special note of any existing dental restorations, formulating a plan with the patient to replace any restorations due to post-bleaching color mismatch (Figure 1). In addition, the dentist should note with the patient any clinical white spot lesions, which may appear accentuated immediately after bleaching (Figure 2). A history of tooth sensitivity should be discussed by asking the patient if the teeth are generally sensitive to thermal changes, such as when the patient drinks hot or cold beverages.
Setting Expectations
As part of the initial patient interview, the advantages and disadvantages of in-office professional bleaching should be discussed relative to at-home bleaching and expected outcomes. By far, the most appealing advantage for most is the prospect of “instant” results. The total time savings is material and tooth dependent. Clinical studies have shown 7 days of at-home bleaching with 10% carbamide peroxide equals 45 minutes with 38% hydrogen peroxide,1 or a 1-hour treatment with 28% hydrogen peroxide using supplemental light.2 A more recent study compared peroxide-based whitening with a 10-day, 2-hours-per-day take-home whitening system to an immediate in-office light-enhanced whitening treatment. Efficacy was measured objectively as L*a*b* color change using digital images at baseline and day 11. The study concluded that daily use of take-home whitening system resulted in equivalent tooth whitening to a professional 1-hour LED light-assisted whitening treatment.3 Patients should understand that results may vary.
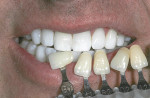
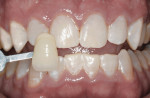
Some patients have unrealistic expectations based on a distorted perception of his or her existing tooth color. One caveat is the patient who over-bleaches. A patient who presents with extremely white teeth from repeated bleaching may falsely believe his or her teeth appear yellow. These patients may have an obsession or addiction to whitening, colloquially known as bleachorexia, and should be advised against further bleaching. Education may help by showing the patient his or her extremely white teeth next to the B1 tab from the VITA Classical Shade Guide (Vident, https://vident.com), for example (Figure 3).
The Whitening Lamp
The use of light to supplement the bleaching process in dentistry has been reported as early as 1918.4 Not until recently has the use of bleaching lights become widespread.
Several light sources with different spectral distributions and efficiencies all purport to accelerate or enhance the bleaching process. Tooth whitening lamps that result in heat activation of the bleaching agent may lead to elevated pulpal temperatures and increased tooth sensitivity.5 Current bleaching lamps may incorporate optimum blue light LEDs designed with a near-monochromatic light energy source. Using a current bleach lamp, researchers have demonstrated the complex interactions of hydrogen peroxide and stain molecules, which involve factors such as the bleaching agent’s pH, the presence of chemical activators, and specific-spectrum blue light intensity.6 Because LEDs produce a discrete or narrow spectrum of light, they require no additional filtration of extraneous energy and produce very little heat. As a result, an LED bleaching-light system is less dependent on heat but more on the wavelength specific photochemistry of the bleaching formula and possible energy absorption of the stain molecules to accomplish tooth whitening.
In-Office Vital Teeth Technique
Precautionary Statements/Management of Adverse Effects
No Anesthesia/Patient Monitoring. Anesthesia should not be used with this procedure. The doctor is monitoring for sensitivity at all times. The patient can be instructed to raise a hand to signal if any burning, tingling, or discomfort is experienced. The procedure may need to be abandoned if patient sensitivity cannot be overcome.
Sensitivity. Proper screening of the patient during the initial interview and dental examination can minimize this risk. Some risk factors for tooth sensitivity include existing decay, gingival recession, cervical abrasions, or a history of tooth sensitivity. Greater tooth sensitivity has been reported for in-office bleaching with a high-intensity halogen light compared to no light.7 Patients reporting a history of tooth sensitivity may pre-brush for 2 weeks with a potassium nitrate–containing toothpaste to alleviate or minimize discomfort.8 The patient identified as high risk for sensitivity may be provided with 600 mg of ibuprofen 30 minutes prior to treatment to reduce the incidence of tooth sensitivity.9 This may allow the patients to complete the procedure with minimal discomfort and obtain the most benefit from the appointment. Another strategy may be to provide a 3% to 6% potassium nitrate gel to the lingual surface of the teeth if the patient experiences sensitivity during the appointment.
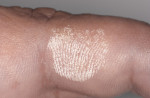
Tissue Burn or Swollen Lip. The ideal method to avoid chemical burn is through meticulous application of the gingival barrier. If the bleach penetrates beneath the barrier or accidental soft tissue contact is made, immediately flush the site with copious water spray and apply mineral oil, such as vitamin E. The oil should provide relief from the stinging sensation within minutes and the white oxidation typically resolves within a few hours (Figure 4). The patient may be provided with additional oil or topical anesthetic for home use. The need for antihistamine administration should be considered for allergic skin reactions.
White Spots. Any white spot lesions or striations should be identified prior to the appointment if possible because they may become accentuated during the bleaching process (Figure 2). As the teeth begin to rehydrate in the next 24 hours, these white spots may blend, or subsequent microabrasion techniques may be planned. If the blemishes are suspected to be recent lesions, successful treatment has been demonstrated using fluoride-containing amorphous calcium phosphate-casein phosphopeptides.10 High concentrations of fluoride (greater than or equal to 5000 ppm) should be avoided because rapid remineralization of superficial enamel may impede remineralization of the deeper layer of the lesions, resulting in white-enamel opacities that will not allow return to the normal opalescence of sound enamel. This is based on rapid remineralization of the surface layer with high concentrations of fluoride and lack of remineralization with the deeper demineralized areas of clinically evident white spot lesions.
Photosensitivity. Before using a light device for bleaching, the dentist should be aware of any patient taking phototoxic drugs or those with certain skin conditions associated with photosensitivity. Some reports of patients experiencing negative skin reactions following light exposure, especially ultraviolet light, have occurred. These reactions have manifested as swelling of the lips and surrounding tissues (Figure 5).
Pregnant or Lactating Women/Young Children. As a precautionary measure, post-
pone treatment for pregnant/lactating women and young children. The author’s team generally advises in-office bleaching be postponed on vital teeth of young children until they are beyond the mixed dentition stage.
Case Presentation
A healthy 50-year-old male dentist requested tooth whitening. Because of his busy schedule and past history of noncompliance with take-home whitening systems, he decided on in-office whitening using the Philips Zoom WhiteSpeed Light-Activated System (Philips Oral Healthcare, www.philipsoralhealthcare.com). Zoom WhiteSpeed uses an LED lamp rather than emitting ultraviolet light.
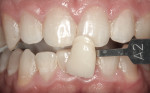
Clinical and radiographic examinations were completed. No medical or dental contra-indications were noted. The patient had no existing anterior restorations. Photographs and a preoperative shade of A2 were recorded (Figure 6). No history of tooth sensitivity was reported.
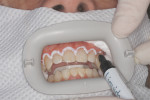
After the patient signed an informed consent form, his lips were protected using vitamin E oil, a retractor was placed, and his teeth were isolated with liquid rubber dam and cotton rolls (Figure 7). Zoom 25% hydrogen peroxide gel was applied three times for 15 minutes per application (Figure 8). The patient requested that the dental team do only a 45-minute treatment. During the procedure, the patient was monitored for sensitivity and reported none. Postoperative photos and a shade of B1 were recorded at the end of treatment. Because the patient already had a bleaching tray, he was given two additional syringes of Zoom Nite White for touchup if needed. The patient was seen 1 week after whitening (Figure 9) and reported he had performed only 1 night of tray whitening. The patient was pleased with the results.
Disclosure
Dr. Kugel has done research and lecturing for Philips.
References
1. Auschill TM, Hellwig E, Schmidale S, et al. Efficacy, side-effects and patients’ acceptance of different bleaching techniques (OTC, in-office, at-home). Oper Dent. 2005;30(2):156-163.
2. da Costa JB, McPharlin R, Paravina RD, Ferracane JL. Comparison of at-home and in-office tooth whitening using a novel shade guide. Oper Dent. 2010;
35(4):381-388. doi: 10.2341/09-344-C.
3. Kugel G, Perry R, Magnuson B, et al. Comparative Response of Whitening Strips versus In-office Light-assisted Whitening. Presented at: AADR Annual Meeting; March 20, 2014; Charlotte, North Carolina.
4. Abbot CH. Bleaching discolored teeth by means of 30% perhydrol and the electric light rays. J Allied Dent Soc. 1918;13:259.
5. Buchalla W, Attin T. External bleaching therapy with activation by heat, light or laser--a systematic review. Dent Mater. 2007;23(5):586-596.
6. Young N, Fairley P, Mohan V, Jumeaux C. A study of hydrogen peroxide chemistry and photochemistry in tea stain solution with relevance to clinical tooth whitening. J Dent. 2012;40(suppl 2):e11-6. doi: 10.1016/
j.jdent.2012.07.016.
7. Ontiveros JC, Paravina RD. Color change of vital teeth exposed to bleaching performed with and without supplementary light. J Dent. 2009;37(11):840-847. doi: 10.1016/j.jdent.2009.06.015.
8. Haywood VB, Cordero R, Wright K, et al. Brushing with a potassium nitrate dentifrice to reduce bleaching sensitivity. J Clin Dent. 2005;16(1):17-22.
9. Charakorn P, Cabanilla LL, Wagner WC, et al. The effect of preoperative ibuprofen on tooth sensitivity caused by in-office bleaching. Oper Dent. 2009;34(2):131-135.
10. Robertson MA, Kau CH, English JD, et al. MI Paste Plus to prevent demineralization in orthodontic patients: a prospective randomized controlled trial. Am J Orthod Dentofacial Orthop. 2011;140(5):660-668. doi: 10.1016/j.ajodo.2010.10.025.
ABOUT THE AUTHORS
Joe C. Ontiveros, DDS, MS
Head, Esthetic Dentistry
Head, Oral Biomaterials Division
Houston Center for Biomaterials and Biomimetics
Associate Professor, Department of Restorative and Prosthodontics
The University of Texas Health
Science Center at Houston
School of Dentistry
Houston, Texas
Gerard Kugel,
DMD, MS, PhD
Dean for Research
Department of Prosthodontics and Operative Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts
For more information, contact:
Philips Oral Healthcare
800-422-9448
www.philipsoralhealthcare.com