Creating an Esthetic Tissue Profile for Immediate Single-Tooth Replacement
A clinical case with contours facilitating a life-like final result
An implant-supported crown is often the treatment of choice for single-tooth replacement in the esthetic zone. However, maintaining and creating natural soft tissue contours and emergence profiles around dental implants is a key challenge in producing a seamless restoration that is harmonious with the adjacent teeth. In the anterior maxilla, atrophy is most severe during the first month following extraction, and the resulting loss of the buccal alveolar plate may lead to palatal implant positioning of the implants.1
Over the past 10 years, immediate implant placement and restoration of single maxillary teeth has been predictably employed.2 Advances in dental implant technology such as enhanced surface technology, thread designs, implant collar designs, and soft tissue seal in the implant/abutment interface have led to an implant process whereby bone and soft tissue preservation can be extremely predictable.3-5
Potential advantages noted with immediate implants include:6,7
• fewer surgical procedures, with completion of treatment in a shorter time frame.
• minimal soft tissue changes or loss.
• more predictable soft tissue emergence profiles for the final restoration.
• the patient is not compromised esthetically and functionally during the healing period.
The dental literature has shown that provisionalization of dental implants at placement, following minimally invasive surgical protocols and properly contoured esthetic provisionals, aids in the sculpting and preservation of esthetic soft tissue contours around dental implants in the esthetic zone.6,8,9
Case Presentation
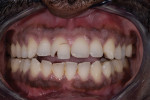
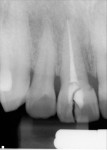
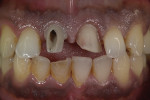
A 41-year-old male presented to the office as an emergency case after a bicycle accident that resulted in fracture of his upper right central incisor. Clinical examination revealed vertical and horizontal fractures of tooth No. 8 (Figure 1), indicating hopeless prognosis, and thus requiring extraction and prosthetic replacement. Radiographs revealed sound bone support and no periapical pathology (Figure 2).
Smile analysis showed that the patient’s original smile was not esthetically pleasing. There was a tooth width discrepancy between the maxillary central incisors, and their axial inclinations were canted with wear of the incisal edge, thus creating a reversed smile line. The upper and lower incisors were misaligned and crowded with mesial and buccal rotation of tooth No. 9, contributing to the upper centrals’ width discrepancy and the cant of the midline.
Thorough examination and bone sounding verified normal dentogingival complex (3 mm from the free gingival margin to the bone crest on the buccal aspect and 4.5 mm interproximally) and medium to thick gingival biotype. There were asymmetrical gingival levels between tooth Nos. 8 and 9, which contributed to the unpleasing look of the patient’s smile.
After reviewing multiple alternatives for implant placement procedures, the patient selected the option of immediate tooth removal, implant placement, and immediate provisional. It was determined that veneering of tooth No. 9 and replacing tooth No. 8 with an implant-supported Lava™ Zirconia (3M ESPE, www.3mespe.com) crown would accomplish the patient’s goal of a more uniform and symmetrical smile. Central dominance would be achieved by increasing the centrals’ length, which would result in a fuller, more pleasing smile that would correct the reverse smile line.
Treatment Protocol
Diagnostic casts were mounted on a semi-adjustable articulator for analysis of the occlusal factors influencing the case, and a diagnostic wax-up was facbricated to assess the effects of the proposed treatment.
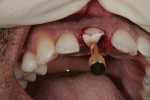
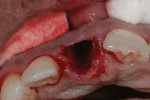
After administration of an appropriate local anesthetic, tooth No. 8 was removed by an atraumatic technique using periotomes (Salvin Dental Specialties, www.salvin.com) to luxate the tooth. A hole was drilled into the pulp chamber of the luxated tooth, and a post was drilled and cemented to the root canal. The tooth was then removed with coronal and rotational force (Figure 3), thus preserving the natural emergence profile of the surrounding gingival tissues as well as the labial and interproximal bone (Figure 4).
A tapered dental implant (5 x 13 mm NobelReplace® Tapered Groovy, Nobel Biocare, www.nobelbiocare.com) was then placed into the extraction site, which had been sized and extended following the long axis of extracted tooth to provide immediate fixation.
The bone architecture was normal, with marginal gap voids approximately 1 to 2 mm in width between the implant surface and the buccal cortex. When approximately two thirds of the implant fixture’s length had been placed, the marginal voids were grafted with bone graft material (mixture of Puros Allograft, Zimmer Dental, www.zimmerdental.com and Geistlich Bio-Oss®, Geistlich Biomaterials, www.geistlich-na.com) was placed into the differential between the fixture and the socket wall, and the fixture was advanced a few turns. This sequence was repeated until the fixture was fully seated to the level of the bony crest, approximately 3 mm below the gingival margin as measured on the labial. This technique causes the particles to be slightly compressed into the defect and results in excellent primary implant fixation.
Then a temporary abutment (Replace, Nobel Biocare) for the implant fixture was cut to length to keep it out of occlusion and coated with an opaque composite (Cosmedent, www.cosmedent.com) to eliminate any gray shine-through of the metal abutment.
The temporary implant abutment was screwed into the fixture and the temporary crown form was filled with provisional crown material (Luxatemp, DMG America, www.dmg-america.com) and seated. A cut section of a large size disposable applicator brush handle was placed into the hollow center of the abutment to keep the screw access hole clear of the provisional material.
When set, the temporary crown on the abutment was removed and additional composite was added from the abutment collar to the soft tissue margin area to support and maintain the soft tissue contour, creating a natural emergence profile for the provisional crown. The provisional abutment/crown was then contoured, adjusted to position it just out of occlusion, and polished all the way down to the collar of the temporary abutment. This assembly was placed by hand onto the fixture, and the access hole was closed with cotton and flowable composite.
The patient was monitored over the following 3 months to allow soft tissue healing and ensure that a stable gingival margin around the implant abutment existed. During this phase, some gingival margin contouring was performed on tooth No. 9 using a Biolase laser (Biolase, Inc., www.biolase.com) to correct uneven tissue heights between tooth Nos. 8 and 9, thus optimizing symmetry and maximizing esthetics.10
A fixture-level implant impression was taken with polyether impression material (3M ESPE) in a custom tray (open-tray implant impression technique). The impression was taken immediately on removal of the provisional, thereby giving very accurate gingival placement. It was very important that the implant abutment be waxed to the correct subgingival contours to give the identical tissue support as the provisional and ensure that contours led to a maximum distance of 5 mm from bone to interproximal contact. This would give good papilla support and prevent a black triangle from developing. The provisional abutment crown was reinserted in the mouth in the same manner as before.
By using the accurate gingival contours from the impression, the margin was placed approximately 1 mm subgingivally; this would allow excellent esthetics and ease of resin cleaning during seating and bonding of the crown.
Patient’s teeth were bleached with Zoom2 Whitening System (Philips Oral Healthcare, www.philipsoralhealtcare.com) and shade selection was made few days later.
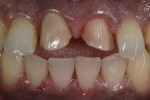
Three weeks later, the custom-made zirconia abutment was tried onto the implant fixture and a radiograph was taken to confirm complete seating of the abutment. The abutment screw was torqued down to 32 Ncm with a torque driver. Tooth No. 9 was prepared for a veneer (Figure 5) and an impression was taken for the No. 9 veneer and the No. 8 crown. The stump shade was recorded with a digital photograph for the laboratory. Provisional restorations were fabricated in a clear matrix material. The provisionals were trimmed, polished, and cemented.
A detailed prescription including a shade map, specification of crown form and length, surface texture, and incisal edge treatment was sent to the laboratory along with preoperative photographs, photographs of the preparations and provisionals, and the impressions and models. A wash bake of dentine was added onto the high value coping until the shade of the coping was identical to that of the stump shade of the prepared veneer of tooth No. 9 (Figure 6), then the Lava Zirconia crown for tooth No. 8 and the feldspathic veneer for tooth No. 9 were layered simultaneously to mimic each other.11
At the seating appointment, the completed restorations were evaluated for fit, color, and contour, and the restorations were shown to the patient for approval.
Some shade-matching challenges were anticipated because of the pure opaque white nature of the zirconia abutment. When dissimilar restorative materials are used, it is important to establish similar values before any addition of chroma is made. Excellent communication with the laboratory will facilitate the pursuit of an excellent treatment outcome.
The veneer was bonded to tooth No.9 and the Lava Zirconia crown was assessed for shade match with the bonded veneer. Additional staining was applied, and the crown was reglazed in the porcelain oven. The crown was then temporarily cemented into place. The patient was evaluated for occlusal contact in the centric, protrusive, and lateral excursive movements to ensure no contact was present at the implant site, and the restorations were polished.
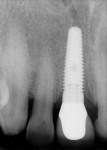
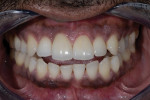
The patient returned 4 weeks later for reassessment of the No. 8 crown for stability of the gingival margin position; it appeared unchanged. The crown was then removed and recemented with Rely-X™ Unicem resin cement (3M ESPE) and a post-treatment digital radiograph was taken (Figure 7). Two weeks later, examination revealed no functional or esthetic problems. The postoperative photograph was taken at this time (Figure 8). Note the perfect matching between the final restorations and the natural dentition.
Slight mucosal asymmetry of Nos.8 and 9 was still observed after final treatment. This could be due to the facial remodeling that occurs even with the flapless extraction approach.12 Another reason could be the use of a temporary abutment after immediate implant placement. It is recommended to insert the final implant abutment as soon as possible after implant placement, preferably on the same day. This will avoid repetitive mutilation of the fragile peri-implant soft tissue collar, which compromises the mucosal barrier and results in a more “apically” positioned zone of connective tissue, thus leading to marginal bone resorption.13
A more predictable esthetic outcome could have been achieved in this case by using a smaller implant (4.3 mm instead of 5.0 mm); by using platform-switched abutments, which causes significantly less crestal bone resorption;14 or by placing a connective tissue graft at the time of immediate placement.15
Conclusion
Immediate placement and provisionalization of anterior single implants is a viable and predictable treatment option for single-tooth replacement in the esthetic zone; however, careful patient selection and treatment planning are still as important as the treatment itself. The treatment outcome in this presentation exceeded the patient’s expectations in creating an esthetic, bio-acceptable restoration.
About the Author
Emil Hawary, DDS, FAACD, FAGD, DICOI
Private Practice
Irvine, California
References
1. Younis L, Taher A, Abu-Hassan MI, Tin O. Evaluation of bone healing following immediate and delayed dental implant placement. J Contemp Dent Pract. 2009;10(4):35-42.
2. Cannizzaro G, Leone M, Consolo U, et al. Immediate functional loading of implants placed with flapless surgery versus conventional implants in partially edentulous patients: a 3-year randomized controlled clinical trial. Int J Oral Maxillofac Implants. 2008;23(5):867-875.
3. Brunski JB. Biomaterials and biomechanics in dental implant design. Int J Oral Maxillofac Implants. 1988;3(2):85-97.
4. Fischer K, Backstrom M, Sennerby L. Immediate and early loading of oxidized tapered implants in the partially edentulous maxilla: a 1-year prospective, clinical radiographic, and resonance frequency analysis study. Clin Implant Dent Relat Res. 2009;11(2):69-80.
5. Neugebauer J, Weinlander M, Lekovic V, et al. Mechanical stability of immediately loaded implants with carious surfaces and designs: a pilot study in dogs. Int J Oral Maxillofac Implants. 2009;24(6):1083-1092.
6. Petrungaro PS. Immediate implant placement and provisionalization in edentulous, extraction, and sinus grafted sites. Compend Contin Educ Dent. 2003;24(2):95-113.
7. Saadoun AP, Le Gall MG. Periodontal implications in implant treatment planning for aesthetic results. Pract Periodontics Aesthet Dent. 1998;10(5):655-664.
8. Petrungaro PS. Implant placement and provisionalization in extraction, edentulous, and sinus grafted sites: a clinical report on 1,500 sites. Compend Contin Educ Dent. 2005;26(12):879-890.
9. Petrungaro PS. Creation and preservation of natural soft tissue emergence profiles around dental implants in the esthetic zone. J Cosmetic Dent. 2009;24(4):66-80.
10. Adams TC, Pang PK. Lasers in aesthetic dentistry. Dent Clin North Am. 2004;48(4):833- 860.
11. Jones L. The art of matching select porcelain restorations to the anterior teeth: accreditation case type 2. Presented at: AACD Annual Scientific Session; May 15-19, 2007; Atlanta, GA.
12. Covani U, Cornelini R, Barone A. Bucco-lingual bone remodeling around implants placed into immediate extraction sockets: a case series. J Periodontol. 2003;74(2):268-273.
13. Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol. 1997;24(8):568-572.
14. Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
15. Grunder U. Crestal ridge width changes when placing implants at the time of tooth extraction with and without soft tissue augmentation after a healing period of 6 months: report of 24 consecutive cases. Int J Periodontics Restorative Dent. 2011;31(1):9-17.