The Bioclear Matrix and Peg Lateral Treatment
Three new factors give clinicians a new dimension in esthetics.
Treatment of a peg or undersized lateral incisor is a relatively common dilemma. Reported incidence of peg and undersized lateral (combined) is 4% to 5% of the population.1,2 This article will present an update of the treatment options and a novel technique using a new diastema closure matrix, the Bioclear Matrix System (Bioclear Matrix Systems, www.bioclearmatrix.com) and a balanced use of both flowable and paste composites.
There are many times when treatment of the peg or undersized lateral with a porcelain laminate is contraindicated because of orthodontic staging or patient age. There is also a second limiting factor, that of finances. Further steepening the financial impediment is lack of insurance coverage for the indirect (porcelain laminate) procedure.
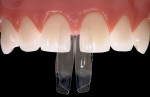
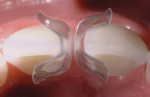
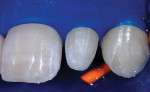
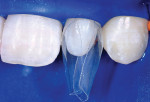
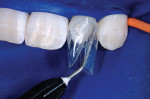
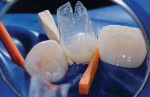
When choosing between composite and porcelain, aside from contraindications and finances, a third and most important consideration is that of ethics. Which procedure is the least invasive, most esthetic, periodontally healthiest, and most color-match stable? And, which can most predictably regenerate a papilla? Until recently, composite has been considered the “ugly cousin” and inferior to porcelain. However, with the introduction of the Bioclear diastema closure matrix, (Figure 1 and Figure 2) the improvement in some of the paste and flowable composites (Filtek™ Supreme Ultra, 3M ESPE, www.3mespe.com, in this example) and simplified polishing (Jazz™ polishers by SS White Burs, Inc, www.sswhiteburs.com) clinicians are beginning to consider direct composite as better than a porcelain veneer for diastema closure procedures, especially when only one or two teeth require treatment. To justify the clinician's time and overhead, a commensurate fee should be charged. For example, the author's fee ranges between 150% and 200% of a 4-surface composite fee. In this case, because both interproximal areas needed restoring, it was 200%. Others charge the crown fee less the laboratory cost.
In years past, a composite veneer was grainy, ugly, and clinically difficult to perform. Today the composite veneer can be very esthetic, smoother than porcelain, and a joyful procedure for both the doctor and patient.
In the author's experience he has observed that many of the no-reduction porcelain veneers done elsewhere that have later presented in his office have marginal discrepancies compromising the “pink esthetics” and periodontal health of the affected teeth. Research has shown that prosthetic marginal discrepancy greater than 50 µm will cause untoward tissue response.3-6 A large percentage of the diastema closures currently being treated with direct composites or porcelain can have marginal ledges exceeding 500 µm. If we are to “do no harm” as we embark on elective diastema closure, we must “elevate our game.”
Case Presentation
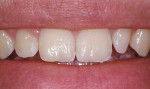
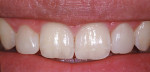
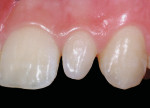
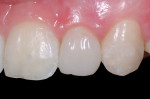
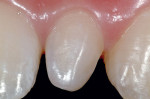
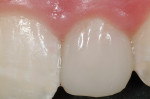
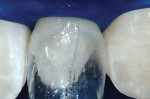
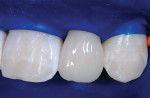
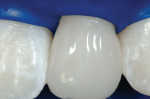
This 15-year-old female patient had recently finished orthodontic treatment. Preoperative and 2-week follow-up photographs show the ideal tissue response and highly polished composite surface (Figure 3, Figure 4, Figure 5 and Figure 6). High-magnification views (Figure 7 and Figure 8) demonstrate the ideal tissue response and the good esthetics of the composite's infinity edge gingival margin.
Using a Rubber Dam
The rubber dam is often dismissed for anterior esthetics as unnecessary or worse, counterproductive. As developer of the matrix, the author has found that, in most cases, the amount of interproximal gingival retraction afforded by the rubber dam is ideal for predicting the amount of static tension needed to generate or regenerate a papilla (Figure 9). Immediately before matrix placement, application of an astringent such as aluminum chloride underneath the dam and brushed into the sulci provides an ideal control of crevicular fluids for 15 minutes. Once the rubber dam is removed, the tissue rebounds and tissue contour generally becomes extremely favorable.
To adequately remove biofilm, the teeth are painted with disclosing solution and then meticulously sprayed with a pressurized aluminum tri-hydroxide/water mix (such as ProphyJet® DENTSPLY International, www.dentsply.com; or Prophy Plus, Bioclear Matrix Systems) Clinicians must be reminded that phosphoric gel etchant alone cannot be relied upon to remove plaque to achieve an ideal bond to enamel or dentin.
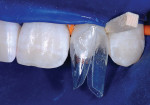
Two dedicated diastema closure matrices (Bioclear Matrix DC-202) are inserted inciso-gingivally until the gingival aprons of the matrices are near the depth of the sulcus (Figure 10 and Figure 11).
The Staged Wedging Technique
Stage I
In this case and with most similar cases, the author used only the gentle cuffing pressure of the rubber dam and the self-sealing action of the Bioclear matrix to seal the gingival margin. Clinicians also can incorporate a gentle approximating device such as a Wedjet® (Coltène Whaledent, www.coltene.com) or an Interproximator (Bioclear Matrix Systems) to provide additional gentle lateral pressure to seal the gingival margins. Use of a traditional wooden or plastic wedge during phase one of staged wedging must be avoided to prevent deformation of a pre-curved matrix.
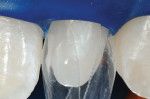
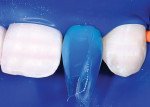
The teeth are then etched with 37% phosphoric acid (Figure 12), rinsed, dried, and a thin layer of bonding resin is placed and air-thinned but not cured. Next, the small canula of the flowable composite is angled into the interproximal from both facial and lingual and a small amount of flowable composite is placed and then light-cured (Figure 13, Figure 14 and Figure 15).
Stage II
Once two small “hips” of flowable composite have been placed and light-cured, an aggressive wedging force (Stage II) with a traditional wedge must be implemented to separate the teeth to compensate for the thickness of the Mylar for a snug contact (Figure 16 and Figure 17). For anterior teeth that are more easily displaced than posterior teeth, strong wedging pressure will generally compensate for the two sheets of Mylar (or Bioclear matrices) mesially and distally in order achieve a tight contact. Once the teeth are wedged, the remainder of the space is injection molded (a small dollop of uncured flowable chased with paste composite) then light-cured all together.
“In the Sulcus” vs “On the Gingiva”
The key to ideal papilla regeneration in the diastema closure procedure whether performed with porcelain or composite is to provide aggressive cervical curvature that begins subgingivally.7 Many traditional diastema treatments achieve closure with composite or porcelain that reaches mesio-distally—“on top” of the gingiva. The “on top” approach leads to myriad problems that have given diastema closure, particularly with direct composite and a flat matrix, a bad name.
The Composite/Porcelain Tipping Point
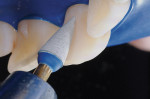
Unlike many of the porcelain veneer cases presented in dental journals, most of today's porcelain veneers in hometown dental practices are fabricated as monolithic (one single shade/type) porcelain, with either pressed or milled porcelain. While these monolithic porcelains are durable, they are generally more monochromatic than the older style, hand-stacked porcelains. Composites, on the other hand, just keep getting better. Single-step, diamond-impregnated polishers, such as the SS White Jazz polisher, in the properly trained hands, can create a smoother composite finish than is often possible with typical porcelain (Figure 18, Figure 19 and Figure 20). The new Bioclear matrices, which now come in twenty unique versions (Figure 21 and Figure 22), including eight matrices just for diastema closure, make the needed shapes such as the double convexity required for peg laterals or black triangle elimination.
A full discussion of the advantages of direct resins is beyond the scope of this article. However, two advantages that must be mentioned are color matching and pink esthetics. Most dentists will agree that when doing only one or two veneers, achieving an ideal color match is extremely challenging. This can lead to a joyless and unprofitable procedure. The advantage of the contact lens effect with direct composite makes color matching more predictable and simpler than is the case with a single unit of porcelain next to natural teeth. The color of the tooth is leveraged through the composite in a different way than through porcelain. The advantage is manifested when the patient's nonrestored anteriors change colors throughout the day (when dehydrated for smiling and talking) or gradually darken over the years. In this aspect, the composite restored lateral incisor can have a more consistent long-term color match than will the porcelain restored lateral incisor.
The true infinity edge (feather edge on non-prepared enamel) margin is only possible with direct composites. A composite margin can easily be thinned and polished to have an almost microscopically imperceptible margin. Composites' infinity edge benefits both color matching and pink esthetics.
Resin Veneer Maintenance
Some of the new microfills (nano-composites) hold their polish quite well and wear at similar rates to human enamel. They are, however, susceptible to the harsh abrasives—such as the hygienist's prophy paste, indiscriminate use of metallic ultrasonic scalers, and aggressive air blasters. This is no longer a problem in the author's practice. He spent a few minutes training his hygienists to use the Jazz polisher to restore the factory finish to the patient's composites as needed at each recall. It takes the hygienists approximately 3 seconds per tooth and the Jazz polishers can be autoclaved and re-used up to 100 times. Patients love the glassy smooth feel, and it creates a value added for the patient's hygiene appointment and a source of pride for the hygienists.
Conclusion
Three new factors—modern resin chemistry, breathtaking composite polishing, and Bioclear anatomic matrices—are combined with procedural advances such as the balanced application of flowable/paste composite along with the staged wedging technique, giving clinicians a new dimension in anterior esthetics. While some training is necessary, these techniques should be within the grasp of all clinicians especially those who use magnification.
References
1. Albashaireh ZS, Khader YS. The prevalence and pattern of hypodontia of the permanent teeth and crown size and shape deformity affecting lateral incisors in a sample of Jordanian dental patients. Community Dent Health. 2006;23(4):239-243.
2. al-Emran S. Prevalence of hypodontia and developmental malformation of permanent teeth in Saudi Arabian schoolchildren. Br J Orthod. 1990;17(2):115-118.
3. De Boever JA, De Boever AL, De Vree HM. Periodontal Aspects of cementation: materials, techniques and their biologic reactions. Rev Belge Med Dent. 1998;53(4):181-192.
4. Sorensen Se, Larsen IB, Jorgensen KD. Gingival and alveolar bone reaction to marginal fit of subgingival crown margins. Scand J Dent Res. 1986;94(2):109-114.
5. Sorenson JA. A rationale for comparison of plaque-retaining properties of crown systems. J Prosthet Dent. 1989;62(3);264-269.
6. Lang NP, Kiel RA, Anderhalden K. Clinical and microbiological effects of subgingival restorations with overhanging or clinically perfect margins. J Clin Periodontol. 1983; 10(6):563-578.
7. Bichacho N. Cervical contouring concepts: enhancing the dentogingival complex. Pract Periodontics Aesthet Dent. 1996;8(3):241-254.
About the Author
David Clark, DDS
Private Practice
Tacoma, Washington