Prescriptive and Predictable Black Triangle Treatment
Matrix system and universal composite offer noninvasive solution
Jihyon Kim, DDS
Providing minimally invasive esthetic solutions to patients in order to help increase their comfort and confidence is one of the most critical aspects of a dentist's job. As the emphasis on having an attractive smile continues to grow throughout society, more and more patients are coming forward to request a variety of treatments to improve their smiles.
One request that is becoming increasingly commonplace is for treatment to eliminate the appearance of black triangles. Also known as open gingival embrasures, black triangles are not only unesthetic but are also prone to food and plaque buildup. Unfortunately, adult orthodontic treatment results in black triangles approximately 40% of the time.1,2
Fortunately, however, there is a straightforward and noninvasive solution that is simple to perform and provides esthetic results for patients. The following case demonstrates a step-by-step method to achieve black triangle closure using an additive approach featuring a matrix system and a universal composite.
Case Report
A male patient presented to the office with unesthetic black triangles in his upper anterior and lower anterior sextants. He had recently completed orthodontic treatment to address the situation; however, he was disappointed that this initial treatment not only failed to resolve his esthetic concerns but actually made them worse. Because the black triangles remained, the patient subsequently sought out alternative treatment options. He was primarily interested in finding a conservative solution that would successfully and effectively close his black triangles.
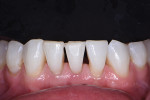
Before beginning treatment, the patient's overall situation was assessed in order to identify any potential challenges. In this case, the patient was congenitally missing tooth No. 26, and his black triangles were moderate to large in size (Figure 1). The challenge was to close the spaces while creating anatomic tooth contours and widths and maintaining the proper verticality of the contact lengths.
The first step was to isolate the area using a rubber dam in order to guarantee the best field control and soft-tissue retraction. Following isolation, the teeth were dried, and a disclosing solution was applied once to reveal any biofilm, which was then removed with aluminum trihydroxide in an air polisher (The Blaster, Bioclear) (Figure 2). Completely clean interproximal spaces are crucial for strong adhesion and the effective closure of black triangles; therefore, the use of a rubber cup and pumice would have been inadequate to remove the biofilm that was present in these interproximal spaces.
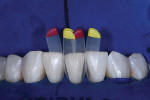
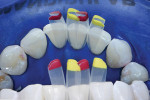
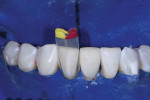
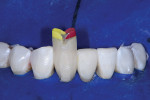
Next, small incisor matrices were selected from a matrix system (Black Triangle Intro Kit, Bioclear) and placed (Figure 3 and Figure 4). This matrix system was specifically designed for the postorthodontic finishing of cases in which black triangles may have resulted as well as for the closure of black triangles in orthodontically well-aligned cases. A black triangle gauge, which is included with the system, was used prior to isolation to select an appropriate mix of matrices in order to close the patient's spaces and maintain the vertical contacts without canting. Tooth No. 24 was injection molded first, followed by tooth No. 25, using a universal composite (Filtek™ Universal Restorative [shade A1], 3M) (Figure 5 and Figure 6). Critical to injection molding is the excess volume, which creates a monolithic inner core while driving defects to the outer layer. This outer layer is subsequently removed, and discs are used to finish the inner core into the final desired shape.
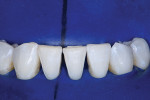
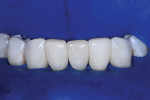
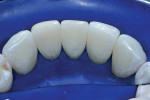
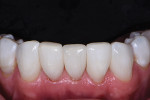
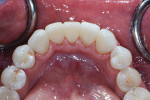
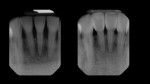
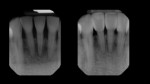
At the end of the case, a total of four black triangles were closed between tooth No. 22 and tooth No. 27 (Figure 7). It was important that the treatment resulted in proper anatomic shapes and a polish that was pleasing and felt natural to the tongue (Figure 8). The final result achieved an immediate closure of the spaces as well as an atraumatic tissue condition with adaptation to the new shapes (Figure 9). In the immediate postoperative retracted view, it can be seen that the teeth are still dehydrated, but the color blending that was possible with the universal composite can already be appreciated (Figure 9). The immediate postoperative retracted occlusal view (Figure 10) and pre- and postoperative radiographs (Figure 11 and Figure 12) further demonstrate the atraumatic and favorable tissue response and adaptation.
In conclusion, the black triangles were closed with a minimally invasive additive technique (ie, no tooth reduction) using the matrix system and universal composite. The anatomic matrices enabled predictable, atraumatic outcomes with subgingival contour changes that would be difficult to achieve with other direct restorative methods. The final result accomplished a beautiful blend of the universal composite with the natural tooth color. As a result of the composite's excellent polishability and shine retention, the restorations exhibited both natural-looking contours and colors. The black triangles were successfully closed, and most importantly, the patient was thrilled with his new smile.
About the Author
Jihyon Kim, DDS
Private Practice
Bellevue, Washington
References
1.Kim J, Clark DJ. Full-mouth black triangle treatment protocol. Dentistry Today website. https://www.dentistrytoday.com/restorative/minimally-invasive-dentistry/10320-full-mouth-black-triangle-treatment-protocol. Published August 1, 2017. Accessed November 19, 2019.
2. Kurth JR, Kokich VG. Open gingival embrasures after orthodontic treatment in adults: prevalence and etiology. Am J Orthod Dentofacial Orthop. 2001;120(2):116-123.
3. Tanaka OM, Furquim BD, Pascotto RC, et al. The dilemma of the open gingival embrasure between maxillary central incisors. J Contemp Dent Pract. 2008;9 (6):92-98.
For more information, contact:
3M
3m.com
888-364-3577