Replacing the Natural Tooth System in the Esthetic Zone: Flapless Implant Placement and Simultaneous Restoration to Preserve Tissue Contours and Guarantee Esthetics
Paul S. Petrungaro, DDS, MS
Over the last decade, the number of cosmetic dental procedures performed in the general dental practice has increased steadily each year. Likewise, the use of dental implants as a tooth replacement option has become a more routine treatment alternative for patients missing teeth or requiring tooth removal.1-3 However, these dental disciplines—cosmetic dentistry and dental implantology—have rarely been mentioned at the same time. Some of the reasons for this have been pre-existing dental materials, implant systems, abutment options, and/or ceramic materials. One of the most significant reasons for compromised esthetics when replacing the natural tooth system in the esthetic zone is the surgical procedure itself. Insufficient gingival and/or alveolar contours, biologic width invasions, endodontic failures, aggressive post and core preparations, and advanced periodontal disease can lead to difficult situations when the surgeon places the dental implant fixture after tooth removal.4,5 Current concepts in bone grafting and soft-tissue replacement can be effective in replacing both hard- and soft-tissue contours; however, due to the necessity for incisions, many times the significant areas that provide the foundation for the esthetic restorations, the emergence profile area, and papillary regions are the ones that remain cosmetically affected.6-8
The multi-step, conventional approach to implant reconstruction also contributes to a loss of gingival structure, especially in the esthetic zone. In the case presented here, a buccal fenestration existed that was 8 mm from the midfacial crest of bone. This scenario can lead to an increased incidence of gingival recession after surgical manipulation following tooth removal. This results from the fact that support of the buccal soft tissue does not exist following tooth removal in the site with a buccal dehiscence and/or fenestration. If the site is not grafted at this point, or a combined bone graft/implant placement procedure is not accomplished at the time of removal, collapse of the buccal soft tissues will be observed.
Multiple surgical procedures, flap elevations, and flap advancements can all result in gingival recession and discrepancies in the esthetics of the final implant-supported restoration and the adjacent and/or contra-lateral tooth. This dilemma has led this author and others to adopt, whenever possible, a conservative flapless surgical approach for the placement of the dental implant and replacement of necessary alveolar contours, in conjunction with the immediate provisionalization of the dental implant at placement.9-13
The following case report demonstrates a conservative, state-of-the-body technique for tooth replacement in the esthetic zone that simplifies the surgical and restorative implant process and provides a high success rate for the esthetic replacement of the natural tooth system in the esthetic zone.
Case Presentation
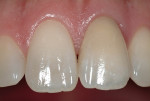
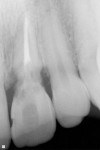
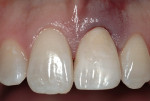
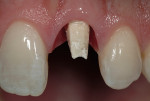
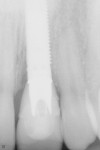
A 31-year-old, non-smoking male presented for tooth replacement at the left central incisor (Figure 1). The past history of the tooth included a traumatic injury, 2 root canal treatments and, at the time of consultation, the tooth was undergoing external resorbtion (Figure 2). The patient declined any restorative alteration of teeth #8 and #10, as well as esthetic enhancement of tooth #8. In addition, he requested an implant restoration at tooth #9 to correct the existing papillary height present between tooth #8 and #9. The challenge in this case was to remove tooth #9 and complete the implant reconstruction process without changing the gingival appearance in the esthetic zone.
Clinical Protocol
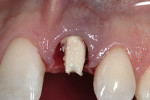
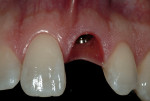
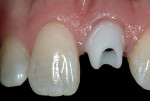
An appropriate local anesthetic was administered, and tooth #9 was removed by an atraumatic process, maintaining the pre-existing gingival contours (Figure 3). Salvaging the natural tooth shell of #9 allowed the natural tooth to serve as the esthetic provisional. After a thorough debridement of the extraction socket and removal of all remnants of the periodontal ligament space, site preparation for placement of the dental implant was completed. Following atraumatic coring procedures, healing enhancement precedes implant placement.
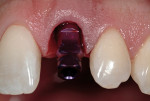
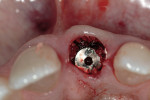
Platelet-rich plasma, fabricated by harvesting 20 cc of autologous whole blood from the patient prior to surgery and centrifuged in a cell separator (SmbodyPReP®2, Harvest Technologies, Plymouth, MA), allows a concentrated application of platelets that contain growth factors, which have been shown to enhance soft tissue healing, and the bone replacement process.14-17 Once platelet-rich plasma has been placed into the osteotomy site and the implant surface has been coated, the implant fixture is seated within the housing of the extraction socket (Figure 4).
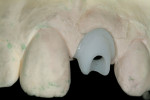
A 4.7 mm x 16 mm in length internal hex implant (Tapered Screw-Vent, Zimmer Dental, Carlsbad, CA) was seated to the appropriate depth and correct spatial angulation. Implant placement was followed by construction of the esthetic temporary restoration. Preparation of a stock temporary abutment (Hex-Lock® plastic temporary abutment, Zimmer Dental) to the appropriate dimensions and insertion into the implant fixture (Figure 5) precedes retrofitting of the shell of the natural central incisor.
Following removal of the root at the level of the cementoenamel junction, the tooth shell is hollowed out and acid etched, and a bonding agent is applied. Filling the shell with composite material (Filtek™, 3M™ ESPE™, St. Paul, MN) and placement of the shell over the prepared provisional abutment is followed by curing of the composite with a curing light (Figure 6). Once the composite is set, the provisional is removed, along with the provisional abutment. The provisional abutment is then placed into an analog; the retrofitted tooth shell seated back on the provisional abutment; and the margins corrected with flowable composite (Filtek™ Flow, 3M ESPE) extra-orally (Figures 7 and 8). Once the natural tooth shell has completed its conversion into the esthetic provisional and prior to re-insertion of the temporary abutment/ restoration complex, the flapless bone grafting procedure is accomplished.
To correct the osseous defect present between the buccal surface of the implant fixture and the pre-existing buccal plate, the platelet-rich plasma-enhanced graft complex (Puros®, Zimmer Dental) is condensed into the void previously described (Figure 9). Once the defect has been obliterated with the graft complex, a final application of platelet-rich plasma serves as a bioactive barrier.
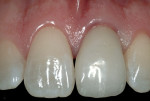
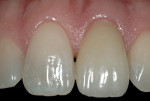
Reinsertion of the abutment/provisional complex was completed by seating the provisional with a temporary cement (Provicol QM, VOCO, Cuxhaven, Germany). When viewing the immediate post-treatment clinical results (Figure 10), it should be noted that the soft-tissue contours were preserved throughout the entire surgical and provisionalization procedure. At the 1-month postoperative visit (Figure 11), the desired soft-tissue emergence profiles had been obtained (Figure 12).
A fixture-level impression taken at this time facilitated the fabrication of an esthetic ceramic abutment. The custom ceramic abutment (Figure 13) was seated at the 2-month post-implant placement visit (Figure 14), along with an esthetic tissue sculpting provisional (Figure 15), to allow continued tissue sculpting and maintenance for the remainder of the healing phase. At the 3-month post-implant placement visit, the patient was returned to the esthetic dentist for the fabrication of the all-ceramic final implant-supported restoration (Figure 16).
Tissue contours and emergence profiles remained consistent throughout the entire treatment process and enhanced the ceramic restoration (compare Figure 16 to Figure 1). As a result of this technique process, the treatment provided a natural appearing implant restoration, all within a 4-month time period that spanned tooth removal to final restoration (Figure 17).
It is important to note that the incidence of less than 1 mm of soft-tissue recession at the distal line angle of the left central incisor in this case can be attributed to the immediate restoration procedure and subsequent provisionalization at placement. This may relate to the contours of the provisional/abutment complex, method of extraction, lack of bone replacement procedures, pre-existing gingival inflammation, and/or lack of gingival thickness or improper implant placement. These carious problems can be attributed to the difficulty in evaluating subgingival bony contours that are usually associated with flapless, immediate restoration/loading procedures. Adequate training and surgical experience are required to decrease the incidence of such complications occurring.
Conclusion
The immediate temporization of dental implants at placement, following a flapless approach after tooth removal, can lay the foundation for the formation and maintenance of the soft-tissue contours necessary to enhance the clinical appearance of the implant-supported restoration in the esthetic zone. The conservative nature of this technique promotes simplification of the implant process, provides an esthetic, non-removable provisional, and facilitates a shorter healing phase. The patient is returned to a normal lifestyle in a more rapid fashion after receiving a natural-looking tooth replacement.
Acknowledgments
The author would like to thank Mr. Edgar Jimenez of North Oaks, MN, for his excellence in fabricating the ceramic abutments, final provisionals, and esthetic ceramic restorations; and Dr. David Kell of Hudson, WI, for his excellence in cosmetic dentistry.
Disclosure
The author is a shareholder in Harvest Technologies and a paid consultant for Zimmer Dental.
References
1. Kois JC. Altering gingival levels: The restorative connections. Pbody 1: Biological variables. J Esthet Dent. 1994;6:3-9.
2. Spear FM. Maintenance of the interdental papilla following anterior tooth removal. Pract Periodontics Aesthet Dent. 1999;11(1):21-8.
3. Garber DA, Belser UC. Restoration-driven implant placement with restoration-generated site development. Compend Contin Educ Dent. 1995;16(8):796-804.
4. Grunder U, Spielman HP, Gaberthuel T. Implant-supported single tooth replacement in the esthetic region: a complex challenge. Pract Periodontics Aesthet Dent. 1996;8(9):835-42.
5. Touati B. Improving aesthetics of implant-supported restorations. Pract Periodontics Aesthet Dent. 1995;7(9): 81-92.
6. Petrungaro PS. Bone grafting at the time of extraction, a new technique for achieving natural bone and tissue contours in esthetic tooth replacement. J Cosmetic Dent. 2000; 16(2):30-43.
7. Petrungaro PS. Forming interdental bone contours and tissue emergence profiles. Contemp Esthet Restor Pract. 2000;16(3):30-7.
8. Saadoun AP. Single tooth implant restorations: surgical management for aesthetic results. Int J Dent Symp. 1995;3(1):30-5.
9. Saadoun AP, Le Gall MG. Periodontal implications in implant treatment planning for aesthetic results. Pract Periodontics Aesthet Dent. 1998;10(5): 655-64.
10. Salama H, Salama M. The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: a systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent. 1993;13(4): 312-33.
11. Petrungaro PS. Immediate restoration of implants utilizing a flapless approach to preserve interdental tissue contours. Pract Proced Aesthet Dent. 2005;17(2):151-8.
12. Kan JY, Rungcharassaeng K. Immediate placement and provisionalization of maxillary anterior single implants: a surgical and prosthetic rationale. Pract Periodontics Aesthet Dent. 2000;12(9): 817-24.
13. Petrungaro PS. Immediate implant placement and provisionalization in edentulous, extraction, and sinus grafted sites. Compend Contin Educ Dent. 2003;24(2):95-113.
14. Petrungaro PS. Platelet-rich plasma for dental implants and soft-tissue grafting. Interview by Arun K. Garg. Dent Implantol Update. 2001;11(6): 41-6.
15. Petrungaro PS. Using platelet-rich plasma to accelerate soft tissue maturation in esthetic periodontal surgery. Compend Contin Educ Dent. 2001;22(9):729-46.
16. Marx RE, Garg AK. Bone graft physiology with use of PRP and hyperbaric oxygen. In: Jensen OT, ed. The Sinus Bone Grafts. Chicago: Quintessence Pub. Co; 1999.
17. Anitua E. Plasma rich in-growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants. 1999;14(4): 529-35.
About the Author
Paul S. Petrungaro, DDS, MS
Director
The Institute for Advanced Dental Education, Inc.
Lake Elmo, Minnesota
Private Practice
Chicago, Illinois
Private Practice
Lake Elmo, Minnesota