Class II Restoration Combining a Low-Shrinkage Composite and a Centripetal Technique
A protocol for managing polymerization shrinkage and stress
Direct posterior resin composites are both esthetic and cost-effective.1 In larger restorations, enamel adhesion by the resin offers the potential to partially reinforce weakened tooth structure relative to a metallic restoration.2 Because of the large volume of resin required, however, polymerization stresses must be minimized at the time of placement to avoid fracture of either enamel bonds or remaining tooth structure.3 The increasing incidence of secondary caries and postoperative sensitivity observed with increased restoration size can probably be attributed to this factor.4,5 The large volume of missing enamel and dentin in these situations also necessitates the use of multiple layers of resin composite to restore a life-like appearance.6
In the clinical technique presented, a centripetal build-up technique was used to minimize polymerization stresses and to maximize esthetics.7 In an attempt to further minimize stresses, a resin composite that demonstrates reduced laboratory polymerization shrinkage was used. This characteristic results from a base resin, which polymerizes via a novel ring-opening reaction, and the resulting resin composite has demonstrated short-term clinical performance in posterior restorations comparable to methacrylate-based resin composites.8-11 The chosen resin composite (Filtek™ LS, 3M ESPE, www.3mespe.com) was paired with selective enamel etching and a self-etching adhesive compatible with its base resin.
Case Presentation
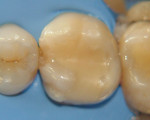
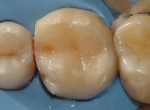
A 22-year-old Hispanic male presented to the clinic complaining of food impaction, difficulty flossing between teeth Nos. 3 and 4, and sensitivity on tooth No. 3 during mastication. After reviewing his medical history, he was classified as ASA I. Clinical and radiographic examination revealed the presence of a fractured Class II resin composite restoration and secondary caries at the gingival floor of the mesial box of a mesio-occlusal (MO) resin composite restoration of tooth No. 3 (Figure 1). A percussion test was mildly positive but sensitivity disappeared immediately. Periodontal examination revealed no bleeding upon probing and normal sulcular depths.
A direct restorative option was presented to the patient and benefits were discussed.
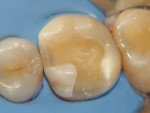
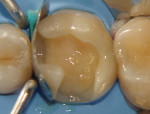
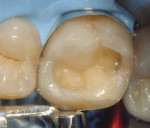
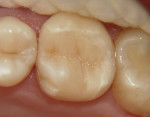
After local infiltration of articaine with 1:100,000 epinephrine (Septocaine®, Septodont, www.septodontusa.com), rubber dam isolation was achieved followed by the removal of the existing restoration using a high-speed handpiece with a 330 carbide bur (SS White, www.sswhitedental.com) under constant water cooling. Carious dentin was removed using a No. 4 round carbide bur (SS White) in a slow-speed handpiece under water irrigation. The finished cavity preparation with rounded internal line angles and cavosurface margins on sound enamel with no bevels can be seen in Figure 2. A 2% chlorhexidine digluconate Cavity Cleanser™ (Bisco, Inc, www.bisco.com) was used for 60 seconds to eliminate any surface contaminants. A pre-contoured sectional matrix band (Composi-Tight® Sectional Matrix band, Garrison Dental, https://garrisondental.com) was held in place by a wooden wedge (Sycamore Interdental Wedges, Kerr Corporation, www.kerrdental.com) and secured by G-Rings (Garrison Dental) (Figure 3). After selective etching of the enamel for 15 seconds, LS System Adhesive Self-Etch Primer (3M ESPE) was applied to the dentin using a disposable brush (Microbrush® International, www.microbrush.com) by rubbing for 15 seconds, followed by a gentle stream of air to evaporate the solvent, and then light-cured for 20 seconds at 450 nm (Elipar™ S10, 3M ESPE). The bonding agent (LS Adhesive Bond, 3M ESPE) was applied over the dentin and enamel using a disposable brush until a uniform layer was achieved and then light-cured for 20 seconds. A low shrinkage posterior A3 shade composite resin utilizing a silorane-based resin (Filtek™ LS, 3M ESPE) was placed, starting with the proximal wall of the proximal box followed by the first two of four triangular increments to restore the cusps, with each increment light-cured independently (Figure 4). Ochre color intensifier (Tetric® color, Ivoclar Vivadent, www.ivoclarvivadent.us) was placed in the central fossa before the final composite increment to enhance its natural appearance (Figure 5). Occlusal anatomy was enhanced using a NTI® OA3 finishing carbide (Axis Dental, www.axisdental.com). Excess adhesive and composite were removed from the proximal area using thin finishing strips (Sof-Lex™, 3M ESPE) and a No. 12 surgical blade. Finally, occlusion was checked using articulating paper (AccuFilm® II, Parkell, www.parkell.com) followed by polishing with an Enhance® finishing point (DENTSPLY Caulk, www.dentsply.com) (Figure 6).
Discussion
Posterior composite resin materials make durable and successful restorations if they are properly placed in teeth that meet the criteria for maintaining an enduring bond, especially in large preparations where the technique may be challenging. Positive outcomes are dependent on the clinician knowing the advantages and disadvantages of the material, especially concerning polymerization shrinkage and destructive polymerization stresses, which may develop without proper management. This clinical case demonstrated some clinical techniques to mitigate polymerization stresses.
In this case, a silorane composite resin was used because of its low-shrinkage properties.9 Despite its good mechanical, physical, and biologic characteristics,12,13 it is important to mention that there are not enough long-term clinical studies of the silorane-based composite,14 and this material cannot be used with conventional adhesive systems made for methacrylate-based resins.9,15
The centripetal build-up technique is a well-recognized method of reducing the effects of polymerization shrinkage. It allows development of proper anatomy and esthetics, enhances control of marginal overhangs, and reduces the need for finishing.7,16,17 Precise adaptation of the first increment in the box to restore the mesial surface of the tooth is a very important step.3 During this procedure, a thin proximal composite layer is placed against the matrix band and cured before additional composite increments are placed into the preparation. The restoration can then be completed using the Class I technique. The advantage of this is that the proximal layer of composite has no contact with the axial walls and thus has less risk of contracting away from the gingival margin during polymerization.7
Each individual cusp was then restored one at a time up to the level of the dental-enamel junction. Small sloping increments were applied in each line angle of the cavity and manipulation was kept to a minimum to avoid folding voids into the material. While initially time-consuming, this method can greatly reduce finishing time because the natural morphology of the teeth is progressively reconstructed.1
To improve the esthetic appearance of the restoration, an ochre color intensifier was placed in the central fossa before the final composite increment to create an appearance of depth. Many resin composite systems are designed in such a way that at least two different opacities with different optical properties are used to replace dentin and enamel separately. It is important to mention that Filtek™ LS does not have different opacities, thus with the addition of color intensifiers, the polychromatic variances in natural teeth can be simulated. However, in this case, the resin composite was selected more for its low shrinkage rather than for its esthetic qualities.10
Despite some disadvantages, posterior resin composite restorations are a cost-effective treatment. It is vitally important that practitioners use meticulous techniques to assure restoration durability and avoid postoperative complications.
Summary
The placement of composite restorations in posterior teeth is very popular and requires multiple considerations. The techniques described in this report provide patients with a durable and esthetic posterior restoration.
About the Authors
Mario F. Romero, DDS
Assistant Professor
Department of Oral Rehabilitation
Georgia Regents University
Augusta, Georgia
Fernando J. Haddock, DDS
Assistant Professor
Department of Oral Rehabilitation
Georgia Regents University
Augusta, Georgia
William W. Brackett, DDS, MSD
Professor
Department of Oral Rehabilitation
Georgia Regents University
Augusta, Georgia
Martha G. Brackett, DDS, MSD
Associate Professor
Department of Oral Rehabilitation
Georgia Regents University
Augusta, Georgia
References
1. Mackenzie L, Burke FJ, Shortall AC. Posterior composites: a practical guide revisited. Dental Update. 2012;39(3):211-212, 215-216.
2. Bernardo M, Luis H, Martin MD, et al. Survival and reasons for failure of amalgam versus composite posterior restorations placed in a randomized clinical trial. J Am Dent Assoc. 2007;138(6):775-783.
3. Tjan A, Bergh BH, Lidner C. Effect of various incremental techniques on the marginal adaptation of class II composite resin restorations. J Prosthet Dent. 1992;67(1):62-66.
4. Brackett WW, Browning WD, Brackett MG, et al. Effect of restoration size on the clinical performance of posterior “packable” resin composites over 18 months. Oper Dent. 2007;32(3):212-216.
5. Browning WD, Blalock JS, Callan RS, et al. Postoperative sensitivity: a comparison of two bonding agents. Oper Dent. 2007;32(2):112-117.
6. Lopes GC, Vieira LC, Araujo E. Direct composite resin restorations: a review of some clinical procedures to achieve predictable results in posterior teeth. J Esthet Restor Dent. 2004;16(1):19-31; discussion 32.
7. Bichacho N. The centripetal build-up for composite resin posterior restorations. Pract Periodontics Aesthet Dent. 1994;6(3):17-23.
8. Arrais CA, Oliveira MT, Mettenburg D, et al. Silorane- and high filled-based “low-shrinkage” resin composites: shrinkage, flexural strength and modulus. Braz Oral Res. 2013;27(2):97-102.
9. Duarte S Jr, Phark JH, Varjão FM, Sadan A. Nanoleakage, ultramorphological characteristics, and microtensile bond strengths of a new low-shrinkage composite to dentin after artificial aging. Dent Mater. 2009;25(5):589-600.
10. Tezvergil-Mutluay A, Lassila LV, Vallittu PK. Incremental layers bonding of silorane composite: the initial bonding properties. J Dent. 2008;36(7):560-563.
11. Weinmann W, Thalacker C, Guggenberger R. Siloranes in dental composites. Dent Mater. 2005;21(1):68-74.
12. Brackett MG, Bouillaguet S, Lockwood PE, et al. In vitro cytotoxicity of dental composites based on new and traditional polymerization chemistries. J Biomed Mater Res B Appl Biomater. 2007;81(2):397-402.
13. Burke FJ, Crisp RJ, James A, et al. Two year clinical evaluation of a low-shrink resin composite material in UK general dental practices. Dent Mater. 2011;27(7):622-630.
14. Mine A, De Munck J, Van Ende A, et al. TEM characterization of a silorane composite bonded to enamel/dentin. Dent Mater. 2010;26(6):524-532.
15. Lopes GC, Baratieri LN, Monteiro S Jr, Vieira LC. Effect of posterior resin composite placement technique on the resin-dentin interface formed in vivo. Quintessence Int. 2004;35(2):156-161.
16. Park J, Chang J, Ferracane J, Lee IB. How should composite be layered to reduce shrinkage stress: incremental or bulk filling? Dent Mater. 2008;24(11):1501-1505.
17. Szep S, Frank H, Kenzel B, et al. Comparative study of composite resin placement: centripetal buildup versus incremental technique. Pract Proced Aesthet Dent. 2001;13(3):243-250.