Interdisciplinary Full Mouth Rehabilitation
A systematic approach to design and execution
Amelia Orta, DMD
Patients who present with complex dental needs that require full mouth rehabilitation can make treatment planning difficult. Many clinicians have a vision of the overall treatment that they would like to provide; however, deciding where to start the case and how to sequence interdisciplinary care proves challenging. This article discusses a case that leveraged a systematic approach for the design and execution of a full mouth rehabilitation that required both restorative and surgical specialists.
Presentation, History, and Examination
A 42-year-old male patient expressed displeasure with his recently fabricated removable partial denture. To enhance his smile, he was seeking a "fixed solution" to replace his missing teeth that would improve both the function and esthetics.The patient's medical history included recent diagnoses of gastroesophageal reflux, hypertension, and obstructive sleep apnea. The patient's conditions were being managed by his primary care physician and controlled with Ziac and Prilosec OTC. Furthermore, the patient used a continuous positive airway pressure (CPAP) machine nightly and reported good compliance.
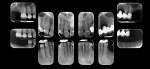
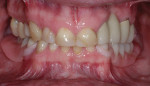
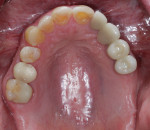
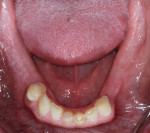
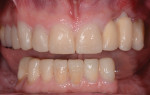
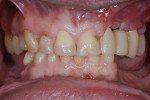
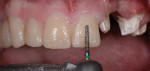
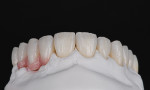
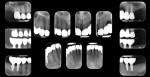
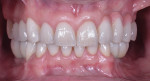
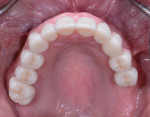
After a full mouth series of radiographs was taken to aid in diagnosis (Figure 1), a clinical examination was performed, which revealed a heavily restored dentition with recurrent dental caries and multiple restorations exhibiting poor marginal adaptation (Figure 2 through Figure 4). A comprehensive periodontal examination confirmed that all of the probing depths were 3 mm or less and that the maxillary and mandibular incisors demonstrated Class I mobility. Both the plaque and gingival inflammation indices were noted to be below 20%.
A dietary analysis and caries risk assessment revealed that the patient enjoyed sipping on sodas, which was likely the main contributing factor to his caries. A dietary consultation was provided, and an oral hygiene routine specific to caries management was recommended.
Next, a comprehensive occlusal analysis was performed, which included a digital pantographic tracing, a facebow record, a centric relation record, and diagnostic study models. The records and casts were transferred to a fully adjustable articulator by standard methods, and then it was programmed using the digital pantographic tracing system (Cadiax® Compact 2, Whip Mix), which allowed the patient's condylar pathways to be accurately reproduced throughout the treatment. Occlusal wear related to nocturnal bruxism was noted, so an occlusal guard was planned to protect the dentition following restorative treatment.
Diagnoses and Treatment Plan
After a review of the clinical findings and diagnostic information was completed, a comprehensive list of diagnoses was formulated, including recurrent caries, attrition, erosion, partial edentulism, a lack of posterior support, occlusal plane discrepancy, endodontically treated teeth, primary occlusal trauma (ie, excessive occlusal forces acting on teeth with normal periodontal support), localized compensatory eruption (ie, tooth eruption following tooth wear), and a loss of vertical dimension of occlusion.
The three diagnoses that were the most critical in designing the ultimate treatment plan were the primary occlusal trauma, compensatory eruption, and loss of vertical dimension of occlusion. The primary occlusal trauma, as indicated by splaying and mobility of the anterior teeth with radiographic signs of periodontal ligament widening, would require reestablishment of firm posterior support with a fixed solution. The compensatory eruption of the maxillary central incisors, which presented as uneven gingival levels and incisal and palatal wear, would require orthodontic intrusion or esthetic crown lengthening. The loss of vertical dimension of occlusion, clinically evident as excessive interocclusal rest space, excessive closest speaking space, loss of posterior support, and drooping lip commissures, would require the vertical dimension of occlusion to be restored.
A treatment plan was formulated and accepted by the patient for a full mouth rehabilitation that would utilize his remaining natural teeth and replace key missing teeth with implant-supported fixed restorations at a restored vertical dimension of occlusion. Due to financial limitations, restoring the patient to a full complement of teeth was not possible. The shortened dental arch concept was used to provide fixed posterior support for the vertical dimension of occlusion on a reduced number of occlusal units, and implants were planned for the sites of teeth Nos. 11, 20, 21, 29, and 30.1-3
Diagnostic Wax-Up
The casts were duplicated in preparation for a diagnostic wax-up. The wax-up, which was performed with the desired final esthetics as the guiding principle while also addressing the diagnoses, was systematically carried out in the following sequence4,5:
• Incisal edge position. The dental literature has established that anterior tooth display at rest follows average values for men and women.6 Examining the existing display at rest is a valuable parameter to assess when beginning a full mouth rehabilitation. Clinically, this patient displayed approximately 0.5 mm of the maxillary central incisors at rest, and the incisal edges appeared to be an appropriate length for both esthetics and phonetics. The existing incisal edge position of the maxillary central incisors served as the starting point for the wax-up.
• Facial volume. The facial volume of the maxillary incisors provides lip support and contributes to esthetics and phonetics. Clinically, the volume of the patient's anterior teeth appeared to be slightly deficient related to the wet/dry line. An additive wax-up on the facial surfaces was performed to provide pleasing volume. This allowed for the wax-up to be transferred to the mouth as a mock-up prior to any dental treatment and also contributed to more minimally invasive tooth preparations during the restorative phase.7
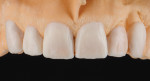
• Proportions. The width-to-length proportions of the central incisors are most pleasing when they follow the values established in the dental literature.8 Ideally, the central incisor width-to-length ratio should fall between 75% and 80%. Clinically, the patient displayed a reverse proportion, where the width appeared greater than the length. This reverse proportion was corrected by adding wax in an apical direction beyond the existing gingival margins to establish central incisors with a 10.5-mm length and an 80% width-to-length ratio. The lateral incisors and canines were waxed to complement the established proportions of the central incisors and provide pleasing gingival zenith positions (Figure 5).9
• Continuation of harmony. The buccal cusps of the posterior teeth were contoured to produce a smile curve that complemented the patient's flat lower lip,10 and buccal volume was added to increase the buccal corridor fill.
• Establish vertical dimension and occlusal plane. The patient's existing interocclusal rest space and closest speaking space were clinically evaluated and used to determine the proposed increase in vertical dimension of occlusion. In addition, the mandibular plane was evaluated, which revealed a negative display of the mandibular anterior teeth at rest. This information and the position of the retromolar pad were used to guide an additive wax-up of the incisal edges of the mandibular anterior teeth and establish the occlusal surfaces of the mandibular posterior teeth. The diagnostic wax-up was completed at a restored vertical dimension of occlusion, providing bilateral simultaneous contacts and a mutually protective occlusal scheme with shallow anterior guidance (ie, an occlusal scheme in which the posterior teeth prevent excessive contact of the anterior teeth in maximal intercuspal position and the anterior teeth disengage the posterior teeth in all mandibular excursive movements).
Intraoral Mock-Up
The diagnostic wax-up was transferred to the mouth using a putty matrix loaded with tooth shade bis-acryl material (Integrity® Temporary Crown and Bridge Material, Dentsply Sirona). Prior to seating the mock-up, the patient's teeth were lubricated with petroleum jelly to facilitate easy removal with a dental explorer following clinical evaluation. The mock-up was reviewed for the proposed esthetic changes, including enhanced facial volume of the central incisors, corrected tooth proportions, and increased buccal corridor fill. A phonetic assessment was performed to ensure that the additive mock-up did not pass the wet/dry line (Figure 6 through Figure 8). In addition, the increased vertical dimension of occlusion was evaluated by ensuring that the patient displayed a sufficient interocclusal rest space and closest speaking space while the mock-up was in place. The mock-up illustrated the need to apically position the gingival margin locations of teeth Nos. 6, 7, 8, and 9, which could be accomplished by means of orthodontic intrusion or esthetic crown lengthening.8 The mock-up appeared to be acceptable in all areas and was approved by both the patient and the clinician to guide the treatment that would be provided by the interdisciplinary team.
Consultations
Consultations with an orthodontist and periodontist were arranged to discuss the risks and benefits of each treatment. The patient wanted to avoid conventional orthodontic treatment, if possible. Due to the need for full coverage restorations and the fact that there was adequate root length, which was evident on the preoperative radiographs, esthetic crown lengthening was chosen as the preferred treatment approach.11
The periodontist evaluated the patient for esthetic crown lengthening via bone sounding of the facial margins of teeth Nos. 6, 7, 8, and 9. The bone sounding revealed a normal crest relationship of 3 mm from the free gingival margin to the bone crest, confirming the need for both osseous and soft-tissue alteration.12 A cone-beam computed tomography scan was used to evaluate the width and height of the alveolar bone and the proximity of anatomic structures at the edentulous site.
An endodontic assessment was performed, which confirmed that the roots of teeth Nos. 12 and 13 had been adequately obturated. Although tooth No. 25 demonstrated a slightly irregular fill, it was asymptomatic, so the decision was made to monitor it.
Treatment Sequence
Sequencing and executing the treatment plan required a coordinated approach between specialists. Optimizing healing and decreasing the amount of time that the patient would be in provisional restorations was a priority when developing the specific sequence of the treatment steps, which included the following:
• Provision of oral prophylaxis, fluoride varnish, and oral hygiene instruction specific to caries prevention by the periodontist.
• Creation of a removable splint by the prosthodontist to test alteration of the vertical dimension of occlusion in centric relation.
• Determination of the restorability of the previously crowned abutment teeth and provision of surgical access to the site of tooth No. 11 by the prosthodontist.
• Esthetic crown lengthening of teeth Nos. 6, 7, 8, and 9 by the periodontist.
• Surgical placement of implants by the periodontist at the sites of teeth Nos. 11 (to support a single-unit, implant-supported crown), 20 and 21 (to support splinted implant-supported crowns), and 29 and 30 (to support splinted implant-supported crowns), followed by a 4-month healing period.
• Removal of all existing restorations and caries by the prosthodontist, which was followed by the placement of full mouth provisional restorations over the natural teeth and osseointegrated implants at the restored vertical dimension of occlusion.
• Full mouth rehabilitation of the natural teeth and osseointegrated implants by the prosthodontist, which involved placement of all-ceramic restorations at the restored vertical dimension of occlusion.
In preparation for the surgical phase, the existing fixed partial denture (FPD) spanning Teeth Nos. 10 to 13 was removed to evaluate the restorability of the abutment teeth and provide surgical access to the tooth No. 11 site. An acrylic provisional FPD was then placed with temporary cement, and a removable splint at the proposed vertical dimension of occlusion was provided to the patient to test his adaptability.
Surgical Treatment
The surgical templates for both the esthetic crown lengthening and the implant placement were fabricated from the diagnostic wax-up using vacuum-formed stents. The periodontist used the surgical templates to guide the esthetic crown lengthening of teeth Nos. 6, 7, 8, and 9 (Figure 9) and implant (NobelActive®, Nobel Biocare) placement at the sites of teeth Nos. 11, 20, 21, 29, and 30. The implants were placed with insertion torque values in excess of 30 Ncm, and cover screws were placed as part of a two-stage surgical protocol. The implant at site No. 11 experienced an early failure due to a postoperative infection and was later recovered using reverse torque. The patient declined additional surgery, so the prosthetic plan was updated to include a natural tooth double abutment 5-unit FPD spanning teeth Nos. 9 through 13, using pink porcelain to camouflage the ridge defect. The patient remained in the care of the periodontist for 4 months while the implants healed, then the second stage of the surgery was performed to uncover them and place healing abutments. During the 4-month healing period, the patient continued to use the removable splint and demonstrated good adaptability to the proposed vertical dimension of occlusion with no signs of muscular or joint pain.
Restorative Treatment
After completion of the surgical treatment and osseointegration of the implants, the restorative treatment was initiated by the prosthodontist. The teeth were prepared for full-coverage polycrystalline ceramic restorations using the seated mock-up to guide the necessary tooth reduction (Figure 10). Teeth Nos. 9, 10, 12, and 13 required common draw to serve as FPD abutments for the pontic in position No. 11. Non-engaging temporary abutments were placed at implant site Nos. 20, 21, 29, and 30. Acrylic shells (Jet Provisional Crown & Bridge, Lang Dental), which were previously fabricated from the diagnostic wax-up using an indirect technique in preparation for this appointment, were relined over the tooth preparations and temporary implant abutments. The implant segments were sectioned from the natural tooth segments, and all of the sections were trimmed and polished. The natural tooth provisional restorations were cemented with temporary cement, and the implant provisional restorations were screw-retained. During the provisional phase, the patient was monitored to ensure his ongoing adaptation to the vertical dimension of occlusion and occlusal scheme as well as the presence of acceptable phonetics and esthetics.
Vinyl polysiloxane (VPS) impressions of the maxillary and mandibular provisional restorations were taken and poured in dental stone. The maxillary provisional cast was transferred to a fully adjustable articulator (Denar® D5A, Whip Mix) using a facebow record, and the mandibular cast was mounted using an interocclusal registration record in centric relation. A custom incisal guide table was then fabricated to replicate the guidance developed by the provisional restorations in the final restorations.
After the tooth preparations were refined, retraction cord soaked in buffered hemostatic solution (Hemodent®, Premier Dental) was packed in each gingival sulcus to facilitate the final impressions. The maxillary arch was impressed with VPS material (Extrude®, KaVo Kerr) using a stock tray. Open tray impression copings were placed at implant site Nos. 20 and 21 as well as at site Nos. 29 and 30, and each pair was splinted together with floss and pattern resin. The mandibular arch was then impressed with VPS material using a custom tray. Stump shade photographs and gingival shade photographs were taken for the ceramist's reference, and a series of interocclusal registration records in centric relation were made at the established vertical dimension of occlusion to allow cross-mounting of the working casts with the provisional casts. The impressions were poured, and the models were segmented into dies and mounted.
A full-contour wax-up was performed on the die models using the provisional matrices to precisely reproduce the incisal length and volume established by the provisional restorations (Figure 11). The excursive pathways were waxed according to the custom incisal guide table. Next, the die system casts and full contour wax-up were scanned into CAD design software and digitally cut back to facilitate a minimal layering design for maxillary unit Nos. 4 through 13 and mandibular unit Nos. 22 through 27.13 All of the remaining units were kept monolithic. The implant restorations at the sites of teeth Nos. 20 and 21 and 29 and 30 were splinted and screw retained. The units were milled from 3Y-TZP zirconia (Katana Zirconia HTML, Kuraray Noritake Dental). After an internal stain was applied directly to the zirconia to establish color contrast zones, firing porcelain (Cerabien™ ZR, Kuraray Noritake Dental) was added to create depth and color with minimal thickness.
A bisque try-in was performed, and each unit was inspected for proper interproximal contact, internal fit, marginal adaptation, and occlusion. The tooth supported FPD and splinted implant units were evaluated to ensure that they provided sufficient gingival embrasure space for hygiene. In addition, the esthetics of the case were reviewed, and any desired changes were photographed and noted for the ceramist. The ceramist then completed the desired adjustments, and all of the units were highly polished and glazed to prepare for their insertion (Figure 12).
Prior to placement, the intaglio of each zirconia unit was sandblasted with 50-μm alumina particles at 2 bars of pressure, and a single-component adhesive primer (CLEARFIL Ceramic Primer Plus, Kuraray Noritake Dental) was applied and allowed to air dry. To prepare the teeth for cementation, retraction cord soaked with buffered hemostatic solution was packed, followed by air abrasion with 30-μm silica-coated alumina particles. The tooth preparations were then rinsed and isolated. Once the preparations were completed, the units were bonded with a dual-cure self-adhesive resin cement (PANAVIA SA Cement Plus, Kuraray Noritake Dental), and the occlusion was adjusted and verified. A postoperative series of radiographs was taken to confirm marginal adaptation and the absence of cement debris (Figure 13).
To protect the restorations from nocturnal bruxism, a maxillary occlusal splint was fabricated in centric relation that was designed to not interfere with the patient's existing CPAP device. The patient was appointed to 1-day, 1-week, and 1-month recalls, and the importance of oral hygiene maintenance was enforced at each visit.
Conclusion
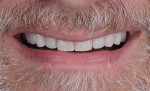
Adherence to the treatment sequence allowed for a predictable full mouth rehabilitation to be carried out by the interdisciplinary team. The final restorations provided an esthetically pleasing outcome that followed the design established in the diagnostic wax-up. In addition, the rehabilitation provided improvement to the patient's function because the fixed dental implant restorations supported the vertical dimension of occlusion with firm bilateral simultaneous contacts and a mutually protected occlusal scheme (Figures 14 through Figure 18).
Acknowledgement
The author would like to thank the team at the Ronald Goldstein Center for Esthetic and Implant Dentistry at The Dental College of Georgia at Augusta University, including faculty members Gerald Chiche, DDS; Jimmy Londono, DDS; Philip Baker, DDS; and Darshanjit Pannu, DDS, as well as periodontic resident Jason Strever, DMD, and Aram Torosian, MDC, CDT, for their advisement and contributions to the case. This work was supported by the Nobel Biocare/Augusta University Center of Excellence in Augusta, Georgia.
About the Author
Amelia Orta, DMD
Fellow
American College of Prosthodontics
Adjunct Clinical Faculty
Advanced Prosthodontics Program
Dental College of Georgia
Augusta, Georgia
Private Practice
Washington, DC
References
1. Käyser AF. Shortened dental arches and oral function. J Oral Rehabil. 1981;8(5):457-462.
2. Amsterdam M, Ingber J. The Distal Extension Case-Tooth-Tissue Borne Removable Appliance. Chicago, IL: Quintessence Publishing; 1981.
3. Starr NL. The distal extension case: an alternative restorative design for implant prosthetics. Int J Periodontics Restorative Dent. 2001;21(1):61-67.
4. Spear FM, Kokich VG, Mathews DP. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
5. Chiche G, Kokich V, Caudill R. Diagnosis and treatment planning of esthetic problems. In: Pinault A, Chiche G, eds. Esthetics in Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994.
6. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
7. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-16; discussion 17-18.
8. Sterrett JD, Oliver T, Robinson F, et al. Width/length ratios of normal clinical crowns of the maxillary anterior dentition in man. J Clin Periodontol. 1999;26(3):153-157.
9. Chu SJ, Hochman MN. A biometric approach to aesthetic crown lengthening: part I--midfacial considerations. Pract Proced Aesthet Dent. 2008;20(1):17-24; quiz 26.
10. Frush JP, Fisher RD. The dynesthetic interpretation of the dentogenic concept. J Prosthet Dent. 1958;
8(4):558-581.
11. Robbins JW. Tissue management in restorative dentistry. Functional Esthetics and Restorative Dentistry. 2007;1(3):2-5.
12. Kokich VG, Kokich VO. Interrelationship of orthodontics with periodontics and restorative dentistry. In: Nanda R, ed. Biomechanics and Esthetic Strategies in ClinicalOrthodontics. St. Louis, MO: Elsevier; 2005:348-372.
13. Venezia P, Torsello F, Cavalcanti R, et al. Retro-spective analysis of 26 complete-arch implant-supported monolithic zirconia prostheses with feldspathic porcelain veneering limited to the facial surface. J Prosthet Dent. 2015;114(4):506-512.