Creating Predictable Composite Contacts
Advances in matrix systems alleviate Class II restoration challenges
Parag R. Kachalia, DDS
On any given day, numerous Class II lesions caused by initial approximal or recurrent carries are restored across the world. For many years, the primary material of choice for these restorations was amalgam. When amalgam was properly condensed in conjunction with a Tofflemire matrix band and a wedge, more often than not, a proper proximal contact was achieved. During the last 20 years, amalgam has been used with less frequency for Class II restorations, and more of these lesions are being restored with composite.1 In many cases, composite allows the practitioner to use more conservative preparation designs when compared with traditional GV Black preparation designs and provides the patient with a more esthetic restoration; however, one of the key drawbacks is that creating the proper anatomical form as well as a dense proximal contact can be challenging. A proper contact is critical to prevent excessive tooth movement, minimize the chance of food impaction, decrease the rate of decay, and maintain periodontal health.2 Unlike amalgam, when composite is condensed, there is no true distension of the matrix band and adaption to the adjacent tooth. Instead, the composite generally moves coronally. To combat this issue, some manufacturers have released packable-type composites over the years; however, these packable composites can be difficult to manipulate, and they have been shown to form better contacts when used in conjunction with a sectional matrix system versus a circumferential matrix.3 In addition to the density of the contact, the anatomical form is also important. A proper Class II system should aid in the creation of an optimally tight and broad contact, proper embrasure form, and an adequate marginal seal as well as minimize flash. In recent years, tremendous advances have been made with respect to Class II matrix systems. This article explores how these advances can help alleviate a number of challenges to allow predictable proximal contacts when placing Class II composite restorations.
Class II Matrix Systems
When one thinks of an ideal Class II matrix system, the wedge, matrix, and separating ring must all be considered. Each component of the system can have a significant impact on the outcome of the restoration.
Wedges
Traditional wooden triangular wedges do a reasonably good job in terms of separating teeth and creating a gingival seal; however, the body of these wedges tends to invade the contact area. In addition, if a concavity exists in the gingival box form, a triangular-shaped wedge may not properly adapt, and an overhang may be present after completion of the restoration.4 Over the years, wooden wedges that are more anatomically shaped have been introduced; however, the industry has been trending toward the use of plastic wedges. During the last decade, manufacturers have introduced numerous plastic wedges that facilitate better adaptation in terms of creating a gingival seal yet stay clear of the contact area.
Matrices
An appropriate sectional matrix band is one of the most important aspects of creating a restoration with ideal contour and proper contacts.5 The composite that is placed will ultimately take the shape of the matrix; therefore, the clinician must take into account its vertical sizing, thickness, extensions, and shape. When Class II systems were first introduced, most sectional matrices had a kidney bean shape. They generally had a nice contour in the contact area; however, they tended to lack an occlusal contour to create a proper occlusal embrasure. In addition, many of these matrices did not have enough buccal-to-lingual extension to wrap around a line angle. Today, many manufacturers make matrix bands that address these issues. Many have also included tabs on the matrices so that they can be picked up easily, and the tabs can be approximated to the adjacent marginal ridge so that the restoration is not built too high occlusally. One key attribute of this new generation of matrices is that they extend past the line angles. This improvement allows practitioners to restore wider lesions with predictability, assuming they have invested in a newer-generation separating ring system as well.
Separating Rings
Although the improvements in matrices and wedges have helped with the predictability of Class II restorations, the greatest improvements seem to have come from advances in separating rings. The original Class II separating rings were made of stainless steel and had parallel or tapered tines. These tines were designed to engage the lateral portion of the embrasure space and adapt the matrix against the tooth to minimize flash. By applying force in the embrasure space, the teeth are pushed mesially and distally so that an appropriate contact can be created. One of the main issues with these rings was that there was relatively little forgiveness if the box form started to approach the line angles. As soon as the ring was placed, it would create a concavity in the matrix and then collapse. A decision also needed to be made regarding where to place the ring in conjunction with the wedge. The ring needed to be placed either on top of the wedge, between the wedge and the box form, or between the wedge and the adjacent tooth. When later separating ring designs were introduced, this problem was solved because they allowed the ring to sit on top of the wedge. In addition, newer rings also utilized a combination of stainless steel and nickel titanium to allow for greater adaptation and minimize the distortion and over-springing that was evident in the first generation of rings. During the last 10 years, many manufacturers have released rings that now allow an area for the wedge as well as possess some form of reinforcement so that the rings do not get overstretched and better maintain their memory. Furthermore, when compared with rings in the past, many of today's separating rings have added features so that they can be used on box forms that are much wider.
Case Report
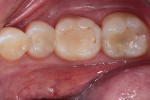
A patient presented with failing composite restorations on teeth Nos. 30 and 31, and the decision was made to replace these res-torations (Figure 1). After anesthetizing the patient with 1 carpule of lidocaine hydrochloride 2% and epinephrine 1:100,000 (Lignospan® standard, Septodont), a rubber dam (Paro® Non-Latex Rubber Dam, Clinician's Choice) was placed utilizing a No. 12A clamp (No. 12A Black Rubber Dam Clamp, Berman Dental Instruments) to provide proper isolation (Figure 2).6
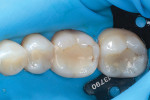
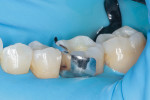
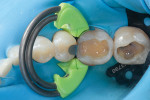
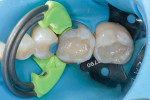
After removing the prior restorations and excavating the carious material, a matrix band (DualForce™ Ultra-Wrap™ Matrix Band, Clinician's Choice) was placed (Figure 3) in conjunction with an interproximal wedge (DualForce™ Active-Wedges, Clinician's Choice) (Figure 4). Anatomically, this wedge provides two important contours. It is concave on the lateral portions so that it adapts around the cervical portion of the dentition on both the mesial and distal surfaces, and it has a concavity on the spine so that it drops below the contact point. In addition, the tip of the wedge collapses when it is inserted and fully expands once it is completely seated in order to minimize the chance of it backing out.
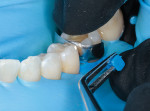
Once a complete insertion of the wedge was achieved, a separating ring (DualForce™ Molar Rings, Clinician's Choice) was placed on top of the wedge and fully seated to allow complete adaptation of the matrix band to the tooth. This separating ring has two concentric nickel titanium wires for increased separation force and memory retention. These factors are critical in achieving proper contact tightness.7 The ring goes a step further by incorporating separating prongs that closely mimic the anatomy, allowing for intimate adaption of the matrix and minimizing flash. In addition, the plastic used on the separating prongs is designed to prevent composite and adhesives from sticking.
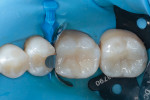
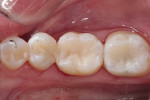
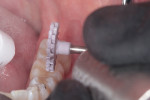
Next, a total-etch adhesive technique was employed, starting with a 35% phosphoric acid etchant (Ultra-Etch™, Ultradent Products, Inc.), followed by a complete rinse that was blotted dry. A 5% glutaraldehyde-based desensitizer with 35% 2-hydroxyethyl methacrylate (HEMA) (G5™ All-Purpose Desensitizer, Clinician's Choice) was then applied for 30 seconds to help mitigate sensitivity and provide an antibacterial effect.8 After air thinning, an adhesive (OptiBond™ Solo Plus, Kerr) was applied, air thinned, and polymerized for 20 seconds with a curing light (Valo™ Grand, Ultradent Products, Inc.). The light was placed in close proximity to each occlusal surface for the duration of curing. After placing a 0.5-mm layer of flowable restorative (Evanesce™ Flow, Clinician's Choice) and polymerizing for 20 seconds with a curing light outputting 1,000 mW/cm2, the mesial wall of tooth No. 30 was built up with a nanohybrid composite (Evanesce [shade B2, Universal opacity], Clinician's Choice) and polymerized (Figure 5). The teeth were then restored in sub-2 mm horizontal increments using the same nanohybrid composite that was used for the mesial wall (Figure 6). Each layer of composite that was placed was polymerized for 20 seconds from the occlusal aspect. After building to full contour, the ring was removed, and tooth No. 30 was polymerized again from the buccal and lingual aspects for 10 seconds each (Figure 7). The rubber dam was removed, and the occlusion was adjusted as needed with an extra-fine, small-diameter, football-shaped bur (379EF.FG.018, Komet USA) (Figure 8). Once proper occlusion was confirmed, the restorations were polished with a two-step technique, using polishers (A.S.A.P.® All Surface Access Polishers, Clinician's Choice) that provide luster without altering the anatomy (Figure 9).
Conclusion
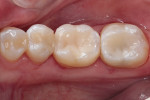
For many years, composite restorations were thought of as inferior in terms of function when compared with amalgam restorations. Thankfully, numerous advances have occurred in the world of adhesives and resins to allow for better materials, and there have been significant advances in complete Class II matrix systems. These systems focus on the pinch points with resin placement and allow composites to be placed with dense contacts and appropriate emergence profiles so patients can have both proper function and excellent esthetics (Figure 10).
Disclosure
Parag R. Kachalia, DDS, is a key opinion leader for Clinician's Choice Dental Products Inc.
About the Author
Parag R. Kachalia, DDS
Innovative Dental Concepts
San Ramon, California
References
1. Zabrovsky A, Neeman Levy T, Bar-On H, et al. Next generation of dentists moving to amalgam-free dentistry: survey of posterior restorations teaching in North America. Eur J Dent Educ. 2019;23(3):355-363.
2. Barnes DM, Blank LW, Thompson VP, et al. A 5- and 8-year clinical evaluation of a posterior composite resin. Quintessence Int. 1991;22(2):143-151.
3. Peumans M, Van Meerbeek B, Asscherickx K, et al. Do condensable composites help to achieve better proximal contacts? Dent Mater. 2001;17(6):533-541.
4. Patras M, Doukoudakis S. Class II composite restorations and proximal concavities: clinical implications and management. Oper Dent. 2013;38(2):119-124.
5. Kampouropoulos D, Paximada C, Loukidis M, et al. The influence of matrix type on the proximal contact in Class II resin composite restorations. Oper Dent. 2010;35(4):454-462.
6. Wang Y, Li C, Yuan H, et al. Rubber dam isolation for restorative treatment in dental patients. Cochrane Database Syst Rev. 2016;9:CD009858.
7. El-Shamy H, Sonbul H, Alturkestani N, et al. Proximal contact tightness of Class II bulk-fill composite resin restorations: an in vitro study. Dent Mater J. 2019;38(1):96-100.
8. Lopes AO, de Paula Eduardo C, Aranha ACC. Eval-uation of different treatment protocols for dentin hypersensitivity: an 18-month randomized clinical trial. Lasers Med Sci. 2017;32(5):1023-1030.