Sealing Exposed Dentin for a Maximum Bond
Efficient planning, preparation, temporization, and placement of porcelain using immediate dentinal sealing and a hydrogel separating medium.
Bonded porcelain veneers have been successfully placed for more than 20 years with a large degree of physiologic success and patient satisfaction, particularly when the majority of the preparation is on enamel.1 Conservative lamination of the teeth allows us to correct smile deficiencies when unwanted color exists, teeth are misaligned, or teeth are improperly positioned.2,3 Although many clinicians settle on a particular treatment protocol to satisfy their comfort level, there is always the need to re-evaluate our clinical techniques in the hopes of better clinical efficiency or treatment outcome.
Understanding patient expectations, thorough case documentation, non-anesthetized mock-up, provisional previews, and accurate laboratory communication are keys to case success.4 Transitional/temporary restorations are a critical part of that chain of success, particularly when dentin is involved in the preparation. Not only do they protect prepared tissues, transitional restorations allow a patient to preview the basic shade and shape of the proposed final restorations.5 Unfortunately, when considerable dentin is exposed during the preparation, their fabrication, patient tolerance, and removal can be stressful for both the patient and office staff.
Bonding to enamel is both predictable and desirable when placing porcelain veneers. However, many times because of decay, tooth position, or existing restorations, it is necessary to prepare and place porcelain on prepared dentin. The bond to dentin can be less dependable than the bond to enamel and can lead to potential problems with sensitivity and microleakage, especially during the temporary phase. Chipping, breakage, sensitivity, microleakage, and difficulty in removal are too often part of the experience. Most of these problems can be nearly eliminated by instituting the principles of immediate dentinal sealing (IDS).6
Clinical Advantages
The clinical advantages of IDS include achieving the highest bond strength to dentin, reducing sensitivity by sealing the dentinal tubules, reducing the chance of pulpal damage by bacterial habitation, and reducing contamination of dentin from microorganisms, blood, or chemicals during the temporary phase.
Achieving maximum bond strengths is critical to the success of long-term restoration and techniques for improving bond strengths should be considered for clinical efficiency. The best bond strengths to dentin are achieved immediately after tooth preparation using a three-step etch-rinse-dentin bonding agent (DBA) system.7,8 Total-etch bonding systems have produced higher bond strengths than self-etch systems because of superior etch patterns on enamel with phosphoric acid and the penetration of the hydrophilic primer and hydrophobic resins which infiltrate the micromechanically created area.9 Effective dentin bonding can diminish bacterial leakage, which can lead to staining, sensitivity, and potential pulpal irritation.10,11
Protocol
Immediately after tooth preparation or after the impressions are taken, the entire prepared tooth surface is etched, DBA is placed, the surface is air-thinned thoroughly to reduce film thickness, and then light-cured.12 The air-inhibited layer on the surface is then removed with ethyl alcohol on a 2 x 2 inch gauze and microbrushes and rinsed well. Wiping and rinsing with alcohol is then repeated. The removal of this layer on cured resin is important to reduce undesired bond of the temporary composite to the DBA.13
A bond between the temporary and the primed tooth can be catastrophic to office efficiency and dentist stress. The key is a predictable treatment sequence and reliable separating medium. A separating material designed specifically for IDS has been developed, which simplifies the procedure and increases predictability. PRO-V COAT® (Bisco, Inc., www.bisco.com) is a water-soluble hydrogel polymer separating medium that is placed on bonded teeth after the air-inhibited layer has been removed with alcohol.14 It is water soluble and provides worry-free placement of composite temporaries on top of the pre-bonded teeth without interference with mechanical retention of the temporary material. This hydrogel has a low water sorption to decrease microleakage between the bonded tooth and the temporary composite.
The temporaries are made using a self-cure composite material placed inside a matrix and onto the tooth. This “shrink wrap” technique is used where the provisionals are made to the tooth, not removed, and trimmed intraorally. IDS can be used as well for an indirect technique in which the provisionals are made, removed, trimmed, and re-cemented. The separating medium provides a predictable non-bondable interface between the bis-acrylic temporary material and the sealed dentin or between the temporary cement and the sealed tooth.
At the definitive restoration appointment, the temporaries are removed in conventional fashion with hemostats or prying instruments. After verification of restoration fit, the previously bonded surface is prepared for luting by pumice, diamond roughening, or light aluminum oxide abrasion.15 There are no apparent drop-in bonding strengths for up to 12 weeks between preparation, sealing, and restoration placement. Lower bond strengths have been observed with non-presealed methods.16
Case Presentation
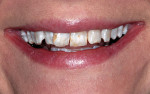
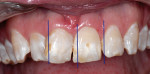
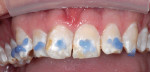
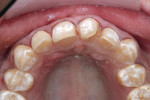
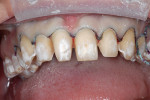
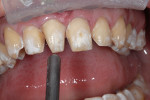
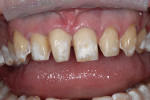
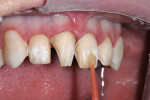
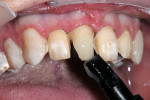
A woman with crowding, non-esthetic tooth coloration, and interproximal decay presented to the office wanting a more pleasing smile (Figure 1). There were both opaque white and light brown areas as well as decay between her incisors (Figure 2). Of particular concern was the right anterior area because of the overlap of teeth Nos. 9 through 11. The patient declined orthodontics. The midline was 3 mm to the right with a cant and the rotation of tooth No. 8 caused its distal aspect to protrude out of the arch. The accepted treatment plan was to place porcelain veneers on teeth Nos. 5 through 12 with composite bonding on the second bicuspids and molars.
The Direct Mock-up and Tooth Preparation
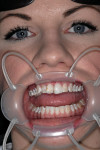
A direct composite mock-up was done before anesthesia so that incisal edge position, phonetics, and esthetics could be evaluated. Those changes were captured with photographs and an impression for laboratory consultation. A mock-up is critical for fabrication of the temporaries, to serve as a guide in tooth reduction and preparation, to evaluate esthetics and phonetics, and to give the patient a preview of the desired treatment.17
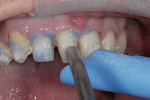
The work-up photographs were studied and marked to use as a “blueprint” during the mock-up and preparation (Figure 3). The teeth were spot-etched, bonding agent was applied, and composite was added before anesthesia providing a mock-up to check tooth proportions, phonetics, esthetics, and a color preview (Figure 4).17 Composite was added to tooth No. 9 first and the patient sat up to check the midline position and cant before proceeding (Figure 5). The remainder of the composite was added, length and incisal edges were verified, and the preliminary color was approved by the patient.
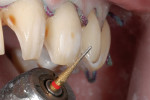
Tooth reduction was performed with a medium-grit finishing diamond (Diatech, Inc., www.diatechusa.com). The mock-up was removed and the enamel was prepared starting with tooth No. 9. All of the teeth were reduced in an “ideal” form in a three-plane, rounded preparation beveled toward the facial to allow for incisal characterization by the laboratory and a definitive stop when seating (Figure 6).18 The interproximal areas were prepared to compensate for the midline discrepancies and to cover areas of decay. Decay was removed, the defects were repaired with composite, and cord was placed (Figure 7).
Transitional Restorations
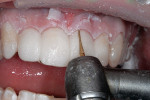
The materials needed for IDS are etch, DBA, and a separating medium. The teeth were first isolated with retraction and cord (Figure 8) and the entire prepared surface was etched with 32% phosphoric acid for 10 to 15 seconds and rinsed thoroughly (Figure 9). Two coats of DBA (ALL-BOND 3®, Bisco, Inc.) were applied and blown with air to ensure a thin, even layer of bonding resin (Figure 10). The DBA was light-cured for 20 seconds per tooth. It is important to remove the air-inhibited layer by wiping with gauze moistened with ethyl alcohol and/or microbrushes followed by a thorough rinsing. The removal of this surface layer is to ensure the complete set of the impression material and to decrease the chance of adherence of the composite temporary material.
After impressions, bite registration, and preparation shades, two coats of separating medium (PRO-V COAT) were applied with a brush and air-thinned. The material should be generously applied so that the surface is shiny (Figure 11). A self-curing composite temporary material (Luxatemp®, DMG America, www.dmg-america.com) was chosen in a color near to what the patient wanted in the final restorations, placed in the matrix onto the teeth, and trimmed with a finishing diamond (Figure 12). All records were sent to the laboratory, including patient feedback from the transitional veneers 4 days after placement.19
Insertion Appointment
The transitional restorations on the four incisors were scored with a finishing diamond, torque was applied with a metal instrument, and they were easily removed (Figure 13). The surface was then cleaned with pumice and an alcohol wipe to remove all debris. After try-in of the veneers and the fit was verified, the porcelain was shaken in an ultrasonic bath with ethyl alcohol, silanated, and a hema-free bonding agent was applied (CHOICE™ 2 veneer kit, Bisco, Inc.).
The entire tooth surface was etched with 32% phosphoric acid, rinsed, and DBA (ONE-STEP®, Bisco, Inc.) was applied per the manufacturer’s instructions (Figure 14). The luting composite was place directly on the tooth and the veneers were then placed and tacked for 3 seconds with a mini light-curing tip (Figure 15). The remainder of the cement was cleaned up and the entire surface was cured for 40 seconds with a large curing-light tip. The temporaries were then removed on the cuspids and bicuspids and the insertion procedure was performed in the same manner as the incisors.
Treatment of IDS-treated teeth during veneer insertion includes these steps:
- Pumice, roughen with fine diamond, or light aluminum-oxide sand blasting.
- Control tissue fluid with cord or retraction paste.
- Etch the entire surface.
- Apply DBA, air-thin, no cure.
- Apply light-cure luting material, seat veneers.
- Finish with usual techniques.
Conclusion
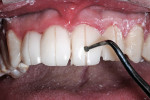
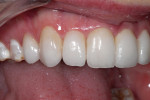
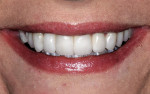
At 12-months postoperative, the soft tissue acceptance to the restorations was very good with resolution of crowding (Figure 16). The goals of the case were met with improvement in tooth proportions, color, and the position of teeth within the arch. Preoperative planning helped ensure proper tooth preparation to help meet the case objectives. The tooth proportions and interarch positions were corrected as desired (Figure 17).
Achieving patient satisfaction while maintaining physiology principles are key to a successful treatment outcome. IDS provides consistent results with almost no problems with sensitivity or microleakage. Sealing fresh dentin provides a maximum bond to the tooth while a suitable separating medium reduces the anxiety associated with removal of the temporaries or subsequent bond of the porcelain to the tooth. The results are restorations that are bonded tenaciously to the teeth while increasing office efficiency and an excellent patient experience (Figure 18).
Acknowledgment
The author would like to thank Mr. Adrium Jurim at Jurim Dental Studio for his excellent esthetic work and for understanding the principles of smile design.
References
1. Swift EJ Jr, Friedman MJ. Porcelain veneer outcomes, part II. J Esthet Restor Dent. 2006;18(2):110-113.
2. Tipton, PA. Aesthetic tooth alignment using etched porcelain restorations. Pract Proced Aesthet Dent. 2001;13(7):551-558.
3. Dumfahrt H. Porcelain laminate veneers. A retrospective evaluation after 1 to 10 years of service: Part 1 – Clinical procedure. Int J Prosthodont. 1999;12(6):505-513.
4. Peumans M, Van Meerbeek B, Lambrechts P, et al. Porcelain veneers: a review of the literature.J Dent. 2000;28(3):163-177.
5. Bassett JL. Replacement of missing mandibular lateral incisors with a single pontic all-ceramic prosthesis: a case report. Pract Peridodontics Aesthet Dent. 1997;9(4):455-461.
6. Cohen RG, Razzano MV. Immediate dentin sealing using an anti-bacterial self-etching bonding system. Pract Proced Aesthetic Dent. 2006;18(9):561-566.
7. Lee JI, Park SH. The effect of three variables on shear bond strength when luting a resin inlay to dentin. Oper Dent. 2009;34(3):288-292.
8. Magne P, Kim TH, Cascione D, et al. Immediate dentin sealing improves bond strength of indirect restorations. J Prosthet Dent. 2005;94(6):511-519.
9. Duarte S Jr, de Freitas CR, Saad JR, et al. The effect of immediate dentin sealing on the marginal adaptation and bond strengths of total-etch and self-etch adhesives. J Prosthet Dent. 2009;102(1):1-9.
10. Magne P. Immediate dentin sealing: a fundamental procedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17(3):144-154.
11. Pashley EL, Comer RW, Simpson MD, et al. Dentin permeability: sealing the dentin in crown preparations. Oper Dent. 1992;17(1):13-20.
12. Stavridakis MM, Krejci I, Magne P. Immediate dentin sealing of onlay preparations: thickness of pre-cured Dentin Bonding Agent and effect of surface cleaning. Oper Dent. 2005;30(6):747-757.
13. Papacchini F, Dall’Oca S, Chieffi N, et al. Composite-to-composite microtensile bond strength in the repair of a microfilled hybrid resin: effect of surface treatment and oxygen inhibition. J Adhes Dent. 2007;9(1):25-31.
14. PRO-V Coat Material Safety Data Sheet. Available at: https://bisco.com/instructions/Pro-V%20Coat%20MSDS.pdf. Accessed June 18, 2011.