SDF for Managing Open Gingival Floor Margins in Class II Restorations
Saturation with SDF may be a viable treatment option to attenuate the progression of caries
Theodore P. Croll, DDS | Joel H. Berg, DDS, MS | Gordon J. Christensen, DDS, MSD, PhD, ScD
Silver diammine fluoride (SDF) was developed in Japan a half century ago, and since then, it has been used in many parts of the world to attenuate dental caries infections.1,2 Since 2000, clinical interest and research regarding SDF has increased greatly, and in 2015, the material was granted FDA approval for treatment of tooth sensitivity. Off-label use followed, and now, modern dentistry publications are filled with commercial, clinical, and research articles about possible applications of SDF.3-12 Pubmed searches for the terms "silver diammine fluoride" (the correct spelling), "silver diamine fluoride," and "SDF" resulted in 36, 300, and 7,081 results, respectively, demonstrating the large body of research that has been conducted regarding its use.
In 2018, the Gordon J. Christensen Clinicians Report published two articles relevant to the treatment presented in the following case. The first revealed the bacteriological status of caries lesions treated with a certain regimen involving exposure to a 38% SDF solution,13 and the second addressed the epidemic of cervical caries in Class II resin box forms.14 The latter article reviews the causes of marginal openings at the gingival floor of Class II resin-based composite restorations and discusses a number of methods to help prevent such marginal voids. Although further research is necessary for clinical validation, this case report proposes SDF treatment as a possible solution to the problem of open margins rather than replacing the restoration.
Case Report
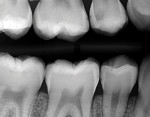
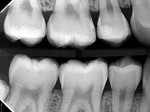
A teenage patient with deficient flossing habits exhibited radiographic evidence of a caries lesion on the distal aspect of his maxillary right second premolar (ie, tooth No. 4) as well as several interproximal radiolucencies indicative of beginning caries lesions (Figure 1). Tooth No. 4 received a Class II restoration with a resin-based composite material, and all of the posterior contacting proximating tooth surfaces were treated with soft dental pick insertion of 38% SDF followed by a fluoride varnish.15
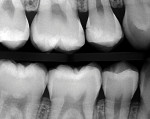
Six months later, the patient returned for a routine preventive dentistry appointment, and the maxillary second premolar disto-occlusal restoration was seen to have a small open margin on the gingival floor (Figure 2). The decision was made to perform a second SDF/varnish application to follow the initial treatment rendered 6 months prior.15 The thought was that the new SDF application would saturate the marginal opening at the gingival floor of the restoration and not only intercept potential bacterial proliferation, but also saturate the peripheral enamel to remineralize those surfaces and protect against continuing intraoral acid challenges.16
Treatment
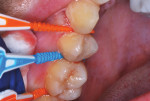
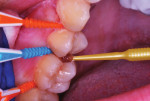
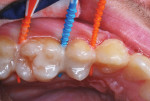
After a rubber cup and pumice were used to clean the maxillary right posterior teeth, the teeth were flossed, and each surface of the contacting molars and premolars was air dried, suitable soft dental picks were dipped in a 38% SDF solution and inserted interproximally (Figure 3).15 At some of the sites, a bit of blood resulted from the flossing, so that was absorbed into a cotton swab, and water and air spray were used to clear the area before insertion of the SDF-soaked tips. While the dental picks remained in place, a small brush applicator was used to paint SDF along each sluiceway, ensuring complete coverage with the SDF liquid as it spread by capillary action (Figure 4). The dental picks were then moved in an out several times at each site in order to further ensure complete coverage by the liquid. After 60 seconds, the entire working field was painted with 5% fluoride varnish (Figure 5). A 2.5% fluoride varnish can also be used for this step as an alternative. Next, the mandibular posterior teeth and the distal surfaces of the canine teeth were treated in the same manner (The patient's first premolars had been extracted years ago for orthodontic purposes). A 2" x 2" cotton gauze was then placed between the teeth, and the patient was asked to bite down on it for several minutes. Before being dismissed, the need for daily flossing was re-emphasized to the patient, and a proper flossing technique was demonstrated. In addition, dramatic photographs of the results of not flossing were shared as part of the educational process.17
Discussion
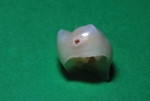
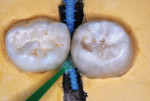
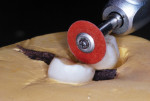
A demonstration performed with extracted teeth that showed how SDF delivered interproximally by a soft dental pick can saturate a proximal tooth surface caries lesion was previously reported by Croll and Berg.15 Using an exfoliated primary molar that had a proximal surface caries lesion (Figure 6) with an adjacent contacting extracted third molar positioned in dental stone, this experimental model was used to simulate soft dental pick insertion of SDF in the mouth (Figure 7). Discing the carious tooth surface after the third molar was cut away revealed SDF saturation to a depth of 1 to 2 mm in the primary tooth (Figure 8 and Figure 9), which demonstrates that SDF does indeed penetrate the proximal surface caries lesion using this treatment protocol. When considering this result, it is logical that an open margin at the gingival floor of a Class II resin-based composite restoration would also be saturated with the SDF fluid during this treatment regimen. Additional soaking of the surface at certain intervals, such as during 6-month recall appointments, could continue to guard against subsequent caries progression. Longitudinal bitewing comparisons will be needed to determine if the SDF intervention has been successful. This concept is in need of research to prove its efficacy, and an in vitro experiment using an artificial caries model or a carefully planned in vivo longitudinal study could elucidate its value.
Fluoride varnish coverage of the treatment field provides all of the enamel surfaces with the topical benefit of exposure to concentrated fluoride; however, the thixotropic consistency and "staying power" of the varnish also blankets the region for minutes after treatment, which may prevent salivary dilution of the SDF. This effect may allow more time for the undisturbed saturation and penetration of the SDF liquid into the caries lesion, but it too requires experimental confirmation.
Figure 1 and Figure 2 show a side-by-side bitewing comparison of the patient's initial status and his status 6 months after the repair of the premolar and the first SDF application to all posterior proximal tooth surfaces. When compared with the initial radiograph, the 6-month follow-up bitewing film demonstrates that the radiolucencies have either remained the same or improved with one exception. The distal surface radiolucency on the mandibular right first molar appears to have slightly advanced. Another bitewing radiograph, which was recorded 13 months after the premolar restoration and the original SDF applications, arguably shows insignificant progression of the proximal radiolucencies and, in several areas, perhaps evidence of some remineralization (Figure 10).
One fact about interproximal soft dental pick delivery of 38% SDF fluid must be emphasized. Such chemical interception of the caries process will not achieve long-term success unless food debris and bacterial plaque accumulation are disrupted and cleared away by brushing and careful flossing on a daily basis. This fact must be emphasized to the patient and parent. Continued fluoride exposure by fluoridated dentifrices and rinses can also augment the treatment to protect enamel surfaces from constant intraoral acid challenges. For certain patients, ongoing soft dental pick delivery of SDF at 6-month recall appointments should be considered.
Acknowledgement
Figures 5 through 8 were republished with permission from: Croll TP, Berg JH. Delivery methods of silver diammine fluoride to contacting proximal tooth surfaces and history of silver in dentistry. Compend Contin Educ Dent. 2020;41(2):84-90.
References
1. Nishino M. Studies on the topical application of ammoniacal silver fluoride for the arrest of dental caries [in Japanese]. Osaka Daigaku Shigaku Zasshi. 1969;14(1):1-14.
2. Yamaga R, Nishino M, Yoshida S, Yokomizo I. Diammine silver fluoride and its clinical application. J Osaka Univ Dent Sch. 1972;12:1-20.
3. Llodra JC, Rodriguez A, Ferrer B, et al. Efficacy of silver diamine fluoride for caries reduction in primary teeth and first permanent molars of schoolchildren: 36-month clinical trial. J Dent Res. 2005;84(8):721-724.
4. Yee R, Holmgren C, Mulder J, et al. Efficacy of silver diamine fluoride for arresting caries treatment. J Dent Res. 2009;88(7):644-647.
5. Mei ML, Lo EC, Chu CH. Clinical use of silver diamine fluoride in dental treatment. Compend Contin Educ Dent. 2016;37(2):93-98.
6. Gao SS, Zhao IS, Hiraishi N, et al. Clinical trials of silver diamine fluoride in arresting caries among children: a systematic review. JDR Clin Trans Res. 2016;1(3):201-210.
7. Crystal YO, Niederman RN. Silver diamine fluoride treatment considerations in children's caries management. Pediatr Dent. 2016;38(7):466-471.
8. Crystal YO, Marghalani AA, Ureles SD, et al. Use of silver diamine fluoride for dental caries management in children and adolescents, including those with special health care needs. Pediatr Dent. 2017;39(5):135-145.
9. Burgess JO, Vaghela PM. Silver diamine fluoride: a successful anticarious solution with limits. Adv Dent Res. 2018;29(1):131-134.
10. Zhao IS, Gao SS, Hiraishi N, et al. Mechanisms of silver diamine fluoride on arresting caries: a literature review. Int Dent J. 2018;68:67-76.
11 Crystal YO, Niederman R. Evidence-based dentistry update on silver diamine fluoride. Dent Clin North Am. 2019;63(1):45-68.
12. Christensen R. Focus On: Silver diamine fluoride. Dentistry Today. 2017;36(2):18.
13. Clinicians Report Foundation. 38% silver diamine fluoride (SDF): does it arrest dental caries lesion progression? Clinicians Report. 2018;11(1):1-3.
14. Clinicians Report Foundation. The epidemic of cervical caries in Class II resin box forms. Clinicians Report. 2018;11(6).
15. Croll TP, Berg JH. Delivery methods of silver diammine fluoride to contacting proximal tooth surfaces and history of silver in dentistry. Compend Contin Educ Dent. 2020;41(2):84-90.
16. Horst JA, Heima M. Prevention of dental caries by silver diamine fluoride. Compend Contin Educ Dent. 2019;40(3):158-163.
17. Croll TP. The Grossest, Truly Terrifying, But Utterly Awesome Mouth Book. Greenville, NC: PRACTICON, Inc.; 2020:8, 12, 13, 22-25, 32, 33.