Atraumatic Tissue Management for a Perfect Impression
Techniques and guidelines
Gildo Coelho Santos Jr, DDS, MSc, PhD | Leendert Boksman DDS, BSc, FADI, FICD | Maria Jacinta Moraes Coelho Santos, DDS, MSc, PhD
The atraumatic management of gingival tissues when making an impression is one of the most challenging aspects of crown-and-bridge. Tissue management includes the necessary movement of the gingival tissues away from the preparation margins so that they can be accurately impressed, as well as the management of vascular hemostasis when the gingival tissues are susceptible to bleeding.1,2 Whether the impression is made with a conventional impression material or by a digital impression technique, the rationale for and methodology of tissue management is a critical aspect of impression making; all tooth preparation margins must be totally captured in the impression to assure an excellent marginal fit of a laboratory-fabricated restoration.1,3
The aim of the present article is to discuss materials, techniques, and guidelines to promote atraumatic tissue management leading to a perfect impression. It includes a rational step-by-step description of the “double cord” gingival displacement method associated with a one-step/double-mix impression technique.
Tissue Management Materials
The gingival crevice is normally only about 2 mm in depth and must be treated with caution. Any technique used to expose the tooth margins and control bleeding and moisture must be conservative and atraumatic in order to avoid detachment of the tissue from the tooth or causing either mechanical or chemical injury to the tissue, which might result in permanent tissue recession.
To obtain a low-trauma, non-permanent gingival displacement, great importance must be given to the choice of products used and the technique employed. Frequently, the materials used for gingival retraction can be used alone or in combination with other materials and techniques.
Among the different techniques proposed in the literature, the retraction cord procedure seems to be less traumatic than electrosurgery4 or rotative gingival curettage,5 and it lowers the risk of gingival recession caused by the impression.
Gingival retraction cords can be knitted, woven, braided, or twisted in a variety of configurations to accommodate various thicknesses and diameters. Knitted cords, when placed in the gingival sulcus, expand post insertion, thus producing the physical effect of enlarging the sulcus by mechanical displacement, creating access for impressions. Examples of knitted cords are UltraPack® CleanCut (Ultradent Products, Inc., www.ultradent.com) and Re-Cord (Clinician’s Choice, www.clinicianschoice.com).
There is a variety of currently available chemical solutions and gels that have been recommended for use with gingival retraction cords because of their ability to act as an astringent or hemostatic agent.1,2 In most cases, these drugs are both an astringent—causing a transient ischemic contraction, thereby shrinking the gingival tissue—and a hemostatic, which creates blood vessel coagulation. When these reagents are placed on a retraction cord, the result is both a chemical and mechanical retraction of the gingival tissues and hemostasis, constricting blood flow through coagulation.
A 20% to 25% aluminum-chloride solution (Hemodent®, Premier Dental www.premusa.com), a 25% aluminum-chloride gel (ViscoStat Clear, Ultradent), a 25% aluminum-sulfate gel (Tissue Goo, Clinician’s Choice), and a 15.5% to 20% ferric-sulfate gel (ViscoStat, Ultradent) are among the most popularly used chemical reagents. They cause minimal tissue damage when used within the gingival sulcus for durations of less than 10 minutes.1,2,6 Epinephrine-impregnated retraction cords are not recommended because they can induce local necrosis and systemic effects.7 In fact, it has been previously shown that no discernible clinical benefit in gingival retraction could be recognized between an epinephrine-containing cord and other cords.8
Tissue-Management Techniques
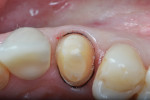
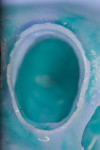
The insertion of two different retraction cords of different diameters, which are adapted to the variable morphology of the sulcus, is suggested. The first thinner cord, the compression cord (#000), is applied deep in the sulcus around each preparation with light pressure and without overlapping (Figure 1). The aim of this cord is to “seal” the sulcus and to avoid contamination of the margins by blood or crevicular fluid, and it is maintained in place during application of the impression material. This cord should be pre-moistened with water and squeezed to artificially reduce its volume to facilitate insertion and avoid tissue damage. If the cord is inserted dry, it will attach to the intrasulcular epithelium, and, if pulled back while packing, may cause bleeding.
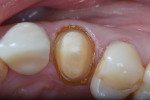
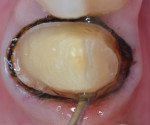
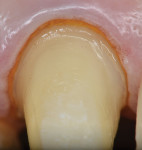
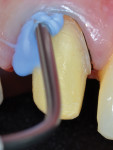
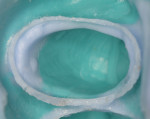
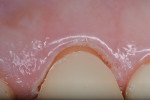
The second wide-diameter cord, the deflection cord (most frequently #00), is then soaked in an astringent/hemostatic solution such as Hemodent (aluminum-chloride solution), Astringedent (aluminum-chloride gel), or Tissue Goo (aluminum-sulfate gel) and inserted in the entrance of the sulcus to achieve tissue displacement (Figure 2 and Figure 3). Again, these solutions act as a lubricant during cord placement. Both the first and second cords will expand after placement, causing a mechanical displacement of the soft tissue. Ideally, the cord should remain in place for about 5 minutes to achieve the optimum tissue displacement. The astringent or hemostatic agent will complement the retraction because transient ischemia shrinks the gingival tissue (Figure 4). Again, the hemostatic agent needs about 5 minutes to promote the chemical retraction of the soft tissue, which helps the dentist to achieve a perfect impression (Figure 5).
The selection of the second cord size is based on the depth of the sulcus and soft-tissue type. In general, when there is minimal sulcus depth, the clinician is limited in many cases to placing only a single cord. A thin and delicate gingiva needs to be treated with small retraction cords in order to avoid permanent retraction. A thick gingiva needs a larger-size cord in order to achieve best displacement. In general, the second cord needs to be visible after packing (Figure 4). If it “disappears” inside the sulcus, a larger size should be considered. The bottom line is that the second cord must be small enough to allow an atraumatic placement and large enough to promote a perfect impression with clear margins (Figure 5).
After 5 minutes, the hemostatic agent is rinsed, and the second cord is removed, keeping in mind that the retraction is maintained for only 30 seconds.l During this time, one should inject the light-body vinyl polysiloxane (VPS) material (Figure 6) while the assistant finishes loading the impression tray with the heavy-body VPS impression material. To obtain a perfect impression without distortion, the operator needs to wait until the tray is (almost) fully loaded with the heavy-body material before removing the second cord and starting to inject the light-body material around the preparation. This will prevent distortion caused by premature setting of the light-body VPS material due to an early exposure to mouth temperature, which promotes a faster setting of the material. Following these steps will lead to a perfect impression, one with no voids, no pulls at the margins, and no distortions (Figure 7).
It is important for the clinician to remove the first retraction cord from the gingival sulcus as soon as possible after the impression is taken to minimize the risk of potential soft-tissue damage. Leaving a cord in the sulcus over a long period of time can cause inflammation, comparable to experimental ligament-induced periodontitis.9 In this type of clinical situation, a major gingival recession could occur, making the reconstruction margin of the restoration visible.
Tissue Management Maintenance
To avoid long-term inflammation, it is important to protect the soft tissue against external irritants, such as plaque accumulation caused by provisional restorations with open margins, or sharp and irritating edges that were not properly trimmed and polished.
As mentioned before, after the impression procedure is finished, a provisional restoration should be fabricated with perfect contour and margins that are well adapted to the tooth (Figure 8). One predictable way to deliver a high-quality provisional is to use a high-definition temporary matrix material, such as a silicone matrix Template (Clinicians Choice) to copy the diagnostic wax-up or original tooth. This material sets in 30 seconds, and its fluid viscosity allows it to flow into the embrasure areas, capturing details to prevent/reduce the amount of interproximal flash. Different techniques have been proposed including alginate impressions, suck-down plastic trays, VPS bite registration materials, or putty. These techniques will not deliver an effortless high-quality provisional due to their lack of detail, and the dentist will spend an inordinate amount of time producing an adequate temporary restoration.
Special attention should also be given to the quality of the provisional restorative material. One of the most popularly used temporary materials is the bis-acryl temporary composite. Examples of bis-acryl composites are: Protemp™ Plus (3M, www.3m.com), Inspire (Clinicians Choice), MirrorImage (Cosmedent, www.cosmedent.com), Expertemp (Ultradent), Integrity® (DENTSPLY, www.dentsply.com), and Luxatemp (DMG America, www.dmg-america.com). Mechanical properties, such as flexural and compressive strength, are important when selecting the temporary material in order to have a strong temporary restoration that will not fracture, especially at the margins. Another important property is low polymerization shrinkage. This will prevent missing margins, reducing the time spent when fabricating the provisional restoration. Polymerization shrinkage occurs toward the greatest mass, usually producing an open gingival margin. If needed, re-capitulating the margin with a flowable resin composite decreases the size of the gap and decreases temporary cement washout, thereby creating a healthier tissue at insertion.
Finally, a precise adaptation of the provisional restoration not only guarantees the gingival health during the period of time that the crowns are being manufactured at the lab, but also improves the quality of the cementation procedure at the delivery session due to the maintenance of healthy soft tissue (Figure 9).
Conclusion
The quality of final impressions plays a major role in the success of the prosthetic rehabilitation. The integrity of soft tissues must be preserved during the entire treatment, from the subgingival placement of crown margins, the impression phase, and cementation. For this reason, the gingival displacement must be carried out carefully and atraumatically. After that, the soft tissue should be protected with a temporary restoration that presents perfect margins and contour, and that is cemented with a temporary cement that is kind to tissues and does not wash out prematurely.
Disclosure
The authors have no relevant financial relationships to disclose.
References
1. Rosenstiel SF. Tissue management and impression making. In: Rosenstiel SF, Land MF, Fujimoto J, eds. Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby-Elsevier; 2006:431-465.
2. Morgano SM, Malone WF, Gregoire SE, Goldenberg BS. Tissue management with dental impression materials. Am J Dent. 1989;2(5):279-284.
3. Wöstmann B, Rehmann P, Trost D, Balkenhol M. Effect of different retraction and impression techniques on marginal fit of crowns. J Dent. 2008;36(7):508-512.
4. Ruel J, Schuessler PJ, Malament K, Mori D. Effects of retraction procedures on the periodontium in humans. J Prosthet Dent. 1981;45(4):458-460.
5. Azzi R, Tsao TF, Carranza FA Jr, Kenney EB. Comparative study of gingival retraction methods. J Prosthet Dent. 1983;50(4):561-565.
6. Akca EA, Yildirim E, Dalkiz M, et al. Effects of different retraction medicaments on gingival tissue. Quintessence Int. 2006;37(1):53-59.
7. Pelzner RB, Kempler D, Stark MM, et al. Human blood pressure and pulse rate response to racemic epinephrine retraction cord. J Prosthet Dent. 1978;39(3):287-292.
8. Jokstad A. Clinical trial of gingival retraction cords. J Prosthet Dent. 1999;81(3):258-261.
9. Lindhe J, Hamp S, Löe H. Experimental periodontitis in the beagle dog. J Periodontal Res. 1973;8(1):1-10.
About the Authors
Gildo Coelho Santos Jr, DDS, MSc, PhD
Associate Professor and Chair of the Division of Restorative Dentistry
Schulich School of Medicine & Dentistry
University of Western Ontario
London, Ontario, Canada
Leendert Boksman DDS, BSc, FADI, FICD
Adjunct Professor in Division of Restorative Dentistry
Schulich School of Medicine & Dentistry
University of Western Ontario
London, Ontario, Canada
Maria Jacinta Moraes Coelho Santos, DDS,MSc, PhD
Associate Professor in Division of Restorative Dentistry
Schulich School of Medicine & Dentistry
University of Western Ontario
London, Ontario, Canada