Periodontal Plastic Surgery in the Esthetic Zone
A cooperative approach to excellent esthetics and optimal function
If the patient is left with an esthetic problem, the outcome of dental care, whether periodontal, prosthodontic, orthodontic, or a combination of these, is unacceptable.1 Many clinicians have agreed that merely saving teeth is no longer an ultimate goal for periodontal therapy, especially in the maxillary anterior region (ie, the “esthetic zone”).1-6 Patients want individualized and predictable dental care that will also successfully address esthetic outcomes.
This article presents a case of periodontal care that not only enhanced the esthetic appearance of a maxillary central incisor (tooth No. 9) but also strengthened its periodontal support. The patient required a new crown for this tooth, which had a history of trauma but was otherwise asymptomatic and periodontally stable (ie, normal probing depths, no bleeding on probing). However, the patient was not happy with the bluish gingiva and the shade of his crown for this tooth, which had subgingival caries.
Case Presentation
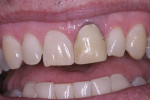
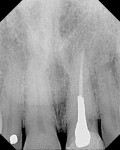
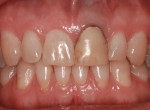
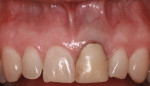
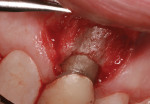
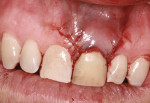
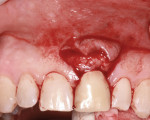
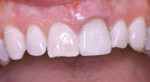
Subgingival caries was detected at the midfacial aspect of tooth No. 9 in this 45-year-old white man, who had received trauma to this tooth several years previously. The crown on tooth No. 9 needed to be replaced, but neither the restorative dentist nor the patient was happy with the look of the soft tissue, which appeared bluish. The patient requested correction of the dark tissue prior to placement of a new crown, as pink gingiva would enhance the esthetics (Figure 1 through Figure 4).
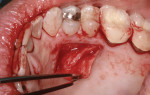
A vertical incision was made to gain access to the root and prepare the recipient site for grafting. A #15C blade (Carbon Steel, Benco Dental, www.benco.com) was used for the initial sulcular incision and placement of two vertical incisions on the mesial and distal aspects of tooth No. 9. The facial flap was extended apically beyond the mucogingival junction to facilitate full reflection and coronal advancement. Flap reflection enabled observation of paper-thin facial bone and a dark root that could be seen through the tissue (Figure 5). No attempt was made to perform bone grafting. The authors believed that the tooth No. 9 had sufficient bony support from the mesial, distal, and palatal aspects and the use of a subepithelial connective tissue graft (SCTG) alone could satisfy the patient’s esthetic complaint. To ensure a thick tissue specimen was obtained to help maintain adequate vascularity and prevent recession, the SCTG was harvested from the maxillary left palate in the canine/premolar region (Figure 6) and secured to the recipient site with single interrupted 5.0 Vicryl® sutures (polyglactin 910, P3, Ethicon, www.ethicon.com) (Figure 7). The facial flap was then coronally advanced to cover the SCTG and sutured with single interrupted 5.0 Vicryl sutures (Figure 8). This corrected the chief complaint and strengthened the supporting structure of tooth No. 9 for optimal health of the periodontium and the associated restoration.
After surgery, the patient was given amoxicillin orally (500 mg three times daily), ibuprofen (800 mg, three times daily as needed), methylprednisolone to control swelling (Medrol Dosepak, Pfizer, Inc., www.pfizer.com), and chlorhexidine rinse (Acclean®, chlorhexidine gluconate, 0.12% oral rinse USP, Henry Schein Dental, henryschein.com) twice daily. Placement of the graft corrected the color by making the tissue thicker and healthier (Figure 7 and Figure 8). The definitive crown was delivered 3 months later, and the results were evident (Figure 9). Both the patient and restorative dentist were pleased with the outcome.
Discussion
Gingival grafting has been performed for many years to correct various periodontal problems. Kina and colleagues7 used a free gingival graft (FGG) to restore biologic width in combined periodontal/prosthetic treatment. Harris3 encountered a patient previously treated with a FGG who required further periodontal plastic surgical treatment due to the unesthetic outcome. Hall and Lundergan8 used FGG as a predictable means of increasing the volume of attached gingiva but noted that it was unreliable for root coverage.
The aforementioned drawbacks of FGG have led to more frequent use of SCTG, which has become the treatment of choice for many situations. The dual supply of blood from the graft itself and the flap overlying it mean that healing is more predictable, and the esthetic outcome is better than with the FGG because the graft is covered with gingiva that is already present in the affected area. Many studies have documented the success of the SCTG for the correction of recession defects,9-14 ridge deficiencies,9,15 root coverage,16-19 and mucogingival reconstruction.17 Levine16 achieved 97.04% success in root coverage on 21 teeth that received SCTGs. Other dentists have modified the SCTG with a “tunnel envelope”; the additional blood supply beneath the graft assists in healing and incorporation of the graft.1,13,19
Tarnow20 originated the semilunar coronally advanced flap, which Hagighat modified in 200621; Pai and colleagues22 used Hagighat’s modified flap with great success to treat both single and multiple adjacent recession defects. Landsberg and Fuhrer23 used a coronally advanced flap/SCTG in conjunction with crown preparation, with a slight overcorrection to account for expected postsurgical recession of the gingiva after placement of the provisional crown. Cabrera17 added a labial extension to the SCTG for situations with a limited vestibule or excessive frenum pull. If an SCTG is not possible or a patient prefers more conservative treatment to restore the gingiva and enhance esthetics, prosthetic gingival tissue is an option, either temporarily or permanently.24,25
Pai and colleagues22 noted that “periodontal plastic surgery is defined by 1996 World Workshop in Clinical Periodontics as surgical procedures performed to correct or eliminate anatomic, developmental, or traumatic deformities of the gingiva.” Pasquinelli1 added that periodontal plastic surgery should restore or enhance the esthetic component of the tissues supporting and surrounding the teeth. He reviewed various periodontal plastic surgery procedures and demonstrated their use, noting the transformation of the periodontics discipline from mere disease treatment to a field that seeks esthetic solutions to curing diseases of the periodontium. In agreement with Pasquinelli, Ravon and colleagues5 stated that “the goal of periodontal therapy is not only to establish and maintain the dentition and the periodontium free of any oral infections, but also to provide an environment with optimal function and esthetics. Esthetics has become an integral portion of the overall treatment goal in periodontics.” Schunke and colleagues26 added that “esthetics and function—not only of the teeth—form an entity that needs to be viewed and treated as a whole.”
In the present case, a bluish hue of the gingiva was among the patient’s principal complaints. Depigmentation of tissues may signify a clinical problem, such as underlying hard tissue that is too thin to cover dark roots, as in the present case, or melanin coloring of the gingiva itself may cause it. In patients with excessive gingival display, this is unacceptable. In the present case, this was treated with SCTG, because the gingiva itself was not discolored, and grafting of thicker tissue into the area addressed the problem. Other authors have used electrosurgery, surgical abrasion, and lasers to eliminate discolored gingiva.27,28
In addition to esthetics becoming a greater concern for periodontists, interdisciplinary treatment has now become mandatory in many cases. Pasquinelli,1 in a review of periodontal plastic surgical techniques, emphasized that proper diagnosis and multidisciplinary treatment are essential if a predictable result is expected. Allen and Winter29 advised that clinicians set a plan first, with interdisciplinary cooperation, prior to beginning treatment, and they stressed that the choice of proper crown and gingival proportions should be decided by all team members. Anson30 combined periodontal and esthetic approaches to treat subgingival caries, noting that “the synergy developed by combining these two fields of dentistry allows for better esthetic outcomes for our patients.” Dersot,31 Mankoo and Frost,32 and Monnet-Corti and colleagues33 investigated the interactions between periodontal and orthodontic treatments with respect to ideal timing and sequence of procedures. There was agreement that periodontics and orthodontics can work well together to create ideal gingival profiles. Mankoo and Frost32 orthodontically extruded hopeless teeth prior to extraction and implant placement to improve hard- and soft-tissue profiles. Prosthodontic treatment, too, can assist the periodontist in obtaining an attractive outcome; either provisional or definitive restorations can be used to strengthen the underlying hard and soft tissues to enhance esthetics.4,7,34,35 Santamaria and colleagues36,37 applied resin-modified glass-ionomer restorations together with grafting and achieved significant gains in attachment levels and improvements of probing depths. Faiella38 emphasized the importance of interdisciplinary consultations to prevent treatment failure or unhappy patients: “The ability to counsel in an informed way—outside the restorative arena—allows dentists to demonstrate their true commitment to the best outcome for the person they are dedicated to serve, the patient.”
Conclusion
Periodontal treatment now takes into consideration the need for addressing esthetic issues. Clinicians who are well trained and experienced with these challenging procedures can make significant differences in the outcome in these cases. To meet patients’ demands and high expectations in the esthetic zone, clinicians should receive additional training and experience in handling technically demanding procedures that, in most cases, necessitate interdisciplinary treatment planning. A clearly explained treatment plan with a customized consent form should be presented to patients who desire quality work rather than an inexpensive and inadequate alternative.
“Team dentistry”—that is, close cooperation between professionals during diagnosis, planning, treatment, and follow-up execution—enables delivery of outstanding dentistry. “Many hands make light work”; therefore, we must work together for the benefit of everyone concerned.
Acknowledgment
The assistance of Jennifer P. Ballinger, ELS, in drafting this manuscript is gratefully acknowledged.
About the Authors
References
1. Pasquinelli LK. Periodontal plastic surgery as an adjunctive therapeutic modality for esthetic restorative dentistry. J Calif Dent Assoc. 2005;33(3):217-221.
2. Butler B, Kinzer GA. Managing esthetic implant complications. Compend Contin Educ Dent. 2012;33(7):514-188, 520-522.
3. Harris RJ. Treatment of a previously placed autogenous masticatory mucosa graft (free gingival graft). A case report. J Periodontol. 1998;69(6):717-723.
4. Polack MA, Mahn DH. Biotype change for the esthetic rehabilitation of the smile. J Esthet Restor Dent. 2013;25(3):177-186.
5. Ravon NA, Handelsman M, Levine D. Multidisciplinary care: periodontal aspects to treatment planning the anterior esthetic zone. J Calif Dent Assoc. 2008; 36(8):575-584.
6. Reddy MS. Achieving gingival esthetics. J Am Dent Assoc. 2003;134(3):295-304; quiz 337-338.
7. Kina JR, Dos Santos PH, Kina EF, et al. Periodontal and prosthetic biologic considerations to restore biological width in posterior teeth. J Craniofac Surg. 2011;22(5):1913-1916.
8. Hall WB, Lundergan WP. Free gingival grafts. Current indications and techniques. Dent Clin North Am. 1993;37(2):227-242.
9. Cohen ES. Ridge augmentation utilizing the subepithelial connective tissue graft: case reports. Pract Periodontics Aesthet Dent. 1994;6(2):47-53; quiz 55.
10. Kassab MM, Badawi H, Dentino AR. Treatment of gingival recession. Dent Clin North Am. 2010;54(1):129-140.
11. Martorelli de Lima AF, da Silva RC, Joly JC, Tatakis DN. Coronally positioned flap with subepithelial connective tissue graft for root coverage: various indications and flap designs. J Int Acad Periodontol. 2006;8(2):53-60.
12. Saadoun AP. Current trends in gingival recession coverage—part I: the tunnel connective tissue graft. Pract Proced Aesthet Dent. 2006;18(7):433-438; quiz 440.
13. Rossberg M, Eickholz P, Raetzke P, Ratka-Krüger P. Long-term results of root coverage with connective tissue in the envelope technique: a report of 20 cases. Int J Periodontics Restorative Dent. 2008;28(1):19-27.
14. Simon Z, Rosenblatt A. Challenges in achieving gingival harmony. J Calif Dent Assoc. 2010;38(8):583-590.
15. Sharma P, Hn DA, Kaur P, Dahiya V. Implant esthetic restoration in ridge deficiencies in cases of trauma—a case report. J Oral Implantol. 2011 Nov 21. [Epub ahead of print]
16. Levine RA. Covering denuded maxillary root surfaces with the subepithelial connective tissue graft. Compendium. 1991;12(8):568, 570, 572 passim.
17. Cabrera PO. The connective tissue graft with labial vestibular extension. Pract Periodontics Aesthet Dent. 1994;6(5):57-63.
18. Sedon CL, Breault LG, Covington LL, Bishop BG. The subepithelial connective tissue graft: part II. Histologic healing and clinical root coverage. J Contemp Dent Pract. 2005;6(2):139-150.
19. Tözüm TF. Root coverage with subepithelial connective tissue grafts and modified tunnel technique. An evaluation of long-term results. N Y State Dent J. 2006;72(4):38-41.
20. Tarnow DP. Semilunar coronally repositioned flap. J Clin Periodontol. 1986;13:182-185.
21. Haghighat K. Modified semilunar coronally advanced flap. J Periodontol. 2006;77:1274-1279.
22. Pai BS, Rajan SA, Padma R, et al. Modified semilunar coronally advanced flap: a case series. J Indian Soc Periodontol. 2013;17(1):124-127.
23. Landsberg C, Fuhrer N. “Crown-then-graft:” a novel approach to optimize teeth for crown placement and root coverage procedures. A 5-year case report. Eur J Esthet Dent. 2012;7(3):296-308.
24. Gopakumar A, Sood B. Conservative management of gingival recession: the gingival veneer. J Esthet Restor Dent. 2012;24(6):385-393. Epub 2012 May 7.
25. Ahmed F, MacLeod IK, Roberts A. Prosthetic rehabilitation of an individual papillary unit: a clinical report. Eur J Prosthodont Restor Dent. 2011;19(4):146-150.
26. Schunke S, Enssle A, Kreisl A, Schlee M. Teeth and posture. Eur J Esthet Dent. 2011;6(4):406-427.
27. Kasagani SK, Nutalapati R, Mutthineni RB. Esthetic depigmentation of anterior gingiva. A case series. N Y State Dent J. 2012;78(3):26-31.
28. Thangavelu A, Elavarasu S, Jayapalan P. Pink esthetics in periodontics - gingival depigmentation: a case series. J Pharm Bioallied Sci. 2012;4(suppl 2):S186-S190.
29. Allen EP, Winter RR. Interdisciplinary treatment of cervical lesions. Compend Contin Educ Dent. 2011;32(spec no 5):16-20.
30. Anson D. Periodontal esthetics and soft-tissue root coverage for treatment of cervical root caries. Compend Contin Educ Dent. 1999;20(11):1043-1046, 1048-1050, 1052; quiz 1054.
31. Dersot JM. Gingival recession and adult orthodontics: a clinical evidence-based treatment proposal. Int Orthod. 2012 Mar;10(1):29-42.. Epub 2012 Jan 17.
32. Mankoo T, Frost L. Rehabilitation of esthetics in advanced periodontal cases using orthodontics for vertical hard and soft tissue regeneration prior to implants - a report of 2 challenging cases treated with an interdisciplinary approach. Eur J Esthet Dent. 2011;6(4):376-404.
33. Monnet-Corti V, Barrin A, Goubron C. Reciprocal relationships between orthodontics and periodontics in esthetic treatments. Orthod Fr. 2012;83(2):131-142.
34. Le D, Hu WJ, Zhang H. Combined crown lengthening surgery with restorative therapy for inducing papilla growth: a case report. Beijing Da Xue Xue Bao. 2013;45(2):312-315.
35. Bitter RN. The periodontal factor in esthetic smile design—altering gingival display. Gen Dent. 2007;55(7):616-622.
36. Santamaria MP, Saito MT, Casati MZ, et al. Gingival recession associated with noncarious cervical lesions: combined periodontal-restorative approach and the treatment of long-term esthetic complications. Gen Dent. 2012;60(4):306-311.
37. Santamaría MP, Ambrosano GM, Casati MZ, et al. Connective tissue graft and resin glass ionomer for the treatment of gingival recession associated with noncarious cervical lesions: a case series. Int J Periodontics Restorative Dent. 2011;31(5):e57-e63.
38. Faiella RA. Periodontal plastic surgical indications in the restorative practice. J Mass Dent Soc. 2005;53(4):26-28