Choosing an Endodontic Post System
Making an informed decision about product design
When restoring severely broken down, endodontically treated teeth, the clinician is faced with a plethora of choices when post placement is indicated. An indirect, two-stage procedure has been extensively used in the past to create a custom-fitted post using cast gold or, more recently, to fabricate custom zirconia posts (dowels).
More often, for the sake of expediency, a direct one-step approach is used, with the choices available including stainless steel, nickel chromium, titanium, zirconia, carbon fiber, glass fiber, and quartz fiber posts. There are a myriad of shapes and configurations available, such as tapered, parallel, double taper, and parallel-tapered, with multiple choices available for the surface characteristics of the post, including smooth, spiral, notched, serrated (and combinations of these), or threaded and threaded split shank.
Because threaded posts gain retention by engaging the sides of the canal root dentin by means of their threads, they are classified as active posts. These must still be cemented or adhesively cemented into place to prevent microleakage and fill the voids that inevitably occur due to the shape of most canals (ovoid) and tapered pre- and post-endodontic instrumentation. Passive posts are so called because their retention is derived solely from regular cementation, luting, or adhesive cementation.
Making Treatment Choices
When assessing the relative merits, drawbacks, and challenges of the many available post systems, restorative clinicians must ask some basic questions:
• Does the endodontic post system allow for protecting and preserving the dentin that remains?
• Does it allow for integration of natural ovoid and tapered shapes into the restorative post process?
• If all canals are ovoid and tapered and a parallel post (threaded or not) is used, how does this affect the C-factor stresses of the composites used? Can the clinician modify the technique to minimize these stresses?
Relying on independent research will lead to an informed decision and help one avoid some of the erroneous concepts and claims that have been put forward.
Protecting and Preserving Dentin
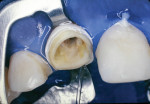
Multiple research studies have shown that the long-term survival of endodontically treated teeth is heavily influenced by the amount and preservation of dentin, with remaining coronal and radicular tooth structure affecting strength and resistance to root fracture.1-4 Endodontic protocols have shifted away from over-flaring access openings, which needlessly removed large amounts of internal dentin, leading to a structural weakening of the tooth5 (Figure 1).
The removal of radicular dentin,6,7 which is required when preparing a post space for parallel posts, and the removal of dentin in the coronal portion of the tooth to be restored8,9 change tooth biomechanics, re-enforcing the concept that a highly conservative approach is indicated.10-12 It has been shown that if one increases the size or diameter of a post, this does not greatly increase the retention of that post13,14; however, the potential exists for lateral root perforations, strip perforations (in the lateral root invaginations), excess root thinning, increased cervical stresses,15 and a decrease in resistance to tooth fracture, resulting in a higher incidence of failure15-17 (Figure 2).
Therefore, when restoring a tooth with a post, the canal must not be enlarged unnecessarily; the canal shape must be respected, and the post diameter minimized to preserve essential dentin and increase the ability of the tooth to resist fracture.18 Thus, the chosen post system must have a wide range of small sizes and an anatomical shape that will allow for the placement of a post with minimal dentin removal, especially apically, as well as be adaptable in the case of canals that have a non-round configuration. The system must allow for the simultaneous placement of multiple posts, accessory posts, or small auxiliary posts such as the Fibercone™ (RTD, www.rtddental.com) rather than over-preparing the root canal to fit a larger post.
Current threaded post systems do not facilitate this approach. Also, according to Ricketts and colleagues, clinicians should consider that “some post systems have root facers to flatten the root face to facilitate seating and stabilization of the post” and some posts require dentin removal for the placement of a flange, needlessly “removing more coronal tooth tissue that is available to create the ferrule effect.”19
Tapered and Ovoid Canals
Assuming that the focus of any post preparation is to maximize the amount of dentin remaining, clinicians must also accept the fact that parallel-sided posts pose a conceptual problem in relation to the natural contours of a canal. If the canal is tapered, there are only three choices in placing a parallel post:
• Do not prepare the canal and fit a small post that touches dentin at the apical end only and has no approximation to the flare of the dentin above that point.
• Prepare the canal and remove dentin so that the parallel post touches dentin part of the way towards the cervical but not at the top of the flare.
• Overly and excessively remove sound dentin, preparing the canal so that the parallel post touches the dentin all the way from the apical to the cervical.
In some post manufacturers’ ads, the parallel post always shows total adaptation to the dentin from the apex to the cervical region of the root canal preparation. Realistically, this can only be done by overpreparation and unnecessary sacrifice of sound tooth structure. Because rigid posts move the stresses towards the apical portion of the root, the last thing a clinician wants to do is to compromise the longevity of the final restoration by creating an irretrievable fracture and, if failure does occur, by overpreparing and removing the critical dentinal thickness at the apical portion of the post.20,21
Canal spaces are typically not round. More than 50% of lower incisors have a long oval form with the hazard of potential strip perforations.22 Premolars have an ovoid or ribbon shape, with 72.4% of maxillary first premolars having a deep mesial depression and 52.7% showing a distal side depression;23 in a study of 1181 teeth with cross sections, the number of cases with a long oval exceeded 50%.24 C-shaped canals are also seen regularly, dictating a minimal post width to preclude perforation.25
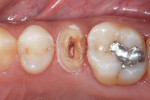
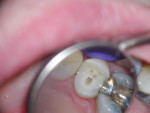
In a traditional approach, the more oval a canal is, the greater the discrepancy between it and the prefabricated post, requiring a technique that either removes sound tooth structure or yields a post not adapted to the canal.26 Therefore, if the “traditional approach” is contraindicated, the authors suggest using a nontraditional or augmented approach in which a tapered fiber “master post” is inserted where appropriate in the largest portion of the canal and in the flanges or irregular spaces of the access opening—where all the gutta-percha must be removed (round twist drills leave it in these areas, leading to failure) (Figure 3)—and secondary smaller tapered fiber posts or “auxiliary” Fibercones are inserted (Figure 4). This approach is much like how clinicians use a master gutta-percha point and auxiliary gutta-percha points when filling an endodontically treated canal.27
This technique also increases anti-rotational resistance, allows for an increase in composite conversion in the canal, and decreases the internal C-factor contraction vectors associated with composite polymerization, as discussed below. Of course, parallel and threaded posts, whether metal or fiber, do not allow for this passive, nontraditional, conservative approach.
C-Factor Polymerization Contraction Stresses
During the polymerization of a resin composite dental material, the volume of monomers is reduced, creating shrinkage stresses. As the thickness of the material is reduced, the volumetric shrinkage is reduced, which results in a reduction of the shrinkage stress.
Microleakage, recurrent caries, marginal discoloration, debonding, and sensitivity have been but a few of the consequences of using self-, dual-, or light-cured composite resins. C-factor is recognized as the ratio of bonded surfaces to nonbonded surfaces in cavity preparations, and this number is related to how the composite reacts within that cavity configuration.28 In a prepared canal space, there are no unbound surfaces upon the insertion of a post with a composite resin cement. Therefore, C-factor stresses are highest with post cementation,29 in which all surfaces involved competing against each other, resulting in C-factor estimates of 200 to infinity.30
Porciani and colleagues state, “One of the main reasons for failure by way of debonding of post restorations is due to the presence of an excessive amount of cement, especially at the coronal level, and a thin and uniform cement layer between the post and canal walls can only be achieved with a good fitting post with knowledge of the anatomy, which is a decisive factor during fiber post luting procedures.”31 By using an anatomically complementary post system that minimizes the lateral amount of cement (tapered) and by effectively using the augmented fiber post approach, the amount of composite is minimized, thereby minimizing the C-factor configuration stresses.
Threaded Post Stress Factors
The American Dental Association (ADA) Council on Scientific Affairs has taken the position that active threaded posts are well-retained but introduce stress to the tooth, and are therefore associated with increased risk of root fracture.32 Similarly, it states that because of these drawbacks, participants in the ADA’s expert panel discussion on endodontic posts opted for passive posts. What does the independent literature say about threaded posts in general and the split shank in particular?
Musikant said that split-shank designs are notable for a reduction in insertional stress resulting from “the threads on a split-shank parallel-threaded post distribute [stresses] evenly over the entire working length.”33
Peutzfledt and colleagues, in a survey of failed post-retained restorations, stated, “The superior retention of threaded posts obtained by engaging in dentin, simultaneously is accompanied by increased stress formation within the root and thus by an increased risk of root fracture.”34 The tapered Surtex® (Dentatus, www.dentatususa.com) post has been reported to increase the risk for failure;44 similarly, the Radix-Anker (DENTSPLY International, www.dentsply.com) shows very high apical stresses when engaging the bottom of the prepared channel.36 The introduction of high stresses and the higher failure rate of threaded posts has been reported in many studies.19,37-41 It has been suggested that practitioners take steps to decrease the high stress levels by counter-rotation or “backing off”36 after seating the threaded post, even though “counter rotation cannot undo any crack formation that may have occurred during full engagement.”42
Ricketts and colleagues noted that although manufacturers claim that the collapsing nature of a split-shank post design reduces the stresses induced into the root, they are in fact active posts, and the introduction of stress is inevitable. “The coronal half of the post is not split and it is in this area that the highest strain has been recorded in the root,” they explained.19 High coronal stress with more evidence of coronal tooth fracture has also been found by Dhavavel.43
Burns and colleagues found that the split-shank post design recorded elevated shoulder stress at the countersink, created additional stresses during the tapping procedure, and displayed asymmetric patterns of stress distribution. Furthermore, stress concentrations were associated with each thread, and it demonstrated high shoulder stresses in both the static and loaded state.40 Inherent to split-shank post design is the fact that the slot provides minimal change in diameter44 and it “compresses into an ellipse, whose greatest width is almost equal to the original diameter.”45 Finally, one study that evaluated stresses at inclined loading found that the split-shank post showed significantly higher stress in the cervical and middle surfaces than any of the other posts studied.46
Summary
With active posts, the introduction of stress is inevitable, despite any claims manufacturers might make. The cumulative and additional negative effects of using high modulus of elasticity stainless steel and titanium in addition to threaded posts are discussed in the second part of this article, which will appear in the November 2013 issue of Inside Dentistry. This article addressed some of the questions every clinician should ask when restoring severely compromised, endodontically treated teeth. To help ensure long-term success, clinicians should carefully evaluate claims about endodontic post systems and choose from the many options available to meet the needs of individual cases.
Disclosures
Dr. Boksman does some writing, lecturing, and consulting for manufacturers, including Clinician’s Choice. Dr. Santos has received materials support from Clinician’s Choice. Dr. Friedman has no disclosures.
References
1. Pilo R, Shapenco E, Lewinstein I. Residual dentin thickness in bifurcated maxillary first premolars after root canal and post space preparation with parallel-sided drills. J Prosthet Dent. 2008;99(4):267-273.
2. Heydecke G, Butz F, Strub JR. Fracture strength and survival rate of endodontically treated maxillary incisors with approximal cavities after restoration with different post and core systems: an in-vitro study. J Dent. 2001;29(6):427-433.
3. Fernandes AS, Dessai GS. Factors affecting the fracture resistance of post-core reconstructed teeth: a review. Int J Prosthodont. 2001;14(4):355-363.
4. Baba NZ, Goodacre CJ, Daher T. Restoration of endodontically treated teeth: the seven keys to success. Gen Dent. 2009;57(6):596-603.
5. Kishen A. Mechanisms and risk factors for fracture predilection in endodontically treated teeth. Endodontic Topics. 2006;13(1):57-83.
6. Trope M, Ray HL Jr. Resistance to fracture of endodontically treated roots. Oral Surg Oral Med Oral Pathol. 1992;73(1):99-102.
7. Reeh ES, Messer HH, Douglas WH. Reduction in tooth stiffness as a result of endodontic and restorative procedures. J Endod. 1989;15(1):512-516.
8. Linn J, Messer HH. Effect of restorative procedures on the strength of endodontically treated molars. J Endod. 1994;20(10):479-485.
9. Pantivisai P, Messer HH. Cuspaldeflection in molars in relation to endodontic and restorative procedures. J Endod. 1995;21(2):51-61.
10. Dietschi D, Duc O, Krejci I, Sadan A. Biomechanical considerations for the restoration of endodontically treated teeth: a systematic review of the literature, Part II (Evaluation of fatigue behavior, interfaces, and invivo studies). Quintessence Int. 2009;39(2):117-129.
11. Creugers NH, Mentink AG, Fokkinga WA, Kreulen CM. 5-year follow-up of a prospective clinical study on various types of core restorations. Int J Prosthodont. 2005;18(1):34-39.
12. Torbjörner A, Fransson B. A literature review on the prosthetic treatment of structurally compromised teeth.Int J Prosthodont. 2004;17(3):369-376.
13. Krupp JD, Caputo AA, Trabert KC, Standlee JP. Dowel retention with glass-ionomer cement. J Prosthet Dent. 1979;41(2):163-166.
14. Standlee JP, Caputo AA, Hanson EC. Retention of endodontic dowels: effect of cement, dowel length, and design. J Prosthet Dent. 1978;39(4):400-405.
15. Trabert KC, Caputo AA, Abou-Rass M. Tooth fracture–a comparison of endodontic and restorative treatments. J Endod. 1978;4(11):341-345.
16. Trope M, Maltz DO, Tronstad L. Resistance to fracture of restored endodontically treated teeth. Endod Dent Traumatol. 1985;1(3):108-111.
17. Sorensen JA, Martinoff JT. Endodontically treated teeth as abutments. J Prosthet Dent. 1985;53(5):631-636.
18. Al-Omiri MK, Mahmoud AA, Rayyan MR, Abu-Hammad O. Fracture resistance of teeth restored with post-retained restorations: an overview. J Endod. 2010;36(9):1439-1449.
19. Ricketts DN, Tait CM, Higgins AJ. Post and core systems, refinements to tooth preparation and cementation. Br Dent J. 2005;198(9):533-541.
20. Dietschi D, Duc O, Krejci I, Sadan A. Biomechanical considerations for the restoration of endodontically treated teeth: a systematic review of the literature - Part I. Composition and micro- and macrostructure alterations. Quintessence Int. 2007;38(9):733-743.
21. FokkingaWA, Kreulen CM, Vallittu PK, Creugers NH. A structured analysis of in vitro failure loads and failure modes of fiber, metal, and ceramic post-and-core systems. Int J Prosthodont. 2004;17(4):476-482.
22. Shemesh H, vanSoest G, Wu MK, et al. The ability of optical coherence tomography to characterize the root canal walls. J Endod. 2007;33(11):1369-1373.
23. Pécora JD, Saquy PC, Soussa Neto MD, Woelfel JB. Root form and canal anatomy of maxillary first premolars. Braz Dent J. 1992;2(2):87-94.
24. Wu MK, R’oris A, Barkis D, Wesselink PR. Prevalence and extent of long oval canals in the apical third. Oral Surg Oral Med Oral Path Oral Radiol Endod. 2000;89(6):739-743.
25. Jafarzadeh H, Wu YN. The C-shaped root canal configuration: a review. J Endod. 2007;33(5):517-523.
26. Plotino G, Grande MN, Pameijer CH, Somma F. Influence of surface modelling using burs on the macro and micro surface morphology of anatomically formed fibre posts. Int Endod J. 2008;41(4):345-355.
27. Boksman L, Santos GC, Friedman M. Post preparations: the dichotomy of using rotary instrumentation in the treatment of ovoid canals: clinical solutions for long term success using combined bonded fiber posts. Dentistry Today. In press.
28. Braga RR, Ballester RY, Ferracane JL. Factors involved in the development of polymerization shrinkage stress in resin-composites: a systematic review. Dent Mater. 2005;21(10):962-970.
29. Breschi L, Mazzoni A, De Stefano DE, Ferrari M. Adhesion to intraradicular dentin: a review. J Adhes Sci Technol. 2009;23(7-8):1053-1083.
30. Bouillaguet S, Troesch S, Wataha JC, et al. Microtensile bond strength between adhesive cements and root canal dentin. Dent Mater. 2003;19(3):199-205.
31. Porciani PF, Coniglio I, Magni E, Grandini S. Fiber post fitting to the canal anatomy: a review of the morphology and shape of root canal system. Int Dent S Afr. 2008;10(6):52-58.
32. ADA Council on Scientific Affairs. Endodontic Posts: Tips for Securing Restorative Success. www.ada.org/sections/scienceAndResearch/pdfs/0604_tips_endoposts.pdf. Accessed June 5, 2013.
33. Musikant BL. Principles for safe and effective post placement. Inside Dentistry. 2012;8(3):82-84.
34. Peutzfeldt A, Sahafi A, Asmussen E. A survey of failed post-retained restorations. Clin Oral Investig. 2008;12(1):37-44.
35. Metink AG, Creugers NH, Meeuwissen R, et al. Clinical performance of different post and core systems—results of a pilot study. J Oral Rehabil. 1993;20(6):577-584.
36. Standlee JP, Caputo AA, Holcomb J, Trabert KC. The retentive and stress-distributing properties of a threaded endodontic dowel. J Prosthet Dent. 1980;44(4):398-404.
37. Ross RS, Nicholls JI, Harrington GW. A comparison of strains generated during placement of five endodontic posts. J Endod. 1991;17(9):45-456
38. Standlee JP, Caputo AA, Collard EW, Pollack MH. Analysis of stress distribution by endodontic posts. Oral Surg Oral Med Oral Pathol. 1972;33(6):592-560.
39. Schmitter M, Rammelsberg P, Gabbert O, Ohlman B. Influence of clinical baseline findings on the survival of 2 post systems: a randomized clinical trial. Int J Prosthodont. 2007;20(2):173-178.
40. Burns DA, Krause WR, Douglas HB, Burns DR. Stress distribution surrounding endodontic posts. J Prosthet Dent. 1990;64(4):412-418.
41. Standlee JP, Caputo AA. The retentive and stress distributing properties of split threaded endodontic dowels. J Prosthet Dent. 1992;68(3):436-442.
42. Stockton LW. Factors affecting retention of post systems: a literature review. J Prosthet Dent. 1999;81(4):380-385.
43. Dhanavel C, Madhuram K, Naveenkumar V, Anbu R. Fracture resistance of endodontically treated maxillary central incisor with five different post and core systems–an in-vitro study. Internet J Dent Sci. 2011;10(1). doi:10.5580/1d18.
44. Manning KE, Yu DC, Yu HC, Kwan EW. Factors to consider for predictable post and core build-ups of endodontically treated teeth. Part II: Clinical application of basic concepts. J Can Dent Assoc. 1995;61(8):696-707.
45. McLean A. Predictably restoring endodontically treated teeth. J Can Dent Assoc. 1998;64(11):782-787.
46. Thorsteinsson TS, Yaman P, Craig RG. Stress analyses of four prefabricated posts. J Prosthet Dent. 1992;67(1):30-33.
About the Author
Leendert Boksman, DDS, BSc, FADI, FICD
Retired from Private Practice
London, Ontario, Canada
Adjunct Clinical Professor of Dentistry
University of Technology, Jamaica
Kingston, Jamaica
Gildo Coelho Santos, JR, DDS, MSc, PhD
Assistant Professor and Chair Division of Restorative Dentistry
Schulich School of Medicine and Dentistry
University of Western Ontario
London, Ontario, Canada
Manfred Friedman,BDS, BChD
Adjunct Clinical Professor
Division of Restorative Dentistry
Schulich School of Medicine and Dentistry, UWO
London, Ontario, Canada
Private Practice
London, Ontario, Canada