Digital Imaging for Cosmetic Cases
Cosmetic imaging allows the patient to view possible treatment outcomes, which can lead to a higher case acceptance rate for the dentist.
Martin Jablow, DMD
Digital imaging has changed the way we interpret, diagnose, treatment plan, and educate our patients. Through the use of digital radiography, we are able to see larger images and manipulate them for better diagnosis. Cone-beam imaging has propelled us into the world of three dimensions. Cosmetic imaging allows us to allow the patient to view possible treatment outcomes. All of these modalities greatly assist us in educating our patients and ourselves.
In the author’s office, all different types of digital imaging are used routinely, starting with the patient’s initial entry into the office. All patients have a quick photograph taken with an inexpensive point-and-shoot digital camera. The photograph is uploaded into the practice management software. This way the patient can always be properly identified—no more wondering which patient is sitting in the reception area.
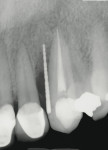
After the patient is seated, radiography is started using both sensors and phosphor plates. Both types of digital radiography have their advantages and disadvantages, but both can produce diagnostic images. Patients are usually intrigued the first time they see the images popping up on the computer screen. Because the images are larger then the standard #2 sized film, it is much easier to read the radiograph and explain any pathology to the patient. The ability to manipulate the image can make diagnosis much easier. There are programs such as LOGICON Caries Detector Software by Carestream Dental (www.carestreamdental.com) that can assist in caries lesion diagnosis. Images on the larger computer monitor greatly assist in educating the patient about their pathology.
Then a series of digital photographs are taken. These photographs can be taken with either a point-and-shoot camera or, for better images, a digital single-lens reflex (DSLR) camera. This series of photographs allows the author to do what he calls the virtual examination. Referencing both digital radiographs and photographs allows for a very comprehensive review of the patient’s current dental status without looking in the mouth. It is at this time where the author starts discussing any problems the patient might have and different treatment options. If the patient is missing any teeth and has indicated that he or she may be interested in implants as a prosthetic option, a cone-beam scan may be taken. Cone-beam imaging allows for a three-dimensional rendering of the patient’s condition. This greatly assists in implant planning. Some cone-beam machines can also take images of the facial soft tissue. Manipulation of the cone-beam image assists in seeing where facial features may be altered by placement of the teeth, orthognathic surgery, or orthodontics.
Cosmetic Concerns
With the photographs on the computer monitor, the author discusses any cosmetic concerns the patient may have. Many times the patient has never seen their teeth in this manner. The ability to discuss any cosmetic concerns in depth and point out areas of concern during treatment makes this the best way to communicate with the patient. We can discuss the many facets of designing a new smile no matter what treatment maybe indicated. Explaining to an adult patient the various treatment choices, such as a possible need for gingival recontouring and porcelain laminates, as well as discussing the benefits or disadvantages of each option, allows the patient to interact with the dentist on a more interactive level in order to determine the best treatment plan.
If the patient does have concerns about the treatment outcome, the use of digital images makes it easy to show the patient the potential benefits of the proposed treatment. Through manipulation of the before photographs, the patient can view possible treatment outcomes. It can be very simple to show the patient the potential benefits of whitening. While designing a smile, treatment information, such as the need for altering a smile line and crown lengthening, can be gathered. There are many imaging software programs that can do this type of manipulation, such as Adobe® Photoshop (www.photoshop.com). Dentists who do a lot of cosmetic cases may choose a specific dental cosmetic software package for its ease of use and shorter learning curve. Many of the current imaging software programs have add-on cosmetic imaging modules. For those who do an occasional cosmetic case, there are outside services that can provide the before-and-after simulations. The preoperative images are e-mailed and simulations are returned either via e-mail or by mail with photographs to give to the patient.
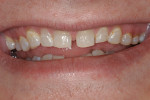
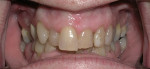
Simulations are not so much for the doctor as they are to present visual information to the patient. Sam Laundon of SmilePix (www.smilepix.com), who has been providing patient smile simulations for years, recommends that full-face portrait photographs be used and have the patient choose the photograph they want to have the smile simulation done on (written communication, September 2011). Dentists like to look at teeth, but the patient is not used to looking at teeth, and so they prefer to see only their own teeth. The better the photograph, the better the simulation and patient response. Make sure a natural smile is included in the portrait, so ask the patient to say “cheese” (Figure 1 and Figure 2).
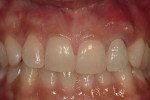
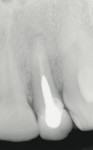
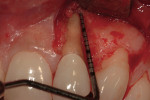
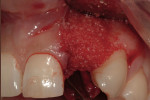
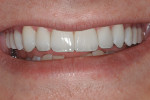
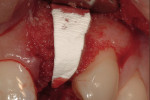
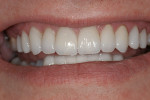
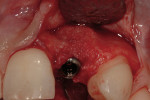
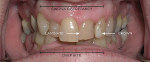
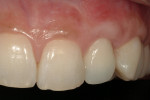
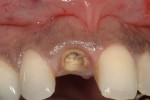
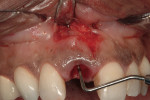
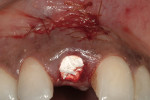
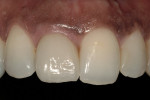
The use of photography and computer software for shade matching and dental laboratory communications is well documented.1 Imaging is a great tool for the laboratory technician. Images sent to the ceramist help them to replicate esthetic restorations. The key to digital imaging is making sure everything is anatomically correct. The patient’s full face must be visualized, including their smile, along with lateral smile views. A thorough knowledge of smile design is necessary to adequately create a good imaging solution (Figure 3, Figure 4, and Figure 5). Envision A Smile (www.envisionasmile.com) helped develop this case through imaging.
Caries detection has become image-based through specialized intraoral cameras such as Air Techniques’ Spectra Caries Detection Aid (www.airtechniques.com) and Acteon’s SOPROLIFE® (www.aceteongroup.com). These devices can assist in detecting caries lesions through the use of fluorescence. The images obtained by these devices can be shown to educate the patient and are then stored in the imaging software.
Seventy-five percent of all learning is visual, so patient education software can make explaining different treatment procedures easier for the dentist and allows for better understanding by the patient. Examples of patient education software are CAESY, a Patterson Technology (www.caesy.com) and Henry Schein’s Guru (www.howdoyouguru.com). The author uses Guru when he needs to discuss a cosmetic case in depth. The reason the author likes Guru is for its ability to show the patient animations of the proposed treatment and the ability to add his own photographs and radiographs to the presentation. The images can be drawn on to further enhance the proposed treatment plan presentation (Figure 6 and Figure 7).
Oral Cancer
Photographing soft-tissue pathology allows for better monitoring and communicating about the pathology. Fluorescent imaging using an Identafi® 3000 (Star Dental/Dental EZ Group, www.identifi.net) or VELscope® VX (LED Dental, www.velscope.com) can supplement normal white-light cancer examinations and assist in viewing a lesion2 along with assisting the surgeon in determining the borders of the lesion.3 Sending a photograph of a lesion to the oral pathologist will assist in the diagnosis. You will no longer have to describe the lesion; you will have shown the lesion to the pathologist.
Digital imaging provides many benefits to both the doctor and patient. Enhanced diagnostics in both 2D and 3D assist in better treatment planning, which leads to better cosmetic outcomes. The most important aspect of digital images is the ability to better communicate the need for treatment and the possible treatment procedures that can provide the necessary care that the patient needs.
References
1. Schropp L. Shade matching assisted by digital photography and computer software. J Prosthodont. 2009;18(3):235-241.
2. Roblyer D, Kurachi C, Stepanek V, et al. Objective detection and delineation of oral neoplasia using autofluorescence imaging. Cancer Prev Res. 2009;2(5):423-431.
3. Poh CF, Zhang, L, Anderson DW, et al: Fluorescence visualization detection of field alterations in tumor margins of oral cancer patients. Clin Cancer Res. 2006;12(22):
16-6722.
About the Author
Martin Jablow, DMD
Private Practice
Woodbridge, New Jersey