The Bonded Single-Wing Zirconia Bridge
A conservative and esthetic treatment option to replace missing maxillary lateral incisors
J. William Robbins, DDS, MA | Marcela G. Alvarez, DDS, MSD | Hiro Tokutomi, CDT
There are several possible treatment options for the replacement of a missing maxillary lateral incisor.1 These include placing an implant or a mini-implant, orthodontic substitution, autotransplantation, and placing a bonded bridge. Because each of these approaches has different indications and inherent advantages and disadvantages, they should be assessed on a case-by-case basis.
Implants
Due to the longevity and relatively high success rates of implants, they are one of the most popular treatment options. However, there are several disadvantages associated with placing an implant in the anterior maxilla. A missing anterior tooth is generally the result of trauma or agenesis. In both of these circumstances, there is commonly inadequate bone for an implant, and both hard- and soft-tissue grafting is required. A second disadvantage is the potential for implant failure. This can be due to peri-implantitis2 or due to thinning of the supporting tissue, which can result in blue or grey show-through.3 For younger adult patients, a third and significant disadvantage is relative intrusion of the implant due to late vertical maxillary growth.4 It is well known that late maxillary growth can occur, and there is no definitive way to predict when it will occur.5-8 For this reason, the belief that an implant can be safely placed in, for example, a 19-year-old female patient or a 21-year-old male patient is not supported by the literature.9-10 A mini-implant has been proposed as an intermediate treatment option.11-12 However, there is minimal information in the literature to support this concept. A final disadvantage of implant placement in these cases is related to increased awareness of the maxillary transverse deficiency and its relation to the airway. With the current technology, adult patients who have passed the window for tooth-borne palatal expansion can still undergo palatal expansion. The expansion can be accomplished with an implant-borne palatal expander.13 However, if the patient has an implant in the anterior maxilla, it is not possible to do adult palatal expansion because the presence of the implant makes it impossible to redistribute the space after expansion.
Orthodontic Substitution
Orthodontic substitution, especially canine substitution to replace congenitally missing maxillary lateral incisors, is a commonly used option.14 However, there are clinical requirements for this treatment. The canines should be small enough so that they can be reshaped to look like lateral incisors, and they should also be a similar in color to the adjacent central incisors. In addition, the orthodontic movement should be accomplished in a manner that doesn't result in loss of arch length.14
Autotransplantation
Autotransplantation can be a viable treatment option when the timing requirements are met. This option is most commonly used when a maxillary central incisor is ankylosed or lost due to trauma. An osteotomy is created at the site of the missing central incisor, and a tooth (commonly a mandibular second premolar), is surgically extracted, placed in the osteotomy site, and stabilized. Ideally, autotransplantation should be accomplished when the root of the donor tooth is approximately three quarters of the way formed, which is usually around age 10 to 12. This technique has been used for many decades in Europe,15 and it is reported to have a high rate of success when a stringent protocol is used.16
Bonded Bridges
The final treatment option is the bonded bridge. This treatment has been available since it was first described by Howe and Denehy in 1977.17 When bonded to an enamel substrate, bonded bridges with metal frameworks were very successful.18 Initially, the technique required two wings to be bonded to the abutment teeth adjacent to the pontic. However, over time, it became clear that a pontic with one wing bonded to the larger abutment tooth was preferable to the two-wing technique.19-20 In addition, the metal wings lowered the value of the abutment teeth, resulting in less-than-ideal esthetics. For this reason, the metal framework fell out of favor. Several other framework materials were utilized, including reinforced composite, leucite-reinforced glass-ceramic, and lithium disilicate; however, none of these materials demonstrated the necessary degree of fracture resistance. In recent years, the material of choice has become zirconia.21-22 Its fracture resistance approaches that of metal,23 and its white color doesn't change the color of the abutment tooth, making it an ideal substrate material. The substructure should be constructed from 3Y zirconia, and then glass-ceramic or lithium disilicate should be layered on the facial surface of the pontic to improve the esthetics. To optimize the success of bonded single-wing zirconia bridges, there are soft-tissue, pre-prosthetic, and prosthetic factors that should be considered.
Soft-Tissue Factors
Oftentimes, there is a soft-tissue deficit at the pontic site. This requires a soft-tissue grafting procedure to provide the correct emergence profile for an ovate pontic.24 It has been reported that the volume of soft tissue created with a connective tissue graft remains stable under an ovate pontic over the long term.25 The ovate pontic site can be created 3 months after the grafting procedure.24
Pre-Prosthetic Factors
When treatment planning a bonded bridge, the edentulous site should be approximately the same width as the contralateral tooth. The abutment tooth should be large enough to provide 30 mm2 of enamel surface and a 3 mm connector height.26 In addition, the zirconia wing must be at least 0.7-mm thick.26 Because it must be bonded to an enamel substrate and only minimal tooth structure can be removed from the lingual surface of the abutment tooth, the space to accommodate the necessary wing thickness is commonly created orthodontically or with enameloplasty of the opposing tooth.
Prosthetic Factors
When replacing one tooth, the bridge will have only one wing bonded to the largest abutment tooth.19-20 Therefore, the abutment tooth should have an anti-rotation groove or box adjacent to the pontic site to provide resistance form.27 In addition, the bridge should have a small extension onto the lingual surface of the adjacent tooth to provide resistance from facial movement of the pontic.1 This extension is not bonded, and the contact between it and the adjacent tooth is flossable. Single-wing bridges should be bonded with a dual-cure resin cement that is designed to be used with zirconia, and a precise protocol should be followed.28-30 There should be no contact on the pontic in maximum intercuspation or in excursions.
Case Report
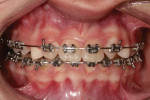
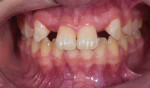
A 13-year-old female patient was referred for an evaluation for a restorative treatment plan. She presented with retained primary maxillary canine teeth, and although she was congenitally missing teeth Nos. 7 and 10, she had been in active orthodontic treatment for one year, and teeth Nos. 6 and 11 were in the lateral incisor positions (Figure 1). During the examination, it was noted that the canine teeth were large mesiodistally and had high yellow chroma. For these and other reasons, the decision was made to distalize the canine teeth to make room for bonded bridges to replace the missing lateral incisors.
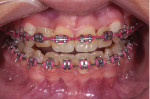
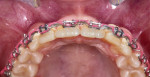
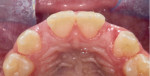
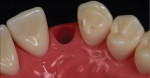
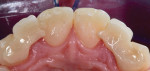
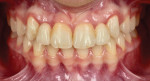
The patient's primary canine teeth were extracted, and she continued with orthodontic treatment until teeth Nos. 6 and 11 were retracted into their correct positions in the arch (Figure 2). However, at the completion of the retraction, there were hard- and soft-tissue deficits at the edentulous sites of teeth Nos. 7 and 10 (Figure 2 and Figure 3). After removal of the orthodontic appliances, connective tissue grafts were placed at the tooth No. 7 and 10 sites to create adequate soft tissue for ovate pontics (Figure 4 and Figure 5). Following the healing period, tooth bleaching was accomplished with home bleaching trays (Clear Mouthguard Material, Great Lakes Dental Technologies). Teeth Nos. 6 and 11 were then prepared for bonded single-wing bridges (Figure 6), and the zirconia bridges (KATANA™ Zirconia HTML PLUS, Kuraray Noritake) were bonded into place with a dual-cure resin cement (PANAVIA™ V5, Kuraray Noritake) (Figure 7 through Figure 9). In this case, the canines were selected as the abutment teeth because their shape permitted the placement of better retention grooves than the central incisors. A clear retainer (Clear Splint Biocryl, Great Lakes Dental Technologies) was fabricated and delivered for orthodontic retention. Also, in the event that either of the bridges de-bonded, the retainer would retain them until they could be re-bonded.
Conclusion
There are several options available for the replacement of missing maxillary lateral incisors. Although the placement of implants and mini-implants, canine substitution, and autotransplantation can offer advantages when indicated in certain cases, these treatments present with many disadvantages. Bonded single-wing zirconia bridges offer many advantages, particularly for younger patients, and when placed using the techniques outlined in this article, they can deliver outcomes with excellent esthetics that achieve long-term success.
Acknowledgement
The authors would like to thank Darrell Childers, DDS, for the orthodontic treatment and Eric Rindler, DDS, for the connective tissue grafting on the patient in the case report.
About the Authors
J. William Robbins, DDS, MA
Clinical Professor
School of Dentistry
University of Texas Health Science Center at San Antonio
San Antonio, Texas
Private Practice
San Antonio, Texas
Marcela G. Alvarez, DDS, MSD
Private Practice
San Antonio, Texas
Hiro Tokutomi, CDT
Owner
Art Box Boston Esthetic Dental Laboratory
Tewksbury, Massachusetts
References
1. Robbins JW, Alvarez MG. Treatment options for the replacement of the missing maxillary lateral incisor. Compend Contin Educ Dent. 2021;42(9):504-509.
2. Lindhe J, Meyle J. Perio-implant diseases: consensus report of the Sixth European Workshop on Periodontology. J Clin Periodontol. 2008;35(Suppl 8):282-285.
3. Garber DA, Salama MA, Salama H. Immediate total tooth replacement. Compend Contin Educ Dent. 2001;22(3):210-218.
4. Bernard JP, Schatz JP, Christou P, et al. Long-term vertical changes of the anterior maxillary teeth adjacent to single implants in young and mature adults. A retrospective study. J Clin Periodontol. 2004;31(11):1024-1028.
5. Jemt T. Measurements of tooth movements in relation to single-implant restorations during 16 years: a case report. Clin Implant Dent Relat Res. 2005;7(4):200-208.
6. Zachrisson BU. Single implant-supported crowns in the anterior maxilla - potential esthetic long-term (>5 years) problems. World J Orthod. 2006;7(3):306-312.
7. Covani U, Crespi R, Cornelini R, Barone A. Immediate implants supporting single crown restoration: a 4-year prospective study. J Periodontol. 2004;75(7):982-988.
8. Bishara SE, Treder JE, Jakobsen JR. Facial and dental changes in adulthood. Am J Orthod Dentofacial Orthop. 1994;106(2):175-186.
9. Thilander B, Odman J, Jemt T. Single implants in upper incisor region and their relationship to the adjacent teeth. An 8-year follow-up study. Clin Oral Implants Res. 1999;10(5):346-355.
10. Thilander B. Dentoalveolar development in subjects with normal occlusion. A longitudinal study between the ages of 5 and 31 years. Eur J Orthod. 2009;31(2):109-120.
11. Cope JB, McFadden D. Temporary replacement of missing maxillary lateral incisors with orthodontic miniscrew implants in growing patients: rationale, clinical technique, and long-term results. J Orthod. 2014;41(Suppl 1):S62-S74.
12. Ciarlantini R, Melsen B. Semipermanent replacement of missing maxillary lateral incisors by mini-implant retained pontics: a follow-up study. Am J Orthod Dentofacial Orthop. 2017;151(5):989-994.
13. Moon W, Wu KW, MacGinnis M, et al. The efficiency of maxillary protraction protocols with micro-implant-assisted rapid palatal expander (MARPE) and the novel N2 mini-implant-a finite element study. Prog Orthod. 2015;16:16.
14. Norris RT, Caesar RR. Esthetic substitution and autotransplantation of teeth in the maxillary anterior region. Semin Orthod. 2013;19(1):3-12.
15. Andreasen JO, Paulsen HU, Yu Z, et al. A long-term study of 370 autotransplanted premolars. Part II. Tooth survival and pulp healing subsequent to transplantation. Eur J Orthod. 1990;12(1):14-24.
16. Machado LA, do Nascimento RR, Ferreira DM, et al. Long-term prognosis of tooth autotransplantation: a systematic review and meta-analysis. Int J Oral Maxillofac Surg. 2016;45(5):610-617.
17. Howe DF, Denehy GE. Anterior fixed partial dentures utilizing the acid-etch technique and a cast metal framework. J Prosthet Dent. 1977;37(1):28-31.
18. Saker S, El-Fallal A, Abo-Madina M, et al. Clinical survival of anterior metal-ceramic and all-ceramic cantilever resin-bonded fixed dental prostheses over a period of 60 months. Int J Prosthodont. 2014;27(5):422-424.
19. Briggs P, Dunne S, Bishop K. The single unit, single retainer, cantilever resin-bonded bridge. Br Dent J. 1996;181(10):373-379.
20. Kern M, Gläser R. Cantilevered all-ceramic, resin-bonded fixed partial dentures: a new treatment modality. J Esthet Dent.1997;9(5):255-264.
21. Kern M, Passia N, Sasse M, Yazigi C. Ten-year outcome of zirconia ceramic cantilever resin-bonded fixed dental prostheses and the influence of the reasons for missing incisors. J Dent. 2017;65:51-55.
22. Sailer I, Hämmerle CHF. Zirconia ceramic single-retainer resin-bonded fixed dental prostheses (RBFDPs) after 4 years of clinical service: a retrospective clinical and volumetric study. Int J Periodontics Restorative Dent. 2014;34(3):333-343.
23. Rosentritt M, Preis V, Behr M, Strasser T. Fatigue and wear behavior of zirconia materials. J Mech Behav Biomed Mater. 2020;110:103970.
24. Robbins JW. The ovate pontic. Inside Dentistry. 2022;18(11):35-38.
25. Bienz SP, Sailer I, Sanz-Martín I, et al. Volumetric changes at pontic sites with or without soft tissue grafting: a controlled clinical study with a 10-year follow-up. J Clin Periodontol. 2017;44(2):178-184.
26. Kern M. RBFDPs. Resin-Bonded Fixed Dental Prostheses. Quintessence Publishing; 2018:74-75.
27. Kern M. RBFDPs. Resin-Bonded Fixed Dental Prostheses. Quintessence Publishing; 2018:134-135.
28. Blatz MB, Phark JH, Ozer F, et al. In vitro comparative bond strength of contemporary self-adhesive resin cements to zirconium oxide ceramic with and without air-particle abrasion. Clin Oral Investig. 2010;14(2):187-192.
29. Blatz MB, Chiche G, Holst S, Sadan A. Influence of surface treatment and simulated aging on bond strengths of luting agents to zirconia. Quintessence Int. 2007;38(9):745-753.
30. Blatz MB, Alvarez M, Sawyer K, Brindis M. How to bond zirconia: the APC concept. Compend Contin Educ Dent. 2016;37(9):611-617.