Immediate Implant Placement and Provisionalization
The new standard for predictable esthetics in single-tooth implants
Abstract
Ever since the introduction of root-form implants, experts have advocated a staged approach whereby the implant is placed in an edentulous area and allowed to heal undisturbed so that osseointegration can occur, after which the fabrication of the definitive restoration can take place. The use of immediate implant placement and loading protocols, however, has increased because of advantages in terms of predictable esthetics, decreased treatment duration, and lower morbidity. The purpose of this article is to review the rationale, techniques, and evidence for the use of immediate implant placement and provisionalization for single-tooth applications. The author also describes an approach that entails: atraumatic extraction of the tooth; appropriate implant selection; use of a flapless placement approach; lingualized implant placement; grafting of the labial gap with a xenograft; immediate provisionalization; and occlusal management.
A review of esthetic outcomes reported in the implant literature revealed that the single-tooth replacement was the only clinical situation where predictable esthetic outcomes could be consistently achieved.1 Other clinical scenarios—such as adjacent implants or treatment of multi-tooth defects—did not yield predictable esthetic results. This has been attributed to the fact that the interproximal crest of the adjacent teeth provides the support necessary to maintain the peri-implant soft-tissue levels in sites without defects.2
In 2005, Furhauser et al proposed the “Pink Esthetic Score” in an effort to systematize the evaluation of implant esthetic outcomes.3 The Pink Esthetic Score includes rating scales for seven peri-implant soft-tissue parameters. This emphasizes that the achievement of natural-looking gingival tissues may be one of the most challenging aspects in implant esthetics.3
Single-Tooth Implant Options
When considering replacement of a single tooth with a dental implant, the clinician is faced with the options of choosing a delayed (traditional) or immediate approach, depending on whether or not the tooth is present.
However, in situations where the tooth is present, the clinician has several alternatives, including the traditional approach, immediate implant placement, and site development, which are described below.
Traditional Approach
In the traditional approach, the tooth is extracted, and the implant is placed after the ridge has healed. Without socket preservation, healing of extraction sites is accompanied by significant vertical and horizontal bone resorption, which may subsequently require multiple procedures to reconstruct the collapsed ridge and further prolong treatment duration.
Immediate Implant Placement
Immediate implant placement, in which the clinician places the implant immediately following extraction, can be chosen if the periodontium is intact. This approach offers the advantages of decreased treatment time and morbidity, while exhibiting success rates similar to those of the traditional approach.4 Additionally, it offers the option of immediate provisionalization and enhanced esthetic outcomes.
Site Development
If there are hard- or soft-tissue defects associated with the hopeless tooth, forced eruption may be used to optimize the site prior to implant placement. Co-treatment with specialists is advisable in these instances.
Immediate Implant Placement and Provisionalization: A New Paradigm for The Esthetic Zone
An immediate implant placement and provisionalization approach has been increasingly adopted by clinicians because the technique seems to predictably improve esthetic outcomes. Favorable results were originally reported over a decade ago.5,6 However, subsequent publications reported recession and loss of labial crest height.7 Although buccal implant placement was the main cause of recession in many instances, biotype and factors affecting crestal bone maintenance may also play a role. A more recent animal study demonstrated that the labial plate is maintained when implants are placed in a lingual position.8 Furthermore, a recently published cone beam computed tomography (CBCT) study in humans confirms the preservation of the labial plate following flapless, lingualized, immediate implant placement.9
The use of an adequately contoured immediate provisional restoration is essential in preserving the peri-implant soft-tissue profiles following immediate implant placement, particularly with respect to the mid-facial gingival margin level.10
Immediate Implant Placement and Provisionalization
The technique of immediate implant placement and provisionalization that is advocated by the author requires the following elements: atraumatic extraction of the tooth; appropriate implant selection; use of a flapless placement approach; lingualized implant placement; grafting of the labial gap with a xenograft; immediate provisionalization; and occlusal management.
Atraumatic Extraction
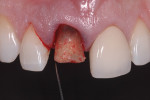
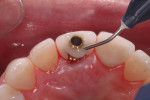
Since immediate implant placement and provisionalization is recommended only in intact sockets, it is essential that alveolar bone and gingiva be preserved with an atraumatic extraction technique. Instruments such as periotomes, small elevators, and root forceps may be used to avoid damage to the labial plate. Following extraction, the site must be thoroughly inspected to verify the integrity of the osseous crest (Figure 1).
Flapless Approach
The use of a flapless approach is essential to preserve the thickness of the buccal plate. Elevation of a muco-periosteal flap will disrupt the blood supply and result in resorption of the exposed bone.
Implant Selection
Immediate placement and provisionalization requires the choice of an implant that will provide adequate primary stability and crestal bone maintenance.
Tapered implants facilitate the achievement of high insertion torque, which may serve as an indicator of implant stability.11 A minimum insertion torque of 45 Ncm is required for immediate placement and provisionalization of single-tooth implants.5,6
Traditionally designed implants exhibit crestal bone loss of approximately 1 mm to 1.5 mm, which is observed radiographically to the level of the first thread. The lateral dimension of this bone loss has been reported to measure approximately 1.5 mm.12 This defect develops circumferentially around the implant, manifesting itself on the labial aspect as well.13 Since CBCT studies have reported the width of buccal crest to be in the 1-mm to 1.5-mm range, the establishment of a 1.5-mm-wide circumferential defect will result in apical remodeling of the buccal crest.14
Many factors have been postulated as potentially responsible for this circumferential bone loss. In 2006, however, the “platform switching” concept was introduced, whereby implants restored with components, then “switched” to a narrower diameter platform did not exhibit the crestal bone loss associated with traditional implants.15 While the exact mechanism is not fully understood, there is ample evidence to suggest that positioning the implant/abutment junction in a medial location is beneficial in preventing crestal resorption, regardless of other contributing factors. In fact, platform switching is the most widely documented method for preserving crestal bone around implants.
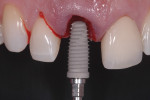
Additional factors that may contribute to crestal bone preservation are decreased component changes and selecting implants that may provide resistance to peri-implantitis16,17 (Figure 2).
Lingualized Implant Placement
Recession has been reported as a complication of immediate implant placement, and it is the main reason why some clinicians recommend a delayed protocol instead.
Several publications have associated recession with buccal implant placement, which often results from attempting to place the implant in the tri-dimensional center of the socket.7
Recent animal and human studies have demonstrated that placing the implant in a lingual position will preserve the buccal plate.8,9 The author recommends lingualized placement within the fresh extraction socket so that a gap will remain between the implant surface and the buccal plate. This gap should measure a minimum of 2 mm to ensure that the implant does not impinge on the buccal plate, therefore isolating it from surgical trauma secondary to the osteotomy preparation or implant insertion.
Grafting of the Labial Gap
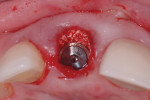
It is the author’s recommendation that the gap resulting from lingualized placement be grafted in all instances with a bovine-derived xenograft (Figure 3). Although other alternatives are available, the author advocates the use of this material due its slow-resorbing characteristics, which may provide long-term support for the soft tissue if there is more-than-expected remodeling of the labial plate. Additionally, a recent CBCT-based human case series demonstrated complete gap fill and radiographic bone-to-implant contact utilizing this technique.9
Immediate Provisionalization
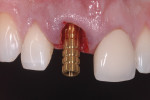
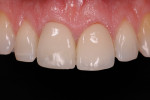
The main objectives of the immediate provisional are to satisfy the patient’s esthetic needs and provide support for the peri-implant soft tissues. The latter requires that the contours of the provisional be adequately designed so that the position of the gingival margin is preserved. Overcontouring near the marginal area will result in apical migration, while undercountouring will cause coronal migration of the gingival margin. In the sub-critical contour area, a concave emergence profile will result in increased peri-implant tissue thickness, which may potentially improve the stability of the gingival margin18 (Figure 4 and Figure 5).
Any of the traditional techniques may be used for fabrication of the immediate provisional, which may be cemented or screw retained. The anatomy of the maxillary incisors and the corresponding alveolar process often cause the long axis of the implant to exit labially. With a screw-retained provisional, obturation of the labial access may become an esthetic challenge. Although this could be avoided with the use of a cemented temporary, the potential disadvantage of residual cement must be considered. Another alternative is to retrofit the clinical crown of the pre-existing tooth, so that it can be utilized to fabricate the provisional restoration. Although particularly effective with respect to preserving the soft-tissue contours, this is an advanced technique that is better reserved for the experienced clinician (Figure 6 through Figure 8).
Occlusal Management
When an immediate provisional is placed, there is a potential for premature loading, which may prevent osseointegration. Although successful outcomes have been reported on implants placed with a minimum insertion torque of 45 Ncm, immediate provisionalization of single implants should be approached with caution. Ideally, all occlusal contacts should be avoided, both in maximum intercuspation as well as eccentric movements. This may become increasingly difficult in deep overbite cases.
Additionally, considering that immediate provisionalization is mostly utilized in the maxillary anterior area, shortening the temporary restoration so that all centric and eccentric contacts are avoided may not be esthetically acceptable. For these purposes, the author recommends the use of occlusal bite planes to ensure non-occlusal loading.
Conclusions
Immediate implant placement and provisionalization offer the potential for predictable esthetic outcomes. Of paramount importance for the success of this surgical technique are the presence of an intact site, integrity of the buccal alveolar plate following extraction, the use of a flapless surgical approach, appropriate implant selection, and lingual placement, followed by grafting with a bovine-derived bone substitute. The immediate provisional must be designed to adequately support the peri-implant tissue architecture while avoiding occlusal contact.
References
1. Belser U, Schmid B, Higginbottom F, Buser D. Outcome analysis of implant restorations located in the anterior maxilla: a review of the recent literature. Int J Oral Maxillofac Implants. 2004;19 Suppl:30-42.
2. den Hartog L, Slater JJ, Vissink A, et al. Treatment outcome of immediate, early and conventional single-tooth implants in the aesthetic zone: a systematic review to survival, bone level, soft-tissue, aesthetics and patient satisfaction. J Clin Periodontol. 2008;35(12):1073-1086.
3. Fürhauser R, Florescu D, Benesch T, et al. Evaluation of soft tissue around single-tooth implant crowns: the pink esthetic score. Clin Oral Implants Res. 2005;16(6):639-644.
4. Esposito M, Grusovin MG, Polyzos IP, et al. Timing of implant placement after tooth extraction: immediate, immediate-delayed or delayed implants? A Cochrane systematic review. Eur J Oral Implantol. 2010;3(3):189-205.
5. Wöhrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: Fourteen consecutive case reports. Pract Periodontics Aesthet Dent. 1998;10(9):1107–1114.
6. Kan JY, Rungcharassaeng K. Immediate placement and provisionalization of maxillary anterior single implants: A surgical and prosthodontic rationale. Pract Periodontics Aesthet Dent. 2000;12(9):817–824.
7. Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Implants Res. 2008;19(1):73-80.
8. Caneva M, Salata LA, de Souza SS, et al. Influence of implant positioning in extraction sockets on osseointegration: histomorphometric analyses in dogs. Clin Oral Implants Res. 2010;21(1):43-49.
9. Lee EA, Gonzalez-Martin O, Fiorellini J. Lingualized flapless implant placement into fresh extraction sockets preserves buccal alveolar bone: a cone beam computed tomography study. Int J Periodontics Restorative Dent. 2014;34(1):61-68.
10. De Rouck T, Collys K, Wyn I, Cosyn J. Instant provisionalization of immediate single-tooth implants is essential to optimize esthetic treatment outcome. Clin Oral Implants Res. 2009;20(6):566-570.
11. Trisi P, Perfetti G, Baldoni E, et al. Implant micromotion is related to peak insertion torque and bone density. Clin Oral Implants Res. 2009;20(5):467-471.
12. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
13. Grunder U, Gracis S, Capelli M. Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent. 2005;25(2):113-119.
14. Huynh-Ba G, Pjetursson B, Sanz M, et al. Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant placement. Clin Oral Implants Res. 2010;21(1):37-42.
15. Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
16. Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol. 1997;24(8):568-572.
17. Zetterqvist L, Feldman S, Rotter B, et al. A prospective, multicenter, randomized-controlled five-year study of hybrid and fully etched implants for the incidence of peri-implantitis. J Periodontol. 2010;81(4):493-501.
18. Su H, Gonzalez-Martin O, Weisgold A, Lee E. Considerations of implant abutment contour and subcritical contour. Int J Periodontics Restorative Dent. 2010;30(4):335-343.
About the Author
Ernesto A. Lee, DMD
Clinical Professor and Director
Postdoctoral Periodontal Prosthesis Program
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Bryn Mawr, Pennsylvania