Restoring a Tooth With a Short Clinical Crown
Consideration of the remaining tooth structure and desired restorative material optimizes preparation design and delivery
Dennis J. Fasbinder, DDS
Restoring a tooth that has a short clinical dimension can be a challenge due to the limited availability of interarch space. The selection of a restorative material and preferred method of delivery are initial considerations; however, is there enough tooth structure available to create sufficient geometric retention and resistance form in the preparation? This article reviews perspectives regarding material selection, tooth preparation, and delivery techniques to help clinicians engineer optimal clinical outcomes based on current clinical research.
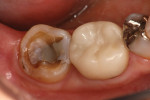
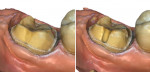
It can be disheartening to start a day in the office when the first patient presents with a mandibular second molar that requires a crown, and the gingiva is already at the height of the distal marginal ridge (Figure 1). This is the essential problem of managing short clinical crown cases: how can the crown be retained when there is limited vertical dimension for the restoration and minimal tooth structure to work with?
There are several possible treatment options that can improve a crown's restorability by increasing the amount of available tooth structure, including crown lengthening surgery or orthodontic treatment. However, in clinical practice, the majority of these situations are managed without such procedures due to patient preferences related to the required treatment time or cost. A lack of interarch space and a lack of clinical crown height are two complementary problems in the restoration of short clinical crowns. The restorative material selected for the crown must have adequate occlusal thickness to resist fracture, and the cervical margin of the crown may need to be subgingival because there is minimal height to the tooth with which to create geometric or mechanical retention, complicating predictable delivery.
Material Selection
Full-contour zirconia and lithium disilicate are two popular materials used for single tooth crowns that have replaced porcelain-fused-to-metal (PFM) crowns in popularity and provide equal clinical predictability. In a systematic review that included 4,663 metal-ceramic and 9,434 all-ceramic single tooth crowns from 67 clinical studies, a meta-analysis of the data indicated that the estimated survival rate of the metal-ceramic crowns after 5 years was 94.7%.1 This was similar to the estimated 5-year survival rates of the all-ceramic lithium disilicate crowns (96.6%) and zirconia crowns (95%). Although selecting between full-contour lithium disilicate and zirconia materials is as much about preference as desirable physical properties, the strength of these materials is an important factor.
Both lithium disilicate and zirconia are desirable for these short clinical crown cases because they are reported to have high strength properties. Strength is an interesting property, especially in cases with limited interarch space. Obviously, if there is limited restorative space, high strength to resist fracture would be a desirable feature. The challenge is that strength is often thought of as an inherent material property. However, strength is actually a dependent material property. This means that the actual strength of a material is dependent on how it is handled instead of being a constant that is independent of other variables. For example, the "strength" of ceramics, including zirconia, is reduced as the thickness of the material is reduced. Zimmerman and colleagues investigated the fracture load of several types of all-ceramic crowns with occlusal thicknesses of 0.5 mm, 1.0 mm, and 1.5 mm that were adhesively bonded to resin dies. None of the 0.5-mm thick crowns survived fatigue testing, and the crowns with 1.5 mm of occlusal thickness demonstrated significantly greater fracture strength when compared with the crowns with 1.0 mm of occlusal thickness.2 In another study, Nakamura and colleagues measured the fracture load of monolithic zirconia crowns that varied by occlusal and axial wall thickness.3 The occlusal thicknesses of the crowns were 0.5 mm, 1.0 mm, and 1.5 mm, which included the cement space (70 µm), and the axial wall thicknesses were 0.5 mm, 0.7 mm, and 1.0 mm. Although the researchers reported a significant difference in the strength of the crowns based on their occlusal thickness, axial wall thickness was not found to significantly affect crown strength. Studies such as these strongly support the assertion that occlusal thickness is the most important volumetric dimension to ensure the strength of a crown and that it is essential to ensure that the minimum recommended thickness for the material is available in the preparation. Reducing the occlusal thickness of a crown relative to the manufacturer's recommendation consistently results in a crown with less "strength" that will not exhibit the desired properties of the material selected.
Tooth Preparation
Recognizing that there is limited space for the restoration, an advantage of using full contour zirconia for short clinical crowns is that its minimal recommended occlusal thickness is the thinnest of the ceramics, and it is still able to retain the desired high strength. Another desirable feature of using zirconia is that it can be conventionally cemented. However, this mandates a mechanically retentive preparation to retain the crown. "Retention" refers to the prevention of crown dislodgement in the direction of the vertical axis of the preparation. "Resistance" refers to the aspects of the tooth preparation that allow it to resist lateral dislodging forces.4 Even though these two terms are sometimes used interchangeably, resistance is considered to be more relevant to crown dislodgement than retention.
Whether a preparation is retentive or nonretentive will significantly influence how the crown is delivered. A retentive preparation permits the crown to be conventionally cemented because it has the necessary geometry to mechanically retain the restoration. Nonretentive preparations lack the necessary geometry to retain the crown and instead rely on an adhesive bond between the tooth and crown to retain the restoration. So, what are the key elements that determine if a tooth preparation is retentive or not? Goodacre and colleagues listed several key features of a retentive preparation, including 10° to 20° of total occlusal convergence (ie, taper), a minimal preparation wall height of 4.0 mm for molars and 3.0 mm for other teeth, and an occlusocervical-to-faciolingual dimension ratio of 0.4 or greater.5 Years later, Podharsky and colleagues found that the ability of a cemented crown to withstand dislodging forces is largely determined by three geometric aspects: the preparation taper, the preparation wall height, and the preparation wall height to base width ratio.6
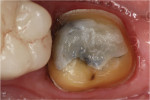
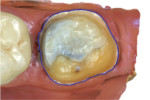
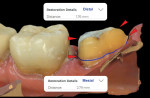
One study evaluated the clinical crown preparations of maxillary first molars completed by 75 general dentists during the course of patient treatment.7 The stone models of the final impressions were digitized into .STL files, and computer software was used to evaluate them regarding preparation undercuts, occlusal reduction, wall taper, margin design, and axial wall height. Although a mean preparation height of 4.0 mm was observed, only 13.3% of the preparations had a convergence angle between 6° and 15°, and the mean convergence angle (ie, taper) observed was 26.7°. A wall taper of less than 15° was considered by the authors to be the most difficult to create clinically, which suggests that adhesive luting may be a more reliable alternative when compared with conventional cementation (Figure 2 through Figure 4). Due to the material selected for the crowns, the desired occlusal thickness was 1.5 mm; however, 33% of the preparations observed demonstrated less than 1.5 mm of clearance for the crown. Studies such as this reveal that even with an understanding of what is desired in a geometrically retentive preparation, it can be challenging to consistently transfer it to the intraoral environment.
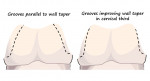
For preparations that are somewhat short or over-tapered, auxiliary retentive features such as axial grooves or boxes, preferably on proximal surfaces, may be considered to enhance the geometry for retention and resistance and permit conventional cementation of the crown (Figure 5).5 One early study reported that the use of interproximal grooves and boxes increased the resistance form of tooth preparations. It also reported that the placement of boxes was more effective than the placement of grooves.8 In another study, the authors reported that grooves and boxes were not effective at increasing resistance form for an over-tapered preparation with greater than 20° total occlusal convergence.9 However, they did indicate that grooves would be expected to be effective if they were prepared with less taper in the cervical third of the tooth to improve the overall taper of the preparation (Figure 6).
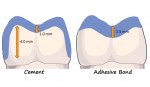
Consider the different dimensional requirements for a mechanically retentive preparation for a conventionally cemented crown when compared with those for a nonretentive preparation for an adhesively bonded crown (Figure 7). For the sake of easy math, 1.0 mm of occlusal reduction is needed for a zirconia crown, recognizing that some full contour materials can be somewhat thinner, and a preparation with remaining tooth structure that is 3.0 to 4.0 mm in height with minimal taper is required for a mechanically retentive preparation, which results in a total of 4.0 mm to 5.0 mm of prepared vertical tooth dimension. Alternatively, 1.5 mm of occlusal reduction may be needed for a ceramic crown, recognizing that some manufacturers recommend at least 1.0 mm, but to adhesively bond and adhesively retain it, no additional vertical tooth structure is required for retention. This results in a considerably smaller amount of tooth dimension required, which is advantageous when restoring a clinically short tooth. If less space is required to adhesively retain a restoration and less tooth structure is required for the preparation, then the delivery technique becomes as critical a factor to consider as the material or tooth preparation.
Delivery Techniques
Significantly less vertical dimension is required for adhesive retention because it is based on the surface area available for bonding. Conventional cementation may be an attractive option due to the simplicity of the technique and cleanup; however, there is no improvement of the restoration's retention or resistance. For short clinical crowns, the ability to provide adhesive retention is an advantage of using a resin bonding technique.
High strength glass ceramics can be predictably bonded to teeth. A well-tested and documented technique includes etching the internal aspect of the crown with hydrofluoric acid for a period of time dictated by the manufacturer, rinsing it off, and then coating the etched surface with a silane coupler. This provides a very dependable bond to the resin cement that is subsequently bonded to the tooth structure. Adhesive bonding is considered to be a technique-sensitive procedure with multiple steps that require good isolation from contaminating moisture to be effective. Nonetheless, clinical studies have demonstrated high survival rates for adhesively bonded restorations.
In one clinical study that included 1,960 complete-coverage lithium disilicate restorations that were adhesively bonded using a total-etch protocol, bonding agent, and dual-cure resin cement, the estimated survival rate of the 1,410 monolithic lithium disilicate restorations was 96.5% at 10.4 years and the estimated survival rate of the 550 bilayered lithium disilicate restorations was 100% at 7.9 years.10 The 10-year estimated cumulative survival rate was 99.6%. In another study by the same group that included a total of 2,392 posterior lithium disilicate restorations that were adhesively bonded using a total-etch protocol, bonding agent, and dual-cure resin cement, there were 1,782 complete coverage restorations and 610 partial coverage restorations.11 The estimated cumulative survival rate of posterior complete and partial coverage restorations was 96.75% at 10.5 years and 95.27% at 16.9 years. No statistically significant difference was found between the survival rates of posterior complete and partial coverage restorations.
Research also indicates similarly high survival rates for ceramic restorations bonded using different protocols. A study of 100 lithium disilicate chairside CAD/CAM crowns found no significant difference in crown survival between those that were delivered using a self-etching, self-adhesive resin cement and those that were delivered using a total-etch protocol, bonding agent, and dual-cure resin cement.12 The crowns demonstrated a cumulative success rate of 92% over 10 years. Edelhoff and colleagues reported on seven patients who underwent full-mouth restorations that included a total of 103 adhesively bonded lithium disilicate occlusal onlays. They reported a 100% survival rate after an average recall period of 7.9 years (5.7 years to 11.6 years).13
One challenge involved in bonding lithium disilicate to short clinical crowns is that the margin may be significantly subgingival. This leads to concerns regarding whether or not the preparation can be adequately isolated for predictable adhesive bonding. However, because bonding a crown does not require the preparation to have as much vertical tooth structure as conventional cementation, in situations involving short clinical crowns, choosing bonding as the delivery technique can oftentimes minimize the need to prepare subgingival margins.
Bonding Zirconia
Is there equally compelling evidence that adhesive bonding is as successful for zirconia as it is for ceramics? The answer to this question becomes more significant in clinical situations, such as those involving short clinical crowns, that present challenges to creating mechanically retentive preparations for zirconia. When delivering zirconia crowns, conventional cementation may be preferred because it is easier and more efficient, but any deficiencies in the geometric retention/resistance form of the preparation limit clinical success. This is one of the reasons for the increased interest in adhesive bonding protocols for zirconia crowns.
A number of in vitro studies have shown that to create a bond to zirconia it must be pretreated with airborne-particle abrasion and then have a phosphate monomer applied.14,15 There are several types of materials advocated for application of the phosphate monomer. These include materials that contain phosphate monomers and are marketed as zirconia primers, certain bonding agents, and certain resin cements. The most popular phosphate monomer to facilitate zirconia bonding is 10-methacryloyloxydecyl dihydrogen phosphate (10-MDP), and it is available in many bonding agents and resin cements.
Regarding the success of adhesively bonded zirconia restorations, some of the most compelling published research is based on zirconia fixed partial dentures. In one study that reported on 108 resin-bonded, single-wing cantilevered anterior zirconia prostheses, there were six debonds in 10 years with 50% of the debonds resulting from physical trauma to the restoration rather than simple dislodgement.16 The researchers reported a survival rate of 98.2% and a success rate of 92.0% after 10 years. Although this is comparable to the results seen with adhesively bonded lithium disilicate crowns, studies on bonded zirconia bridges are based on anterior teeth and primarily depend on enamel bonding. There is a lack of published long-term data on posterior indirect zirconia restorations that primarily depend on dentin bonding.
There are a few short-term clinical studies on adhesively bonded zirconia crowns. In one study that assessed the clinical outcome and survival rate of posterior third-generation monolithic zirconia crowns, 30 posterior full-contour zirconia crowns cemented with a self-adhesive, dual-cure resin cement were followed for a 2-year period.17 The height of the preparations was not reported, but the convergence between the axial walls was described as being less than 6°. No biologic or mechanical complications were observed, and the survival and success rates were reported to be 100%. In another study that evaluated 50 monolithic zirconia crowns, a survival rate of 98% was reported after 5 years, which represents only 2 cases of debonding.18 All of the crowns were placed with a self-adhesive, dual-cure resin cement containing a phosphate monomer. The internal aspect of the crowns was not air-abraded, and there was no etching of the preparation in accordance with the cement manufacturer's instructions; therefore, the retention achieved may have been more mechanical than adhesive, but no specific details on the preparation height or taper were included in the study to make that determination. In one systematic review on the effect of cement type on the clinical performance and complications of zirconia and lithium disilicate crowns, the researchers reported that the published data for conventionally cemented zirconia crowns and conventionally cemented lithium disilicate crowns were limited when compared with those on adhesively bonded lithium disilicate crowns.19 They note that there were no articles available on the most recent generation of high-translucency zirconia to include in the review and that there is a lack of long-term clinical data.
Conclusion
Regarding the three factors that influence the decision of how to restore a short clinical crown, the tooth preparation is a function of the size of the existing defect to be restored as well as the amount of remaining tooth structure, the crown material selected is a function of the desired strength and esthetic demands of the case, and the delivery technique selected is a function of the preparation, including the ability to isolate it, and the material selected.
Clinician preferences often factor strongly into this decision tree. A desire to use zirconia and a conventional cement requires a geometrically retentive tooth preparation for success. When the tooth preparation does not allow for a geometrically retentive design, then adhesive retention is considered. However, if the margins have become significantly subgingival in trying to create sufficient wall height for conventional cementation, this can affect the adhesive outcome. Alternatively, if an adhesive delivery is considered initially, it can influence the tooth preparation to potentially avoid problems with isolation relative to margin location and lead to a more predictable outcome.
The key interrelated decisions for the restoration of short clinical crowns invariably involve zirconia and lithium disilicate crowns. Acknowledging the fact that preparations for adhesively retained restorations require less vertical tooth structure than those for mechanically retained restorations, adhesive delivery may offer significant advantages for short clinical crowns. Both lithium disilicate and zirconia can be adhesively bonded to teeth, but there is a lack of clinical evidence on zirconia restorations bonded to adhesive-style preparations in the posterior dentition. Engineering a predictable clinical outcome for the restoration of a short clinical crown involves more than simply selecting a preferred restorative material; it involves careful consideration of the remaining tooth structure and desired restorative material in order to facilitate the optimum tooth preparation and delivery technique.
About the Author
Dennis J. Fasbinder, DDS
Clinical Professor
School of Dentistry
University of Michigan
Ann Arbor, Michigan
References
1. Sailer I, Makarov NA, Thoma DS, et al. All-ceramic or metal-ceramic tooth-supported fixed dental prostheses (FDPs)? A systematic review of the survival and complication rates. Part I: single crowns (SCs). Dent Mater. 2015;31(6):603-623.
2. Zimmerman M, Egli G, Zaruba M, Mehl A. Influence of material thickness on fractural strength of CAD/CAM fabricated ceramic crowns. Dent Mater J. 2017;36(6):778-783.
3. Nakamura K, Harada A, Inagaki R, et al. Fracture resistance of monolithic zirconia molar crowns with reduced thickness. Acta Odontol Scand. 2015;73(8):602-608.
4. Academy of Prosthodontics. Glossary of prosthodontic terms seventh edition. J Prosthet Dent. 1999;81(1):48-110.
5. Goodacre CJ, Campagni WV, Aquilino SA. Tooth preparations for complete crowns: an art form based on scientific principles. J Prosthet Dent. 2001;85(4):363-376.
6. Podhorsky A, Rehmann P, Wöstmann B. Tooth preparation for full-coverage restorations-a literature review. Clin Oral Investig. 2015;19(5):959-968.
7. Güth JF, Wallbach J, Stimmelmayr M, et al. Computer-aided evaluation of preparations for CAD/CAM-fabricated all-ceramic crowns. Clin Oral Investig. 2013;17(5):1389-1395.
8. Reisbick MH, Shillingburg HT Jr. Effect of preparation geometry on retention and resistance of cast gold restorations. J Calif Dent Assoc. 1975;3(4):51-59.
9. Proussaefs P, Campagni W, Bernal G, et al. The effectiveness of auxiliary features on a tooth preparation with inadequate resistance form. J Prosthet Dent. 2004;91(1):33-41.
10. Malament KA, Natto ZS, Thompson V, et al. Ten-year survival of pressed, acid-etched e.max lithium disilicate monolithic and bilayered complete coverage restorations: performance and outcomes as a function of tooth position and age. J Prosthet Dent. 2019;121(5):782-790.
11. Malament KA, Margvelashvili-Malament M, Natto ZS, et al. Comparison of 16.9-year survival of pressed acid etched e.max lithium disilicate glass-ceramic complete and partial coverage restorations in posterior teeth: performance and outcomes as a function of tooth position, age, sex, and thickness of ceramic material. J Prosthet Dent. 2021;126(4):533-545.
12. Fasbinder DJ, Neiva GF, Heys D, Heys R. Ten-year clinical evaluation of lithium disilicate chairside CAD/CAM crowns. Abstract presented at: 2018 AADR/CADR Annual Meeting; March 24, 2018; Fort Lauderdale, Florida. Presentation ID 1489. https://iadr.abstractarchives.com/abstract/47am-2853967/ten-year-clinical-evaluation-of-lithium-disilicate-chairside-cadcam-crowns. Accessed June 12, 2023.
13. Edelhoff D, Güth JF, Erdelt K, el al. Clinical performance of occlusal onlays made of lithium disilicate ceramic in patients with severe tooth wear up to 11 years. Dent Mater. 2019:35(9):1319-1330.
14. Blatz MB, Vonderheide M, Conejo J. The effect of resin bonding on long-term success of high-strength ceramics. J Dent Res. 2018;97(2):132-139.
15. Kern M, Wegner SM. Bonding to zirconia ceramic: adhesion methods and their durability. Dent Mater. 1998;14(1):64-71.
16. Kern M, Passia N, Sasse M, Yazigi C. Ten-year outcome of zirconia ceramic cantilever resin-bonded fixed dental prostheses and the influence of the reasons for missing incisors. J Dent. 2017;65:51-55.
17. Gseibat M, Sevilla P, Lopez-Suarez C, et al. Prospective clinical evaluation of posterior third-generation monolithic zirconia crowns fabricated with complete digital workflow: two-year follow-up. Materials (Basel). 2022;15(2):672.
18. Solá-Ruiz MF, Baixauli-López M, Roig-Vanaclocha A, et al. Prospective study of monolithic zirconia crowns: clinical behavior and survival rate at a 5-year follow-up. J Prosthodont Res. 2021;65(3):284-290.
19. Maroulakos G, Thompson GA, Kontogiorgos ED. Effect of cement type on the clinical performance and complications of zirconia and lithium disilicate tooth-supported crowns: a systematic review. Report of the Committee on Research in Fixed Prosthodontics of the American Academy of Fixed Prosthodontics. J Prosthet Dent. 2019;121(5):754-765.