Comprehensive Restorative Dentistry With Super Translucent Zirconia
Digital technologies and innovative materials complement time-tested techniques
Jenny Apekian, DDS
The number of adults aged 65 and older in the United States is expected to reach 74 million by 2030. That would represent a 46% increase since 2010 and make this group nearly 20% of the US population.1 Oftentimes, restorative dental procedures performed on elderly patients present unique challenges, and with such a large segment of the population getting older, dentists will need to be ready to serve this aging population.1-3 According to the American Dental Association's research on aging and dental health, some of the more common oral conditions that affect this population include xerostomia, root and coronal caries, tooth loss, and periodontitis.4
Case Report
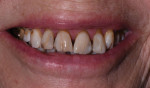
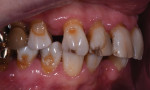
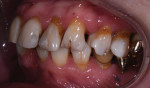
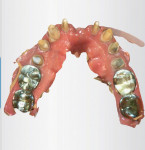
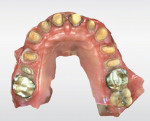
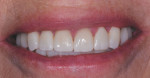
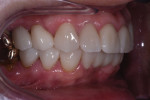
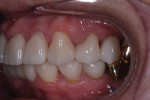
A 75-year-old female patient presented to the office seeking quite extensive restorative and cosmetic treatment (Figure 1 through Figure 4). She presented with several areas of arrested cavities and a history of periodontal disease that had resulted in the extraction of teeth Nos. 24 and 25. She also had a history of undergoing radiation therapy for breast cancer treatment, which lead to the presence of dry mouth-related dental repercussions, significant spacing issues, and discolored teeth. Due to the patient's age and history of bisphosphonate therapy, she was unwilling to consider orthodontic treatment. She had no active decay, and her cancer was in remission.
Treatment Plan
Following a full evaluation and the completion of a diagnostic wax-up, the recommendation was made to restore the patient's smile by placing chairside-fabricated super translucent multilayered zirconia crowns (KATANA™ Zirconia STML, Kuraray Noritake) on teeth Nos. 4 through 13, 20 through 22, and 27 through 29 with a 4-unit bridge that would extend from tooth No. 23 to tooth No. 26. Considering that a 4-unit bridge would be necessary to replace the missing lower anterior teeth where connector strength is important, even with well-defined embrasures, this zirconia material was chosen for its high strength and optimal esthetic properties. The patient only wanted to address the teeth that were visible in her smile, so her existing posterior crowns would be maintained. A facially generated treatment plan was utilized to digitally wax up the patient's broken and missing teeth. The primary objectives were to level her cant, restoratively close her open gingival embrasures, and reduce the proclination of her anterior teeth.
Restorative Technique
At the first appointment, facial reference points were taken into consideration to determine if the patient required an increase in vertical dimension. Once it was established that her vertical dimension of occlusion was acceptable, a digital wax-up was created. This was used as a preparation guide as well as to inform the design for her temporary restorations. After achieving adequate anesthesia, the teeth were prepared, and digital scans of the preparations were acquired with an intraoral scanner (CEREC® Primescan™, Dentsply Sirona) (Figure 5 and Figure 6). Based on the digital wax-up and preparation scans, the temporary restorations were 3D printed (Envision One CDLM, EnvisionTEC) from a resin material (Flexcera™ Smile, EnvisionTEC). After processing, the temporary restorations were seated, the excess cement was removed, and a second appointment was scheduled for placement of the final restorations.
The final restorations were digitally designed (CEREC® Software 5, Dentsply Sirona), and once the proposed designs were approved, the restorations were milled (CEREC® Primemill, Dentsply Sirona) from the chosen super translucent multilayered zirconia material. Following milling, the anatomy was defined by hand, and then the restorations were sintered in an oven (CEREC® SpeedFire, Dentsply Sirona) and characterized with stains and glazes (CERABIEN™ ZR, Kuraray Noritake).
For the second appointment, the patient returned to the office for try-in and cementation of the final restorations. The try-in of each restoration involved checking for marginal integrity, proper interproximal contacts, and an ideal occlusal relationship. No adjustments were necessary, so the final restorations were cemented with a self-adhesive resin cement (PANAVIA™ SA Cement Universal, Kuraray Noritake). After the excess cement was removed, occlusion was once again verified, and final polishing was performed to complete the procedure. The patient stated that she was extremely pleased with her new smile (Figure 7 through Figure 10).
Discussion
Restorative and cosmetic treatment for senior adults should be carefully planned, taking into consideration each patient's past and present oral health status and overall medical history. The range of treatment options proposed should focus on simple, stable, and proven prosthetic concepts that provide patients with the appearance that they are looking for while restoring natural function and integrity.
About the Author
Jenny Apekian, DDS
Private Practice
Sacramento, California
MANUFACTURER INFORMATION
Kuraray Nortiake
kuraraydental.com
800-879-1676
References
1. A State of Decay: Are Older Americans Coming of Age Without Oral Healthcare? Vol. III. Oral Health America and Wisdom Tooth Project 2016.
2. Berkey D, Berg R. Geriatric oral health issues in the United States. Int Dent J. 2001;51(3 Suppl):254-264.
3. Thomson WM, Ma S. An ageing population poses dental challenges. Singapore Dent J. 2014;35C:3-8.
4. Aging and dental health. American Dental Association website. https://www.ada.org/resources/research/science-and-research-institute/oral-health-topics/aging-and-dental-health. Updated November 9, 2021. Accessed September 27, 2022.