A Streamlined Cementation Technique for Indirect Glass Ceramics
Advanced resin cements offer a simplified glass-ceramic restoration process
The esthetics, biocompatibility, and durability of ceramic materials make them highly favored by many dentists and patients. In addition to these advantages, characteristics such as the materials’ chemical stability, high compressive resistance, and a thermal expansion similar to tooth structure help explain why these restorations are so useful to the clinician. These materials also have their drawbacks, however, including brittleness and a risk of fracture.1
When placing ceramic restorations, dentists must keep these advantages and disadvantages in mind and select the proper materials to help mitigate risks. The luting agent used with a ceramic material is one factor that can play a major role in the restoration’s ultimate success.1,2 Using the wrong luting material, or using the material incorrectly, can have a negative impact on the treatment’s longevity.3
Reviewing the Options
Cements have been organized into five categories: zinc phosphate, polycarboxlyate, glass ionomers, resin-modified glass ionomers, and resin-composite cements. Dentists should understand the benefits and drawbacks of each. In determining which type of material to use, the clinician should consider several factors, including the restorative material, the ability to control moisture, and whether the preparation design is retentive or adhesive.4
A luting agent (called such because it bonds to both the tooth and the restorative material)5 contributes to mechanical retention when the bonded surfaces interlock via pores and capillaries within the substrates. After polymerization of the luting agent, the undercuts of the pores prevent mobility between the bonded substrates.6 This type of luting works well with retentive preparations that have a large surface area, and are long and parallel or near parallel.1 Cements made with zinc phosphate, polycarboxlyate, and glass ionomers work principally through mechanical retention.6
However, as ceramic materials became more popular, it became clear that the adhesion power of these materials was not sufficient for tooth-colored restorations. These cements also did not provide a strong color match, and suffered from high solubility and abrasion. When used with cast gold restorations, these weaknesses were not an issue. But as the demand for tooth-colored materials increased, so did the need for a luting agent that could provide strong bonds to all surfaces, a good color match, and a marginal zone that could be polished.6
To meet today’s needs, an ideal cement should present biocompatibility, adhesion (the chief consideration for reduction in microleakage), resistance to marginal ditching, high bond strengths to dentin, radiopacity, consistent mixing, and a low film thickness.1 Resin cements and hybrid materials were introduced to meet these needs and particularly to provide a material that would offer adhesion, as opposed to simply mechanical retention.6 They have since become quite popular for these reasons.7,8
The Importance of Adhesion
In the early days of resin luting cements, some clinicians were slow to adopt the materials because of a perception that they were technique sensitive.9 Indeed, adhesive luting of tooth-colored restorations is complex. This is due to the fact that the luting material must connect the restoration to both enamel and dentin. Conditioning of the surfaces involved is required to maximize the chances of the restoration’s success. When conditioned properly, bond strengths of resin-based cements to ceramic surfaces have been found to be similar to the strength of the resin-enamel bond, provided that the ceramic surfaces are etched and silanated.6
Not only can adhesion help prevent microleakage, but it can also provide additional support to the tooth and the restoration via the adhesion at the interfaces between the cement and the restoration as well as between the cement and the dentin. This reinforcement gives the restoration better ability to distribute occlusal forces along the restoration and the tooth.6,10 Adhesive luting can also help compensate for clinical situations such as when the dentist does not achieve the ideal taper or crown height.9 The procedure has been recommended to improve clinical retention and marginal fit even in cases in which the restoration could be placed with a conventional cement.11
Proper adhesion technique must take the tooth surfaces carefully into account, particularly when acid-etching is involved. Although the practice is fairly straightforward on enamel, dentists have had to use special care when etching dentin. Acid-etching of dentin removes the smear layer and then causes demineralization of the upper layer of hydroxyapatite crystals, thereby increasing the surface energy. When adhesive is applied, the material’s resin monomers penetrate the areas between the collagen fibers and create a hybrid layer of collagen, resin, hydroxyapatite, and a small amount of water. This method of etching is recommended with two- and three-step adhesive systems.10 However, it has traditionally been extremely important to carefully control the level of moisture in this technique to avoid postoperative sensitivity.
It has been rightly pointed out that although a restoration may be functional and esthetically strong at the time of placement, even a small amount of postoperative sensitivity can raise doubts in the patient’s mind about the quality of the work. It is vital, therefore, for clinicians to select adhesive systems carefully and to use proper technique to help prevent this doubt.12
Curing Considerations
An examination of the polymerization qualities of resin cements reveals that they can be divided into three categories: chemically activated materials, light-cured cements, and dual-cured cements. The chemically activated cements are typically used with Maryland bridges and intraradicular posts, whereas light-cured cements are useful in placing veneers. Dual-cured cements have the broader functionality to be used with inlays, onlays, and crowns, and are ideal for luting because of their low solubility, high mechanical strength, and adhesive properties.10,13
With their extended working times and controlled polymerization, dual-cure systems work well with indirect tooth-colored restorations.6 They are also able to provide adequate polymerization in areas that light cannot reach. Data have shown, however, that light curing does result in better outcomes with dual-cure materials than relying solely on the chemical process. Light curing has been found to increase the degree of conversion and surface hardness of the material as well as reduce the wear of the cement.10
An Optimal Adhesive-Cement Combination
A recently introduced dual-cure adhesive resin cement, RelyX™ Ultimate Adhesive Resin Cement (3M ESPE, www.3mespe.com), was developed specifically for use in glass-ceramic cementation. The material has fewer components than other cementation systems, eliminating the need for up to four separate bottles in the operatory. The esthetics are quite good with glass-ceramic restorations, and the material also offers moisture tolerance, making it useful in difficult clinical situations. This cement is recommended for use with Scotchbond™ Universal Adhesive (3M ESPE), and the two are designed to work optimally together. A unique dark cure activator is integrated into the cement for use with the adhesive, so no separate activator is necessary when the two are used together.
The following case will demonstrate the simple use of this cement and adhesive system with a selective etch technique in the placement of a glass-ceramic inlay.
Case Presentation
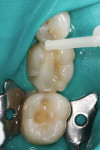
The patient presented to the office with a large fractured amalgam filling and fractured distal-lingual cusp on tooth No. 19. After consultation, it was decided to replace the amalgam filling with an indirect ceramic restoration made of lithium disilicate. The amalgam was removed (Figure 1). Vitrebond™ Light Cure Glass Ionomer Liner/Base (3M ESPE) was applied to seal the dentin. The liner was mixed and applied to the dentin surfaces in a thin layer, then cured for 30 seconds with a curing light. Impressions were taken and the case was sent to the laboratory.
Upon receipt of the finished restoration from the laboratory, the patient returned to the office for final placement. The surface of the inlay was prepared in accordance with the manufacturer’s instructions, and a rubber dam was placed for isolation.
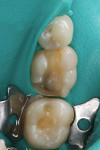
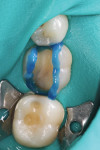
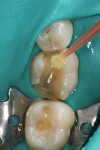
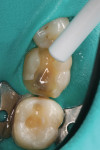
Selective enamel etching was performed with a 35% phosphoric acid etching gel and allowed to react for 10 seconds (Figure 2). The area was then rinsed with water and lightly dried. Scotchbond Universal adhesive was applied to the preparation on both the dentin and the enamel (Figure 3), air thinned (Figure 4), allowed to react for 20 seconds, and then air dried for 5 seconds. Because the adhesive was being used with RelyX Ultimate cement, neither a dual-cure activator nor light curing of the adhesive was necessary.
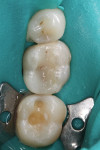
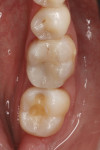
RelyX Ultimate cement was dispensed onto the preparation (Figure 5). The internal aspect of the onlay was scrubbed with Scotchbond Universal adhesive for 20 seconds, air dried for 5 seconds, and then seated in place and held in position for 20 seconds (Figure 6). The area was spot-tacked and excess cement around the edges and interproximal area was removed, followed by final curing of each surface for 20 seconds. Final polishing was then performed (Figure 7 and Figure 8).
Conclusion
As described, proper adhesion and cementation require an understanding of the properties at work in both the materials and the substrates. Typically, the products involved have been multi-component systems that demand careful attention to technique and chemistry. However, the new system used in this case helps significantly simplify the cementation procedure, and also contributes to a final outcome that is esthetically pleasing with no postoperative sensitivity.
References
1. Haddad MF, Rocha EP, Assuncão WG. Cementation of prosthetic restorations: from conventional cementation to dental bonding concept . J Craniofac Surg. 2011;22(3):952-958.
2. Hill EE. Dental cements for definitive luting: a review and practical clinical considerations . Dent Clin North Am. 2007;51(3):643-658.
3. Hill EE, Lott J. A clinically focused discussion of luting materials . Aust Dent J. 2011;56(suppl 1):S67-S76.
4. Radovic I, Monticelli F, Goracci C, et al. Self-adhesive resin cements: a literature review . J Adhes Dent. 2008;10(4):251-258.
5. Simon JF, Darnell LA. Considerations for proper selection of dental cements . Compend Contin Educ Dent. 2012;33(1):28-35.
6. Krämer N, Lohbauer U, Frankenberger R. Adhesive luting of indirect restorations . Am J Dent. 2000;13(Spec No):60D-76D.
7. Manso AP, Silva NR, Bonfante EA, et al. Cements and adhesives for all ceramic restorations . Dent Clin North Am. 2011;55(2):311-332.
8. Christensen GJ . Why use resin cements? J Am Dent Assoc. 2010;141(2):204-206.
9. Ferracane JL, Stansbury JW, Burke FJ. Self-adhesive resin cements-chemistry, properties and clinical considerations . J Oral Rehabil. 2011;38(4):295-314.
10. Santos GC Jr, Santos MJ, Rizkalla AS. Adhesive cementation of etchable ceramic esthetic restorations . J Can Dent Assoc. 2009;75(5):379-384.
11. Osorio R, Castillo-de Oyagüe R, Monticelli F, et al. Resistance to bond degradation between dual-cure resin cements and pre-treated sintered CAD-CAM dental ceramics . Med Oral Patol Oral Cir Bucal. 2012;17(4):e669-e677.
12. Pameijer CH. A review of luting agents . Int J Dent. 2012;2012:752-861.
13. Silva RA, Coutinho M, Cardozo PI, et al. Conventional dual-cure versus self-adhesive resin cements in dentin bond integrity . J Appl Oral Sci. 2011;19(4):355-362.
Robert Ritter, DMD
Private Practice
Jupiter, Florida