Management of a Unilateral Joint Trauma Case
Anterior deprogramming appliance facilitates restoration in centric relation
Georgia Haddad, DDS
The use of an anterior deprogramming appliance can be an effective protocol to find a reproducible and stable centric relation position for patients with severely traumatized or damaged temporomandibular joints who are undergoing therapeutic restoration.1 These removable, plastic appliances cover the hard palate and create a single point of contact between the lower central incisors and the anterior bite plane while disengaging the posterior teeth during function. When they are worn for a sufficient period of time, patients' jaw muscles relax and move into an optimal position with respect to their occlusion.
Case Report
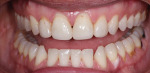
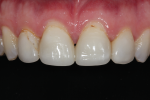
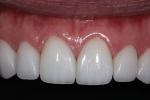
A 48-year-old female patient presented to the practice unhappy with the esthetics of her maxillary anterior teeth. Her chief complaint was the deterioration of her existing veneers, which were placed more than 10 years prior. She was also concerned about the disharmony of the periodontal architecture and the open cervical embrasure between her central incisors.
History and Clinical Examination
A clinical examination and a review of her dental history indicated active occlusal and functional issues. Further inquiry revealed a history of trauma to the left mandible, which resulted from an automobile accident that occurred 5 years prior to her visit. She stated that, since the accident, she had received chiropractic and Rolfing treatments to attempt to realign her jaw and relieve her pain.2 In addition, she had visited a physician who prescribed her pain medication. She reported transient pain relief from her chiropractic visits and noted that she would repeat treatment based on the return of her discomfort. Her pain score remained a 10 for the first few months but improved to a 3 thereafter. At the time of her presentation to our office, she stated that she was essentially pain free most of the time, but experienced intermittent awareness (ie, a pain score of 3) in her left jaw.
The patient's dental exam findings included the following:
• Minimal bone loss and acceptable oral hygiene (ie, low periodontal risk)
• Decay and erosion on more than 3 posterior teeth (ie, high biomechanical risk)
• An inconsistent maximal intercuspal position and wear facets on the posterior teeth (ie, high functional risk)
• Fremitus on teeth Nos. 8 and 9 with negligible lingual wear facets
• Faulty margins on the existing veneers on teeth Nos. 7, 8, 9, and 10 with a high smile line and lip mobility (ie, high dentofacial risk)
The patient's myofascial exam findings included the following:
• Mild awareness in the left temporomandibular joint area upon jaw mobility; not enough to render a positive result on an immobilization test
• A negative result on a load test
• A normal maximum interincisal opening (ie, 55 mm) and normal right and left lateral excursive movements (ie, 12 mm)
• No deviations upon opening
• No sounds upon opening or closing
• Right interferences during excursion
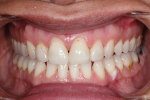
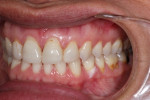
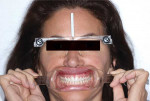
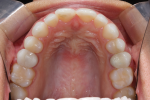
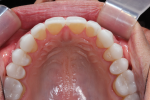
• An inconsistent maximal intercuspal position with deficiency of stable occlusal contacts in the left posterior (Figure 1 and Figure 2)
• Initial contact in the right posterior on tooth No. 2 following bimanual manipulation
Diagnosis and Treatment Planning
Although the patient was seeking treatment to address dental esthetic concerns, there was a definitive dysfunctional component that would require management in order to achieve predictability. After co-diagnosis of her condition and patient education regarding her potential solutions, an anterior deprogramming appliance (Kois Deprogrammer, Kois Center) was recommended to deprogram her muscles and place her into a consistent and reproducible restorative position from which we could begin our evaluation and make recommendations.3 The anterior deprogramming appliance was indicated to establish jaw relation records because the neuromusculature was asymptomatic and the load test was negative. Using an anterior deprogrammer for a patient who receives a positive score on a load test is contraindicated.
Record Taking and Appliance Therapy
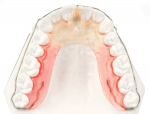
At the patient's records appointment, a complete series of radiographs and photographs were taken, as well as a vinyl polysiloxane impression with a bite record in maximum intercuspation. The deprogramming appliance was then fabricated, which incorporated palatal acrylic that extended in the anterior area to a 3-mm wide platform (Figure 3).
Two weeks later, the patient returned for deprogrammer delivery and instructions for use. The platform was adjusted to ensure a single contact point in the center. The patient stated that she felt comfortable, and she committed to wearing the deprogrammer full time except for when she was eating. She was also asked to record what she perceived was her first point of tooth contact upon the initial removal of the appliance each morning.
Once the patient achieved a consistent first point of contact for 4 consecutive days, she was instructed to return to our office for jaw relation records. Deprogramming of the patient's muscles4 and the establishment of a consistent, reproducible first point of contact was achieved in approximately 2 weeks, and a centric relation record was taken using bite registration wax (DeLar Bite Registration Sheet Wax, DeLar Corporation) with the deprogrammer in place intraorally.
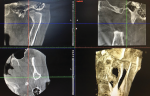
An occlusal analysis of the mounted diagnostic models revealed that the left posterior teeth demonstrated a complete lack of occlusal contact. Forensically, there were significant wear facets on teeth Nos. 4 and 5. Based on the patient's history of trauma, her immediate subsequent myofascial symptoms and occlusal changes, and the present occlusal analysis, it was determined that there was a need for additional imaging of the joint with magnetic resonance imaging (MRI)5 to definitively diagnose the anatomic conditions and histologic compromises that existed. Comprehensive examination of the patient's clinical conditions underscored the need for treatment solutions that went beyond correcting her chief complaint regarding the esthetics of her maxillary incisors. It became evident that the occlusal and functional component needed to be mitigated and corrected to allow for a good future prognosis of any anterior restoration.
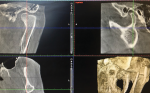
After evaluation of the MRI scan, it was discovered that there was trauma to the left joint complex and that the head of the condyle had undergone bone remodeling-a process consistent with anticipated osseous features associated with adaptive change. Given that the patient's symptoms had been resolved, additional surgical intervention to correct the anatomy was not indicated (Figure 4 and Figure 5).6
Restorative Treatment Planning
Having achieved what was clinically and symptomatically a stable jaw relationship, the balance of the patient's treatment plan focused on developing dental relationships that were congruent with her osseous arch relationships. This could have been accomplished through a combination of treatment options, including but not limited to orthodontics and restorative treatment.7 The patient did not wish to pursue orthodontic treatment, so she elected an exclusively restorative solution. The patient was informed that the ultimate goal of her treatment was to provide harmonious functional relationships despite the anatomical damage that existed. In addition, she was advised that, depending on the ongoing stability of the completed restorative solution, she might require future adjustments to balance the occlusal scheme due to the potential for additional adaptive changes in the joint. A complete restorative treatment plan was presented, including the following:
• A 14-unit functional, yet non-invasive (ie, minimal preparation and prep-less) wax-up of teeth Nos. 2 through 15 in centric relation
• Temporization for a minimum of 3 months in this centric relation position and a reestablishment of the left-side occlusion8
• The elimination of pain and any possibility of bite changes after the minimum 3-month temporization period
• Placement of conservative, all-ceramic final restorations
• Delivery of a maxillary splint for nighttime use
Clinical Records and Provisionalization
Due to the nature of this case and considering the adaptive anatomical joint changes, the decision was made to use centric relation as the restorative position.9 The deprogrammer was set at the necessary vertical position informed by the determined incisal edge position, opening the vertical dimension of occlusion by 0.5 mm in the anterior region.1
Next, facebow records (Kois Dento-Facial Analyzer and Facial Reference Glasses, Panadent) were taken and used to mount the case on an articulator (Model PCH Articulator with Kois Adjustable Platform, Panadent). The maxillary posterior occlusal plane was based on a horizontal line, starting from the anterior position determined by the deprogrammer and extending posteriorly to the existing position of the right first molar's buccal cusp.
The mandibular incisal edge and occlusal plane were not altered. To enhance the patient's smile design, her existing veneers on teeth Nos. 7 through 10 would be replaced, and minimal preparation and no-prep restorations were planned for teeth Nos. 2 through 6 and 11 through 15.10 The occlusal surfaces of teeth Nos. 2 through 6 were slightly altered to provide occlusal clearance for the restorations, but teeth Nos. 11 through 15 were left unaltered. These noninvasive restorations, which covered the buccal and occlusal surfaces, were determined to be the least compromising of tooth structure while accomplishing the functional and esthetic goals.
The existing veneers were removed from teeth Nos. 7 through 10, and a splinted provisional restoration was placed to cover the entire maxillary arch from tooth No. 2 to tooth No. 15. The deprogrammer was used to equilibrate the provisional restoration,11 and any interferences were removed to accommodate the patient's chewing pathway. Finally, oral hygiene instructions were provided, and a postoperative follow-up appointment was set for 1 week later to check the occlusion for any changes that may have occurred.
Follow-Up and Final Restorations
At the 1-week postoperative follow-up appointment, the patient's occlusal relationships were reevaluated (Figure 6). The occlusion remained unchanged, and the patient stated that it was comfortable. Centric occlusion was verified with the use of 7-μm shimstock paper, and no new interferences in her chewing pathway had developed. The deprogrammer was altered by removing the anterior bow, and it was able to be placed in the mouth identically because the lingual surfaces were not altered. Once in place, the coincidental reproducible point of contact on the anterior platform confirmed the lack of any occlusal changes. Subsequent follow-up appointments were set for every other consecutive week to check for any neuromuscular discomfort or changes in the occlusion. Three months later, the occlusion was confirmed to be stable, and the patient's dull myofascial discomfort/awareness had been eliminated. The decision was made to proceed with the definitive restorations.12
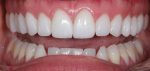
Based on the approved provisional restoration, all-ceramic final restorations (IPS e.max®, Ivoclar Vivadent) were fabricated, delivered, and checked for occlusal stability (Figure 7 through Figure 12). A maxillary splint was also fabricated and delivered to the patient for nighttime use. Subsequently, the patient's final restorations were checked at her next recare appointments. Although her preoperative risk assessment (ie, periodontal: low, biomechanical: high, functional: high, dentofacial: high) was relatively high, her postoperative risk assessment (ie, periodontal: low, biomechanical: medium, functional: medium, dentofacial: low) was much improved. The patient's occlusion and joint function have remained stable since delivery of the final restorations in September 2018.
Closing Remarks
An anterior deprogramming appliance is a powerful diagnostic tool that can be used to determine a stable restorative position in the presence of neuromuscular discomfort and joint trauma. When a patient who has a negative result on a load test presents with a joint that is severely damaged, the anterior platform of a deprogrammer is sufficient to provide a stabilization point as the joint undergoes adaptive change. A deprogrammer can also be used to determine a quantitative vertical position, which can act as a reference in the fabrication of provisional and definitive restorations.
About the Author
Georgia Haddad, DDS
Private Practice
Oxnard, California
References
1. Kois DE, Kois JC. Comprehensive risk-based diagnostically driven treatment planning: developing sequentially generated treatment. Dent Clin North Am. 2015;59(3):593-608. doi: 10.1016/j.cden.2015.03.001.
2. Tassorelli C, Tramontano M, Berlangieri M, et al. Assessing and treating primary headaches and cranio-facial pain in patients undergoing rehabilitation for neurological diseases. J Headache Pain. 2017;18(1):99. doi: 10.1186/s10194-017-0809-z.
3. Gnanashanmugham K, Saravanan B, Sukumar MR, Tajir TF. Gnathological splint therapy in temporomandibular joint disorder. J Pharm Bioallied Sci. 2015;7(5):314-318. doi: 10.4103/0975-7406.155972.
4. de Kanter RJ, Battistuzzi PG, Truin GJ. Temporo-mandibular disorders: "occlusion" matters! Pain Res Manag. 2018;2018:8746858. doi: 10.1155/2018/8746858.
5. Bag AK, Gaddikeri S, Singhal A, Hardin S, et al. Imaging of the temporomandibular joint: an update. World J Radiol. 2014;6(8):567-582. doi: 10.4329/wjr.v6.i8.567.
6. Soni A. Arthocentesis of temporomandibular joint- bridging the gap between non-surgical and surgical treatment. Ann Maxillofac Surg. 2019;9(1):158-167. doi: 10.4103/ams.ams_160_17.
7. Faus V, Faus-Matoses I, Jorques-Zafrilla A, Fraus-Llacer VJ. Orthodontics and veneers to restore the anterior guidance. A minimally invasive approach. J Clin Exp Dent. 2017;9(11):e1375-e1378. doi: 10.4317/jced.54358.
8. Milnar FJ, Using diagnostic wax-ups and provisional restorations when re-establishing canine function. Inside Dentistry. 2008;4(1):78-80.
9. Park I, Heo S, Koak J, Kim S. Post traumatic malocclusion and its prosthetic treatment. J Adv Prosthodont. 2010;2(3):88-91. doi: 10.4047/jap.2010.2.3.88.
10. Farias-Neto A, da Cunha Ferreira Gomes E, Sánchez-Ayala A, Sánchez-Ayala A. Esthetic rehabilitation of the smile with no-prep porcelain laminates and partial veneers. Case Rep Dent. 2015(9):1-6. doi: 10.1155/2015/452765.
11. Bynum JH. Clinical case report: testing occlusal management, previewing anterior esthetics, and staging rehabilitation with direct composite and Kois deprogrammer. Compen Contin Educ Dent. 2010;31(4):298-302, 304, 306.
12. Kois JC. New paradigms for anterior tooth preparation. Rationale and technique. Oral Health. 1998;88(4):19-22, 25-7, 29-30.