Management of the Incisal Edge
The key to functional and esthetic success in anterior restorations
According to Peter Dawson, DDS, founder of The Dawson Academy, “Determination of precisely correct incisal edges is the second most important decision a dentist must make regarding occlusion (centric relation is the first in importance).” The position of the incisal edges influences the esthetics of a patient’s smile, phonetic comfort, lip comfort, envelope of function, anterior guidance, posterior disclusion, and tooth contour. Therefore, it is critical to understand the rational for prosthodontic incisal edge placement.
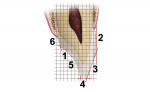
An excellent example of this rationale is the functional esthetic matrix as described by Dr. Dawson1 (Figure 1). The matrix is composed of the following six factors:
1. Lingual centric stop. This is an ideal holding contact contoured for the anterior teeth with the mandible in centric relation.
2. Gingival half of the labial surface. This tooth surface continues as an extension of the alveolar process, thus allowing a smooth and unaltered emergence profile.
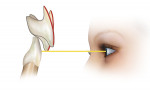
3. Horizontal position of the incisal edge. Minor variations in this position can greatly affect patient comfort and tooth stability. A slight change in the horizontal position can change the perceived length of the ncisors (Figure 2).
4. Vertical incisal position. The terminal position of the incisal plane is determined by combining the horizontal with the vertical position.
5. Lingual contour. This contour establishes the anterior guidance, which must be in harmony with the envelope of function. This area starts with the centric relation contact point and ends with the incisal edge position, and is the starting and ending point of the functional envelope.
6. Cingulum contour. This area from the gingiva to the centric stop should be smooth and care should be taken not to overcontour.
Planning for Functional Success
Managing complicated restorative situations can often be overwhelming. When a complex situation arises, it is often helpful to divide the problems of the case into manageable components. Predictable success is usually the product of a consistent methodology in the diagnosis and planning stages. It also allows patient and dentist participation in the exploratory process and will aid in both parties commitment to the outcome.
Data collected before prosthodontic restoration should include a complete medical and mental history, preoperative photographs, necessary radiographs, periodontal examination, diagnostic impressions, face-bow record, bite registration in centric relation and maximum intercuspation, and a complete maxillofacial exam with emphasis on the temporomandibular joint (TMJ) condition.2 Although the topic is beyond the scope of this article, the restorative philosophy of this author is based upon working in centric relation. When cases involve anterior reconstruction, often problems have arisen due to some form of instability in the patient’s occlusion. Therefore, effort is put forth to determine the health of the joints and to begin the restorative phase with the joints in centric relation. If stability is to be regained through the proposed treatment, stability must also be evident in the joints to allow long-term success.
Emphasis must be placed on pretreatment photographs obtained in the planning stages. This author uses at 21-photo series on most patients. With regards to the incisal edge position, five photographic shots are critical to the process: 1:3 full smile, 1:3 rest position, 1:3 “e” position, 1:3 full smile tip down, and 1:3 lateral 90° smile.
Factors Related to Position of the Incisal Edges
Anterior Envelope of Function and Anterior Guidance
The envelope of function determines the incisal edge position that then dictates the anterior guidance. The combination of the lingual contours and the position and inclination of the maxillary anterior teeth influence whether the relationship of the anterior guidance and envelope of function is harmonious. Improper positioning of the incisal edges can allow proper anterior guidance yet still interfere with the envelope of function.1
Neutral Zone
The neutral zone is the perioral complex composed of the soft tissues and muscles surrounding the mouth and the opposite pressure exerted by the tongue.3 Prosthodontic errors that violate the neutral zone can be very uncomfortable for a patient and start a chain reaction of compensations. Lip closure paths and muscle-induced function against the teeth must be considered.
Phonetics
The interaction of the lower lip against the incisal edges is critical for many proper speech sounds. Misplacement of the incisal edge can create speech difficulties and minor impediments.
Determining the Length of the Incisors
Vertical Incisal Edge Position
The maxillary incisors are often the starting point for smile rehabilitation. Diagnostic planning of this aspect should be precise, as it influences symmetry, proportion, and functional parameters of the adjacent anterior teeth.4 The final restored length will be influenced by a variety of individual factors. These include the lower lip position during smiling, the lip positions at rest, the lip positions in repose, upper lip characteristics, soft tissue characteristics, the envelope of function, and facial proportion.5
Depending on the preparation style or restorative product used, the length will set the foundation for the width-to-length ratio. An accepted ratio for width to length is approximately 80%.6,7 This also lays the foundation for establishment of the anterior golden proportion. Ideally, the width of the lateral incisor would be assigned a value of 1.0, the canine a value of 0.6, and central incisor a value of 1.6. This is an apparent measurement and should only be relied upon when viewing from the direct anterior. The canine’s value of 0.6 from the anterior is dictated from the facial line angles and height of contour. When viewed laterally, the canine would have a value much greater than 0.6.8
Determining the correct length can be very difficult in patients who present with a worn dentition. The length can only be estimated from known references and collected data. The patient must then test the result during the provisional phase. Studies of crown length have shown that unworn central incisors average 11.69 mm in length and worn centrals average 10.67 mm in length.9
The rest position is accomplished by having patients close their lips with relaxed facial muscles, and then slightly open their lips as if to breathe through their mouth. In this position, Vig and Brundo determined that men and women show average of 1.91 and 3.4 mm of central incisor, respectively.10 These amounts will decrease with advancing age as the soft tissues are more affected by gravity.10
The “e” position is a repose position created by the lips and musculature when having the patient say the long “e” sound. It is similar to a smile position, but simulates the position of the soft tissue in a more functioning position. Ideally, the incisal edge of the central incisor will fall between 50% and 70% of the distance between the upper and lower lip.
This author has found that a good starting point for the central incisor length is 10.5 to 11.0 mm. The “e” and rest positions are then used to determine the approximate vertical position to place the incisal edge. In many cases involving tooth wear, the patient will want longer looking teeth. Simply adding length to the incisal to achieve 10.5 to 11.0 mm will often result in encroachment on the envelope of function and the neutral zone.
Phonetically, the position of the incisal edge is important when considering the lower lip. The lower lip must interact with the incisal edge in a natural, effortless fashion. This is evident during the pronunciation of words beginning in the letters v and f. The incisal edge contact should occur in the moist or inner vermillion boarder of the lip and not the cutaneous or dry portion. This error can often been seen in restorations that are too long incisally.11
Horizontal Position of the Incisal Edge
Establishing the proper horizontal incisal edge position may be one of the most important yet most commonly overlooked factors in anterior reconstruction. This position must accommodate the patient’s envelope of function and neutral zone. A position too far to the facial can lead to interference as the lower lip closes to seal against the upper lip. A facialization error can also affect the function of the upper lip, causing the lip to “work around” the incisal edge. Many times the patient will complain of muscle fatigue and “a not quite right feeling” during function.
A lingualization error of the incisal edge can lead to an anterio-posterior constriction in the patient’s envelope of function. This would occur as the edges interfere with the lower incisors’ arc of closure.4,12 Similarity exists between the horizontal and vertical incisal edge positions in terms of phonetic issues. A horizontal discrepancy can also interfere with the production of “f” and “v” sounds.
In addition, the horizontal edge position must accommodate production of “s” sounds. These are created by squeezing air between the upper and lower incisors. Difficulty in creating this sound can be very frustrating for the patient.1,13 This author has found it to be a more common error with the edge position to the facial, and is usually caused by the preparation design error of failing to reduce anterior teeth in three planes. When the middle and incisal thirds are under-reduced, the lab technician has no choice but to fabricate an overcontoured restoration. Reduction stents can be produced from the diagnostic wax-up to aid in proper reduction depths.
Communicating with the Dental Ceramist
To create predictable success, the laboratory and ceramist must also be a vital part of the process. The technician needs to have a working mastery of functional smile design. Only then can the doctor and technician communicate effectively.
The necessary information to communicate incisal edge position effectively includes preoperative photos, preparation photos, and photographs of the provisional restorations. Impressions of the provisional restorations are an absolute deal breaker. The ceramist must have a reference point to begin the functional contours of the final restorations. Putty stents can be made of the provisional to exactly duplicate the position of the incisal edges and functional contours of the teeth. In addition, a face-bow of the provisional restorations should be included. The face-bow allows a 3D transfer of the maxilla (this includes the incisal edges) and TMJ to the articulator. The face-bow also allows recording of the condylar axis of rotation. This is absolutely necessary when using an open bite record such as in centric relation.1
Incisal Edge Position Errors
Facial Position
As previously mentioned, when the incisal edge is restored too far to the facial, the patient may complain of teeth feeling too long, dry, or in the way of the upper lip. The lower lip may feel overworked or that it must overextend forward to meet the incisal edge when articulating “f” and “v” sounds. Evidence may be found in these cases that the edges are interacting with the dry or cutaneous portion of the lower lip. In addition, the patient may have trouble producing “s” sounds as the mandible strains to get close to the malpositioned incisal edges. In short, this author has found that a facial error produces complaints mostly regarding patients’ feel and phonetic function.
Lingual Position
Errors of lingual position will often be evident from problems associated with restoration failure. With these errors, the edges will hit first in the patients arc of closure. Chipping of porcelain and debonding of the restorations are commonly seen in these cases. Problems with provisional restorations breaking or coming off can be an early warning sign that contour changes are needed. Issues with provisionals should not be view as an aggravation, but rather as a chance to refine positions and correct problems before they become set in porcelain. Be cautious when patients complain of feeling their teeth hitting wrong even when it only occasionally happens. The patient’s lower lip may also be overworking to the lingual to interact with the lingualized edges. Difficulty may also be encountered during pronunciation of “s” sounds because teeth nip each other in this malposition.
Properly contoured and patient tested provisional restorations are the only way to test the correctness of the incisal edge position. Patients often try to rush the process and want to limit the time in provisionals. Proper patient education and production of high quality temporaries will ease this process and provide the necessary information.
Case 1
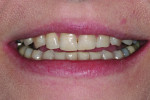
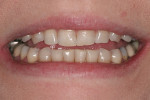
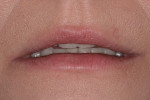
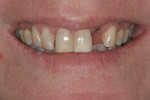
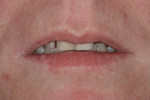
A patient presented with advanced breakdown of her anterior teeth (Figure 3). She had posterior centric relation interference, resulting in advanced lingual wear of the maxillary anterior teeth and incisal edges of the mandibular teeth. In addition, a nocturnal bruxing habit caused advanced maxillary incisal edge wear. With so much instability present, it was critical to place the incisal edges in an esthetic and functionally correct position.
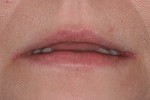
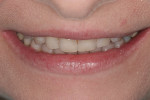
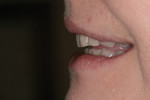
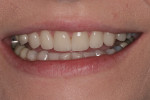
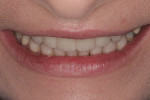
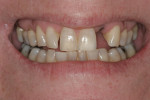
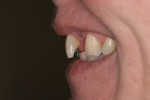
The patient’s rest position photo (Figure 4) showed zero tooth display. The “e” position photo (Figure 5) revealed the incisors to be at a 45% position. Both photos confirmed the loss of tooth structure to wear and showed that 1.0 to 1.5 mm of length could be added vertically at the incisal edge. The tip down photo (Figure 6) and the 90° photo (Figure 7) both show the horizontal edge position to be acceptable (a trajectory of the edge towards the inner border of the lower lip).
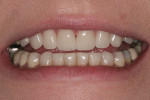
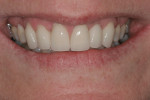
The treatment for this patient included equilibration of the occlusion to eliminate the centric relation to maximum intercuspation slide. Treatment included recontouring and creating incisal edge composite restorations for the mandibular incisal edges; lithium disilicate crowns were prepared for teeth No. 6 through No. 11. Based on the four functional photos, 1.5 mm of length was added vertically in the current horizontal plane of the maxillary incisors. These incisal changes were tested and confirmed in the provisional restorations, and then transferred to the definitive restorations. The postoperative result and functional photos are seen in Figure 8 through Figure 11.
Case 2
A patient who lost tooth No. 10 due to localized severe periodontal disease presented to the dental office (Figure 12). Once periodontal treatment was completed, the patient desired to have tooth No. 10 replaced with an implant and also considered cosmetic improvement to her remaining maxillary anterior teeth.
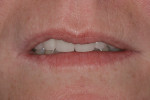
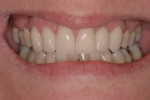
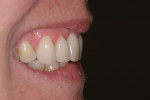
The patient’s rest position photo (Figure 13) revealed excessive tooth display of 4.5 mm. The “e” position photo (Figure 14) showed the incisors at the 75% position. Both photos confirmed that shortening the maxillary anterior teeth would make the centrals less dominant and allow better proportion and a more balanced smile. Both the tip down and 90° photos (Figure 15) confirmed that the incisal edges were too far to the facial. Excessive length and a facial bias resulted in the maxillary incisors functioning against the cutaneous portion of the lower lip.
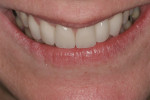
The patient was equilibrated to eliminate a centric relation/maximum intercuspation slide, and teeth No. 6 through No. 11 were restored with lithium disilicate crowns and veneers. The definite treatment shortened the maxillary centrals by 1.2 mm and lingualized the incisal edges. Better symmetry and proportion resulted in an enhanced looking smile. This eliminated what the patient described as her “Bugs Bunny” teeth. The postoperative results and functional photos are seen in Figure 16 through Figure 20.
Conclusion
Patients often present with esthetic issues that occur as a result of functional deficiencies. Restoring the incisal edge into a correct position will not only create a better looking smile, but a functional smile as well. Thinking about the 3D matrix of anterior teeth will allow restorations in the functional zone to be predictable for the patient and the dentist.
References
1. Dawson P. Functional Occlusion. In: TMJ to Smile Design. St. Louis, MO: Mosby; 2006:141-181.
2. Hess L. Restoring the Functional Zone: Correcting anterior constriction with centric relation-based prosthodontics. Inside Dentistry. 2007;3(9):74-79.
3. Dawson P. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St. Louis, Mo: Mosby; 1989:330.
4. Hess L. Esthetic Conservation: A smile makeover does not always have to be extreme. Inside Dentistry. 2007;3(2):74-79.
5. Hess L. Interdisciplinary synergy: managing complex treatment objectives for a predictable esthetic result. Advanced Esthetics and Interdisciplinary Dentistry. 2006;2(2):10-18.
6. Chiche GJ, Pinault A. Esthetics of Fixed Anterior Prosthodontics. Hanover Park, IL: Quintessence Publishing Co;1994:23.
7. Wolfart S, Thormann H, Freitag S, et al. Assessment of dental appearance following changes in incisor proportions. Eur J Oral Sci. 2005;113(2):159-165.
8. Ascheim KW, Dale BG. Esthetic Dentistry: A Clinical Approach to Techniques and Materials. 2nd ed. St. Louis, Mo.:Mosby;2000:31.
9. Mange P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89(5):453-461.
10. Vig RG, Brundo CG. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
11. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, IL: Quintessence Pub. Co.;1994:21.
12. Cranham J. The Horizontal position of the maxillary incisal edge: the key to optimum esthetics, phonetics, and function. Contemporary Esthetics and Restorative Practice. 2006;10(2):22-24.
13. Hess L. The relevance of occlusion in the golden age of esthetics. Inside Dentistry. 2008;4(2):36-44.
About the Author
Leonard A. Hess, DDS
Private Practice
Monroe, North Carolina
Senior Faculty
The Dawson Academy
St. Petersburg, Florida