Treating Carious White Spot Lesions
Flowable composite offers ease of placement with bioactive benefits
Ron Kaminer, DDS
Areas of enamel demineralization, more commonly termed "white spot lesions" because of their dense white appearance, are frequently caused by a buildup of bacterial plaque. They can also occur as a result of a genetic or developmental abnormality. White spot lesions are an established drawback of fixed orthodontic appliances and can appear within 1 month after placement.1 The presence of orthodontic appliances makes oral hygiene maintenance challenging, and hard-to-reach tooth surfaces can be especially problematic. This can lead to an increased likelihood of caries development that is usually not at risk for cavitation.2
Although Class V caries is commonly encountered in a restorative dental practice, predictable placement of a Class V restoration can be difficult.3 A significant challenge is the contraction of composite after light-curing, which can cause microleakage and staining, leading to cariogenic bacteria, postoperative sensitivity, and secondary caries.3,4 Another obstacle that dentists face is choosing the optimal material for high-risk caries patients; ideally, it should be easy to work with and capable of handling the high flexure of the tooth surface area, yet still be esthetically pleasing.
Today, clinicians have numerous direct restorative products from which to choose, and many have similar clinical characteristics. However, the use of a bioactive restorative material that can release and recharge beneficial ions can help protect restorations that are susceptible to recurrent caries and restorative failure.5
Case Report
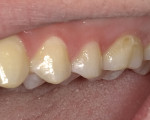
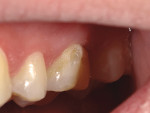
A new patient presented with a demineralized white spot lesion from an orthodontic bracket on tooth No. 14 that had become cavitated (Figure 1). A white spot lesion can be treated without marring the tooth if it is noncarious; however, once cavitated, it needs to be restored with either resin-modified glass ionomer or composite, and in severe cases, tooth reduction and veneer placement may be necessary.1,6 To evaluate whether a white spot lesion is cavitated or not, the tooth surface must be cleaned and dried.6 Carious white spot lesions are usually rough and porous in appearance, whereas noncarious ones are frequently smooth and shiny.6
Treatment options were discussed with the patient, and a mutual decision was made to restore the tooth using bioactive composite material to prevent further deterioration of the tooth structure and maintain an esthetically acceptable appearance.
Oftentimes, gaining access to and achieving isolation of a buccal lesion on tooth No. 14 can be difficult. Ideally, a rubber dam is used to isolate the tooth; however, cotton rolls or a dry shield are sufficient options to keep the cheek and moisture away from the area. Because access is a factor, a flowable composite would be well-suited for the treatment of this type of lesion due to its ease of placement.
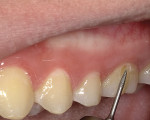
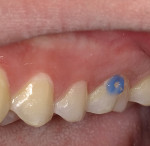
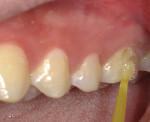
The existing decay was removed using a 330 carbide bur (NeoBurr® Carbide, Microcopy). To create a gradual transition between the tooth structure and restorative material that would enhance retention and prevent microleakage, the buccal surface of the tooth was beveled 2 mm on all sides (ie, occlusal, mesial, distal, cervical) using a flame-shaped diamond (NeoDiamond® Burs, Microcopy) (Figure 2).7 After the bevel was completed, the preparation was selectively etched at the periphery of the enamel using 35% phosphoric acid (Ultra-Etch™, Ultradent Products, Inc) for 15 seconds and rinsed with water (Figure 3). Next, the enamel was air-dried, and a bonding agent (BeautiBond®, Shofu Dental Corporation) was placed on both the enamel and dentin using a microbrush for 10 seconds (Figure 4). Following application, the bonding agent was gently air-dried for 3 seconds, air-dried with more force, and finally, light-cured for 5 seconds with a light-emitting diode (LED) curing light (Figure 5).
Once the bonding agent was cured, a highly viscous injectable hybrid composite (Beautifil Flow Plus® X [F00, shade A2], Shofu Dental Corporation) was syringed directly into the preparation to the cavosurface margin and light-cured with an LED curing light for 20 seconds (Figure 6). This flowable composite allows for precision stacking that will not spill out of the preparation, which is particularly important when working at an awkward angle on the buccal surface.
Conclusion
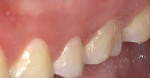
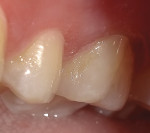
Following composite placement, the restoration was efficiently contoured, finished, and polished using an 8-mm polishing disc system (Super-Snap X-Treme™ Ultra-Gloss Performance Kit, Shofu Dental Corporation). The restorative material blended beautifully with the surrounding tooth surface and an exceptionally high luster was attained (Figure 7).
About the Author
Ron Kaminer, DDS
Private Practice
Hewlett and Oceanside, New York
For more information, contact:
Shofu Dental Corporation
shofu.com
800-827-4638
References
1. Miller MJ, Bernstein S, Colaiacovo SL, et al. Demineralized white spot lesions: an unmet challenge for orthodontists. Semin Orthod. 2016;22(3):193-204.
2. Heymann GC, Grauer D. A contemporary review of white spot lesions in orthodontics. J Esthet Restor Dent. 2013;25(2):85-95.
3. Spear F. Treating class V lesions. Spear website. https://www.speareducation.com/spear-review/2013/
03/treating-class-v-lesions. Published July 27, 2017. Accessed May 20, 2019.
4. Umer F, Khan FR. Postoperative sensitivity in class V composite restorations: comparing soft start vs. constant curing modes of LED. J Conserv Dent. 2011;14
(1):76-79.
5. Lowe RA. "Smart" class V preparation design for direct composites. Dentistry Today website. https://www.dentistrytoday.com/restorative-134/10037-smart-class-v-preparation-design-for-direct-composites. Published February 1, 2015. Accessed May 20, 2019.
6. Readers' Forum, Ask Us. Am J Orthod Dentofacial Orthop. 2010;138(6):690-696.
7. Swanson TK, Feigal RJ, Tantbirojn D, Hodges JS. Effect of adhesive systems and bevel on enamel margin integrity in primary and permanent teeth. Pediatr Dent. 2008;30(2):134-140.