Addressing Excessive Wear and Discoloration
Anterior guidance and occlusal guard protect restorations from future bruxism
Tyler Wynne, DDS
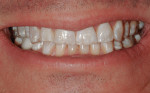
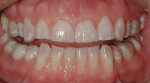
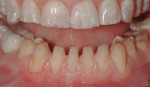
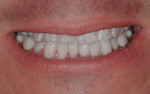
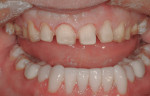
Apatient presented to the office with concerns about the excessive wear and generalized discoloration of his dentition (Figure 1). His maxillary teeth had lost approximately 3 mm of vertical length, which resulted in a smile that appeared much older than he actually was (Figure 2 and Figure 3). He stated that his primary treatment goal was to improve the esthetics of his worn anterior teeth.
Diagnosis andTreatment Planning
Identification of the etiology of the wear is an essential first step in the evaluation of a worn dentition. After eliminating biocorrosion (ie, the chemical, biochemical, and electrochemical degradation of tooth substance caused by endogenous and exogenous acids) and abrasive wear, it was determined that parafunctional attrition was to blame for this patient's situation.1 Occlusal interferences, a restricted envelope of function, and central nervous system-associated dystonias are all potential triggers that can result in nonfunctional grinding of the mandibular teeth against the maxillary teeth in excusive movements.2 In this patient's case, posterior occlusal interferences and a lack of anterior guidance following orthodontic treatment were the triggers for his bruxism. Severe wear due to the teeth being held in a restricted functional alignment without anterior guidance is a common occurrence among postorthodontic patients.2,3 Although there is no single factor responsible for all bruxing and no single treatment that is effective for eliminating, or even reducing, all bruxing, there are reliable methods for reducing the effects of bruxing.2
The patient's smile also exhibited generalized hypocalcification and discoloration due to amelogenesis imperfecta, maxillary gingival zenith asymmetry, a lack of central dominance, and a 1:1 height-to-width ratio of the maxillary central incisors (Figure 3). Incisal embrasures affect the perception of the height-to-width ratio of anterior teeth, and as the vertical dimension of anterior teeth decreases, incisal embrasures disappear and an aged smile is the result. The progression of maxillary incisal edge wear compromises the esthetic principle of central dominance. Just as the mouth is the dominant feature of the face, the central incisors are the dominant feature of the smile; therefore, reestablishing ideal tooth form was essential to attaining an esthetic improvement in this case.4
During the examination, it was determined that both his right and left temporomandibular joints (TMJs) were free from the presence of intracapsular disorders and/or disc pathology. It is essential that the TMJs are functionally stable prior to proceeding with any functional or esthetic rehabilitation of the dentition. To confirm functional stability of the TMJs, first, the structural components of the joints are examined and the patient is asked about any history of clicking or symptomatic issues. Then, masticatory muscle palpation is performed, followed by Doppler auscultation, a range of motion assessment, and load testing in centric relation. From this TMJ exam, the disc shape and alignment, ligament health, masticatory musculature, joint space, and condylar bone anatomy were confirmed to be healthy (ie, Piper classification Stage I).2,5
In order to address the patient's esthetic concerns and reestablish functional harmony, the treatment plan involved placing 10 maxillary restorations (ie, 8 veneers and 2 onlays) and 9 mandibular restorations (ie, 8 veneers and 1 porcelain-fused-to-metal [PFM] crown), equilibrating his dentition, and fabricating a permissive occlusal splint to be worn at night for an indefinite period of time. No changes to the maxillary gingival zeniths would be made because the patient was not interested in correcting the gingival architecture asymmetry due to his low smile line. A pressable ceramic system (Authentic®, Jensen Dental) was selected for its strength, superior optical properties, conservative preparation design, and ability to block out discoloration. An Authentic BOO+ ingot was used for the 16 veneers (ie, teeth Nos. 4, 6 through 11, 13, 20, 22 through 27, and 29) and 2 onlays (ie, teeth Nos. 3 and 14), and an Authentic Pressable to Galileo high noble PFM crown was used to restore tooth No. 19.
Clinical Protocol
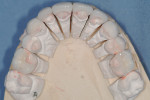
In order to provide maximum control over the placement of the mandibular incisal edge position and the establishment of a proper occlusal plane, the treatment began with the preparation of the mandibular teeth. Teeth Nos. 20, 22 through 27, and 29 were prepared with the goal of achieving a 0.8-mm facial reduction. This began with an initial 0.5-mm depth cut diamond (No. 900-7136, Henry Schein Inc.), after which a permanent marker was used to identify the 0.5 mm depth cuts to ensure precise, uniform reduction of 0.5 mm using a round-ended diamond (No. 112-5161, Henry Schein Inc.). Next, a 0.3-mm depth cut diamond (No. 900-7135, Henry Schein Inc.) was used, following the same protocol, to bring the total facial reduction to 0.8 mm. The contacts were cleared out with the round-ended diamond to provide the technician with the ability to straighten out canted midlines, add characterization, increase retention form, and leave the margins in an easy-to-clean area.6 Next, to achieve a 1.5-mm reduction at the incisal edge, a 0.75-mm diameter round-ended diamond was sunk to twice its depth. All line angles were smoothed and polished with a round diamond (No. 8878K-31, Brasseler USA), and a bite registration was taken in centric relation (Denar® bite registration wax, Whip Mix) (Figure 4). To provisionalize, a thermoplastic translucent matrix was utilized (Luxatemp®, DMG America).
During the diagnostic wax-up on the articulated casts, the lingual anatomy of teeth Nos. 6 through 11 was contoured to ensure predictable, balanced occlusal stops with the mandibular facial incisal edges and posterior disclusion upon canine-guided, lateral excursive movements. The protective mechanism of anterior guidance helps to prevent damaging posterior excursive interferences that can result in occlusal wear, abfractions, tooth mobility, and fractures. Achieving functional harmony by eliminating lateral forces affecting the posterior teeth and establishing vertical forces along their long axes is the healthiest for the periodontal ligament.7
During the provisional phase of treatment, the patient was provided with 0.12% chlorhexidine gluconate (Henry Schein Inc.) to rinse and brush with to promote gingival health. Even with well-adapted margins, temporaries can cause excessive gingival bleeding, and if not controlled after cementation, the color changes at the margins of all-ceramic restorations can compromise the esthetic result. If hemostasis is an issue during cementation, a hemostatic agent (Superoxol, Henry Schein) can be applied to the bleeding tissue for a few seconds, rinsed, and dried.
A total-etch protocol was followed to bond the restorations into place. After a 38% phosphoric gel (Etch-Rite™, Pulpdent) was applied to the preps for 20 seconds, washed, and air-dried, a dentin desensitizer was placed, followed by an application of primer and adhesive (Optibond™ FL, Kerr Corporation). After air-drying, the preparations were light-cured (Rembrandt Sapphire®, DenMat) for 20 seconds. To eliminate phosphate contamination from the try-in, the intaglio surfaces of the restorations were cleansed with a universal cleaning paste (Ivoclean, Ivoclar Vivadent) for 20 seconds. After the bonding surface was primed with a silane primer (Silane Primer, Kerr Corporation) and air-dried, the definitive veneers and crown were cemented (Calibra® Esthetic Resin Cement, Dentsply Sirona).
Maintaining the health of the gingiva requires a meticulous attention to marginal adaptation and an ideal transition from porcelain to natural tooth structure. To finish the margins, a red-striped 30-grit diamond (Brasseler USA) was used, followed by a yellow-striped 15-grit diamond (Brasseler USA) and a white-striped 30-blade finishing bur (Brasseler USA). To polish the margins, no-stripe, yellow-striped, and white-striped polishing points (Shofu Dental Corporation) were used in succession. To ensure interproximal finishing perfection, a Ceri-Saw™ (DenMat) and a red-striped Gateway™ Flexi diamond strip (Brasseler USA) were utilized, followed by Epitex® Strips (GC America) in a sequence of blue, green, gray, and tan, guaranteeing very smooth flossing and marginal adaptation (Figure 5).
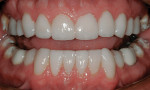
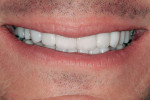
For the eight maxillary veneers and two onlays, an identical preparation sequence was followed as well as the same protocols for provisionalization, cementation of the final restorations, and finishing (Figure 6 and Figure 7). The final restorations transformed the patient's worn dentition into a youthful and healthy smile (Figure 6 through Figure 10).
It should be noted that the vertical dimension was not altered. Several studies have shown that vertical dimension is essentially unaffected by severe wear because elongation of the dentoalveolar process compensates for the lost vertical dimension of the abraded teeth.8 Therefore, a measurement from a fixed landmark on the zygoma to the cementoenamel junction of a maxillary molar will increase with tooth wear; however, a measurement from the same point on the zygoma to the occlusal surface will remain the same, even with severe wear.9 Crown lengthening to reestablish ideal height-to-width ratios and achieve proportions closer to the golden ratio is critical in anterior occlusal wear cases. Although crown lengthening was discussed during the treatment planning phase, the patient would experience little esthetic benefit by having this additional procedure due to his low smile line, so the decision was made not to perform it. Numerous esthetic guidelines exist and are promoted as essential for creating the idealized smile. Although some guidelines, such as those addressing the symmetry of maxillary central incisors and the correct vertical midline position, are absolutely vital for esthetic success, other rules for esthetics, such as the mandate for crown lengthening, can be disregarded if there will be no esthetic benefit realized by the patient, thus avoiding unnecessary overtreatment.
To protect the patient's new restorations and natural dentition from his bruxism, an equilibrated, soft/hard, maxillary permissive occlusal splint was fabricated and provided to him with instructions to wear it indefinitely when sleeping. The purpose of the splint was to obtain posterior disclusion, allowing for full seating of the condyles in the most anterosuperior position and permitting the lateral pterygoids to completely relax.10 The design of the splint accommodated four essential criteria: (1) balanced occlusal contacts in centric relation against the splint surface, (2) an anterior guidance ramp that permits excursive movements, (3) immediate disclusion of posterior teeth during excursive movements, and (4) a stable and comfortable fit.2 Although it has been shown that splints neither stop bruxism nor decrease the intensity of bruxism, they have been shown to redistribute the forces borne by the teeth and masticatory system and decrease the frequency of bruxing episodes.11
Conclusion
This patient desired an improved smile that appeared youthful and was free of wear and the effects of bruxism. Identifying the etiology of the wear to arrive at a correct diagnosis ensured appropriate treatment planning and restorative predictability. Successfully treating occlusal wear cases can be challenging; therefore, a detailed patient history and a long-term plan to manage the effects of bruxism are essential. The patient must be made aware that although the removal of posterior interferences and the establishment of a more harmonious occlusion with anterior guidance can help to reduce the triggers for bruxism, bruxism may still persist-even with an "ideal" occlusion. Consequently, patient compliance with occlusal guard instructions is an essential component of preserving dentition that has been restored after wear due to bruxism. All involved with this case were pleased with the results.
About the Author
Tyler Wynne, DDS
Private Practice
Clemmons, North Carolina
References
1. Grippo JO, Simring M, Coleman TA. Abfraction, abrasion, biocorrosion, and the enigma of noncarious cervical lesions: a 20-year perspective. J Esthet Restor Dent. 2012;24(1):10-23.
2. Dawson P. Functional Occlusion from TMJ to Smile Design. 3rd ed. Philadelphia, PA: Elsevier Health Sciences; 2007.
3. Cory F. The line and plane of occlusion. In: Continuum II. Miami, FL: Science X Medicine Publishing Company Inc; 1981:26.
4. Lombardi RE. The principles of visual perception and their clinical application to denture esthetics. J Prosthet Dent. 1973;29(4):358-382.
5. Dawson, PE, Piper, MA. Temporomandibular disorders and orofacial pain. In: Seminar manual. Center for Advanced Dental Study, St Petersburg; 1993:130-145.
6. Wynne T, Wynne WPD. A multifactorial approach to restorative dentistry. Inside Dentistry. 2015;11(6):72-78.
7. Schweikert EO. Anterior guidance. Quintessence Int. 1987;18(4):253-260.
8. Ahmad I. Geometric considerations in anterior dental aesthetics: restorative principles. Pract Periodontics Aesthetic Dent.1998;10(7):813-822.
9. Crothers A, Sandham A. Vertical height differences in subjects with severe dental wear. Eur J Orthod. 1993;15(6):519-525.
10. Dylina TJ. A common-sense approach to splint therapy. J Prosthet Dent. 2001;86(5):539-545.
11. Holmgren K, Sheikholeslam A, Riise C. Effect of a full-arch maxillary occlusal splint on parafunctional activity during sleep in patients with nocturnal bruxism and signs and symptoms of craniomandibular disorders. J Prosthet Dent. 1993;69(3):293-297.