Safety-Centric Sedation
Reducing sedation morbidity in the dental office
Robert C. Bosack, DDS
Anxiety and fear continue to fuel avoidance of necessary dental care. To help mitigate these issues, dentists may offer various types of analgesia/sedation, including nitrous oxide/oxygen analgesia, minimal or moderate enteral (oral) sedation, intravenous (IV) moderate or deep sedation, or general anesthesia. A clinician's training and license dictate the depth of sedation that can be offered, but the actual depth of sedation that is achieved can be unpredictable, which introduces an additional element of risk. Benzodiazepines, opioids, antihistamines, and hypnotics (among others) are administered orally or parenterally to achieve various levels of sedation (See Table).1 As depth of sedation and cardiopulmonary function both lie on a dose/patient-response continuum, some patients may not fit exactly into this scheme.
More importantly, movement between levels of sedation can be rapid and occur at unexpected doses. Because loss of airway tone and ventilatory insufficiency (ie, decrease in rate and depth) are expected, earlier-occurring side effects of these drugs-especially when given in higher doses or at faster rates or sequences-airway management becomes the cornerstone of patient safety.2 Hypoxia can result in irreversible injury and death within minutes; therefore, any deficiency in airway management during sedation becomes a time-urgent situation.
As a result of the wide variability in patient response, achieving and maintaining an appropriate level of sedation can be challenging. Because of this, the risks associated with sedation can become greater than those associated with the procedure that it was meant to enable, especially when patients descend to a deeper than intended level of sedation and clinicians fail to initiate drug reversal or interrupt the procedure to allow spontaneous recovery to a lighter level of sedation.
Levels of Sedation
The use of sedation instead of general anesthesia does not appear to improve airway safety.3-5 Just like patients under general anesthesia, those who have been deeply sedated can lose airway patency. And unlike the relaxed, paralyzed state of general anesthesia, prior to endotracheal intubation, a deeply sedated patient can present in an unrelaxed state with his or her mouth clenched closed, hampering the triple airway maneuver needed to open and gain visual access to the airway. Deeper than intended levels of sedation due to unintentional (ie, absolute or relative) overdose can be unexpected and not readily noticed or appreciated. The resultant respiratory depression (ie, a loss of airway patency and/or hypoventilation) triggers hypoxia, which also may not be immediately recognized or remediated. Bhananker et al concluded that at least 50% of the claims noted in their review of injury during monitored anesthesia care could have been prevented by better monitoring (including capnography), improved vigilance, and audible alarms.3 In addition, human error has been shown to often be contributory.6
It is important to be mindful of the fact that the "average" initial dose of any medication is determined from the normal distribution graph. Occasionally, patients can be hyperresponsive to a "normal" weight-based dose. Unintentional overdose is more likely to occur in patients at age and weight extremes; patients with eating disorders (eg, anorexia, bulimia), obstructive sleep apnea, or substance abuse disorders; patients who are taking psychotropic medications; and those who are temporarily hypovolemic from prolonged fasting or recent diuretic use, among others.
Loss of airway patency cannot always be predicted, but because it can occur among all patients at all levels of sedation, it should always be anticipated.
When challenged with the same anesthetic insult, less morbidity is expected with healthier patients than unhealthy ones, although this cannot be tested. Patients with normal lung volumes, especially when preoxygenated, can tolerate apnea for a longer period of time when compared with patients whose lung volumes are proportionally smaller, such as those affected by obesity, pulmonary disease (especially with recent exacerbation), cachexia, or young age. In addition, patients with coronary artery disease may be less able to tolerate the increased cardiac workload that accompanies hypertension or tachycardia, which can be triggered by hypoxemia or poorly conducted sedations.
Patients who are provided with supplemental oxygen prior to and during drug administration may be able to tolerate apnea for a longer period of time without experiencing hypoxemia, which can ostensibly provide the clinician with extra time (ie, a margin of safety) to remediate the ventilatory problem. However, because supplemental oxygen delays the onset of hypoxemia caused by apnea, it can also temporarily blind the clinician to the presence of apnea.
Risk Management
Although there is no readily attainable solution that eliminates the risks associated with sedation in the dental office, the following six "patient safety initiatives" can be implemented to minimize the risks and provide a blueprint to improve sedation safety:
1. Establish a Culture of Safety
Safety culture is defined by NASA as an "environment where everyone works safely, feels comfortable communicating safety issues, learns from mistakes and successes, feels confident balancing challenges and risks while keeping safety in the forefront, and trusts that safety is a priority."7 In any safety culture, there is a collective preoccupation with the possibility of failure, and errors are welcome and held in open view as a nonpunitive opportunity to improve systems that limit or minimize adversity. Efforts to sustain an effective safety culture should come from all entities, including the dentist and his or her team, state and national agencies, and professional organizations.8
2. Enhance Patient Selection
Patient selection is, by far, the most complex part of the safety equation. At first glance, it would appear that a healthy, athletic adolescent with a large airway space would be at less anesthetic risk than an obese, elderly, hypertensive, diabetic man with obstructive sleep apnea and a long history of cigarette smoking. However, healthy patients are still susceptible to airway compromise, aspiration, and pulmonary edema. When to "say no" becomes a more difficult question when patients present with less obvious or serious medical and anatomic challenges.
Sedation in the dental office is often elective, and it can be refused. Careful patient selection is initially guided by a thorough evaluation of the medical history and the physical examination. Patients are often unaware of the presence or severity of diseases, which can occur because they are undiagnosed, undisclosed, or forgotten. As such, any indication of a difficult airway should invite concern.
Among the many adverse events that can occur during office-based sedation, there are two that can be particularly dangerous. The first is drug-induced hypoventilation and/or loss of upper airway tone, and the second is adverse cardiovascular changes. With the notable exception of ketamine and the notable implication of opioids, anesthetic medications (especially when used in synergistic combination) can lead to a dose- or rate-of-administration-dependent loss of airway tone and hypoventilation/apnea, leading to hypoxemia, which initially triggers a sympathetic surge (ie, tachycardia and hypertension). Complex cardiovascular changes in heart rate and blood pressure also can occur secondary to both drug action and the neuroendocrine stress response of a poorly conducted anesthetic, triggering sympathetic surge. With this in mind, three parameters are assessed to inform appropriate patient selection:
Airway. Regardless of health status, airway and ventilatory compromise can occur in all patients. Multiple airway parameters should be assessed to inform decisions about case acceptance or depth of anesthesia limit setting. As part of a mandatory airway assessment, Mallampati scores should be recorded and heeded. Like other airway assessment tools, when considered on an individual basis, this score lacks both sensitivity and specificity; however, it should be included in a complete and thorough airway examination. Classic airway assessment for sedation seeks, at a minimum, to predict the likelihood of the following three situations: (1) spontaneous airway collapse after drug administration; (2) the ability to open a collapsed airway with a head-tilt/chin lift or jaw-thrust maneuver; and (3) the ability to attain an airtight facemask seal to allow positive pressure ventilation to stent a potentially collapsed airway. After an inspection of the size and position of the mandible, the maximal opening, level of jaw protrusion, and ability of the neck to extend are assessed. A visual intraoral inspection also should be performed to note the size and position of the tongue in the oropharynx. In addition, the size, tone, and mobility of the spaces surrounding the tongue should be evaluated. Can the tongue be displaced inferiorly or can the mandible be protruded to allow tongue displacement away from the posterior pharyngeal wall? A large tongue or tonsils can encroach, and teeth and trismus (ie, limited opening) can obscure the airway space. Small or retrusive mandibles and narrow palates crowd the tongue, and an inability to protrude the mandible and/or extend the neck will limit the ability to improve airway patency or access. Furthermore, the ability to seal a facemask and provide positive pressure ventilation can be hindered by age, jaw deformities, lack of teeth supporting the lips, facial hair, and a flat nasal bridge, among other factors.
Resilience. A patient's resilience is his or her physiologic ability to tolerate the insults associated with sedation and anesthesia. Apnea is less tolerated when patients have not been preoxygenated or have diminished functional residual lung capacity, whether from extreme age, obesity, pulmonary injury, anorexia, cachexia, skeletal malformations, or other causes. Hypotension is less tolerated in volume-depleted patients (eg, from prolonged fasting on a hot, humid day), in patients with underlying rhythm abnormalities, and in patients in the "beach chair" position, which can impede venous return and cardiac output. Hypertension and/or tachycardia increase myocardial oxygen demand-a situation that should be avoided with coronary artery disease, which limits myocardial oxygenation.
Reserve. A patient's reserve is his or her physiologic ability to compensate for hypoxemia, which is hampered by a loss of airway or opioid-induced hypoventilation, or hypotension, when a compensatory tachycardia, increased contractility, or vasoconstriction is hampered by opioids or beta-blockers. The topics of resilience and reserve are greatly expanded elsewhere.9
3. Set Limits on Depth of Anesthesia
Intended drug action occurs when drugs diffuse toward and bind to their receptor sites in the vessel-rich central nervous system, triggering responses such as anxiolysis, sedation, amnesia, analgesia, and/or hypnosis. Drug effect terminates once the drug diffuses away from its receptor site and undergoes metabolism or excretion. Regardless of the route of administration, drugs also accumulate in fat or muscle stores where they do not exert clinical effect. When drugs leave fat or muscle stores prior to metabolism or excretion, they can once again bind to central nervous system receptors to trigger a response. Therefore, slow-onset drugs that accumulate in fat or muscle stores become difficult to titrate, especially when administered orally, intramuscularly, or in patients with large fat or muscle stores. In these cases, impatient or repeated dosing can easily lead to overdose. A thorough understanding of pharmacokinetics combined with a "start low and go slow" approach minimizes the possibility of overdosing and facilitates depth of anesthesia limit setting.
Drug response is also difficult to predict because the dose and rate of administration effects fall on a normal distribution curve, inviting the possibility of a diminished or exaggerated drug response. It is known, however, that patients with obstructive sleep apnea are more sensitive to opioid-induced respiratory depression and that, without accounting for other parameters, elderly patients require a 50% to 75% initial dose reduction.10 An inadequate patient history as well as concealed or denied substance abuse disorders also challenge the predictability of drug response.
Patients should be made aware of depth of anesthesia limit setting and when the depth of anesthesia is limited by license, training/ability, troublesome airways, or patient resilience or reserve, warned about the possibility of subjective "undersedation."
4. Improve Patient Monitoring
Vigilance is the motto of the American Society of Anes-the-si-ologists.11 It is defined as the action or state of keeping "careful" and continuous watch for possible danger or difficulty. Anticipating critical events makes their timely resolution more likely. Perianesthetic visual patient observation, intermittent blood pressure recording, pulse oximetry, and continuous electrocardiography are standard and well-accepted means of monitoring moderate and deeper levels of sedation. Recommendations for the use of end-tidal capnography during moderate or deeper sedation have recently been made.12 It remains difficult, if not impossible, to demonstrate that robust monitoring does not improve outcomes, especially given the fact that patients can quickly and unexpectedly move between levels of sedation. Because it is well accepted that a sedation provider should be able to rescue patients who move one level deeper than intended, it is reasonable to recommend that patients be monitored in a way that is appropriate for one level deeper than the intended sedation. Because loss of airway tone and hypoventilation are expected side effects of most anesthetic agents, variation in patient response to medication remains an ever-present possibility, and most anesthetic morbidity in the dental office relates to hypoxemia, it seems advantageous to monitor these events with the utmost intensity. Pulse oximetry indirectly measures (with a delay of up to 30 seconds) the partial pressure of oxygen in the blood; capnography measures (with a 6- to 8-second delay) the depth, rate, and cadence of ventilation (and indirectly circulation) when exhaled carbon dioxide is captured; and pretracheal auscultation provides immediate information regarding changes in airway caliber and tone, based on the presence of adventitious breath sounds. Monitoring is optimized when all three of these methods are combined with continuous, visual patient inspection for chest movement and changes in skin color.
5. Rehearse Basic Emergency Airway Management
Expected adverse effects of most anesthetic agents include a loss of upper airway patency (ie, supraglottic obstruction) secondary to relaxation; inspiratory airway collapse; posterior displacement of the tongue, soft palate, and/or epiglottis; and hypoventilation or apnea. Any instance involving even a 1% drop in SpO2 should immediately be given full attention to ensure that oxygen delivery is occurring.
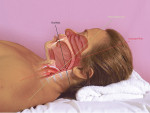
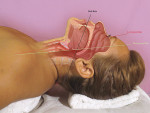
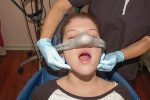
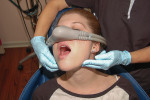
Basic techniques for recapturing a lost upper airway during sedation include noting and recording the time of obstruction, maintaining an open mouth, suctioning the oropharynx, ensuring the delivery of 100% oxygen, and attempting to arouse the patient. These should occur concurrently with the triple airway maneuver: flexion of the lower neck, extension of the upper neck, and protrusion or forward thrust of the mandible (Figure 1 and Figure 2). This manipulation is intended to pull the tongue, epiglottis, hyoid bone, and associated soft tissue forward to open or increase the caliber of the oropharynx and hypopharynx. When these maneuvers fail, the extended head can be rotated approximately 30º to either side to further facilitate airway opening (Figure 3 and Figure 4). When this fails, a full facemask with a self-inflating bag should be sealed over the mouth and nose. The bag is squeezed to force oxygen-enriched air into the airway, which hopefully stents the tongue and palate out of the way to allow oxygen entry into the lungs. Proper ventilation with a bag valve mask is the "brass ring" of airway management, thus it should be practiced often. Oropharyngeal or nasopharyngeal airways and supraglottic devices should be used when positive pressure ventilation cannot otherwise be achieved. Drug reversal can be entertained to awaken an obstructed patient; however, this would not be an initial approach and should not delay performance of the triple airway maneuver and bag valve mask ventilation.
It is important that the entire sedation team understands and frequently rehearses their roles and responsibilities concerning the flow of events and movement of devices during these sequential airway management techniques. During the crucial minutes of an adverse airway event, assistants should be able to act without waiting for prompts or directives from other team members. Protocols should be committed to memory and posted as checklists in highly visible locations.
6. Employ Crisis Resource Management
Crisis resource management involves a series of techniques, actions, and protocols for managing time-urgent, high-stakes events in the medical environment.13 These protocols seek to improve social, team-oriented, "nontechnical" skills as a viable mechanism to prevent deviations from safe practice from causing patient injury-making the environment (ie, systems) more "error resistant." The following are salient components of crisis resource management as it applies to sedation safety in the dental office2:
Anticipate and plan. Consistent with safety culture, practitioners should always plan for the worst-case scenario. Emergency scenarios should be anticipated, and rescue plans consistent with the nature of the practice should be devised and continually rehearsed by all staff. Known as simulation, this rehearsal is intended to reinforce roles, duties, movement of various devices, and protocols for the management of emergency situations.14 Frequent rehearsal improves the retention of these components. Errors that occur during simulation do not result in patient harm and can be noted to eliminate their recurrence. During simulation, psychomotor skills-such as airway interventions, electrical therapy, and auscultation-are best practiced on a manikin; however, manikin proficiency does not guarantee human proficiency. The key principle here is repeated practice.
Know the environment. Before commen-cing any patient treatment, a "time out" should be taken, during which all important features of the case are announced out loud for all to hear, including the patient's name, any health concerns, the status of the airway, the procedure to be performed, etc. At this time, an equipment check is also performed. This check should include monitors, back-up devices, connectors, gas sources, suction, and any other equipment to be used in the procedure.
Use all available information. During any emergency, the team leader must perceive and process all pertinent information, including vital signs, status of intravenous access, patient color, etc. Each team member should know his or her individual responsibilities before any emergent situation arises. Quick glances or fast checks can leave the leader with misinformation.
Allocate attention wisely. Optimal situational awareness allows the practitioner to remain informed of the entire environment while attending to a single problem. A repeating cycle of perceive/process/perform facilitates movement through a situation. Priorities can be set and changed as needed, reevaluation is frequent, and fixation errors are minimized. During an airway crisis, the first intervention is frequently, but sometimes erroneously, presumed to be the correct intervention, when in many cases, it is not.
Mobilize resources. These resources can include additional personnel (eg, colleagues, key staff members) and additional equipment, such as monitors, airway devices, or video laryngoscopes. For any case, at least one back-up airway plan should be formulated and immediately available.
Use cognitive aids. Performance decrement occurs almost universally in stressful, high-stakes, time-urgent situations. Mental and sometimes physical "situational paralysis" can occur, grossly interfering with thought processes. During these times, checklists can help jog memory and guide direction for crisis resolution. Checklists should be posted in visible locations for all to see.
Communicate effectively. During crises, demands or requests are often shouted out, but no one hears. Closed-loop, directed communication is the most effective in these situations (eg, "Mary, please check patient saturation." "Yes, doctor. I will check saturation. It is…"). Junior team members should not be hesitant to speak up; authority grids flatten when all intentions are focused on patient safety.
Distribute the workload. Practitioners need help during urgent airway situations and will not have the time or inclination to start assigning tasks in the moment of crisis. During these procedures, staff should be adequate, informed, and trained, and patient scheduling should be unhurried.
Call for help early. There is no shame in calling for help, such as from colleagues or through activation of the local emergency medical services. It does not indicate a lack of qualification. When a patient's life is at stake, it is always better to be safe than sorry, and this action should be praised.
Conclusion
Regardless of a patient's health status, the use of sedation and anesthesia can result in a compromised airway, associated morbidity, and without appropriate intervention, possibly even mortality. When employing sedation in the dental office, the use of effective risk management techniques, including enhanced patient selection, limits on depth of sedation, and improved patient monitoring can reduce the incidence of adverse events and improve safety.
Disclosure
The author received an honorarium from DENTSPLY for the preparation of this article.
About the Author
Robert C. Bosack, DDS
Private Practice
Orland Park, Illinois
References
1. American Society of Anesthesiologists Task Force on Sedation and Analgesia by Non-anesthesiologists. Practice Guidelines for Sedation and Analgesia by Non-Anesthesiologists. Anesthesiology. 2002;96(4):1004-1017.
2. Rall M, Dieckmann, P. Safety culture and crisis resource management in airway management: General principles to enhance patient safety in critical airway situations. Best Pract Res Clin Anaesthesiol. 2005;19(4):539-557.
3. Bhananker SM, Posner KL, Cheney FW, et al. Injury and liability associated with monitored anesthesia care: a closed claims analysis. Anesthesiology. 2006;104(2):228-234.
4. Cote CJ, Notterman DA, Karl HW, et al. Adverse sedation events in pediatrics: a critical incident analysis of contributing factors. Pediatrics. 2000;105(4 Pt 1):805-814.
5. Cote CJ, Karl HW, Notterman DA, et al. Adverse sedation events in pediatrics: analysis of medications used for sedation. Pediatrics. 2000;106(4):633-644.
6. McIlvaine WB. Human error and its impact on anesthesiology. J Crit Care. 2006;25(3):172-179.
7. Office of Safety and Mission Assurance. Safety Culture. 2015. https://sma.nasa.gov/sma-disciplines/safety-culture. Accessed Dec 3, 2015.
8. Arfanis K, Fioratou E, Smith A. Safety culture in anaesthesiology: Basic concepts and practical application. Best Pract Res Clin Anaesthesiol. 2011;25(2)229-238.
9. Bosack RC, Lieblich S, eds. Anesthesia Complications in the Dental Office. 2015; Wiley-Blackwell.
10. Mickelson SA. Preoperative and postoperative management of obstructive sleep apnea patients. Otolaryngol Clin North Am. 2007;40(4):877-889.
11. Bacon DR. Iconography in anesthesiology. The importance of society seals in the 1920s and 30s. Anesthesiology. 1996;85(2):414-419.
12. American Society of Anesthesiologists Committee on Standards and Practice Parameters. Standards for Basic Anesthetic Monitoring. October 2015. https://www.asahq.org/~/media/sites/asahq/files/public/resources/standards-guidelines/standards-for-basic-anesthetic-monitoring.pdf. Accessed Dec 3, 2015.
13. Howard SK, Gaba DM, Fish KJ, et al. Anesthesia crisis resource training: teaching anesthesiologists to handle critical incidents. Aviat Space Environ Med. 1992;63(9):763-770.
14. Ostergaard D, Dieckmann P, Lippert A. Simulation and CRM. Best Pract Res Clin Anaesthesiol. 2011;25(2):239-249.