Risk Assessment Criteria for Tooth Preservation and Protocols for Successful Reconstruction
Providing treatment for the compromised tooth
Alan M. Atlas, DMD | Samuel Kratchman, DMD
One of the more challenging dental procedures facing clinicians is the restoration of an endodontically treated tooth. This is mainly because of the complexity of the clinical techniques involved and the vast array of treatment options available. An extensive amount of scientific evidence deals with one or more of the components in this multifaceted procedure, but risk factors affecting outcomes are inconsistent in most clinical trials.
What is clearly evident is that successful long-term retention of endodontically treated teeth is dependent on adequate treatment in both the endodontic and restorative phases.1 In a systematic review and meta-analysis of the impact of the quality of the coronal restoration versus the quality of the root canal filling on the success of root canal treatment, Gillen and colleagues1 concluded that either variable, when completed inadequately, contributes equally to a poor outcome.
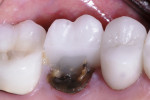
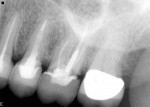
According to Ng and colleagues,2 four variables could help improve the survivability of an endodontically treated tooth: (1) a crown restoration after root canal treatment; (2) the existence of mesial and distal proximal contacts; (3) not using the tooth as an abutment for a fixed or removable partial denture; and (4) the tooth being other than a molar. After examining 46,000 insurance claims, Fennis and colleagues3 reported a higher occurrence of tooth fracture with endodontically treated teeth. When fractures of endodontically treated teeth are seen in a clinical setting (Figure 1 and Figure 2), the causative factors may be numerous.
Possible sources of tooth fracture include stresses that are attributed to endodontic and restorative procedures. These include overpreparation of the access cavity and canals, excess force during obturation, over-enlargement of the post space, and post selection.4 Other possible factors contributing to fracture are post adhesion, cement selection, parafunctional habits, patient age and gender, occlusal scheme and loads, and periodontal status. In a retrospective analysis of 50 teeth treated over 6 years with a minimum 4-year follow-up full-mouth series, Setzer and colleagues5 examined the restorative, periodontal, and endodontic parameters for the success of endodontically treated molars. They determined that a reduced periodontal prognosis and a loss of attachment were the only factors significantly correlated with failure of the endodontically treated teeth. Also, Vire6 and Fonzar7 concluded in their analyses that the most common reasons for extracting endodontically treated teeth were periodontal in nature.
Treatment Planning Considerations
After a tooth is excavated of all carious dentin and enamel, it may be considerably compromised due to loss of structural integrity. Thus, evaluating the amount of remaining healthy tooth structure becomes the first critical treatment planning step in order to determine if enough of it remains to support the foundational core for an eventual coronal restoration. Can the tooth be salvaged? Has endodontic therapy been initiated? Or should extraction followed by implant placement be considered? Has the patient been offered a fixed or removable partial denture? Because significant scientific evidence suggests favorable results with dental implants, some clinicians may be less familiar or comfortable with the long-term outcomes of restoring compromised teeth. Setzer and Kim8 compared the long-term survival of implants and endodontically treated teeth and concluded that both treatment modalities are equally successful.
In evaluating the oral-systemic condition of the patient, the clinician must decide if smoking, diabetes, bisphosphonate use, systemic steroid therapy, radiation therapy, hypertension, polypharmacy, high caries index, or xerostomia may affect the long-term outcomes for either option based on the scientific evidence. Chrcanovic and colleagues9 concluded in a recent systematic review and meta-analysis that smoking negatively affects outcomes of implant treatment.
The clinician must also assess pulpal and periodontal status as well as bone quality. If adjunctive procedures such as grafting and bone augmentation or sinus lifts are needed, they may preclude favorable outcomes for dental implants and instead favor tooth preservation. Other factors affecting decision-making processes include the age and gender of the patient, the intended tooth function, occlusal scheme, directional forces based on the tooth location, and parafunction.
For proper treatment planning, the restorative dentist must carefully assess the quality and quantity of available tooth structure and integrate all risk assessment variables to anticipate the final restoration prior to beginning endodontics. When all other patient factors are acceptable, the decision to retain and restore a severely damaged tooth is ultimately based on the capacity to preserve intact coronal and radicular tooth structure and to keep adequate cervical tissue so that a ferrule effect can be provided, which is critical for optimizing the biomechanical behavior of the restored tooth.
The Ferrule Effect
First described by Rosen10 in 1961, the ferrule effect involves use of a 360° metal collar on the crown that surrounds the parallel walls of the dentin. The collar extends beyond the gingival margin and coronally to the shoulder of the preparation. This results in the bracing of the crown over the tooth structure’s increased resistance form, reduced internal tooth stresses, and protection against fracture. Optimal requirements for the ferrule effect so that an improved prognosis can be gained include healthy dentin circumferentially extending 1.5 mm to 2 mm coronally to the margin of the crown, thereby requiring 5 mm of tooth structure coronal to the alveolar crest.
It is generally presumed that the dentin wall supporting the core should have a minimal thickness of 1 mm; however, few studies actually confirm this. If the clinical situation does not permit an ideal circumferential ferrule, an incomplete ferrule (of at least 180°) is considered a better option than no ferrule at all in providing fracture resistance for an endodontically treated tooth.11-16 When insufficient coronal tissue remains, orthodontic extrusion or surgical crown lengthening may provide an adequate clinical crown length and ferrule height. Orthodontic extrusion is preferable because it preserves more tooth structure, has less adverse effects on esthetics, and ensures a more favorable biomechanical behavior. Unfortunately, this extremely predictable and economical procedure is a dying art in an era when all too many teeth are simply extracted for eventual implant placement. Even so, when restoring teeth that have lost substantial hard tissue, it may be necessary to create a ferrule in the form of a beveled preparation margin, even at the expense of remaining tooth structure.
There has not been enough study on the ferrule effect on multirooted teeth to offer definitive conclusions. The ferrule effect is just part of the overall, complex equation for success; the choice of a post-and-core system, cement luting agent, and final crown substrate are also significant factors.
Access and Obturation
The loss of structural integrity is a primary reason why endodontically treated teeth can be more prone to fracture. To preserve tooth structure, the clinician must take great care in performing access preparation, especially when searching for calcified canals. Over-instrumentation of root canals may result in root fractures.17
The operating microscope has become a necessity for conservative endodontic access. Perrin and colleagues18 evaluated the influence of loupes and microscopes in endodontic therapy and concluded that only the dental microscope enabled significant visual enhancement of root canal anatomy, irrespective of the dentist’s age.
Sealing off the access is essential in preventing the bacteria from saliva from infiltrating the canal system.19-21 Ferreira and colleagues22 concluded that using a dental microscope while performing mechanical cleaning during post space preparation helped improve the bond strength of fiber posts to dentin. The endodontic–restorative connection is synchronized and simplified with the dental microscope by either immediate post space preparation followed by post-and-core placement or immediate placement of a core material.
Role of Bioceramics
Even though this article focuses more on the restoration of endodontically treated teeth and not endodontic techniques, it is important to discuss the use of bioceramics in endodontics. Bioceramics have been around since the late 1960s, initially used in medicine for their ability to form hydroxyapatite. The introduction of bioceramics in endodontics came in 1990 with Torabinejad’s creation of mineral trioxide aggregate. The second generation of bioceramics is being used for root-end surgery, perforation repair, pulp capping, revascularization, and, more recently, as a root canal sealer and obturation material.
The goal of bioceramics is to take advantage of their bioactivity to elicit a biological response at the material–tissue interface, resulting in the development of a “biological bond” or a “monobloc” interface between sealer, obturation material, and the dentinal walls. The sealer material is bioactive during the hydration process (the moisture naturally in the root canal and dentinal tubules initiates and completes the setting reaction) and biostable upon setting. This, along with its hydrophilic nature and resistance to wash out, makes a bioceramic sealer the ideal filling material for root canals.
To Post or Not to Post?
After obturation, the next issue is when and how to restore the endodontically treated tooth to maximize both quality and efficiency for the patient. The most common practice by endodontists is to place a cotton pellet in the root canal chamber and a temporary restoration in the access cavity. However, whether or not the endodontic treatment is performed by a specialist or the restorative dentist, the authors recommend completion of immediate post space preparation for either immediate or delayed post and core placement or completion of just the foundational core build-up at the time of obturation.
Following endodontic treatment, the decision for post placement is based on the authors’ risk assessment criteria: location of the tooth, occlusal loads and habits, remaining tooth structure, age and gender of the patient, and whether the tooth is intended to support a single crown or is to be used as an abutment for a fixed or removable partial denture.
The first critical factor for the restoring clinician is determining the number of walls of tooth structure that remain to retain the foundation for the permanent restoration. It is also important to determine how many walls of tooth structure will remain after preparation for the final crown. When coronal tooth structure loss is minimal and the marginal ridges are intact, a bonded composite resin is suitable to seal the access cavity without further intervention. This is most likely the restoration for an anterior tooth, as the two main factors that differentiate anterior and posterior teeth are their dimensions and direction of forces.
As mentioned above, in addition to the quantity and quality of remaining tooth structure, directional forces based on tooth location and occlusal scheme as well as parafunctional habits should be taken into account while treatment planning. Lateral, horizontal, or oblique forces generated at various angles less than 90° are more destructive and can lead to greater failures when compared to vertical loads.23 With respect to the access cavity for molars, occlusion-related factors play a pivotal role in deciding the type of definitive restoration. It must be determined if a composite resin restoration will be sufficient to withstand the patient’s masticatory forces or whether the composite resin restoration should be used as the foundational crown build-up. In posterior teeth, long cuspal heights and group function may cause greater lateral forces compared to canine-protected occlusions.24 For anterior teeth, deep overbites, a horizontal envelope of function, and extreme parafunctional forces may heighten the possibility of fracture and subsequent tooth loss.
In a study of 220 endodontically treated molars that were not restored with crowns, the success rates were 96% at 1 year, 88% at 2 years, and 36% at 5 years.25 When maximum tooth structure was retained for the direct composite restoration, the survival rate was 78% at 5 years.25 In another study it was concluded that teeth with cuspal coverage had a six times greater survival rate than teeth without cuspal coverage.26 Deciding whether to place a crown or only use a direct composite restoration depends on additional factors previously mentioned, other than remaining tooth structure. Cusp preservation, however, does not always result in low fracture resistance in the long term for an endodontically treated tooth.
Recently, Murgueitio and Avila-Ortiz27 proposed a classification for endodontically treated anterior teeth that took into account the wall thickness and height of the abutment based on ferrule principles. Therapeutic guidelines were summarized based on the classification and the canal diameter of the teeth. This classification may serve to establish a comprehensive treatment plan and accurate prognosis for endodontically treated anterior teeth; this may be helpful for inter-clinician communication and standardized comparisons in clinical research.27
When two or more walls of a tooth are missing after caries excavation and endodontic treatment, a post is usually required for retention of the core foundation along with the final coronal restoration. This also helps to distribute occlusal stresses along the remaining tooth structure. The details of executing this clinical procedure have been the focus of controversy regarding the necessity of posts and the best types to use. It has been shown in the literature that posts do not strengthen a tooth.28 In fact, it is known that post space preparation weakens the radicular structure and may increase the risk of root fractures;28 therefore, post placement should always be balanced against tooth structure removal when selecting the most suitable build-up approach. It has been proven that the use of fiber posts does not improve the fracture resistance of endodontically treated teeth in which a ferrule has been preserved.28 Preservation of tooth structure is the most critical facet of successful management of structurally compromised, endodontically treated teeth. Posts should only be used when other options are not available to retain a core, such as teeth without any ferrule. In such cases, fiber posts may improve the retention and fatigue resistance of the restoration but may not necessarily improve the tooth’s fracture resistance.28
Disclosure
The authors have no relevant conflicts of interest to disclose.
References
1. Gillen BM, Looney SW, Gu LS, et al. Impact of the quality of coronal restoration versus the quality of root canal fillings on success of root canal treatment: a systematic review and meta-analysis. J Endod. 2011;37(7):895-902.
2. Ng YL, Mann V, Gulabivala K. Tooth survival following non-surgical root canal treatment: a systematic review of the literature. Int Endod J. 2010;43(3): 171-189.
3. Fennis WM, Kuijs RH, Kreulen CM. A survey of cusp fractures in a population of general dental practices. Int J Prosthodont. 2002;15(6):559-563.
4. Setzer FC, Boyer KR, Jeppson JR, et al. Long-term prognosis of endodontically treated teeth: a retrospective analysis of preoperative factors in molars. J Endod. 2011;37(1):21-25.
5. AL-Omiri MK, Mahmoud AA, Rayyan MR, Abu-Hammad O. Fracture resistance of teeth restored with post-retained restorations: an overview. J Endod. 2010;36(9):1439-1449.
6. Vire DE. Failure of endodontically treated teeth: classification and evaluation. J Endod. 1991;17(7) :338-342.
7. Fonzar F, Fonzar A, Buttolo P, et al. The prognosis of root canal therapy: a 10-year retrospective cohort study on 411 patients with 1175 endodontically treated teeth. Eur J Oral Implantol. 2009;2(3):201-208.
8. Setzer FC, Kim S. Comparison of long-term survival of dental implants and endodontically treated teeth. J Dent Res. 2014 ;93(1):19-26.
9. Chrcanovic BR, Albrektsson T, Wennerberg A. Smoking and dental implants: A systematic review and meta-analysis. J Dent. 2015;43(5):487-498.
10. Rosen H. Operative procedure on mutilated endodontically treated teeth. J Prosthet Dent. 1961;11(5):973-986.
11. Barkhordar RA, Radke R, Abbasi J. Effect of metal collars on resistance of endodontically treated teeth to root fracture. J Prosthet Dent. 1989;61(6):676-678.
12. Sorensen JA, Engelman MJ. Ferrule design and fracture resistance of endodontically treated teeth. J Prosthet Dent. 1990;63(5):529-536.
13. Pereira JR, Valle AL, Shiratori FK, et al. Influence of intraradicular post and crown ferrule on the fracture strength of endodontically treated teeth. Braz Dent J. 2009;20(4):297-302.
14. Sherfudhin H, Hobeich J, Carvalho CA, et al. Effect of different ferrule designs on the fracture resistance and failure pattern of endodontically treated teeth restored with fiber posts and all-ceramic crowns. J Appl Oral Sci. 2011;19(1):28-33.
15. Carlini-Júnior B, Cecchin D, Farina AP, et al. Influence of remaining coronal structure and of the marginal design on the fracture strength of roots restored with cast post and core. Acta Odontol Scand. 2013;71(1):278-282.
16. Zhang YY, Peng MD, Wang YN, Li Q. The effects of ferrule configuration on the anti-fracture ability of fiber post-restored teeth. J Dent. 2015;43(1):117-125.
17. Cheron RA, Marshall SJ, Goodis HE, Peters OA. Nanomechanical properties of endodontically treated teeth. J Endod. 2011;37(11):1562-1565.
18. Perrin P, Neuhaus KW, Lussi A. The impact of loupes and microscopes on vision in endodontics. Int Endod J. 2014;47(5):425-429.
19. Torabinejad M, Ung B, Kettering JD. In vitro bacterial penetration of coronally unsealed endodontically treated teeth. J Endod. 1990;16(12):566-569.
20. Iqbal MK, Johansson AA, Akeel RF, et al. A retrospective analysis of factors associated with the periapical status of restored, endodontically treated teeth. Int J Prosthodont. 2003;16(1):31-38.
21. Trope M, Chow E, Nissan R. In vitro endotoxin penetration of coronally unsealed endodontically treated teeth. Endod Dent Traumatol. 1995;11(2):90-94.
22. Ferreira R, Prado M, de Jesus Soares A, et al. Influence of using clinical microscope as auxiliary to perform mechanical cleaning of post space: a bond strength analysis. J Endod. 2015;41(8):1311-1316.
23. Arunpraditkul S, Saengsanon S, Pakviwat W. Fracture resistance of endodontically treated teeth: three walls versus four walls of remaining coronal tooth structure. J Prosthodont. 2009;18(1):49-53.
24. Jotkowitz A, Samet N. Rethinking ferrule—a new approach to an old dilemma. Br Dent J. 2010;209(1):25-33.
25. Nagasiri R, Chitmongkolsuk S. Long-term survival of endodontically treated molars without crown coverage: a retrospective cohort study. J Prosthet Dent. 2005;93(2):164-170.
26. Aquilino SA, Caplan DJ. Relationship between crown placement and the survival of endodontically treated teeth. J Prosthet Dent. 2002;87(3):256-263.
27. Murgueitio R, Avila-Ortiz G . A novel diagnostic and prognostic classification for the clinical management of endodontically treated single anterior teeth. Int J Periodontics Restorative Dent. 2012;32(6):713-720.
28. Zicari F, Van Meerbeek B, Scotti R, Naert I. Effect of fibre post length and adhesive strategy on fracture resistance of endodontically treated teeth after fatigue loading. J Dent. 2012;40(4):312-321.
About the Author
Alan M. Atlas, DMD
Clinical Professor
Department of Preventive and Restorative Sciences
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Philadelphia, Pennsylvania
Samuel Kratchman, DMD
Associate Professor of Endodontics
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Endodontic Practice
Exton, Pennsylvania
West Chester, Pennsylvania