Layering Composites Efficiently and Effectively
Incorporating bulk-fill into your practice
Lori Trost, DMD
The most common restorative procedure today is the placement of a direct resin-based composite.1 When cavity forms are large, a traditional incremental layering technique can be time consuming and may yield an unpredictable final restorative result.
To ensure success, composite placement requires the understanding of current materials, the manner in which they can be used, and the translation of their benefits into a consistent technique. Some factors to consider are preparation depth, remaining substrate, adhesion detail, light-curing requirements, and contact re-establishment.2 Each of these components has a great influence on the final restorative outcome and should not be underestimated.
According to the American Dental Association, the most common causes for postoperative sensitivity after placing composite resins are polymerization shrinkage and stress, incomplete material coverage, and under-curing.3 In addition to postoperative sensitivity, composite shrinkage stresses can lead to marginal staining, debonding, micro-leakage, secondary caries, and micro-fractures/cracks.3 To offset shrinkage stresses, a newer category of bulk-fill flowable composites is available to clinicians that feature ease-of-use, excellent adaptation to internal cavity geometry, and the ability to place material in up to 4 mm increments. Although different from conventional flowable composites, bulk-fill composites can also be inferior in physical properties compared to hybrid universal composites (eg, resistance to occlusal wear). For this reason, it is often recommended to place a 2-mm occlusal cap with a universal composite over the bulk-fill flowable.
One of the most challenging aspects of any restoration is delivering enough energy to light cure resin composite in deep preparations.4 All curing lights experience an energy drop-off that decreases the amount of energy delivered to the restoration over distance, and the amount of energy lost varies among curing lights.5 In one study, a 50% reduction of irradiance was reported at a 6 mm distance from the light guide.6 If the average clinical crown height of posterior teeth is 6 mm, clinicians may be faced with curing composite resins in deep preparations a significant distance from the curing light tip.7 Clinicians should remember the following basic principles ensure adequate light curing of composite material: deep composite resin restorations demand a high-quality curing light, good operator technique, the ability to direct the light into the preparation, and sufficient curing time for the individual type and shade of material.8
Case Presentation
Preparation
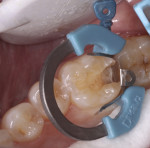
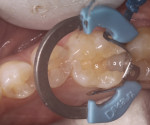
A patient presented with decay on the distal aspect of tooth No. 30 that necessitated a direct composite restoration. The patient was administered a 2% lidocaine solution containing 1:100,000 concentration of epinephrine to achieve an inferior alveolar nerve block. Once comfortable, a 330 carbide bur was used to prepare the distal-occlusal surfaces of the tooth. Decay was removed using a round No. 4 bur and confirmed by the use of a caries indicating solution (Figure 1). The preparation was isolated with the Palodent® Plus Sectional Matrix System (DENTSPLY, www.dentsply.com) by using the subgingival molar matrix band, universal ring, and wedge. In place of a rubber dam, proper suctioning and use of a cotton roll prevented salivary contamination to help achieve an optimal clinical result. A 2% chlorhexidine solution, acting as a disinfectant, was blotted into the preparation and then lightly suctioned.
Adhesion
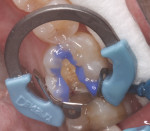
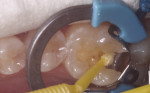
A selective-etch technique was utilized by carefully applying a 35% phosphoric etch gel for 15 seconds on the surrounding enamel framing the preparation (Figure 2). The etchant gel was then thoroughly rinsed for 5 seconds, and lightly suctioned to allow the dentin to remain moist. A universal bonding agent, Prime & Bond Elect® Universal Dental Adhesive (DENTSPLY), was generously scrubbed onto all the internal preparation surfaces for 20 seconds, followed by a thin stream of air for approximately 2 to 3 seconds and then light curing for 10 seconds (Figure 3). Care was taken to make sure no ripples were present before light curing and the freshly bonded surfaces yielded a semi-glossy appearance.
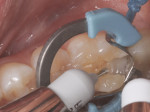
Next, a periodontal probe was used to identify the depth of the proximal box floor. The gingival box floor measured 3 mm from the pulpal floor. A bulk-fill material was selected as the initial flowable base. SureFil® SDR® flow Posterior Bulk Fill Flowable Base (DENTSPLY) was delivered to the base of the gingival box and dispensed, completely covering the margins of the box and then filled to cover approximately 1 mm of the pulpal floor—all without manipulation (Figure 4). The advantage of this bulk-fill material is to provide excellent adaptation and serve as an understory for a final 2-mm composite capping layer. The material was light cured for 20 seconds using a SmartLite LED Pen-Style® Focus® Curing Light (DENTSPLY) (Figure 5). A final capping increment of 2 mm was placed using a universal composite, TPH Spectra® Universal Composite LV, shade B1 (DENTSPLY). The composite was sculpted and light cured for 20 seconds. Care was taken to re-establish the anatomy as close to the original tooth surface as well as rounding the distal marginal ridge for improved contact support and cleansibility.
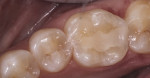
The sectional matrix, ring, and wedge were removed and additional light curing of the buccal and lingual aspects of the Class II distal box were completed. Buccal and lingual trans-enamel curing of the interproximal box is an optional step with these materials, but in this practitioner’s opinion, it can provide added insurance of proper light curing. Finishing was accomplished using a flame-shaped carbide and football-shaped carbide. Occlusion was checked and the contact re-confirmed with floss. Polishing of the final restoration was achieved using the Enhance Finishing System (DENTSPLY); an aluminum oxide–impregnated cup instrument was used in this case. The completed final restoration is shown in Figure 6.
Conclusion
Fundamentally, posterior composite placement is becoming more efficient and resin placement protocols are more predictable due to improved material efficacy. As resin chemistries continue to advance, clinicians must find the means to leverage restorative materials and techniques to provide the best outcomes for patients. SureFil SDR flow as a bulk-fill restorative can help practitioners achieve outstanding results, but when combined with other high-quality materials and techniques, the cumulative benefits of a well-done posterior direct composite restoration can be realized.
Disclosures
Lori Trost, DMD, has no relevant conflicts of interest to disclose.
References
1. 2005-06 Survey of Dental Services Rendered. American Dental Association website. Accessed February 12, 2016.
2. Strassler HE, Price RB. Understanding light curing, part 1. Delivering predictable and successful restorations. Dent Today. 2014;33(5):114-121.
3. Sarrett DC, ed. Flowable composites. In: ADA Professional Product Review: A Publication of the Council on Scientific Affairs. 2009;4(2):2-13.
4. Alrahlah A, Silikas N, Watts DC. Post-cure depth of cure of bulk fill dental resin-composites. Dent Mater. 2014;30(2):149-154.
5. Rencz A, Hickel R, Ilie N. Curing efficiency of modern LED units. Clin Oral Investig. 2012;16(1):173-179.
6. Price RB, Dérand T, Sedarous M, et al. Effect of distance on the power density from two light guides. J Esthet Dent. 2000;12(6):320-327.
7. Volchansky A, Cleaton-Jones P. Clinical crown height (length)—a review of published measurements. J Clin Periodontol. 2001;28(12):1085-1090.
8. The Four CORE™ Variables. BlueLight Analytics website. http://curingresin.com/scientific-evidence/the-four-core-variables. Accessed February 11, 2016.
About the Author
Lori Trost, DMD
Private Practice
Columbia, Illinois
For more information, contact:
DENTSPLY
800-532-2855
www.surefilsdrflow.com