Cosmetic Dentistry for Patients with Bulimia
Important considerations before, during, and after dental treatment
Eating disorders can be extremely serious illnesses that require psychological and physical intervention on several fronts. Anorexia nervosa, bulimia nervosa, and unspecified eating disorders involve an altered self-perception of body weight and morphology. A hallmark is dysfunctional eating, which can include dieting, fasting, binge eating, restricted eating, and/or frequent vomiting after eating. In many cases, these behaviors are driven by psychological rather than biological factors. Young women are especially vulnerable, but eating disorders can occur at any age and in either sex. Athletes can be at risk because certain sports require low or high weights to meet qualifications.
Prevalence and Dental Ramifications of Eating Disorders
According to Doug Bunnell, PhD, a founder and past board chair of the National Eating Disorders Association (NEDA), eating disorders are still under-detected and under-diagnosed. Nevertheless, it is estimated that 35% to 57% of adolescent girls use crash diets, fasting, or self-induced vomiting as a means of maintaining or losing weight.1 More than 50% of teenaged girls and one third of teenaged boys exhibit unhealthy weight-control behavior.2 The incidence of bulimia in females between ages 10 and 39 years tripled between 1988 and 1993.3 Current figures suggest that between 1.1% and 4.2% of women have bulimia symptoms during their lifetime.4 Approximately 0.9% of females are classified as anorexic.5 Many others show some signs of one or both conditions but are not classified as either.
Dentists may have the unique opportunity to be the first health care professionals to identify bulimia and other eating disorders in patients; in fact, 28% of patients with bulimia are first diagnosed during a dental exam.6 Although a comprehensive discussion of the symptoms and presentations of various eating disorders is beyond the scope of this article, NEDA has an abundance of resources to help health care professionals develop an educated and compassionate approach.4,7
The dental and medical ramifications of eating disorders become more severe the longer the condition exists.8 An estimated 89% of patients with bulimia exhibit worn tooth enamel and decayed and sensitive teeth.8 This is due to stomach acids that invade the lingual enamel of upper anterior teeth from the binging and purging associated with bulimia. Acid reflux disorder and other gastrointestinal problems can further damage the oral environment. Eventually, the loss of enamel can cause alterations in shape, length, and color of the anterior teeth. A loss of vertical dimension and major changes in occlusion can occur.
As the condition worsens, salivary glands and ducts may swell in the neck and jaw. This swelling can result in widening of the corners of the jaw, leading to a square-jaw appearance. Lips redden, dry, and crack, and the patient may complain of resultant dry mouth and temporomandibular joint (TMJ) symptoms, which result from the previously stated changes. Other symptoms include electrolyte imbalance that can lead to inappropriate levels of calcium, sodium, and potassium. At its worst, this can lead to heart attacks, stroke, or even mortality.
Treatment Considerations for Patients with Bulimia
Shame and ambivalence make treatment of eating disorders difficult. Bunnell suggests that issues of past or present trauma, anxiety, and depression complicate treatment and long-term prognosis. NEDA has guidelines for initiating difficult conversations with patients suspected of having bulimia.7 The dental team should recommend seeing a physician, nutritionist, and counselor for non-dental treatment. To assist, NEDA can be reached at www.nationaleatingdisorders.org or 800-931-2237 and can serve as a resource for dentists and patients alike.
Recovery is the time when long-term cosmetic dentistry will have the best prognosis. The dentist and patient must decide if the time is right. A thorough new-patient interview is essential prior to initiating dental treatment. Patients with eating disorders may be embarrassed or even defensive about their conditions. Therefore, empathy is essential for creating a bond. A comprehensive examination is also important, as the teeth, muscles, and joints can be damaged by the acid entrenchment from bulimia.
Dental treatment can be accomplished in different ways. Clearly, active decay, infection, and other pathology must be treated. If the condition is still acute, long-term temporization of anterior teeth without enamel makes more sense than permanent porcelain restorations, which may have to be redone due to continued acid infiltration in the area. In many cases, orthodontics is essential because the patient’s bite will change as lingual enamel is destroyed. Occlusal space must be added to allow for protection of the lingual dentin of these teeth unless all maxillary teeth are treated with crowns. Short-term orthodontics can be used in some cases. If an orthodontist provides the patient with treatment, excellent communication between the restoring dentist and specialist is essential. This article presents a rare case in which orthodontics was not deemed necessary for conclusive treatment.
Case Presentation
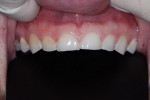
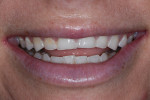
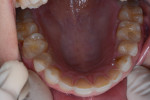
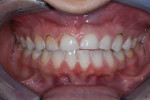
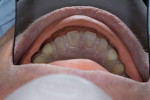
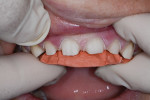
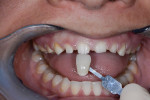
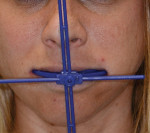
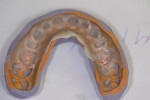
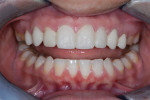
A 31-year-old woman presented to the office with an interest in restoring severely worn upper anterior teeth (Figure 1 through Figure 3). The lingual surfaces of these teeth were badly eroded, and the teeth were extremely short after the loss of perhaps 30% of tooth structure. A review of the patient’s medical history revealed that the patient had a history of bulimia. She stated that she was in recovery and had not regurgitated as part of her past condition for 1 year. She was excited about beginning treatment as soon as possible to restore her teeth. She consented to occlusal analysis and photographs and stated that she would consider short-term tray orthodontics but would not consent to full-banded orthodontics. She also said she had had “mild dislocation” of her left TMJ in the past.
Diagnostics and Treatment Planning
A comprehensive examination included a full-mouth series of x-rays, periodontal charting, and a check for potential mobility and furcation involvement. It also included an examination of the masseters, sternocleidomastoids, pterygoids, and temporalis muscles. All areas of occlusal wear and recession, including abfraction areas, were recorded.
The patient exhibited a translational click on the left as determined by a doppler (Great Lakes Doppler Auscultation, Great Lakes Orthodontics, www.greatlakesortho.com). This can be discerned if a click is noticed when the patient opens wide, to the right, left, and protrusive (translational, not rotational movements). Muscles were stable at this time with the exception of the anterior branch of the sternocleidomastoid on the left. Minimal mobilities were on lower incisors and fremitus on tooth No. 6. Anterior guidance was inadequate, and the patient had many occlusal interferences on posterior teeth in lateral excursions.
The patient consented to the creation of a maxillary deprogrammer appliance as a means of relaxing jaw muscles so her centric relation (CR) position could be determined. Two sets of impressions were taken with alginate. Bite relations were recorded (ACU-flow™, Great Lakes Orthodontics) using an approach suggested by Dr. Frank Spear.9 The patient wore a Lucia Jig (Great Lake Prosthodontics) for 20 minutes before the bite was taken using a “slide forward/slide back and squeeze” technique and face-bow relations were fabricated (Denar® Combi, Whipmix, www.whipmix.com). The author believes that face-bow and CR bite relations are essential in creating a stable bite for these and all complex cases.
The models were later mounted and then sent to Great Lakes Orthodontics for the creation of a mini-deprogrammer. The patient was instructed to wear it nightly for a few nights and to discontinue use if symptoms occur or increase. If asymptomatic, she would subsequently wear it full-time for 48 to 72 hours, with the exception of meals and self-hygiene. Again, she was told to discontinue use if any symptoms recurred.
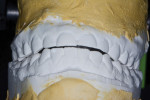
The patient returned a few weeks later and stated that her jaw “felt great.” The dental team took new bite relations and determined a stable, comfortable CR. These models were remounted. One set of mounted models was kept at the office, and a second set was sent to Walt Richardson, manager and technician at Bay View Dental Laboratory (http://bvdl.com). After a consultation with Richardson, a decision was made to retain the patient’s third molars. The mounted models determined a large discrepancy between the patient’s CR bite and her maximum intercuspation (MI) position (Figure 4). This discrepancy would allow the dental team to restore her smile in CR and retain her third molars for stability, after careful occlusal equilibration. Prior to creating the wax-ups, composite resin was added to the incisal edges of the centrals to estimate where the final incisal edges should be (Figure 5), which is especially important to communicate to the laboratory to ensure a successful outcome.10 This measurement was given to the laboratory as a starting point for wax-up fabrication.
The patient agreed to crowns on teeth Nos. 5 through 12 and veneers on teeth Nos. 3, 4, 13, and 14. The lab created functional and cosmetic wax-ups, which would help the dental team create temporary crowns and veneers. During a consultation with the patient, she was told that she would wear these temporary restorations for several weeks to ensure she would be comfortable with the new occlusion and larger teeth. The upper anterior lingual surfaces were severely eroded, so the dental team could do minimal preparation of these areas or risk potential root canal issues. Bulk could be added facially if the patient could adapt to this change.
The patient agreed to at-home tray tooth whitening (Philips Zoom, www.philipsoralhealthcare.com). She also consented to laser crown lengthening of teeth Nos. 7, 9, and 11. Upon consultation with periodontist Lawrence Tesser, DDS, the dental team determined it could accomplish enough symmetry with a diode laser, so periodontal surgery was not indicated.
Early Treatment and Impressions Stage
The wax-ups were created, along with a plastic stent, which aided in the determination of the correct amount of laser crown lengthening for teeth Nos. 11 and 7, and a slight amount on tooth No. 9 (Figure 6) (NV®, DenMat,www.denmat.com). The dental team scheduled the preparation appointment for 2 weeks later after the patient had fully whitened her teeth and the laser recontouring had healed.
At the next appointment, the tissue above teeth Nos. 7, 11, and 9 exhibited excellent healing. Three carpules of articaine 4% with epinephrine 1:2000,000 (Septocaine®, Septodont, www.septodontusa.com) and three carpules of lidocaine with epinephrine 1:1000,000 (Xylocaine®, DENTSPLY, www.dentsply.com) were administered over 5 hours. Teeth Nos. 5 through 12 were prepared for IPS e.max® crowns (Ivoclar Vivadent, www.ivoclarvivadent.us), and teeth Nos. 3, 4, 13, and 14 were prepared for IPS e.max veneers. The use of IPS e.max was determined to be the best option for these restorations due to the product’s strength and esthetics. A technician can press this material to be as thin as 0.3 mm, while still maintaining the strength of 400 MPa.11-13 IPS e.max pressed restorations can be used to create crowns and veneers of different thicknesses in the same arch without noticeable differences in color or texture.13,14 The goal in this case was a minimally invasive approach as well as longevity.
Preparations were created with the help of buccal and lingual prep guides made from the wax-ups (Figure 7 and Figure 8). Impressions were taken using a two-cord technique. Ultrapak Cord 00 nonepinephrine (Ultradent, www.ultradent.com) was placed and later covered with Ultrapak with epinephrine 0 (Ultradent). The second cord was removed prior to the impression. Two full-arch impressions were taken for redundancy. The impression was taken with Flexitime® (Heraeus Kulzer, www.heraeus-kulzer-us.com), followed by bite records using ACU-flow. The stump shade was recorded, and a photograph of the shade tab was taken aligned in the same plane as the preps (Figure 9). A stickbite was taken using the Esthetic CrossRef™ (Whip Mix, www.whipmix.com) and Blu-Mousse® (Parkell, www.parkell.com) (Figure 10). Blu-Mousse was used here rather than ACU-flow because it is more flexible and easier to manipulate.
Temporary crowns and veneers (splinted) were fabricated using a putty matrix with Luxatemp® Ultra (DMG America, www.dmg-america.com) (Figure 11). They were removed from the mouth after 60 seconds. The provisionals (Figure 12) were adjusted in CR, lateral excursions and protrusive. Crossover bite issues were removed. The author uses a shrink-wrap technique for pure veneer cases and for most mixed crown/veneer cases. It was determined that a cementation technique would be advisable in this case, due to the number of crowns involved. Prior to cementation, all teeth were coated with Telio CS desensitizer (Ivoclar Vivadent). The temporaries were cemented with ZONEFree (Dux Dental, www.duxdental.com) because it is a clear material but does not bond to the preparations. The patient was given The Natural Dentist rinse (Caldwell Consumer Health, www.bleedinggums.com) and 4% chlorhexidine gluconate in a blunt syringe to use around the margins for 3 days.
Final Stages
The patient wore the provisional crowns and veneers for 10 days. This period was necessary to monitor her experience with the restorations, including her reaction to the esthetics, occlusion, comfort, speech, and potential issues in the envelope of function and neutral zone.
The “s” sound was found to be normal. In speech, the incisal edges of the maxillary incisors landed slightly lingual to the vermillion border of the lower lip. This was crucial when taking into account the much larger size of the new restorations. All other speech signs were normal. Her muscles and joint were asymptomatic as well. The patient was happy with the esthetics, but she decided she wanted the OM3 shade (VITA Zahnfabrik, www.vita-zahnfabrik.com) instead of the slightly darker Vita B1 shade of the temporaries. She did not want any alteration of the sizes and shapes of these provisional restorations and consented to the permanent restorations to match those of the provisionals.
During the same appointment, alginate impressions of the upper provisional restorations were taken as well as an ACU-flow bite and face-bow relations of the temporaries. A face-bow at this appointment helps to ensure that no cant would be in the final restorations. Photographs were taken as well, including of the OM3 shade above the darker lower teeth. The patient decided to further whiten the lower incisors at a later date.
At an appointment 10 days later, the patient appeared at the office to insert her crowns and veneers. The patient was given nitrous oxide analgesic while the temporaries were removed and the permanent crowns and veneers were placed, using try-in paste (NX3 Nexus, Kerr Dental www.kerrdental.com). The author believes it is essential to try in multiple cosmetic restorations without dental anesthesia. It is important for the patient to see the restorations without lip asymmetry potentially caused by anesthetics. Unfortunately, most try-in pastes can be uncomfortable for the patient. A combination of glutaraldehyde-based desensitizers delivered during the preparation visit and nitrous oxide during this appointment can make the experience more tolerable (nitrous oxide must be removed and the patient placed on oxygen before he/she can give consent to place the permanent restorations). The patient should see the restorations in different light sources, including natural light, before giving consent.
The patient was happy with the restorations. The crowns and veneers were treated with Ivoclean (Ivoclar Vivident) and then with a silane agent (Monobond Plus, Ivoclar Vivadent). The teeth were cleaned with an antibacterial cleansing agent (Consepsis®, Ultradent). The crowns and veneers were then treated with a selective etch technique (Ultra-Etch®, Ultradent), followed by OptiBond™ XTR (Kerr Dental). They were cemented with NX3 cement (Kerr Dental) using a “tack and wave” technique. Curing the cement for 3 seconds using the Demi light (Kerr Dental) creates an excellent initial set. At this point, residual cement is removed and the contacts are gently flossed. The final cure is reached after each restoration is given a 20-second cure on lingual, facial, and occlusal surfaces.
The Cerisaw™ (DenMat, www.denmat.com) and ContacEZ® (ContacEZ, www.contacEZ.com) were used to expedite removal of interproximal cement. Excess labial and lingual cement was removed with a flame-shaped diamond bur. All restorations were adjusted in CR and in lateral and protrusive excursions. A T-Scan® (Tekscan, www.tekscan.com) was used to confirm the accuracy of bite relationships. The patient was seated forward for final bite adjustments and minor cosmetic changes were made on incisal edges. The patient was asked to return in 1 week for any necessary adjustments functionally and cosmetically, as well as an impression for a hard/soft night guard to protect the restorations.
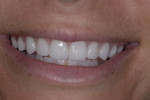
At the final appointment for inserting the night guard, the patient was advised to appear for 6-month recare appointments. The dental team suggested she continue seeing a therapist to aid in long-term recovery from her eating disorder. She was gently told (as she had been multiple times in the past) that a relapse into bulimia could cause the destruction of these restorations and other teeth. The patient was ecstatic about the restorations and fully understood these precautions. (Figure 13 and Figure 14).
Conclusion
All dentists at some time during their careers will see a patient with either a history of bulimia or an existing eating disorder. The dentist may be the first health care practitioner to notice this condition and should be knowledgeable about the best ways to discuss this condition with a patient in a nonjudgmental, caring fashion. In this way, dentists can potentially save or at least positively alter a patient’s life if done correctly.
Treatment can be undertaken in a number of ways. The dental practitioner will need to monitor the stage of the illness and perhaps speak to the patient’s therapist or physician to determine if permanent dental treatment is advisable. If the condition is still acute, a more temporary plan should be undertaken. As the patient heals from an eating disorder, he or she can take better self-care in general. A more attractive, more functionally sound smile may help with improved self-esteem and quality of life on the road to recovery.
References
1. Boutelle K, Neumark-Sztainer D, Story M, Resnick M. Weight control behaviors among obese, overweight, and nonoverweight adolescents. J Pediatr Psychol. 2002;27(6):531-540.
2. Neumark-Sztainer, D. I’m Like, SO Fat! New York, NY: Guilford Press; 2005.
3. Hoek HW, van Hoeken D. Review of the prevalence and incidence of eating disorders. Int J Eat Disord. 2003;34(4):383-396.
4. National Institute of Mental Health. Eating Disorders: Facts About Eating Disorders and the Search for Solutions [publication 01-4901]. Bethesda, MD: National Institute of Mental Health, National Institutes of Health, US Department of Health and Human Services; 2001.
5. Hudson JI, Hiripi E, Pope, HG Jr, Kessler, RC. The prevalence and correlates of eating disorders in the National Comorbidity Survey Replication. Biol Psychiatry. 2007;61(3):348-358.
6. McDaniels AK. Dental problems could be a sign of an eating disorder. Baltimore Sun website. www.baltimoresun.com/health/blog/bs-hs-expert-oral-health-eating-disorder-20141231-story.html. Accessed June 16, 2015.
7. Information for dental practitioners. NEDA website. www.nationaleatingdisorders.org/information-dental-practicioners. Accessed June 19, 2015.
8. Dental complications of eating disorders. NEDA website. www.nationaleatingdisorders.org/dental-complications-eating-disorders. Accessed June 19, 2015.
10. Spear F. Centric Relation: Bite Records (video). Scottsdale, AZ: Spear Education; 2011.
11. Hess LA Determining the correct vertical and horizontal incisal edge position. Inside Dentistry. 2009:5(4):26-34.
12. Steiner M, Sasse M, Kern M. Fracture resistance of all-ceramic crown systems [abstract 2999]. Presented at: IADR General Session; San Diego, 2011.
13. Culp L, McLaren EA. Lithium disilicate: the restorative material of multiple options. Compen Contin Educ Dent. 2010;31(9):716-725.
14. Auster P. Conquering a difficult case, part 2. Lithium disilicate as a restorative solution for amelogenesis imperfecta. Dent Today. 2013;32(8):61-64.
15. Cardoso JA, Almeida PJ, Fernandes S, et al. Co-existence of crowns and veneers in the anterior dentition: case report. Eur J Esthet Dent. 2009;4(1):12-26.