Predictable Treatment for “Gummy Smiles” Due to Altered Passive Eruption
A systematic diagnostic approach based on foundational principles
Depending on the degree, excessive gingival tissue display is a major concern for a large number of patients, as it plays a vital role in the overall harmony of a beautiful smile. To predictably treat this condition and achieve a successful esthetic and stable outcome, the contemporary esthetic dentist must have a clear understanding of the dental-gingival complex and its biologic determinants.1,2
As cosmetic dental treatments are becoming more common, dentists must be able to offer the treatment options available to address their patients’ esthetic concerns. With the awareness and emphasis on overall facial esthetics, both patients and dentists are recognizing the importance of how the amount of gingival display can become a critical component in the make-up of an attractive smile.
Altered passive eruption is a condition in which the relationship between teeth, alveolar bone, and the soft tissues creates an excessive gingival display. Often the patient’s initial chief complaint is of short teeth or a “gummy smile.” In the past, these concerns were often overlooked, or the clinical crowns were lengthened with restorative procedures without investigating the etiologic causes. However, patients and dentists alike are becoming aware of the importance of comprehensive facial evaluations.3-5 Currently, the gingival architecture is a vital aspect of any restorative treatment plan, as clinicians recognize how the gingival complex and its parameters relate to the esthetic treatment of short clinical crowns.
This article presents the differential diagnosis for excessive gingival display and the modality used for the treatment of altered passive eruption.
Possible Etiologies
There are a number of clinical conditions that lead to excessive gingival tissue display when smiling.6 Any successful treatment plan must include a proper diagnosis of the true etiology of the condition with a clear understanding of the dental-gingival complex and its deviation from the norm.7-10
The four etiologies of excessive gingival tissue display include hyper-mobile/short upper lip; compensatory eruption/dental alveolar extrusion; vertical maxillary excess; and altered passive eruption. There are also instances in which a combination of etiologies occurs concurrently.
Normal Tooth Eruption
The normal eruption of teeth occurs in two phases, an active and a passive phase. The active eruption phase involves the physical movement of the tooth out of the alveolar bone into position on the occlusal/incisal plane. The passive eruption phase is the exposure of the crown of the tooth due to the apical migration of the gingival tissues. This apical migration in the passive phase of tooth eruption occurs in four distinct stages:6
Stage 1: The teeth reach the plane of occlusion, and the junctional epithelium is on the enamel.
Stage 2: The epithelial attachment rests partly on the enamel and partly on the cementum apical to the cementoenamel junction (CEJ). The base of the sulcus is on enamel.
Stage 3: The junctional epithelium lies totally on the cementum, with the base of the sulcus at the CEJ.
Stage 4: The epithelial attachment lies totally on the cementum, the base of the sulcus is on the cementum, and a portion of the root may be clinically exposed.
Altered Passive Eruption
Altered passive eruption is the failure of the dental/gingival complex to migrate apically past stage 2 and expose the entire clinical crown to obtain a normal position at the base of the sulcus relative to the CEJ.11 It is estimated that this occurs in about 12% of the general population. Clinically, the most obvious sign of altered passive eruption is a short-looking tooth. Normally, the CEJ resides just apical to the free gingival margin of the anatomic crown, and the sulcus depth usually measures 1 to 3 mm. In cases of altered passive eruption, the CEJ might be up to 10 mm apical to the free gingival margin.
Altered passive eruption, as described by Coslet, is further classified into two case types, based on the free gingival margin and osseous crest relationships with the tooth.6 Type 1 presents with a noticeably thicker biotype and wider band of buccal keratinized tissue, while Type 2 exhibits a narrower band of buccal keratinized tissue that appears to fall into a normal width. Types 1 and 2 are further separated into two subgroups, A and B. In the 1A subgroup, the osseous crest is located 1.5 mm to 2 mm apical to the CEJ, while in the 1B subgroup, the osseous crest is found at the level of the CEJ.
As empirical evidence suggests that Type 1B of Coslet’s classification is the most common type of altered passive eruption observed in nature, this article describes a treatment protocol for this subgroup of altered passive eruption.
Diagnosis
When there are multiple etiologies of excessive gingival display, a series of clinical evaluations is warranted for a clear diagnosis in order to recommend and provide the most appropriate treatment.
In the case of diagnosing altered passive eruption, an assessment is made of the patient’s lips in repose and during a smile. If there is excessive gingival display when the patient smiles naturally, the length and mobility of the upper lip must be evaluated. The normal maxillary lip dynamic has a translation of 6 to 8 mm from rest to full smile and up to 10 mm in a hyper-mobile lip scenario. This first step is utilized to rule out a hyper-mobile/short upper lip, for which the treatment may be lip repositioning surgery or reducing lip mobility with botulism toxin.
The clinical exam should include evaluating any maxillary incisal wear to rule out the possibility of compensatory eruption/dental-alveolar extrusion. Dental-alveolar extrusion is most commonly treated with segmental orthodontic intrusion.12
Traditionally, a cephalometric analysis was utilized to evaluate patients with vertical maxillary excess. An alternative method has been proposed by Misch to rule out vertical maxillary excess by using the maxillary canines and their position relative to the upper lips in repose.13 This study indicates that if the tip of the maxillary canines are at the same level as the maxillary lip line with lips in repose, any excessive tissue display when the patient smiles is not likely a result of vertical maxillary excess. A diagnosis of vertical maxillary excess would be indicated if the amount of maxillary canine cusp tip display were 2 mm or greater with the maxillary lip in repose. In Misch’s study, the maxillary canine position to lips in repose had an average dimension within 1 mm of the upper lip, regardless of gender or age. Due to the very narrow range of the canine exposure in the population, it is suggested that this relationship may be used as a more predictable determinant of anterior tooth position.
The key to arriving at the diagnosis of altered passive eruption also involves the location of the CEJ in the gingival sulcus. If the CEJ is not detectable in the gingival sulcus and the other etiologies of excessive gingival display are ruled out by using a dental explorer, a diagnosis of altered passive eruption can be made.14
An important point the clinician needs to consider when treating someone with excessive gingival tissue display is that a patient may have multiple etiologies present at the same time. While this may require additional investigation, if the clinician implements the previously mentioned comprehensive assessment protocols, this issue should not generate a significant concern pertaining to the definitive diagnosis.
Case Presentation
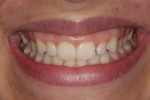
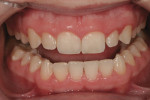
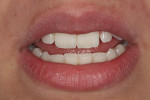
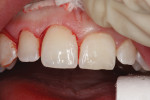
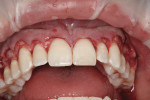
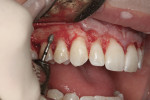
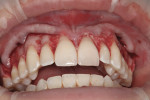
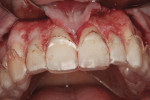
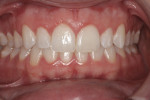
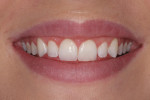
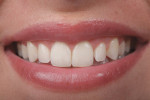
A 23-year-old woman presented with the chief complaint of excessive display of gingival tissue, saying, “I don’t like my gummy smile.” In 2012, she determined that her smile was becoming increasingly unattractive (Figure 1 through Figure 3) to the point that she would position her upper lip to avoid any tissue display when she smiled, or she would cover her mouth with her hand. It was apparent that the way this patient felt about her smile was a significant social disability that had a negative impact on her self-confidence.15
Clinical Diagnosis
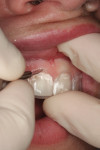
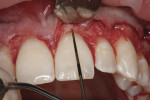
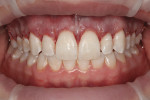
A comprehensive clinical examination revealed that the maxillary central incisors were 8 mm long and 8.5 mm wide, with no appreciable evidence of incisal wear. Photographs taken of the patient with the lips in repose (Figure 4) revealed 6 mm central incisor tooth display with little or no cuspid display. The lip line was also measured from the lips in repose position to the lip line at the full smile position, with the amount of translation found to be 8 mm, which is the average lip movement for a young female. Next, a periodontal evaluation was done where the probing depth of the mid-facial sulcus measured 1 mm deep; it was not possible to locate the CEJ in the sulcus with an explorer. With the patient anesthetized, bone sounding at the mid-facial surface of the central incisor revealed a distance of 3 mm from the free gingival margin to the alveolar crest. This information was then compared to accepted biologic width principles, which consist of 1 mm sulcus depth, 1 mm junctional epithelial attachment, and 1 mm connective tissue attachment. Based on these clinical findings, by which some of the other etiologies of a gummy smile were ruled out, a diagnosis of altered passive eruption was made.
Treatment Plan
Based on the diagnosis of altered passive eruption, the treatment plan formulated for presentation to the patient focused on esthetic crown lengthening to reduce the amount of tissue display in her smile. Given that the patient had a wide band of keratinized gingival tissue coronal to the muco-gingival junction, the gingivectomy approach was used; otherwise the same protocol can be followed, except that an apical repositioning flap would be used rather than the gingivectomy protocol. The criterion is to have approximately 3 mm to 4 mm of keratinized tissue remaining after the surgery. A diagnostic wax-up of ideal tooth dimensions was done on the patient’s study models to demonstrate to the patient the average length of 10.5 mm for a central incisor as well as mock-up of the expected surgical outcome.16 With a duplicate model of the wax-up, a vacu-form template clearly defining the future free gingival margins was made to be used as a surgical guide to re-establish the horizontal gingival zeniths “cuspid, central, central, cuspid” tissue architecture. This effectively communicates the intended outcome to the surgeon before the surgical procedure, as it would be challenging to visualize those parameters once a flap was raised (Figure 5).17 Due to the broad smile of the patient, esthetic crown lengthening was planned from teeth Nos. 3 through 14 to avoid any disharmony of the gingival architecture.
Treatment Phase
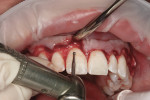
With the patient adequately anesthetized (2% lidocaine, 1/100,000 epinephrine), the prefabricated vacu-form template was verified for fit throughout the teeth that were to be crown lengthened. With a 15-C surgical blade, a gingivectomy was performed along the margins of the vacu-form template, incorporating a reverse bevel in the tissue for improved adaptation when suturing the flap (Figure 6). Once the gingivectomies were completed, full-thickness flaps were raised, leaving the lingual surface of the inter-dental papillae intact (Figure 7). With the reflected full-thickness flap demonstrating that the CEJ of the central incisor was in very close proximity to the level of the osseous crest, the classic phenomena of Type 1B altered passive eruption (Figure 8) was confirmed.
Using the vacu-form template, ostectomies were performed with #4 round carbide and fine football-shape diamond burs up to 3 mm apical from the edge of the template while respecting and contouring the boney architecture to re-create the gingival zeniths (Figure 9 and Figure 10).18 Additional ostectomies were similarly performed on all the treated teeth based on the parameters prescribed by the vacu-form template. Care was taken during the ostectomies to limit crestal bone removal to the facial aspect of the treated teeth from line angle to line angle of the respective tooth crown without removing inter-proximal bone.
At the conclusion of the ostectomies, the new buccal osseous crest from line angle to line angle should be 2 mm apical to the CEJ, allowing for the re-establishment of a normal dental/gingival complex consisting of 1 mm connective tissue attachment, 1 mm junctional epithelium, and 1 mm sulcus depth (Figure 11 and Figure 12).
All the exposed root surfaces were hand scaled to remove any residual bone fragments and tissue tags. A 24% EDTA solution was used to treat the root surfaces for 3 minutes, after which they were conditioned by removing the smear layer and opening the dentinal tubules to enhance reattachment to the gingival tissue. The flaps were repositioned coronally to the treated teeth at the CEJ and secured with individual sling sutures utilizing 5.0 chromic gut. Light pressure was applied over the tissue flaps for 3 minutes to express any excessive fluids and encourage the formation of a very thin fibrin clot underneath the flap to enhance its stability (Figure 13).
The patient was prescribed a non-steroidal anti-inflammatory drug to minimize inflammation and a PerioSciences AO Provantage Gel (www.periosciences.com) for postsurgical plaque management. Instructions were given to the patient to avoid manual brushing for 2 weeks, especially around the free gingival margins. The patient was followed up at 2-week, 1-month, and 3-month intervals (Figure 14 and Figure 15).
Conclusion
The keys to the successful outcome of this case were based on using a differential diagnostic approach and incorporating diligent evaluation of the different etiologies that can lead to a condition with excessive tissue display— ie, the lay term “gummy smile.” Once the diagnosis is determined and the practitioner incorporates sound surgical protocols that adhere to and respect the principles of biologic width, an extremely esthetic result with predictable long-term stability can be expected (Figure 16 through Figure 18).
About the Author
David K. Chan, DMD, AAACD
American Board of Cosmetic Dentistry
American Academy of Cosmetic Dentistry
Private Practice
Vancouver, Washington
References
1. Kois JC. Altering gingival levels: the restorative connection part 1: biologic variables. J Esthet Restor Dent. 1994:6(1):3-9. doi:10.1111/j.1708-8240.1994.tb00825.x.
2. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11(1):29-38. doi: 10.1111/j.1600-0757.1996.tb00180.x.
3. McLaren EA, Phong TC. Smile analysis and esthetic design: “In the zone.” Inside Dentistry. 2009;5(7):44-48.
4. Kokich V. Esthetics and anterior tooth position: an orthodontic perspective. Part I: Crown length. J Esthet Dent. 1993;5(1):19-23.
5. Kokich V. Esthetics and anterior tooth position: an orthodontic perspective. Part 2: Vertical position. J Esthet Dent. 1993;5(4):174-178.
6. Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan. 1997;70(3):24-28.
7. Levine RA, McGuire M. The diagnosis and treatment of the gummy smile. Compend Contin Educ Dent. 1997;18(8):757-762, 764.
8. Robbins JW. Differential diagnosis and treatment of excessive gingival display. Pract Periodontics Aesthet Dent. 1999;11(2):265-272.
9. Kokich VG. Enhancing restorative, esthetic, and periodontal results with orthodontic treatment. In: Schluger S, Yuodelis R, Page RC, Johnson RH, eds. Periodontal Diseases. 2nd ed. Philadelphia, PA: Lea & Febiger;1990:120.
10. Spear FM, Kokich VG, Mathews DP. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
11. Dolt AH 3rd, Robbins JW. Altered passive eruption: an etiology of short clinical crowns. Quintessence Int. 1997;28(6):363-372.
12. Kois JC. Anterior wear: orthodontic and restorative management. In: Cohen M, eds. Interdisciplinary Treatment Planning, Volume II. Chicago, IL: Quintessence Publishing Co, Inc.; 2008:189-210.
13. Misch CE. Guidelines for maxillary incisal edge position-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
14. Lee EA. Aesthetic crown lengthening: classification, biologic rationale, and treatment planning considerations. Pract Proced Aesthet Dent. 2004;16(10):769-778.
15. Locker D. Measuring oral health: a conceptual framework. Community Dent Health. 1988;5(1):3-18.
16. Spear F. Construction and use of a surgical guide for anterior periodontal surgery. Contemp Esthet Dent. 1999;3(4):12-24.
17. Kurtzman GM, Silverstein LH. Esthetic treatment: Soft tissue management and functional mock-ups. Inside Dentistry. 2008;4(6):86-90.
18. Allen EP. Surgical crown lengthening for function and esthetics. Dent Clin North Am. 1993;37(2):163-179.