Controlling Outcomes in the Age of Digital Dentistry
Material and workflow considerations for efficient, optimal outcomes
Arguably, digital dentistry can be envisioned as a wheel with spokes that represent diagnostics, practice management, imaging of various types, and communication between labs, practices, and patients. In this scenario, CAD/CAM dentistry might be considered to be the hub of the digital dentistry wheel, because the restoration is where the “rubber meets the road” in that most dental treatments involve a restorative component, and the restorative process relies on the other aforementioned components. Today, there are many options available in terms of instruments and workflow techniques for restoring a tooth or teeth using digital dentistry. In this author’s 20 years of clinical experience with the most common CAD/CAM systems available, the most practical solution involves a single-visit chairside restorative workflow using the materials and instruments summarized in the case report presented below.
Questions that relate to achieving the goal of excellent restorative dentistry include:
Why am I selecting this material?
What workflow steps will I use?
How might I work more efficiently?
Am I satisfied with the outcome?
This case example focuses on answers to these questions in the context of the clinical workflow for the restoration of several teeth using a variety of restoration types in one visit.
Case Report
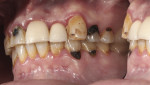
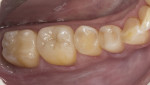
A 38-year-old male patient presented with several sensitive teeth and bleeding gums. A clinical examination revealed a history of poor oral hygiene, resulting in generalized type III (moderate chronic) periodontitis and rampant caries (Figure 1). He also exhibited traumatic occlusal wear and several failing restorations with poor esthetics. The patient reported no significant medical conditions that would impact his dental care.
Attain Periodontal and Occlusal Stability
The author prefers to wait until periodontal stability is attained to address tooth-related conditions. Therefore, in the case described, treatment began with nonsurgical periodontal therapies including four quadrants of scaling and root planing, oral hygiene instructions with patient follow-up evaluations, and counseling and at-home rinses with 0.12% chlorhexidine gluconate solution twice a day for 4 weeks.
The patient responded well to the initial course of periodontal therapy, as evidenced by significant reduction in both periodontal pocket depths and bleeding on probing in all sextants. Subjectively, the marginal gingiva also changed color to match that of the adjacent tissues (Figure 2). It was determined that he was periodontally stable enough to begin the restorative phase of his care.
An analysis of the patient’s occlusion revealed that he exhibited group function occlusion in lateral excursive movements with interferences on the non-working side in both directions. His dynamic occlusion was temporarily converted to a more harmonious, canine-protected occlusion with placement of provisional composite restorations on the linguals of teeth No. 6 and No. 11. These teeth were planned for definitive crown-lay restorations in a later phase of treatment, along with an occlusal orthotic device (biteguard).
Treatment Plan and Material Considerations
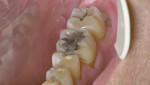
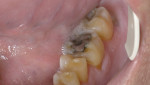
While a comprehensive restorative treatment plan was developed, quadrant III was restored first. Therefore, this area of treatment is the focus of discussion for the remainder of this case report. Preoperatively, the teeth in quadrant III presented with the following conditions:
Tooth No. 18—Decay: mesial and occlusal; wear facet(s): not penetrating enamel
Tooth No. 19—Failing: fractured amalgam; wear facet(s): penetrating into dentin; tooth fractures with staining: mesial margin ridge and mid-lingual; decay: mesial, occlusal, distal; Class V buccal abfraction
Tooth No. 20—Interproximal decay: distal; wear facet(s): penetrating into dentin
Tooth No. 21—Interproximal decay: distal, mesial; wear facet(s): penetrating into dentin; Class V buccal carious lesion
Tooth No. 22—Class V buccal carious lesion; wear facet(s): not penetrating enamel
Based on these findings, the following restorations were planned:
Tooth No. 18—Inlay: mesio-occlusal with leucite-reinforced CAD/CAM glass ceramic (IPS Empress® CAD Multi, Ivoclar Vivadent, www.ivoclarvivadent.com)
Tooth No. 19—Onlay: mesial, occlusal, distal, lingual with lithium disilicate CAD/CAM ceramic (IPS e.max CAD, Ivoclar Vivadent) and composite, Class V: buccal with Nano-hybrid composite (IPS Empress Direct, Ivoclar Vivadent)
Tooth No. 20—Composite: disto-occlusal with bulk-fill composite (Tetric EvoCeram® Bulk Fill, Ivoclar Vivadent)
Tooth No. 21—Crown-lay with lithium disilicate CAD/CAM ceramic (IPS e.max CAD)
Tooth No. 22—Composite, Class V: buccal with nano-hybrid composite (IPS Empress Direct)
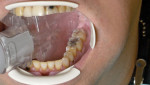
As indicated above, all planned restorations were composed of adhesively bonded materials, some of which were to be created via an in-office CAD/CAM workflow (Planmeca PlanScan™, Planmeca/E4D Technologies, www.planmecacadcam.com). This patient, like many others, had a very active tongue and copious salivary flow (Figure 3). Both effective isolation of the quadrant and moisture control in the sulcular areas are key for successful utilization of these materials.
The combination of a ComfortView™ retractor (Premier Dental Products, www.premusa.com) and an Isolite Mouthpiece (Isolite Systems, www.isolitesystems.com) effectively creates access, visibility, and confidence during technique critical steps such as prepping, scanning, and bonding the restorations (Figure 4). This isolation technique provides an effective alternative to the traditional rubber dam. For sulcular fluid control, a single dry retraction cord was placed where the preparation margins were subgingival. Generally, the ideal size of the retraction cord may be calculated by first determining the minimum probing depth in the area of interest and subtracting that number by 1 to arrive at the cord size to use. Both before scanning and bonding procedures, the tissues were retracted further, and sulcular fluids were mitigated by application of Traxodent® (Premier Dental Products) hemostatic retraction paste.
Two classes of millable ceramic and two classes of composite were chosen for this case. IPS Empress CAD Multi was selected for the second molar due to its ease of handling and more than sufficient strength for inlays. IPS e.max CAD was selected for teeth No. 19 and No. 21 because the prep geometry of these teeth required a higher strength material. Tetric EvoCeram Bulk Fill was chosen for the distal-occlusal composite on tooth No. 20 to take advantage of the ease of handling and wear resistance that this material offers. Lastly, the Class V restorations for teeth No. 19 and No. 22 were fabricated using IPS Empress Direct due to the excellent polishability that nano-hybrid composites offer. The range of preparation styles for these teeth resulted in a variety of bonding strategies as well (Table 1.)
Maximizing Workflow Efficiency
This type of case, with a combination of ceramic and direct composite restorations, lends itself very well to a digital dental restorative workflow. By utilizing the time necessary for milling and then polishing and crystallizing the CAD/CAM restorations to complete the composites, the total patient and office time can be reduced significantly without compromising the outcome. A breakdown of the time and order sequence might follow the pattern seen in Table 2.
This scenario worked out to a total time of 2 hours 20 minutes. During the 20 minutes that is required to complete the crystallization/stain and glaze procedure (Figure 5), the dentist is free to perform other procedures, such as checking a hygiene patient. Some offices take delegation a step further and use a specially trained dental assistant to perform the digital impression, design, and milling steps, so the dentist would be free for other procedures for that time as well. (Note: A formal certification program for dental assistants performing these tasks is offered through Planmeca University in Richardson, Texas. Assistants can achieve certification in various activities such as scanning, designing, and finishing.)
Obviously, an individual’s time may vary somewhat, but even allowing for a total of 4 hours, the production per hour is favorable. The reader is encouraged to create a mock treatment plan using the procedure codes below and his/her usual and customary fees:
• Tooth No. 18—D2620
• Tooth No. 19—D2644
• Tooth No. 20—D2386
• Tooth No. 21—D2740
• Tooth No. 22—D2385
Divide the total amount by both 2.4 (2 hours, 20 minutes) and 4.0 (4 hours). This will provide the reader with a reasonable range of expected office productivity.
Advantages of the Digital Restorative Workflow
In addition to the productivity advantage mentioned above, working digitally throughout the creative process and completing the restorations in one visit offers other benefits. The CAD/CAM ceramic restorations for this case were completed during the single patient visit using a single visit CAD/CAM workflow (PlanScan). Due to the single visit digital workflow, the patient does not have to endure a physical impression or a second anesthesia event. The digital impression that is created has the potential to be more accurate than a model created from a physical impression due to the elimination of steps that introduce errors. Not having to deal with provisional restorations offers the practitioner greater freedom in preparation geometry because mechanical retention of a provisional is no longer necessary. There is no risk of a failed delivery appointment by the patient either.
In this case, workflow efficiency was maximized and clinical outcome was assured by employing a combination of advanced restorative materials and a digital workflow (Figure 6).
For more information, contact:
Planmeca CAD/CAM Solutions
E4D Technologies
972-234-3880
www.planmecacadcam.com
About the Author
Alex Touchstone, DDS
Touchstone Dentistry
Hattiesburg, Mississippi