Caries Crisis Management in Children: Interim Solutions
Today’s “interim” tooth repair solutions for primary teeth can sometimes outlast the tooth itself.
There is much more to treatment planning restorative dentistry for children than the condition of each tooth. Of immediate concern is the child’s comfort. Rapid pain relief for a hurting youngster is top priority. Other considerations, such as a child’s age, developmental and medical status, ability to cooperate and tolerate the rigors of treatment, parents’ attitudes and trust, and financial implications of treatment all influence the dentist’s decisions about how to proceed.
If all considerations are ideal, and the dentist can concentrate only on tooth-by-tooth treatment, clinical pediatric dentistry logistics would be simplified. For example, if a 4-year-old has a moderately sized disto–occlusal caries lesion in a primary first molar and a history of past caries and restorative care, an experienced practitioner would suggest restoring the tooth with a preformed stainless steel crown.1 In the case of a 9-year-old with the same caries lesion, restoration using a resin-modified glass-ionomer (RMGI) or other adhesive system might be a better choice because the tooth would be retained for a much shorter time.2 Perhaps extraction of the infected tooth could be the best choice of all, if eruption of the premolar is impending.
In the last 20 years, dental restorative materials that adhesively bond to tooth structure have given dentists new options for repairing primary and permanent teeth. For decades, zinc-oxide/eugenol (or reinforced ZOE) with a calcium-hydroxide liner was the treatment of choice for rapid emergency repair of a tooth with a severe caries infection. This method of “caries control” was aimed at stopping a caries crisis, and enabling healing to commence until long-term treatment could be planned and implemented. Such “temporary fillings” were usually expected to last 6 to 12 months because of inherent weaknesses and breakdown of the materials.
Today’s “interim” tooth repair solutions, on the other hand, sometimes can last for a decade or more. This is particularly important in restorative dentistry for children. It would be rare for a restored primary molar to be needed in the dentition for more than 7 or 8 years, unless there was no premolar successor. All of these considerations influence the logic and rationale of a dentist’s treatment planning challenge, especially for cases in which the severity of caries infections necessitate rapid action.
This article describes treatment for a 3-year-old with severe carious damage to many of her primary teeth. The child was brought in for a second opinion by her parents after an initial evaluation and treatment planning by another pediatric dentistry specialist. Her 2-year follow-up is documented.
Case Presentation
The parents of a 3-year-old girl brought her to the office, seeking a second opinion about her dental care. Another pediatric dentistry specialist had seen her and planned extensive care, including multiple pulpotomies, followed by full-crown restorations, and perhaps extraction of certain teeth, with treatment rendered under general anesthesia in a local hospital. The estimated cost for the restorative dental treatment alone exceeded $3,000. Hospital and operating room costs were additional. The child’s care was not covered under any dental or medical third-party payment plan, and the parents related that they could not afford to pay for the treatment. They also claimed they were told that there was no other way to treat the child except using general anesthesia.
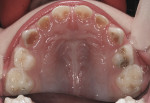
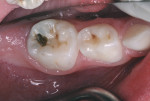
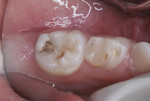
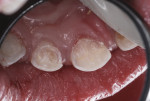
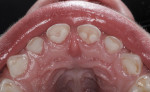
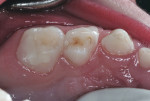
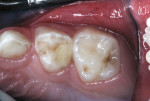
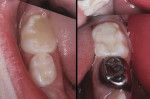
The child was cooperative for examination and denied that any of her teeth hurt. She had extensive carious destruction of the palatal surfaces of all the maxillary anterior teeth along with caries lesions of two maxillary molars (Figure 1). In addition, all four mandibular primary molars were carious, including the left first primary molar that had an occlusal resin-based composite restoration (Figure 2 and Figure 3).
After the parents were queried about the child’s diet (nutritional counseling would follow) and given instructions in daily oral homecare for their daughter, it was decided to appoint her for interim repair of the carious maxillary teeth, using RMGI restorative materials. For the child’s safety and comfort, nitrous-oxide/oxygen mask inhalation would be used in the usual manner. It was not known how many maxillary teeth could be treated in the first appointment. Additional appointments would be scheduled based on what was accomplished in the first visit.
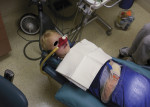
For the first treatment appointment, the child was brought in NPO from the night before. She had been given a small amount of water about 2 hours prior to treatment time. The patient was placed in stabilizing wraps and offered no resistance. After the nitrous oxide/oxygen mask was explained to the patient and placed over her nose, earphones with children’s music were positioned for auditory diversion (Figure 4).
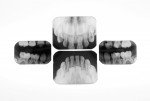
Local anesthetic infiltration was completed in the usual manner using Articaine HCl 4% with 1/200,000 parts epinephrine. Two anterior radiographs and two bitewing films were recorded (Figure 5). For stable mouth opening, safety, and the child’s comfort, a Molt-type mouth prop, cushioned with surgical tubing, was used. A rubber dam was not used, but the oropharynx was protected using 4” X 4” gauze sponges. With several sizes of round burs at slow speed, the carious tooth structure was debrided from the six primary anterior teeth (Figure 6).
Although caries penetration was excessive in each tooth, there was no pulp space perforation. A small portion of RMGI liner (Vitrebond™ Plus, 3M ESPE, www.3MESPE.com) was applied to the deepest portion of each preparation. The “nano-ionomer,” Ketac™ Nano (3M ESPE) was then injected into each prepared tooth and hardened with visible light beam exposure (1,100 mW/cm2) in the usual manner. An AccuDose® syringe tip (Centrix) with the smallest injection lumen was used for precision material placement. The carious occluso–lingual groove of the maxillary right primary second molar was also repaired with the nano-ionomer. With the idea of future stainless-steel crown restoration, the occlusal pit and disto–occlusal surfaces of the maxillary left primary first molar were restored with RMGI liner material. Preparations of the maxillary molars did not involve frank pulp space exposures, and it was assumed that all carious substance had been removed. Treatment time for all the carious maxillary teeth was 60 minutes once the local anesthesia took effect.
A week later, the patient was once again treated using nitrous oxide/oxygen inhalation, with the stabilizing wraps for safety and comfort, along with musical diversion. At that time, the mandibular posterior teeth were treated under rubber dam isolation. The right second molar (large occluso–buccal), the right first molar (disto–occlusal) and the left second molar (occlusal) were all restored with RMGI liner material, overlaid with the nano-ionomer. The left first molar suffered so much carious damage that, after placement of an RMGI liner, a stainless-steel crown was needed. Treatment for the mandibular molars also was completed in 60 minutes. All of the restored teeth were photographed 26 months after treatment (Figure 7 through Figure 10).
Discussion
RMGI restorative cements are particularly suited for tooth repair such as presented here. The liner coats the prepared dentin and, besides flowing into all mechanical undercuts, forms a chemical bond with the tooth structure. Ruiz and Mitra succinctly outlined all of the advantages of RMGI dentin replacement liners.3 The nano-ionomer overlay has the best physical characteristics of any glass-ionomer system available, and has proven itself durable and reliable since its introduction in 2007.2 The child reported no immediate postoperative sensitivity and none has been reported since treatment time. None of the treated teeth have required additional treatment after 2 years.
Ketac Nano is best applied using syringe injection.2 Immediately after it is mixed, it is sticky and difficult to manipulate, except by slow precision injection, with care taken to avoid air bubbles. If the material is left to congeal a bit for about 30 to 45 seconds, handling is facilitated. The manufacturer supplies the material in either a double-barreled dispenser for usual spatulation, or in a self-mixing capsule. Because the lumen of the tip of the capsule is so large, we routinely inject the mixture into an AccuDose tip for more precision syringing into a prepared tooth.
Besides ending the caries crises for this child, treatment fees were about 75% less than had all the crowns and endodontic treatment been completed. In addition, hospital costs were avoided. Had the child been unable to cooperate and tolerate routine chairside treatment, general anesthesia or sedation would have been needed. The condition of the RMGI materials 2 years after placement is typical of our experiences with Ketac Nano. The only restorative dental care needed since the original treatment time has been an occlusal restoration (distal fossa) for the maxillary left primary second molar, and a stainless-steel crown for the adjacent first molar.
Conclusion
There is much more to pediatric restorative dentistry than operative dentistry procedures for restoration of individual teeth. Sometimes, an interim solution for tooth repair is the best possible option for the child and the family, depending on such factors as the child’s developmental and behavioral status, parents’ attitudes, and the costs of various plans of treatment. The latest RMGI systems can play a valuable role in rapidly and completely ending a “caries crisis.” Compared to alternative materials, they offer properties and advantages that make them faster and easier to use, more durable, and longer lasting.
References
1. Croll TP. Preformed stainless steel crowns: An update. Compend Contin Educ Dent. 1999;20:89-106.
2. Killian CM, Croll TP. Nano-ionomer tooth repair in pediatric dentistry. Pediatr Dent. 2010;32(7):530-535.
3. Ruiz JL, Mitra S. Using cavity liners with direct posterior composite restorations. Compend Contin Educ Dent. 2006;27:347-351.
About the Authors
Theodore P. Croll, DDS
Private Practice in Pediatric Dentistry
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry
University of Washington School of Dentistry
Seattle, Washington
Adjunct Professor
Pediatric Dentistry
University of Texas Health Science Center at San Antonio
San Antonio, Texas
Joel H. Berg, DDS, MS
Dean
University of Washington School of Dentistry
Seattle, Washington