NX3 Nexus™ Third Generation
Minimizing tissue trauma with resin cements.
Final placement and cementation of porcelain veneers and crowns can be traumatic to the surrounding tissue. This can lead to bleeding tissue, prolonged clean-up, recession, and sensitivity. With the use of modern resin cements and careful technique, the trauma can be minimized or avoided all together.
Case Report
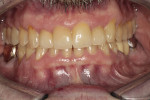
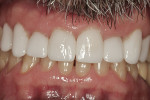
During a hygiene examination, the patient expressed a desire to have a whiter smile as well as restore the recessed areas along his gum line. Eight porcelain veneers were decided on as the best course of treatment (Figure 1).
After anesthesia was administered, retraction cord was placed for 5 minutes and removed. This allowed for preparation closer to the sulcus to avoid lacerating the gum tissue with the diamond bur.
Provisional restorations were placed for the 1-week period while the veneers were fabricated. The provisionals were removed by carefully cutting a groove along the long axis of each tooth and separating the provisionals with a crown remover.
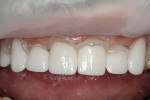
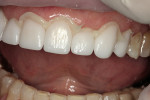
The veneers were tried on using clear try-in gel (NX3 Nexus® Third Generation, Kerr Corporation) to ensure the patient approved of the shape and design of the veneers. The try-in gel is thick enough to allow the patient to sit up to approve the veneers yet washes out easily with water (Figure 2).
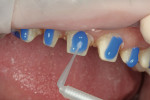
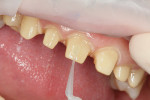
Retraction cord was again placed for 3 to 5 minutes and removed. The prepared teeth were etched (Figure 3) and primed with OptiBond® Solo Plus™ (Kerr). OptiBond Solo Plus was air-thinned and cured for 5 seconds on each tooth (Figure 4).
The veneers were then silanated and allowed to air-dry. Resin cement (NX3) was applied to the restoration and then placed onto the prepared teeth. Once all of the veneers were placed, care was taken to ensure each veneer was properly seated. The resin cement was then spot-cured by waving the curing light for 3 seconds on the buccal and lingual of each tooth. This cured the resin cement to a gel stage that could be easily removed with a scaler. This method is the easiest to clean up but does not give visualization that the veneers are fully cemented before the spot-cure.
A second method is to wipe off the resin cement on the facial. This is done with a cotton roll starting from the tooth and moving onto the gingival. Once each veneer was fully seated, the resin cement was spot-cured for 3 seconds. This method does spread out the cement increasing clean-up time. Once the veneers were spot-cured, floss was very gently used to remove cement interproximally. Care must be taken if floss is used at this point. The resin cement is not fully cured and any bleeding can contaminate the cement (Figure 5).
The veneers were then fully cured for 20 seconds on both the facial and lingual surfaces, and 12-fluted carbide finishing burs were used to carefully remove any remaining cement. This was easily accomplished because at this point the gum tissue was still slightly displaced from the retraction cord.
By using careful technique and resin cements designed to supply not only strong adhesion but remove easily, bonding restorations can be quick and simple with little stress to the dental team or the patient (Figure 6).
Conclusion
This procedure serves as a vivid illustration of the focus of technological innovation in dentistry: While the procedure helps the dental team save time and perform more efficiently, it also has substantial benefit for the patient. This comes in the form of reduced trauma to the tissue, decreased sensitivity and recovery time, and a quicker route to getting the final desired results—in this case, a more esthetically pleasing smile, with minimal wait and discomfort.
About the Author
This article was written by Tony Soileau, DDS, a faculty member of the Institute of Oral Art and Design (IOAD) in Tampa, Florida, and a faculty member of the Pacific Aesthetic Continuum (PAC~Live) in San Francisco, California.
For more information, contact:
Kerr Corporation
Phone: 800-537-7123
Web: www.kerrdental.com
Disclaimer
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dentistry.