Biomimetic, Self-Etch, Direct Composite Restorations
Achieving optimal dentin and enamel bonding with self-etch retained composite restorations.
Adhesion to dentin is more challenging than adhesion to enamel because of its variable tubular structure, high organic content, and positive fluid flow.1,2 Enamel is a highly mineralized and uniform substrate, so the simple application of a 40% phosphoric-acid gel, then rinsing, and drying results in a consistent etch of the enamel surface. The same phosphoric acid applied to the cut dentin leaves an unstable surface due to the unsupported collagen fibrils that collapse when air-dried.
A more biologically compatible conditioning of the cut dentin is accomplished using self-etch adhesives. Unlike the etch/rinse/prime/bond systems, these self-etch bonding agents do not strip off the smear layer or demineralize the dentin. Consequently, the self-etch systems leave the dentinal protein portion in a completely mineralized state that will not interfere with the successful creation of a hybrid layer. Unfortunately, self-etch adhesives do not etch uncut enamel as well as phosphoric acid, so the clinician may elect to employ both systems-which address each of the dental hard tissues separately-to maximize the benefits of each bonding strategy without their associated liabilities.
Enamel Bonding
The application of 32% to 40% phosphoric acid onto enamel has been a routine aspect of restorative dentistry since it was first described by Buonocore in 1955.3 By flowing into the porosities in the enamel created by the acid, the resin forms a stable mechanical bond. Etching of the enamel with phosphoric acid has been shown to eliminate microleakage at the interface between the enamel and the composite restoration,4 as well as creating a consistent and predictable etch of both ground and unground enamel.5
Dentin Bonding
Phosphoric acid has a different effect on cut dentin. The cutting of dentin with burs or diamonds results in the formation of the smear layer, a tenacious film of burnished cellular debris that occludes the dentinal tubules. Adhesive systems that use a phosphoric-acid pretreatment (total-etch) do so because of the necessity to remove this smear layer and decalcify 3 µm to 5 µm into dentin to increase permeability and allow for adequate penetration of the primer and the resin.6
Unfortunately, the demineralization of dentin using phosphoric acid leaves the collagen fiber network in a fragile condition, suspended in the rinse water. If this fibril network is dried too much, the fibrils collapse onto the dentin surface, creating an impermeable organic film that prevents resin penetration and interferes with the formation of the hybrid zone.7 This results in a poor resin-dentin bond leading to gap formation, bacterial infiltration, and recurrent decay, all of which contribute to postoperative sensitivity.8 A weak dentin bond can also occur if the cut dentin surface is allowed to remain too wet, in which case the excess water diffuses into the organic solvents so fast that the adhesive monomers no longer remain dissolved in their solvents. The resulting phase changes that occur result in resin globule and water blister formation. Besides compromising the bond strength, a too-wet surface can create hydraulic pressure within the tubules, leading to fluid movement and dental pain.9
Other factors affect the acid-etching of dentin as well. Once the dentin substrate has been acid-etched, the primer needs to be applied repeatedly to the preparation (8 to 10 times) to fully penetrate the decalcified zone. As a practical consideration, this does not often happen, resulting in voids, bacterial infiltration, and postoperative sensitivity.10
Technique Sensitivity
The dentin must be allowed to remain moist but not too wet after having been etched with phosphoric acid. This way, the collagen fibrils can remain upright while the primer supports and re-expands the fiber network to facilitate resin penetration. Creating the appropriate amount of surface moisture on the dentin surface requires the clinician to operate within the variable and subjective evaluations between what is "too wet" and "too dry." 11 Accordingly, these total-etch systems that rely on the phosphoric-acid pretreatment are considered to be technique-sensitive.
Self-Etch Adhesives
These newer adhesives were developed in response to the difficulty in creating the correct moisture level throughout the entire preparation. The highly acidic primer of self-etching adhesives will etch and prime the dentin simultaneously, thus avoiding the phosphoric-acid pretreatment that removes the protective smear layer and decalcifies the cut dentin surface.
Since self-etch adhesives are designed for use on dry dentin, the difficulty in attaining precise moisture control is not a consideration and clinicians routinely obtain favorable, consistent results. With self-etching, the collagen fibrils cannot collapse during the drying of the dentin because they remain fully supported by the mineralized tissue during the entire bonding procedure. By avoiding the phosphoric-acid dentin treatment, the smear plugs remain in the dentinal tubules, and intratubular fluid movement (with the resulting postoperative pain) is eliminated. Clinicians who routinely use self-etching adhesives report little or no postoperative sensitivity, even in deep restorations.12
While self-etching primers can be effective in creating a thin, strong dentin hybrid zone, they are less effective in etching uncut enamel as deeply as does phosphoric acid, potentially compromising the resin-enamel mechanical bond.13
Therefore, the bond strength to uncut or unetched enamel depends on chemical bonding with acidic monomers such as MDP or 4-META. Because the action of self-etching primers resulted in much less demineralization of intact enamel surfaces, enamel abrasion during cavity preparation can favor the formation of a defined etching pattern, which is what occurs clinically because teeth are prepared with carbide burs or diamonds before restoration. The effectiveness of self-etching adhesives on cut or prepared enamel is reliable and strong, although the effectiveness of self-etching adhesives on unprepared enamel is still less than what is accomplished by phosphoric acid.
Pre-Etch/Self-Etch Bonding Strategy
Pre-etching the enamel prior to beginning the preparation of the tooth is a technique that has been studied.14 By applying the phosphoric acid to the tooth before picking up a handpiece, the clinician avoids its potentially harmful affects on the dentin yet still obtains the benefits of its effect on uncut enamel. Using the antibacterial, milder self-etching adhesive Clearfil™ SE Protect (Kuraray Dental, https://www.kuraraydental.com) on the cut dentin provides a dentin-resin hybrid zone that maintains the protective benefits of the smear layer by keeping the tubules occluded, and avoiding the technique sensitivity of having to maintain the precise moisture levels on the dentin substrate.
Clinical Case
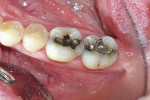
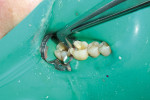
Tooth Nos. 30 and 31 (Figure 1) exhibited signs of recurrent caries, so the decision was made to the remove the failed restorations and replace them with enhanced bonded composite restorations.
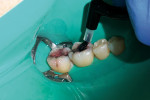
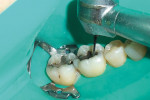
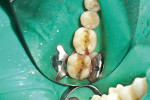
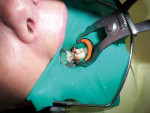
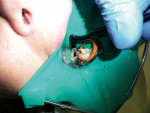
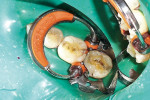
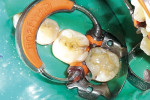
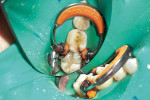
Once the tooth was properly anesthetized, rubber-dam isolation of the field was performed. The entire surface of the tooth and existing restoration was cleaned of plaque with coarse pumice, rinsed, and dried. Using a brush, 40% phosphoric acid was applied (Figure 2) over the entire occlusal surface (K-Etchant gel, Kuraray) for 15 seconds, then rinsed and dried (in order to visualize the frosted appearance of the enamel that would indicate a successful etch). The old amalgam restoration was removed (Figure 3) using a 330 carbide bur (Tri Hawk, store.trihawk.com) and the cut dentin was stained to check for caries (Caries Detector Solution, Kuraray). The cavity walls were created with a tapered shoulder former diamond so that they were completely free of stain, and then diverged occlusally, similar to a cast inlay preparation. Dentin cracks were removed with a round bur No. 4 on the high-speed handpiece, and caries was removed using the No. 4 round bur on the low-speed handpiece under irrigation. Once the preparation was complete (Figure 4), a sectional matrix band (Composi-Tight Sectional Matrix, Garrison Dental Solutions, https://www.garrisondental.com) was inserted proximally using the special forceps such that the top of the matrix band extended minimally above the marginal ridge of the adjacent tooth (Figure 5). A plastic wedge was selected from the kit that provided maximum separation of the teeth yet still was able to pass through to the lingual. Once in position, the wedge handle was twisted so that it separated, leaving the wedge in its proper position to separate the teeth and secure the sectional matrix. Then the ring was clamped into position (Figure 6) using the specialized clamp forceps, the wedge inserted a little further, and the matrix burnished against the adjacent tooth using the multi-functional instrument (TN009, Garrison Dental Solutions). As there was no tooth contact posteriorly, no matrix was required to restore the distal aspect of the preparation.
Once the matrix assembly was secured, the dentin bonding process was begun by applying the antibacterial self-etch primer (Clearfil SE Protect) for the required 20 seconds to the entire preparation (cut dentin and cut enamel, Figure 7). After this conditioning process, the preparation was dried for 20 seconds until the preparation was completely dry.
Then the microfilled resin (bottle No. 2, Clearfil SE Protect) was applied and thinned out with the surgical suction tip and a quick puff from the air syringe, then polymerized for 20 seconds using a standard curing lamp. Next, a dentin-replacing composite (Clearfil AP-X) was applied to the proximal walls, keeping it confined to the enamel,15then cured using a slow-start protocol for 20 seconds from about one half inch away, followed by a 10-second waiting period, followed by another 20-second cure (20/10/20) with the lamp as close to the case as possible (Figure 8). This cure technique has been shown to be effective in reducing the polymerization stress that is transferred to the margins of the restoration.16
Next, a thin liner of flowable composite (Clearfil Majesty Flow, Kuraray) was syringed onto the pulpal floor, keeping it away from the cavity walls to minimize polymerization stress, then light-cured (Figure 9). The bulk of the restoration was then built up horizontally using the dentin replacement composite (Clearfil AP-X) and light-cured according to the 20/10/20 photoactivation method until the DEJ was reached. A 5-minute pause before connecting the enamel and the dentin with a composite increment (described as "de-coupling") will minimize the stress to the dentin bond as it would otherwise cure toward the enamel.17
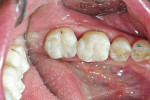
The enamel was restored using increments of a posterior composite (Clearfil Majesty Posterior) placed at an angle to the vertical walls of the preparation to approximate the cuspal inclines and occlusal anatomy (Figure 10). Once the material was fully cured within the cavity preparation, the rubber dam was removed and the occlusion was checked. Prematurities were removed using a shoulder former diamond to maintain the cuspal inclines and occlusal anatomy. Coarse Sof-Lex™ disks (3M ESPE, https://www.3mespe.com) were then used to shape the proximal contours. After the occlusion was correct, flash was removed with a scaler and rubber points and pumice were used to create the final surface. Tooth No. 30 was then restored with the same method (Figure 11). The patient reported no tooth discomfort of any kind on the follow-up telephone call.
Discussion
Total-etch adhesives using a 32% to 40% phosphoric-acid pretreatment are highly effective and predictable in preparing for a resin-enamel bond, but the use of phosphoric acid on cut dentin risks creating an unstable substrate where bond strength can be reduced dramatically. Self-etch adhesives are easy to use and reliably create strong bonds to cut enamel and to dentin; however, their bond to uncut enamel is less than what is produced after a phosphoric acid-etch. Taking these factors into account, the use of phosphoric acid on uncut enamel before opening into dentin, followed by the routine use of an antibacterial, self-etching adhesive is a logical next step toward a more durable resin bond to both hard tissues.
Additional improvement of the resin-tooth bond is achieved by lowering polymerization stress during composite placement by the use of decoupling the enamel and dentin bonds to the resin, by careful placement of composite increments and slow-start curing.
Disclosure
The authors have received honoraria from Kuraray Dental.
References
1. Nakabayashi N, Kojima K, Masuhara E. The promotion of adhesion by the infiltration of monomers into tooth substrates. J Biomed Mater Res. 1982;16(3):265-273.
2. Tay FR, Gwinnett JA, Wei SH. Micromorphological spectrum of acid conditioned dentin following the application of a water-based adhesive. Dent Mater. 1998;14 (5):329-338.
3. Buonocore MG. A simple method for increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res. 1955;34(6):849-853.
4. Retief DH, Woods E, Jamison HC. Effect of cavosurface treatment on marginal leakage in class V composite resin restorations. J Prosthet Dent. 1982;47(5):496-501.
5. Retief DH. Effect of conditioning the enamel surface with phosphoric acid. J Dent Res. 1973;52(2):333-341.
6. Van Meerbeeck B, Inokoshi S, Braem M, et al. Morphological aspects of the resin-dentin interdiffusion zone with different dentin adhesive systems. J Dent Res. 1992;71(8): 1530-1540.
7. Carvalho RM, Yoshiyama M, Pashley EL, Pashley DH. In-vitro study on the dimensional changes of human dentine after demineralization. Arch Oral Biol. 1996;41(4):369-377.
8. Gwinnett AJ. Dentin bond strength after air drying and rewetting. Am J Dent. 1994;7(3): 144-148.
9. Brannstrom M. The hydrodynamic theory of dentinal pain: sensation in preparations, caries and the dentinal crack syndrome. J Endod. 1986;12(10):453-457.
10. Gwinnett AJ. Dentin bond strength after air drying and rewetting. Am J Dent. 1994;7(3):144-148.
11. Pashley DH. The evolution of dentin bonding from no-etch to total-etch to self-etch. Adhes Tech Sol. Premier Issue. 2004:1-6.
12. Christensen GJ. Self-etch primers are here. J Am Dent Assoc. 2001;132(7):1041-1043.
13. Erickson RL, Barkmeier WW, Kimmes NS. Bond strengths of self etching adhesives to pre-etched enamel. Dent Mater. 2009;25(10):1187-1194.
14. Rosenberg JM. The pre-etch technique for achieving enamel bond strength with self etching systems. Pract Proced Aesthet Dent. 2004;16(10):764, 766.
15. Deliperi S, Bardwell DN. An alternative method to reduce polymerization shrinkage in direct posterior composite restorations. J Am Dent Assoc. 2002;133(10):1387-1398.
16. Charton C, Colon P, Pla F. Shrinkage stress in light cured composite resins: influence of material and photoactivation mode. Dent Mater. 2007;23(8):911-920.
17. Nikolaenko SA, Lohbauer U, Roggendorf M, et al. Influence of c-factor and layering technique on microtensile bond strength to dentin. Dent Mater. 2004;20(6):579-585.
About the Authors
Randall G. Cohen, DDS
Private Practice
Newtown, Pennsylvania
Michael V. Razzano, DDS
Private Practice
Woodstock, Georgia