Optimizing the Occlusal Plane Prior to Restoration
An interdisciplinary, digitally planned approach using removable aligners with auxiliary anchorage
Andrew Ferris, DDS, MS | Marc Alexander, BDS, MS | Marc Bienstock, DDS, MD
In complex cases involving occlusal plane discrepancy and restorative treatment, interdisciplinary collaboration between the restorative dentist, the orthodontist, and the oral surgeon is essential. When working as an interdisciplinary team, clinicians are able to achieve optimal cosmetic and functional results. Transitioning from an analog treatment planning approach to a digital approach can be very valuable for interdisciplinary teams. The initial records, which include cone-beam computed tomography (CBCT) scans, intraoral scans, dynamic video, and photographs, have enhanced the ability of clinicians to educate the patient, treatment plan, and communicate with the rest of the interdisciplinary team. The position of the maxillary incisors within the face and the dynamic smile is critical in determining the occlusal plane to achieve both excellent esthetics and optimal function. This article illustrates how clear aligner therapy with skeletal anchorage can be used to control the vertical position of the anterior and posterior teeth, creating a more ideal occlusal plane in preparation for restorative treatment.
Overview of Esthetics and Function
There is a direct correlation between esthetic dentistry and optimal occlusion. Form follows function; therefore, occlusion should be closely evaluated if the goal is a healthy and esthetic result. Although the vertical position of the maxillary incisors is critical for esthetics, the vertical position of these teeth in relation to the posterior teeth is critical for function. If the occlusal plane from anterior to posterior is not carefully planned and executed, issues such as dental wear, joint symptoms, and destruction of restorations can occur.1 Posterior balancing and nonbalancing contacts as well as working and nonworking interferences can result if the maxillary posterior occlusal plane is inferior to the maxillary anterior occlusal plane.2 This S-curve occlusal plane (in the sagittal view) translates to a lack of anterior guidance in class I occlusion. In deep class II division 2 occlusion with a reverse S-curve, accelerated wear of the anterior and posterior teeth can transpire.3
Incisal Position
Treatment planning for where the incisors should be located within the face can be challenging because this position is part of a dynamic system. Using technology that can combine video of the patient talking and smiling, intraoral scans, CBCT images, and photographs, it becomes easier to treatment plan the desired position and smile line. Traditionally, there are acceptable standards that have been applied, but with 3D digital planning, clinicians are better equipped to "interdisciplinarily" agree on the optimal position.4-11
The Occlusal Plane and Wear
The occlusal plane should always be considered to ensure optimal function. The curve of Spee and curve of Wilson are important in discussions of teeth regarding protected function. Plunging palatal cusps of the maxillary posterior teeth can be destructive to the posterior teeth and joints, just as a deep bite from an increased curve of Spee can be destructive to the anterior teeth. On the contrary, if there is a shallow or open bite in the anterior, there may not be a mutually protected occlusion, which can cause an increase in balancing and nonbalancing posterior interferences.3,12
If the occlusal plane is not optimized, dental wear can occur. The enamel is more resistant to wear, but as wear penetrates into the dentin, that resistance is reduced, and the teeth can wear faster. This can be exacerbated by extrinsic and intrinsic erosive factors and parafunctional habits. As teeth wear, they tend to supraerupt in order to maintain contact. Depending on the rate of wear, loss of vertical dimension can occur; however, the vertical dimension of occlusion may be maintained if the eruption of the teeth is commensurate with the wear.13 Wear can also cause rotation of the occlusal plane, which furthers the potential for destruction.
Case Report
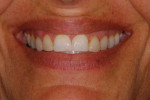
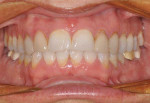
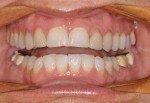
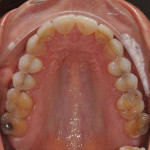
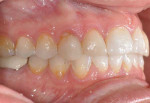
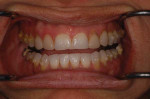
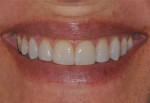
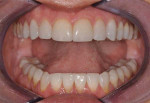
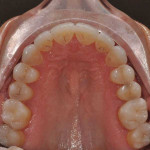
A 51-year-old female patient presented to her prosthodontist for cosmetic reasons. She stated that she did not like the look of her smile and that she thought that her front teeth appeared short (Figure 1 through Figure 3). Specifically, the patient explained that she never liked the look of her teeth, including the color and shape of her existing veneers on teeth Nos. 6, 7, 10, and 11, which were 25 years old (Figure 4).
Initial records were taken by the prosthodontist. The examination revealed a negative incisal smile line and gingival disharmony. The maxillary occlusal plane had a distinct S-curve with the central incisors superior to the posterior occlusal plane in the frontal and sagittal views. The natural central incisors exhibited incisal attrition with less than 1 mm of exposure in repose. Regarding the mandibular occlusal plane, the patient demonstrated a two-step occlusion with supraeruption of the mandibular incisors displayed in the incisal plane and gingival crests. The maxillary incisors were in a good vertical position facially and in her smile. However, the posterior teeth were inferior to the occlusal plane of the incisors (Figure 5).
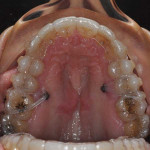
Excessive gingival display was present in the buccal corridors with posterior occlusal wear. The maxillary posterior teeth revealed a multifactorial etiology of wear, including attrition of the occlusal surfaces and erosive wear indicated by the satin surface texture of the enamel and dentin. Erosion of the maxillary molars' lingual surfaces had occurred, and no enamel remained on their occlusal surfaces (Figure 6). After intrinsic and extrinsic sources of acid were discussed with the patient, an analysis was performed.14-16 Her mandibular molar crowns with metal occlusal surfaces had undergone work hardening resulting from functional and parafunctional mandibular patterns. In addition, shallow protrusive and lateral guidance resulting from wear of the maxillary central incisors and mandibular cuspids as well as the S-curve occlusal plane exacerbated the posterior attrition.
Relatively greater wear of the posterior teeth when compared with the anterior teeth could be a result of an anterior open bite, shallow excursive guidance, a large discrepancy between centric relation and maximum intercuspation position, flat condylar eminence, or acid erosion (ie, intrinsic, extrinsic).17,18
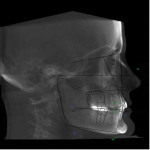
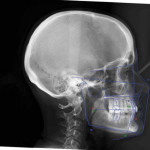
Recognizing the challenges inherent in treating this patient restoratively without correcting the occlusal plane, the patient was referred to the orthodontist. Additional records were taken, including a CBCT scan and an intraoral scan (iTero® Element, Align Technology). The orthodontic findings revealed that the patient was brachyfacial and possessed class I occlusion with mild crowding (Figure 7 and Figure 8).19 Additional findings included that her facial thirds demonstrated correct proportions with a flat to convex profile, she had wear on teeth Nos. 8 and 9 with short clinical crowns and a discrepancy between the vertical position of the anterior and posterior teeth, and she exhibited mild, generalized gingival recession.
Treatment Planning
A treatment plan that would produce the best overall outcome was desired. The poor esthetics and wear in the posterior region could be corrected with surgical crown lengthening of the posterior maxillary quadrants and aggressive tooth preparation and restoration. Alternatively, a more conservative treatment with regard to tooth preservation could be achieved through orthodontic correction of the occlusal planes (ie, intrusion of the posterior occlusal plane, leveling of the mandibular curve of Spee), followed by the placement of ceramic veneers in the maxillary anterior region and porcelain tabletop onlays in the maxillary posterior region as well as replacement of the failing mandibular posterior crowns and composite bonding of the worn incisal edges of the mandibular anterior teeth. In this manner, a mutually protected occlusal scheme could be created.20
The intraoral scanner and its software allowed for the simulation of tooth movement so that the restorative dentist and orthodontist could digitally position the teeth, creating an optimal orthodontic treatment goal.
The main challenge in this case was the orthodontic anchorage that would be required to achieve the desired tooth movement. Because the maxillary incisors were in a good position vertically, but the maxillary posterior teeth were below the occlusal plane, trying to intrude the posterior maxillary teeth would tax the anchorage of the anterior teeth, which could move them inferiorly or extrude them and ultimately compromise the outcome. Therefore, the patient was referred to the oral surgeon in order to develop a plan to use auxiliary skeletal anchorage to support the posterior intrusion.
Interdisciplinary Treatment
Ultimately, two bone plates attached to the zygoma on both the right and left sides and two plates attached to the palate were selected as appropriate anchorage. Clear aligners (Invisalign®, Align Technology) were the orthodontic appliance of choice to position the teeth for restorative treatment. The aligners were designed to keep the maxillary anterior teeth in their current vertical positions. The patient's teeth would be aligned, and her maxillary and mandibular arch forms would be idealized for her face with some mild transverse expansion. The maxillary posterior teeth (ie, premolars and molars) were programmed to intrude 2.75 mm. The desired intrusion of these teeth was actually 2 mm, but 2.75 mm would allow for some overcorrection because the intrusion of posterior teeth is a difficult orthodontic movement, and the teeth do not always respond one-to-one to what is programmed in the orthodontic planning software (ClinCheck®, Align Technology).
The bone plates were attached to the palate and the right and left zygomas. After placement, they were immediately loaded with 3/16 in 6 oz orthodontic elastic that the patient would reinsert each time she seated her maxillary aligner. The elastic connected the plate hook on the palate to the plate hook on the zygoma, bilaterally, which created an intrusive effect by compressing the aligner occlusally with the force necessary to intrude (Figure 9). To prevent unwanted extrusion, composite attachments were not placed on the incisors. The quantity of tooth movement was carefully monitored and evaluated at each follow-up appointment using the intraoral scanner's progress tracking feature, which compares historical scans with the current scan in a visual to show how the teeth are responding. Once the alignment was correct, arch forms idealized, and planned posterior intrusion performed, the patient was ready for the restorative phase of treatment (Figure 10).
After removal of the composite attachments and previous restorations, laboratory-fabricated provisional veneers (New Outline, Anaxdent) and onlays (Integrity®, Dentsply Caulk) were placed. The provisional restorations would be used as a blueprint for the final ceramics. Esthetics, form, and function were evaluated and modified during the following weeks until both the patient and dentist were satisfied.
On the day of delivery of the final restorations, rubber dam isolation was achieved, and the preparations were pumiced with chlorhexidine and medium pumice and then sandblasted. The final layered lithium disilicate maxillary veneers and the final monolithic lithium disilicate posterior onlays and crowns (IPS e.max®, Ivoclar Vivadent) were etched with 4.5% hydrofluoric acid and then cleaned in an ultrasonic bath with alcohol or using steam. Two layers of a universal primer (Monobond® Plus, Ivoclar Vivadent) were then applied and allowed to air dry. The veneers were bonded with a total etch technique using an adhesive (OptiBond FL®, Kerr) and a resin luting cement (Da Vinci Resin Cement, Cosmedent). Light curing was performed in 90-second cycles, starting from the lingual then moving to the facial and proximal surfaces. After a final glycerin-covered cure was performed on all surfaces, the excess cement was removed with a No. 12 scalpel blade, the occlusion was adjusted, and the restorations were polished. The final posterior restorations were placed using the same bonding protocol, but the onlays were placed with a different luting composite (Variolink® Esthetic DC, Ivoclar Vivadent), and the crowns were placed with a different adhesive (Clearfil SE™ Protect, Kuraray Noritake) and resin cement (Panavia™ SA Cement Universal, Kuraray Noritake) (Figure 11 through Figure 18).
Discussion
In this case, clear aligners were the orthodontic appliance of choice for a variety of reasons, including the patient's desires, increased anchorage control, the ability to design selective tooth movement within the software, and the orthodontist's preference for this type of orthodontic movement. With the addition of removable aligner therapy to the orthodontic treatment possibilities, many patients who previously refused conventional treatment with bonded brackets may now be willing to proceed. However, patient compliance is essential to the success of this treatment modality.
Although the aligners were primarily used to maintain the anterior vertical position while using skeletal anchorage to facilitate the posterior intrusion, another advantage of the aligners in this case was that they protected the teeth from additional wear while the correction was taking place. This contributed to the restorative doctor's ability to employ minimally invasive tooth reduction and retain as much of the tooth structure as possible. Aligning and leveling the cementoenamel junctions of the teeth with orthodontics prior to restorative treatment also facilitated minimal crown reduction and the elimination of crown lengthening.
Using the orthodontic planning software in combination with the digital records allowed for the proper planning of tooth movement in all 3 planes of space with accuracy to a tenth of a millimeter.
The orthodontic treatment phase is usually the most time-consuming component of a complex interdisciplinary case; however, if designed properly, clear aligner treatment can oftentimes be more expeditious than bracket and wire. The patient in this case underwent 24 weeks of aligner treatment in conjunction with the osseous anchorage and elastic wear, but she required 12 months of aligner therapy in total to gain the correction needed before placing restorations.
Osseous Anchorage
The zygoma and palate are both very stable anatomic sites to place bone plates. Bone plates were chosen due to their superior stability when compared with traditional temporary anchorage devices (TADs). The bone plates and clear aligners allow for the force of the connected elastic to be directed down the long axis of the teeth, while preventing the unwanted buccal tipping that can occur during intrusion using TADs with traditional braces. Once the desired tooth movement is accomplished, the bone plates can be removed.
Smile Esthetics
The position of the upper incisors, especially at the gingival margins, is essential to a cosmetic result. When they are in the correct position, the proper tooth dimensions and position of the smile line can then be optimized with restorative treatment. An inferior position of the posterior maxillary teeth can create excessive gingival display in the buccal corridors. Intruding these teeth not only corrects occlusal interferences but can also greatly improve smile esthetics.
Function
A major key to the longevity of restorations is establishing a protected occlusal scheme. In this case, the creation of anterior guidance that was comfortable and nondestructive while alleviating posterior destructive contact in working and nonworking side movements was the goal. In addition, providing improved axial tooth inclination with orthodontic treatment allows for less compromise in function. When not managed properly, a lack of anterior guidance can result in peripheral symptoms of bruxing, muscle spasm, and joint dysfunction. Provisional restorations made from dental materials that are compatible and functionally correct can confirm guidance and the elimination of parafunctional habits prior to final restoration.
Conclusion
The occlusal plane is very important to the functional and esthetic outcomes of restorative cases. Digital design has given us improved ways to diagnose and treatment plan cases in all aspects but especially when evaluating the vertical position of the anterior and posterior teeth. Many patients who have been willing to forego needed restorative treatment because they refuse to wear conventional braces are amenable to clear aligner therapy provided by the orthodontist. This can provide restorative dentists with a new group of patients who can be conservatively treated. When clear aligners are combined with auxiliary anchorage using bone plates, tooth position can be optimized in ways that were not previously possible. This case provides a great example of how collaboration among an interdisciplinary team that leverages the advantages of digital treatment planning, clear aligners, and auxiliary anchorage can facilitate optimal occlusion and excellent restorative outcomes.
About the Authors
Andrew Ferris, DDS, MS
Orthodontist
Lecturer
Loma Linda University
School of Dentistry
Loma Linda, California
Private Practice
Santa Barbara, California
Marc Alexander, BDS, MS
Prosthodontist
Associate Professor (Retired)
University of Southern California
School of Dentistry
Los Angeles, California
Private Practice
Santa Barbara, California
Marc Bienstock, DDS, MD
Oral Surgeon
Diplomate
American Board of Oral and
Maxillofacial Surgery
Private Practice
Santa Barbara, California
References
1. Spear F. Interdisciplinary management of worn anterior teeth: facially generated treatment planning. Dent Today. 2016;35(5):104-107.
2. Dawson PE. Evaluation, Diagnosis, And Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: Mosby; 1989:1-28.
3. Brose MO, Tanquist RA. The influence on anterior coupling on mandibular movement. J Prosthet Dent. 1987;57(3):345-353.
4. Coachman C, Alexandre MA, Sesma N. Dynamic documentation of the smile and the 2D/3D digital smile design process. Int J Periodontics Restorative Dent. 2017;37(2):183-193.
5. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
6. Spear F. Too much tooth, not enough tooth. JADA. 2010;141(1):93-96.
7. Ackerman, MB. Digital video as a clinical tool in orthodontics: dynamic smile design in diagnosis and treatment planning. Monograph: 29th Annual Moyers Symposium. Vol 40. Ann Arbor, MI: University of Michigan Department of Orthodontics; 2003.
8. Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning--part II. Am J Dentofacial Orthop. 1993;103(5):395-411.
9. Zachrisson BU. Esthetic factors involved in anterior tooth display and the smile, vertical dimension. J Clin Orthod. 1998;32:432-445.
10. Kokich VO, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. J Esthet Dent. 1999;11(6):311-324.
11. Sarver DM. The importance of incisor positioning in the esthetic smile: the smile arc. Am J Orthod Dentofacial Orthoop. 2001;120(2):98-111.
12. Schuyler C. An evaluation of incisal guidance and its influence in restorative dentistry. JPD. 1959;9(3): 374-378.
13. Turner KA, Missirlian DM. Restoration of the extremely worn dentition. J Prosthet Dent. 1984;52 (4):467-474.
14. van't Spijker A, Kreulen CM, Creugers NH. Attrition, occlusion, (dys)function, and intervention: a systematic review. Clin Oral Implants Res. 2007; 18(Suppl 3):117-126.
15. Litonjua LA. Andreana S, Bush PJ, Cohen RE. Tooth wear: attrition, erosion, and abrasion. Quintessence Int. 2003;34(6):435-446.
16. Bishop K, Kelleher M, Briggs P, Joshi R. Wear now? An update on the etiology of tooth wear. Quintessence Int. 1997;28(5):305-313.
17. Spear F. A patient with severe wear on the anterior teeth and minimal wear on the posterior teeth. J Am Dent Assoc. 2008;139(10):1399-1403.
18. Spear F. A patient with severe wear on the posterior teeth and minimal wear on the anterior teeth. J Am Dent Assoc. 2009;140(1):99-104.
19. Steiner CC. Cephalometrics for you and me. American Journal of Orthodontics. 1953;39(10):7 29-755.
20. Schwartz H. Occlusal variations for reconstructing the natural dentition. J Prosthet Dent. 1986;55(1): 101-105.