Splints Are Not Just for TMD Therapy
Greg Vigoren, DDS; and Edward A. McLaren, DDS
Dentistry in its simplest terms is about controlling bacteria, getting good marginal seals on restorations, and controlling the stresses that break restorations and open marginal seals. Traditionally, the use of splints has been for occlusion or temporomandibular disorders (TMD). Properly made and well-adjusted occlusal splints can help control parafunctional stresses that are applied by the patient to their natural teeth and the restorations that dentists fabricate for them. This in turn should lessen the possibility for restoration fracture from overload and help to maintain marginal seals because the splint would minimize the tooth flexure that puts stress on restorative interfaces.
Much of today’s restorative dentistry is driven by esthetics. Because of patient desires, dentists are using more and more composite, all-ceramic, or metal-free restorations. Dentists are forced to build up porcelain incisally and execute full occlusal replacements with ceramic material. It has been documented that most adult patients brux at night, especially under periods of high stress.1 During periods of bruxing it is difficult to control the applied occlusal stresses without the use of some sort of splint. Wearing a splint (sometimes called a nightguard) gives a measure of protection to the teeth and restorations. The acrylic, which is somewhat flexible and resilient compared to porcelain, will give a little under load and wear when abraded. When a patient bruxes against the splint, there is a stress-dampening effect compared to porcelain against porcelain or porcelain against enamel. It has been the authors’ experience that patients who routinely wear occlusal guards at night after they have had significant tooth restoration will have greatly increased longevity to those restorations. In fact, in the authors’ practice there are no warranties on breakage unless patients regularly wear their splints. This protective device helps share both responsibility and accountability with the patient.
The many uses of splints will be covered in this two-part article. Diagnosis, indications, patient education, and the verbal skills necessary to gain the acceptance of this treatment and get the long-term compliance necessary for the success of this treatment will be discussed in the first segment. The materials, technique, adjustment, and delivery will be covered in the second installment.
UNDERSTANDING FLEXURAL FORCES
About 19 years ago in Hawaii, the top of an airplane was ripped off in flight (Figure 1). The causes of that tragedy were determined to be repetitive compression/elongation cycles. The air corridor where the accident occurred had more short hops, causing many more pressurization/decompression cycles than the average plane would experience in a lifetime, which led to failure much sooner than the industry had expected.2
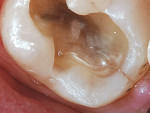
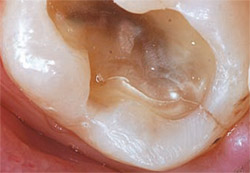
In dentistry, dentists experience these same forces in natural teeth, in materials, and at the interfaces between those two surfaces. Loading and lateral force cause a flexural force in those materials that results in repetitive compression/elongation cycles. With a brick wall it is not always the bricks that fail, but, more commonly, the mortar, the seal, or the interface in between the bricks that fails. In dentistry, whether that is a natural transition between different kinds/types of tooth structure, a bonded, luted, or cemented interface, the repetitive flexural force acts at the interface, causing failure over time and microleakage. Microleakage, margin failure, recession, abfractions, breakage, fractures, debonding, tooth sensitivity, and excessive or accelerated wear (Figure 2 and Figure 3) are some but not all of the signs of these destructive forces. Boney exostosis, mandibular tori, and corrugated borders of the tongue in addition to the standard signs of muscular, joint, and head-and-neck problems are red flags of these excess forces. A restorative dentist’s job is to control and minimize those forces and push that inevitable failure as far as possible into the future. Splint therapy is one of those underdiagnosed and underused treatments that can effectively be used in the preventive treatment of the force-flex-failure cycle.
Taking into account that the first permanent teeth erupt at age 6 or 7 and the average life span is 86 years, the average adult patient needs his or her teeth for almost 80 years. The concepts of predictability, durability, and avoidance of catastrophic failure are as important in any successful long-term strategy or philosophy of treatment as comfort, function, and esthetics. Preventing failure or spreading out the time in between failure cycles is paramount in any philosophy that allows patients to have the use of their teeth for a lifetime.
The purpose of a splint is to disadvantage the natural forces that can be directed at the teeth mechanically, neurologically, and physically. With this splint the nocturnal parafunctional forces cannot be concentrated on a single tooth or group of teeth, except for the lower cuspids, which not only have these forces reduced significantly because of their position in the arch but also have the best ability to resist these forces because of both root length and root structure. The reduction of force in the preceding statement is based on the simple physics of levers, force applied, fulcrum, and force generated. The root length and root structure reference comes from undergraduate dental school or the observations of any sets of radiographs. Cuspids have the longest roots of any teeth in either arch, they have the largest cross-sectional form of any roots, and the largest surface area, which translates to resistance to flexion and resistance to movement based on surface area and periodontal ligament. Dentin is one of the force-absorbing materials/mechanisms in the dentition but it is also its weakest link. The primary purpose of preventive splint therapy is to lower the nocturnal parafunctional forces in the mouth below the threshold where dentin fails and where marginal interface failure occurs.
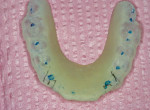
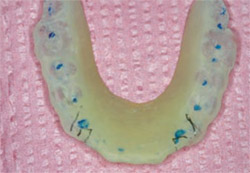
The splint, nightguard, or orthosis appliance being described in this article is a type A, non-positional, flat-plane maxillary splint. It has single-point contact per tooth in the posterior areas and light anterior contact with mild cuspid guidance in the anterior (Figure 4). This concept and these materials can be used and on occasion are fabricated on the mandibular arch.
THE MANY USES OF A SPLINT
A splint may be used to acclimate or show a normal occlusal relationship pretreatment to the skeptical or unknowing patient. If you have a comfortable and correctly fitted splint, it can deprogram a learned or acquired occlusion that could have been based on interferences between the acquired centric relationship and centric relation. How the patient occludes on first closure in the morning without that splint’s guidance represents the relaxed joint relationship and gives an unforced, reproducible centric relationship. This can be used to demonstrate the need for orthodontics, occlusal work, and equilibration or splint therapy.
The authors’ clinical experience has demonstrated that splints may be used to calm an inflamed joint or the musculature of a patient with a difficult occlusal relationship before attempting to equilibrate. Pretreatment splints may be used to make the task of obtaining interocclusal records easier. This process can be used to get the difficult patient ready to take more accurate interocclusal records by wearing the splint to the office. With the face-bow already taken, the models already poured and trimmed, and the maxillary cast mounted, the interocclusal record can be taken, verified, and used to mount the lower cast.
Splints may be used as a diagnostic tool to find an offending tooth (one needing root canal therapy) that is triggering multiple sensitive teeth through bruxing. Splints can also be used after orthodontic cases are finished to stabilize and retain teeth. Splints can help weakened anterior teeth (those with post-and-core and little or no ferrule) by minimizing the load applied to the tooth/restoration. In the authors’ practice, splints have helped to calm sensitive teeth and facilitate accurate endodontic diagnosis vs pain from occlusal trauma.
PATIENT ACCEPTANCE AND COMPLIANCE
How do you get the patient to accept this treatment? Beyond that, how do you get patients motivated to comply and wear their splints over the long time period necessary to benefit from this treatment? Communication is the key; if properly motivated, the authors have found that 50% of patients in their practice wear their splints regularly. The goal of this communication and patient education is to give the patients the information to choose the treatment that is in their own best interest. It should be explained to the patient that splints are a routine part of restorative treatment and that, in the authors’ clinical experience, by wearing a splint nightly all restorative dentistry may last 2 to 4 times longer and normal tooth wear is almost stopped with long-term use.
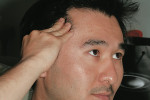
It is easy to demonstrate an experience that conveys to the patient this concept of force and the need for control. Ask patients to place their fingers on their temples lightly while biting on their back teeth so they can feel the contraction/ bulge of their temporalis muscle (Figure 5). Now, with their fingers in the same place have them bite on their front teeth only. Go back and forth several times. Next have them move down to their masseter muscle and repeat this process by biting on the front teeth and then the back teeth several times. This demonstration can be coupled with the explanation that a splint with the same characteristics of a front-tooth protective bite designed into it will neurologically shut down 80% of the strength of the muscles in flexing the teeth in a grinding mode. Or, stated differently, they can bend their teeth with five times the force if they can engage their back teeth in excursive movements (protrusive and lateral movements).
Another explanation that helps patients to understand some of these mechanical concepts and relationships involves a simple nutcracker. Drawing a nutcracker and a simple jaw joint muscle sketch makes a great visual tool. If you place the nut at the hinge end of the nutcracker you break it quite simply (Figure 6); if you place it at the end of the handle, they call you the nut (Figure 7). This is the same mechanical advantage that exists with the jaws; by moving the forces to the front teeth, your natural muscular strength is mechanically disadvantaged 70% to 90%, just like the forces at the handle end of the nutcracker. This is another natural mechanism that reduces the effects of the bruxing and grinding forces.
Worn crayons are the last physical prop that the authors use to demonstrate the mechanics of tooth wear. They are easy to make and have a strong visual ability to communicate. Everyone has had them; everyone knows the difference between new ones and worn ones. Get a 16-crayon box and tape them all together as they would fit in the box and put them back in the box. Now take them to the street/ sidewalk and wear them down at an angle so the two crayons on one end are untouched with the wear graduating to very heavy on the other end. Now put them at a 45° angle on one side and do the same thing by putting little or no wear on the first, unworn crayon graduating to halfway through the worn-down last one (Figure 8). Use this prop as a guide when showing patients the models of their teeth. You can now visually show vertical wear as well as lingual/lateral wear and the crayons allow patients to understand both the type and amount of wear that may be understandable and very visible to you but not to them.
COMPLIANCE
How do we know if patients wear their splint? You can ask, but patients sometimes hide this information. One technique is to leave extremely small articulator marks on the splint in the areas where there is cuspal contact. When the patients come in, look with some form of magnification for remnants of the occlusal marks. If they are there, the splint is not being worn much. In such instances, encourage them to come in and have whatever seems to bother them adjusted or refitted. Offering to credit them their costs also encourages them to discuss compliance. Surprisingly, the authors’ most common office emergency is if a patient loses or breaks a splint.
When patients do not wear their splints regularly and things happen, it is on their ticket. Of the approximate one third of those who do not wear their splint regularly or do not wear it at all, they assume responsibility for failure when it happens. Of those, it has been the authors’ experience that a very high percentage converts to wearing a splint after they see a personal failure in their mouth instead of asking the more common question: "Why did your work fail?"
FEES FOR SPLINT THERAPY
Here some philosophical and psychological discussion may be necessary. For the fee to be appropriate you should be able to justify that procedure at the same hourly rate as your standard restorative procedures. This should not be something you routinely give away because it is one of the most valuable services you can give to your patients. If your fees represent both your true costs and the profit necessary to stay in business, then you can always discount your services when you want and to whom you want. The fee should represent the time and expertise necessary not only for fabrication, delivery, and follow-up, but also the time necessary for records, diagnostic casts, diagnosis, communication, education, motivation, and the original time necessary for both the continuing education and the learning curve necessary to get yourself and your staff up to speed. A big part of this procedure is the education and motivation of the patient. Without patient compliance a splint is just an expensive trinket, as useless as the never-worn, old, ill-fitting partial it replaces.
As a general rule, the authors recommend at least the same as or more than your crown fee as a good place to start. If this is a second splint (ie, one was lost or worn out), one half the normal fee is quite adequate as education, motivation, and communication are significantly reduced. Many, if not most dentists will build the cost of the splint into the comprehensive case fee.
The authors believe so strongly in the uses of splints, as discussed earlier, that for those who have doubts the authors give them a 90-day money-back guarantee. If they cannot wear it, do not wear it, or feel it has been of no use, they can return it after 90 days for a full refund, no questions asked. There is no value in a device that does not work, does not have a purpose, or is not worn. There have been very few instances where the authors have had to return money.
CONCLUSION
Why treat with splints? It is good for the patient. It is good for dentistry. It is good for you. The use of well-made splints means less failure, less frustration, and frequently results in the transfer of ownership of failure to the real culprits—the patients and the forces they generate in the night. As stated earlier, the authors tell their patients that if they will wear their splints, the dental work will last two to four times longer. Through experience, the authors have found that patients, if well educated and informed, will most often choose what they believe is in their own best interest.
References
1. Okeson JP, Phillips BA, Berry DT, Baldwin RM. Nocturnal bruxing events: a report of normative data and cardiovascular response. J Oral Rehabil. 1994;21(6): 623-630.2. National Transportation Safety Board, Aloha Airlines, Flight 243, Boeing 737-200, N73711, Near Maui, Hawaii April 28, 1988. Aircraft Accident Report NTSB/AAR-89/03. Washington, DC: NTSB, 1989.
 |  | |
| Figure 1 A Hawaiian Airlines flight where the fuselage failed from repeated stresses. | Figure 2 A cracked cusp clearly associated with the wear facet. | |
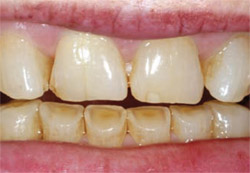 |  | |
| Figure 3 Accelerated tooth wear from bruxism. | Figure 4 A maxillary flat plane splint with anterior disclusion built in. | |
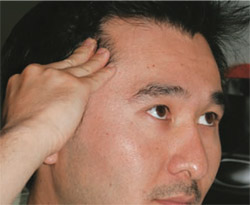 |  | |
| Figure 5 Patient palpating his temporalis (and then masseter) while contracting with posterior teeth in contact. The patient was then instructed to contact only on the incisors in protrusion to demonstrate the difference in contractile force. | Figure 6 A nut placed in a nutcracker in the area that gives the greatest mechanical advantage (ie, generates the greatest force). | |
 |  | |
| Figure 7 A nut placed in a nutcracker in the area that gives the least mechanical advantage (ie, generates the least force). | Figure 8 Crayons that are worn on one end to demonstrate to the patient wear patterns of bruxism. | |
| About the Authors | ||
 Greg Vigoren, DDS Greg Vigoren, DDSPrivate Practice Newport Beach, California | ||
 Edward A. McLaren, DDS Edward A. McLaren, DDSAdjunct Associate Professor Director UCLA Center for Esthetic Dentistry and Founder and Director of UCLA Master Dental Ceramist Program UCLA School of Dentistry Private Practice limited to Prosthodontics and Esthetic Dentistry Los Angeles, California | ||