Atraumatic Laser Extraction for Predictable Anterior Esthetics
Stewart Rosenberg, DDS
Maintaining the gingival and osseous architecture are the keys to outstanding esthetic results, especially in the anterior. Extracting hopeless teeth in the “esthetic zone” can be a very challenging task but losing buccal bone and the accompanying compromise in the gingival form can turn a case into a cosmetic nightmare. This case will demonstrate how an anterior tooth can be gently removed with the use of a Er,Cr:YSGG laser.
CASE PRESENTATION
A 43-year-old man presented with a fistula at the apex of his upper left central incisor in addition to extreme mobility of the tooth. The endodontically treated tooth had a 20-year-old post retaining a porcelain-fused-to-metal crown that, although esthetically poor, was serviceable to the patient up until that time.
Radiographic examination revealed a horizontal fracture through the root as a result of the poor angulation of the post (Figure 1). It was explained to the patient that the tooth was hopeless and ideal treatment would be to extract the tooth and place an implant-retained crown. Because of the periapical infection, it was decided that immediate placement of the implant was contraindicated.
The patient accepted the recommended treatment of extraction, bone graft, and provisional partial denture followed by an immediately loaded implant once healing had properly occurred.
The key to a good esthetic result was maintenance of the buccal plate and gingival architecture from pre-extraction though implant and crown placement. The tooth had fractured about 8 mm above the gingival margin, making the extraction potentially difficult and jeopardizing the buccal plate if conventional methods were to be employed.
For several years the author has been using a Waterlase MD Er,Cr:YSGG laser (Biolase Technology, Inc, Irvine, CA) to assist in all extractions to protect the bone and soft tissue and remove teeth as atraumatically as possible. Results of the technique described here have been very predictable and successful.1-5
To make certain the buccal tissue and interproximal papilla remained intact, a G4 tip at 0.5 W, 11% air, and 3% water was used to carefully sever the periodontal ligament from the coronal portion of the tooth. The fractured portion was then easily removed. Inspection revealed not just a horizontal but also an oblique fracture of the root.
Removing the remaining fractured root was accomplished atraumatically by using the laser to completely loosen the attachment almost to the apex so that the tooth could be removed without any chance of further fracture or loss of bone. A 14-mm, Z6 tip was used at 3 W, 40% air, and 20% water to trough completely around the tooth (Figure 2) until the root tip was so loose that it could be removed with a gentle wiggle of a root pick (Figure 3). The integrity of the socket and surrounding tissues was maintained (Figure 4).
The laser tip was then inserted into the socket and laser energy was used to aid in the removal of granulation tissue and decontamination of the socket from the infection present. To best prepare the socket for an implant, a freeze-dried graft material was placed in the socket followed by a barrier membrane (Figure 5).
The provisional removable partial denture was inserted and checked for fit and occlusion. The socket shows remarkable healing (Figure 6), which is typical when we use the laser in assisting or totally performing surgical procedures. The Er,Cr: YSGG laser appears to enhance healing and reduce postoperative sequelae dramatically. Our patient reported no postoperative pain, took no analgesics, and had no swelling following the procedure.
At 3 months postoperatively, the osteotomy was performed by our implantologist for an immediately loaded implant. A straight handpiece and a T4 tip was used at 0.5 W, 11% air, and 3% water to make an incision through the soft tissue down to the underlying bone. The soft tissue was then removed with a spoon-shaped curette, the osteotomy was performed conventionally, and an implant was placed. The integrity of the tissue is maintained in a more conservative manner by using the laser rather than a flap incision or punch technique.
Three months later, the temporary abutment and crown were removed, an impression post was placed, and final impressions were taken for the permanent crown. Two weeks later, the permanent abutment and crown were inserted, yielding an excellent esthetic and functional result (Figure 7).
CONCLUSION
By using the Er,Cr:YSGG laser to assist in this difficult extraction, the author was able to maintain the buccal plate of the bone and keep the gingival tissue intact for an excellent esthetic result. The laser has enabled the author to routinely perform surgical procedures far more atraumatically, more precisely, and more predictably than ever before. The author’s patients have experienced less pain, less trauma, and less healing time and consequently case acceptance has increased.
References
1. Wang X, Zhang G, Matsumoto K. In vivo study of the healing processes that occur in the jaws of rabbits following perforation by an Er,Cr:YSGG laser. Lasers Med Sci. 2005;20(1):21-27.2. Lee CY. Procurement of autogenous bone from ramus with simultaneous mandibular third-molar removal for bone grafting using the ErCr:YSGG laser: a preliminary report. J Oral Implantol. 2005;31(1):32-38.
3. Miller RJ. Treatment of the contaminated implant surface using the Er,Cr:YSGG laser. Implant Dent. 2004;13(2):165-170.
4. Mark I, Op’t Hof J. The Er,Cr:YSGG hydrokinetic laser system for dentistry—clinical applications. SADJ. 2002;57(8):323-326.
5. Kimura Y, Yu DG, Fujita A, et al. Effects of erbium,chromium:YSGG laser irradiation on canine mandibular bone. J Periodontol. 2001;72(9): 1178-1182.
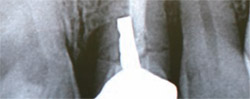 | 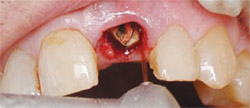 | |
| Figure 1 Radiographic examination revealed a horizontal fracture through the root as a result of the poor angulation of the post. | Figure 2 A 14-mm, Z6 tip was used at 3 W, 40% air, and 20% water to trough completely around the tooth. | |
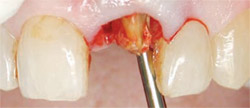 | 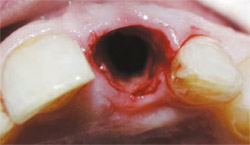 | |
| Figure 3 Once the root tip was loose it could be removed with a gentle wiggle of a root pick. | Figure 4 The integrity of the socket and surrounding tissues was maintained. | |
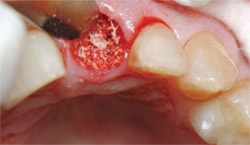 | 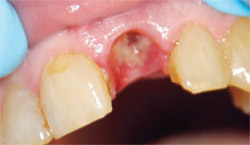 | |
| Figure 5 A freeze-dried graft material was placed in the socket followed by a barrier membrane. | Figure 6 The socket showed remarkable healing. | |
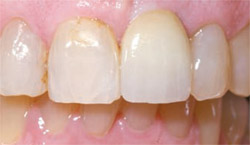 | ||
| Figure 7 The permanent abutment and crown were inserted, yielding an excellent esthetic and functional result. | ||
| About the Author | ||
 Stewart Rosenberg, DDS Stewart Rosenberg, DDSStewart Rosenberg, DDS Private Practice Laurel, MD | ||



