Simultaneous Placement of Minimally Invasive Porcelain Veneers: Predictable, Durable Success
Howard E. Strassler, DMD; Daniel Hoffacker
Our patients are enamored with the concept that they can change the appearance of their smile. While for many patients tooth whitening with bleaching and whitening toothpastes is all that is necessary, there are those who want and need a restorative approach to change their smiles. Esthetic dentistry is elective dentistry; patients seek out the dentist for advice on a condition that they diagnose themselves—dissatisfaction with the appearance of their teeth and smile. It might be small spaces between the teeth, chipped teeth, slightly rotated teeth, minor or major tooth discolorations, or teeth that are unesthetically shaped or undersized. For these patients, whitening alone is not enough. Also, these patients are better informed than in the past through advertisements in local newspapers, articles in magazines, and television shows on total or extreme makeovers that include restorative dentistry to help the person change their appearance. In many cases, changing someone’s smile involves the placement of porcelain veneers. Today dentists have choices on which porcelain veneer technique they choose to use.
More than 2 decades ago, the concept of bonding thin porcelain facings to natural tooth structure was introduced to dentistry.1-3 This and other research greatly advanced esthetic dentistry by providing a treatment modality that not only used the same restorative material—porcelain—that was accepted for its optimal esthetics and durability, but offered an alternative to tooth preparations that stripped all of the enamel from the tooth crown, leaving only dentin. Porcelain veneers were the ultimate conservative esthetic treatment because almost all of the enamel was left intact before the veneer was placed. Unfortunately, the concepts of conservative or “no preparation” veneers have morphed over the years into the philosophy of some that to provide for esthetic veneers, the teeth required a reverse three-quarter crown preparation with a preparation depth of at least 1 mm. Crispin has investigated the thickness of enamel in anterior teeth.4 Based on his findings, veneer preparations that have been recommended for some pressed porcelains would leave the gingival third of the preparation primarily into dentin. Friedman did a 15-year retrospective study on porcelain veneers.5 He reported that adhesive fractures of veneer bonded to enamel was rarely observed but that most failures related to cervical fracture and microleakage occurred when dentin was the bonded tooth substrate. Research on the durability of dentin bonding has demonstrated a bond strength drop-off after 2 years.6,7 Friedman further stated that veneer preparations should remain in enamel only. He reported that if a veneer lengthens a tooth or closes a diastema with the porcelain extending 1 mm to 1.5 mm or more but is not supported by natural tooth structure, there is an increased risk for veneer fracture. When pressed porcelain was first introduced for use as porcelain veneers, preparation on the facial surface with incisal reduction was required because of the limitations in the physical properties and the fabrication method of the pressed ceramic being used.8,9 Based on Friedman’s observations, these pressed ceramic veneers will be at risk.
The evidence supports the concept of “no preparation” or slight tooth modification for porcelain veneers using high-strength physical properties matched to the tooth structure as well as bonding composite resin cement to porcelain veneers fabricated with fired and stacked Cerinate® Porcelain (Den-Mat, Santa Maria, CA). Successful clinical trials with this porcelain have been reported;10-13 this porcelain has unique physical properties that contribute to that success.14,15
Recently, these 0.3-mm to 0.5-mm thick (contact-lens thin) veneers were introduced as LUMINEERS™ (Den-Mat) fabricated with Cerinate Porcelain that are placed over existing teeth without requiring any removal of tooth structure, although in some cases there is the need for minor tooth modification because of tooth misalignments or malpositions or for the placement of mandibular veneers and/or minor incisal reshaping and reduction to accommodate occlusion.16 The thinness of these porcelain veneers eliminates the associated pain, discomfort, and local anesthetic injections required to prepare teeth for an esthetic transformation with porcelain veneers. This translates into the elimination of postoperative pain after preparation and the requirement of fabricating provisional veneers between visits. In this author’s experience, many patients are resistant to the idea of having porcelain veneers because of what they have read or seen in the media. In lay publications and some of the television makeover shows, the clinician performing the treatment demonstrates the administration of local anesthesia, either intravenous sedation or nitrous oxide analgesia, combined with highly invasive tooth preparations before fabricating the veneers. In some cases the patients are shown as being in pain during the process. The author has found that for those clinical situations where “no preparation,” minimally invasive porcelain veneers are indicated, providing the patient with photo-graphic examples of these veneers for clinical situations that are similar to their own leads to very high patient acceptance. In fact, in a recent survey of dentists asked about tooth preparations for veneers, the dentists opted for minimally invasive tooth preparations.17
Clinical Indications for Minimally Invasive Porcelain Veneers
Most esthetic dentistry is elective. For this reason it is the patient who provides the primary indication. It is the patient’s wish and self-perceived need to change the appearance of their smile. Although LUMINEERS primarily refer to the contact-lens thin veneer with a thickness of 0.3 mm to 0.5 mm, in reality they are any porcelain veneer made with either stacked and fired or pressed Cerinate Porcelain. A patient can be treatment planned for the use of this high-strength durable porcelain even in those clinical situation that require more extensive tooth reductions or thicker porcelain. An example of the need for a more extensive tooth preparation includes misaligned anterior teeth. In this author’s experience of over 20 years, most cases can be treated using thin, minimally invasive veneers (Table 1). These cases include changing basic tooth shades, masking tooth discolorations (tetracycline staining, endodontic staining, and fluorosis), and overlaying existing composite resin restorations combined with restoring interproximal, cervical, and incisal edge caries with composite resin to ensure an esthetic restoration. These types of veneers also can be used to close diastemas between anterior teeth; reshape undersized teeth and peg-shaped incisors; reshape tooth contours and incisal edges of anterior teeth; restore worn, chipped, and/or fractured teeth; and correct misalignments of anterior teeth. Other successful uses of porcelain veneers are to change color and repair existing porcelain and porcelain-fused-to-metal restorations through resurfacing.16,18
Case Report
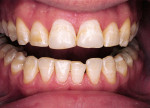
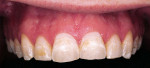
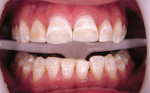
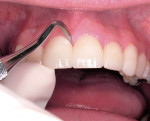
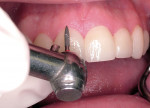
A 26-year-old dental student presented with fluorosis staining of his maxillary anterior teeth and premolars, with overcontoured composite resin on the facial surface of the maxillary central incisors that had been placed several years earlier to mask brown discolorations (Figure 1). The patient’s chief esthetic complaint was he desired a more even and whiter color for his teeth before he graduated from dental school. After discussing treatment alternatives including bleaching, direct composite resin bonding, and minimally invasive porcelain veneers, the patient decided to choose the most conservative treatment choice with the best esthetic result. It was decided that there was only a need to place veneers from the maxillary right first premolar to the left first premolar (teeth Nos. 5 through 12). The only tooth reshaping was removing the composite resin on the middle and incisor thirds of the maxillary central incisors and a slight modification of the mesial line angles of both central incisors using a medium-grit, flame-shaped diamond (Figure 2).
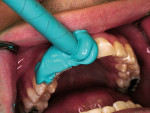
An impression was made using a bite impression technique with a fast-setting, monophase (regular body) viscosity, vinylpolysiloxane impression material in a 3-in-1 tray (Centrix, Shelton, CT). The monophase impression material was directly syringed onto the teeth with the automixing tip (Figure 3). This impression technique provides the laboratory with an accurate impression of the teeth to be restored, the opposing arch, and bite registration. This technique eliminates the guesswork for the laboratory and guarantees accurate articulation of casts.19 The laboratory authorization was completed describing the purpose of the veneers—the shade desired as well as the length and surface texture for the facial surface of the veneer—and the impression was sent to the laboratory for fabrication of the restorations. Because the teeth were minimally reshaped, there was no need for provisional restorations between visits.
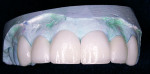
When the veneers were returned by the laboratory (Figure 4), the teeth and surfaces to be bonded were cleaned with a water-pumice paste using a disposable prophylaxis angle. The interproximal surfaces were cleaned using a safe-side� handled diamond tip. The teeth were then moistened with water and the veneers were tried on to verify fit and esthetic shape. The patient was shown the veneers and approved the esthetic appearance of the restorations.
Surface Treatments
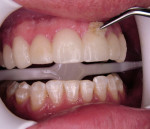
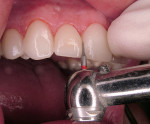
The internal surfaces of all of the porcelain veneers were etched in the laboratory with hydrofluoric acid. At chairside, the etched surfaces of the porcelain had an acidic porcelain conditioner painted on with a disposable brush for 20 seconds. The surface was then rinsed with water and dried. The use of an acidic conditioner chemically activates and enhances the chemical treatment of the porcelain with an organo-silane (porcelain chemical coupling agent). The conditioned surface was then painted with a silane ceramic primer for 30 seconds and then dried from the surface. A resin adhesive was then applied to the internal porcelain surfaces. The dental assistant then placed the automixed resin cement (Ultra-Bond®, Den-Mat) into the veneers. While the veneers were being prepared for bonding, the teeth were etched for 15 seconds with a 25% semi-gel phosphoric acid etchant. The teeth were rinsed for 10 seconds with an air-water spray and then dried, leaving an etched frosty appearance in the enamel (Figure 5). A resin adhesive was applied with a Benda® Brush (Centrix, Shelton, CT) to the etched enamel surfaces of all 8 teeth (Figure 6). The teeth and veneers were now ready for a simultaneous veneer placement technique.
Porcelain Veneer Placement
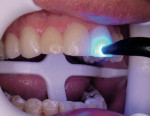
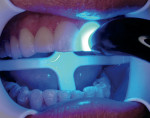
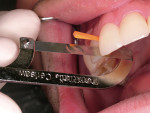
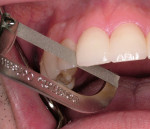
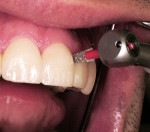
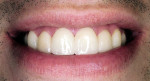
The 8 veneers were bonded to place using a multiple placement, no-matrix technique that has been described by Putter and associates.20,21 This technique has greatly simplified the placement of porcelain veneers. In other techniques, veneers are bonded to place either 1 or 2 at a time. When this is done, the composite resin cement must be finished at the proximal margins before the seating of adjacent veneers. This can be problematic. In some cases, finishing the interproximal margins of porcelain veneers can cause gingival hemorrhage that can interfere with subsequent continued bonding of the adjacent veneers. In this case the veneers were placed simultaneously on the teeth. As each veneer was placed, the back end of the Benda-Brush was used to fully seat the veneers. Because of the viscosity of the resin cement, this seating of the veneers was repeated several times to be certain the veneers were not lifting up on the teeth. When it was verified that all the veneers were fully seated without any matrix strips, each veneer was tack-cured for 1 second using a plasma arc curing light with a 2-mm tacking tip in the middle of the facial surface of each veneer (Figure 7). Using only 1 second of curing time allows for additional easy clean-up of excess resin cement from around the veneer margins, and then floss can be gently passed between the proximal surfaces to allow for easy interproximal clean-up of excess cement. Excess resin cement was removed using a sponge wetted with the resin adhesive, Tenure S (Figure 8). This technique assures that the resin cement will be at the margins of the veneers. The veneers were then finally cured for 5 seconds with a 9-mm curing tip (Figure 9). Finishing and polishing was accomplished using the accessories in the LUMINEERS Finishing Kit (Den-Mat), which includes a CeriSaw, CeriSander, Shure 349 orthodontic instrument, finishing diamonds and burs, and a diamond polishing paste. For this case, the slight excess of polymerized resin cement at the margins and on the porcelain surface was removed using the orthodontic instrument (Figure 10), and finishing and polishing of the margins was accomplished with the finishing diamonds and burs (Figure 11). The interproximal contact areas were cleared of excess composite resin cement with a mosquito diamond (8392-016 Brasseler USA, Savannah, GA) (Figure 12). The contacts were then opened up for access using the CeriSaw intraoral dental saw (Figure 13). This saw uses extremely thin, 0.05-mm stainless steel sharp dental saw blades attached to a miniature hacksaw handle. By having the blades attached to the handle and with the placement of a gingival wedge, the saw was easily controlled, preventing the accidental cutting of gingival tissues.20 It is not necessary to open all contact areas at the placement appointment. The proximal contacts that are more difficult to access are more easily managed and opened up at the follow-up appointment. Tooth movement during function breaks the resin free and loosens tight contacts to allow for easier access at the next appointment. The contact areas were then finished using a handled ultrafine, safe-sided diamond strip (Figure 14). The removal of resin cement and slight recontouring of the interproxmal gingival surfaces was accomplished with a reciprocating handpiece (Profin®, Dentatus, New York, NY) with a thin, flat-bladed, safe-sided diamond Lamineer® tip (Dentatus) (Figure 15). Use of a thin diamond bur in the gingival interproximal areas with a high-speed handpiece is contraindicated because one can notch the veneers in these areas and leave an esthetically unsatisfactory restoration. The restorations were then polished using a disposable prophylaxis angle and cup with a diamond-impregnated polishing paste. When compared to the preoperative smile, the completed veneers provided for a highly esthetic result that met the patient’s expectations (Figure 16).
Discussion
The evidence concerning the need for tooth preparation before placing porcelain veneers supports the use of “no preparation” or minimally invasive porcelain veneers. When porcelain veneers were introduced as a treatment modality more than 20 years ago, there was a fear that a thin porcelain facing would fracture in function. This fear caused some clinicians to recommend routine tooth preparations of 0.5 mm to 1 mm without any evidence to support this view. These recommendations were not based on clinical trials at the time, but rather a concern that thin porcelain would fracture during placement and function or while the technician was fabricating the veneer. Nathanson described the interface and bond between porcelain-composite resin-enamel as strengthening the porcelain and eliminating the propagation of microcracks between the porcelain, composite resin, and enamel.22 Sorensen and coworkers evaluated porcelain durability.23 Their findings indicated that of the 4 systems tested, Cerinate porcelain with Ultra-Bond was the only porcelain that resisted microcracking after thermocycling. They also found that there was significantly less microleakage at the Cerinate/Ultra-Bond interface when compared to the other 3 systems tested. These findings parallel what has been observed in long-term clinical trials with fired, stacked porcelain.10-13 Nash stated that for those patients desiring minor tooth shade and appearance changes, he chose Cerinate Porcelain because he preferred to remove as little tooth structure as possible to accomplish the esthetic result desired.12 He further stated that so little enamel was removed that no temporization was necessary. Also, periodontal assessments comparing teeth restored with porcelain veneers with preparation to teeth restored with porcelain veneers with no preparation demonstrate no difference in periodontal health.24 Peumanns evaluated porcelain veneers at 5 years for gingival health and concluded that smooth finished margins were important to maintain gingival health.25 When porcelain veneers were still a new treatment modality, Jordan10 and Christensen11 reported clinical success with Cerinate Porcelain veneers placed with Ultra-Bond in early clinical trials. Other research supports minimally prepared teeth for veneers. Nordbo and associates reported that veneers without incisal overlap perform successfully.26
Long-term evaluation of minimally invasive porcelain veneers has demonstrated that this treatment modality is highly successful.27 This study evaluated porcelain veneers fabricated with Cerinate Porcelain and placed with Ultra-Bond for up to 20 years with a mean of 15.2 years. Of the teeth veneered, 78% would be considered to be minimally invasive porcelain veneers because there was either no preparation or only very slight tooth reshaping to accommodate misalignments and incisal edge discrepancies. Over the duration of the study, among the patients who were able to be recalled there was 100% retention of the Cerinate veneers with very little change in color. There were no veneers that were completely debonded over the course of the study. At the last recall, 94% of the veneers were clinically successful (157 of 167) with only 10 veneers needing replacement. Replacement was usually needed because of chipping or cracking on stress-bearing surfaces. These fractures were usually cohesive fractures within the porcelain.
Conclusion
Minimally invasive porcelain veneers are a clinically successful treatment modality to cosmetically restore teeth with unesthetic appearances. Clinical research has demonstrated that “no preparation” or slight tooth modifications before fabricating this type of veneer is an optimal conservative treatment technique. In this author’s experience, patients are requesting smile changes for tooth color, space closure, chipped and fractured tooth repair, tooth lengthening because of wear, minor tooth alignment, and reshaping. It has been demonstrated that with minimally invasive porcelain veneers these conditions can be easily treated in a conservative, tooth-saving approach.16 The clinician can provide these thin, contact lens-like veneers with no or little tooth removal and without the need for local anesthetic. The final results are well accepted by the patients being treated.
Disclosure
The author has performed funded research for and has received presentation honorariums from Den-Mat.
References
1. Simonsen RJ, Calamia JR. Tensile bond strength of etched porcelain. J Dent Res. 1983;62(Special Issue):297. Abstract 1154.
2. Calamia JR, Simonsen RJ. Effects of coupling agents on bond strength of etched porcelain. J Dent Res. 1984;63(Special Issue):179. Abstract 79.
3. Horn PH. Porcelain laminate veneers bonded to etched enamel. Dent Clin North Am. 1983;27:671-684.
4. Crispin BJ. Esthetic moieties: enamel thickness. J Esthet Dent. 1993;5:37.
5. Friedman MJ. A 15-year review of porcelain failure- a clinician’s observations. Compend Contin Educ Dent. 1996;19:625-638.
6. Meiers JC, Young D. Two-year composite/ dentin bond stability. Am J Dent. 2001;14: 141-144.
7. Hashimoto M, Ohno H, Kaga M, et al. In vivo degradation of resin-dentin bonds in humans over 1 to 3 years. J Dent Res.2000;79:1385-1391.
8. Strassler HE. Esthetic restoration of discolored teeth using porcelain laminate veneers. Compend Contin Dent Educ. 1998;19: 518-538.
9. Barnes DM Strassler HE. Veneers: a comparison of three techniques. Esthetic Dentistry Update. 1990;1:74-80.
10. Jordan RE, Suzuki M, Senda A. Clinical evaluation of porcelain laminate veneers: a four-year recall report. J Esthet Dent. 1989;1:126-132.
11. Christensen GJ, Christensen RP. Clinical observations of porcelain veneers: a three year report. 1991;3:174-179.
12. Nash RW. A 6-year follow-up on Cerinate porcelain veneers. Compend Contin Educ Dent. 1998;19:664-669.
13. Strassler HE, Weiner S. Long term evaluation of porcelain veneers. J Dent Res. (Special Issue) 2001;80(Special Issue):223. Abstract 194.
14. Chadwick TC, Ibsen RL. Properties of a new porcelain for veneers, inlays and crowns. J Dent Res. (Special Issue) 1989;68(Special Issue):956. Abstract 712.
15. Wassenaar P. The new porcelains-are they any better? Austral Prosthod J. 1990; 4(Supplement):19-25.
16. Strassler HE, Ibsen RL. Improving smiles without removing sensitive tooth structure. Contemporary Esthetics and Restorative Practice. 2005;9(3):54-61.
17. Heymann HO, Swift EJ Jr. Is tooth structure not sacred anymore? J Esthet Restor Dent. 2001;13:318-27.
18. Strassler HE. Aging patients/aging restorations: predictable crown and fixed partial denture repair. Contemporary Esthetics and Restorative Practice. 2002;6(11):20-32.
19. Cevhan JA, Johnson GH, Lepe X, et al. A clinical study comparing the three-dimensional accuracy of a working die generated from two dual-arch trays and a complete-arch custom tray. J Prosthet Dent. 2003;90:228-234.
20. Putter H, Strassler HE. An instrument for opening contact areas for interproximal finishing. J Esthet Dent. 1989;1:194-197.
21. Putter H, Ibsen RL. Simultaneous placement of multiple porcelain veneers. J Esthet Dent. 1990;2:67-69.
22. Nathanson D. Dental porcelain technology. In: Porcelain Laminate Veneers. Eds: Garber DA, Goldstein RE, Feinman RA. Quintessence Publishing, Chicago, Ill. 1988;24-35.
23. Sorensen JA, Kang SK, Avera SA. Microleakage of composite resin to various porcelain surface treatments. J Dent Res. 1990(Special Issue);69:359. Abstract 2008.
24. Yu X, Oulette D, Ibsen R. Periodontal evaluation of long-term pre vs non-prep porcelain veneer restorations. J Dent Res. 1998; 77(Special Issue):954. Abstract 2583.
25. Peumanns M. The influence of 5-year aged porcelain veneers on the marginal gingival tissues. In: The Clinical Performance of Veneer Restorations and Their Influence on the Periodontium. Leuven University Press, Belgium. 1997;71-78.
26. Nordbo H, Rygh-Thoresen H, Henaug T. Clinical performance of porcelain laminate veneers without incisal overlapping: 3 year results. J Dent. 1994;22:342-345.
27. Strassler HE. Long term clinical evaluation Cerinate etched porcelain veneers. J Dent Res. 2005;84(Special Issue A). Abstract 432.
About the Authors
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Daniel Hoffacker, Dental Student
Department of Endodontics, Prosthodontics and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland