The Value of the Diagnostic Wax-up
Walter Richardson, CDT, TE
The diagnostic wax-up is the method or process through which practitioners can fully visualize the true restorative needs of their patients. In fact, it is probably the greatest working tool of our profession. By gathering current information from the initial exam, the integration and assimilation process begins. In some ways the process is like assembling many pieces into a completed jigsaw puzzle, only the goal of the diagnostic wax-up is to develop a unique, complete treatment plan to benefit the patient’s dental health.
For the process to begin, records need to be collected. No matter how simple or complex the case may appear, it cannot be stressed enough how important it is to have all the information together. The diagnostic wax-up is a strategic session. In order to successfully work through the diagnostic process, the following records are necessary:
- Well-impressed models (two sets: archival and working)
- Face bow
- Centric relation (CR) bite
- Maximum intercuspation (MI) bite
- Protrusive bite
- X-rays—full mouth, panoramic, and cephalometric (cephalometric is useful for orthodontic wax-up)
- Periodontal probing chart
- Noted observations of temporomandibular joint (TMJ) status
- Noted observations of muscle examination
- Diagnostic photographs
The idea of gathering a complete set of records for a case may seem time-consuming, however, in the end it will not only save time, but cost for both the practice and the patient. If one of the puzzle pieces is missing or incomplete, the picture cannot be fully visualized. Patient records must be both comprehensive and accurate. For instance, well-impressed models need to reflect all anatomic information contained within the oral cavity, such as the vestibule, bone contour, frenums, full palate, retromolar pad, tuberosities, and details of all the teeth, as well as other unique characteristics such as tori. This information may be essential in deciding whether a bone graft will be necessary or whether orthodontics can correct an unstable occlusion. All pieces of the puzzle must be present so a correct determination can be made.
Also important to the complete picture is the face bow record. The face bow record establishes the relationship of the maxillary arch and dentition to the horizontal reference plane.
The centric relation (CR) bite record adds to the total picture. This bite record provides a true representation of where the teeth are in relation to where the condyles rotate when opening and closing without the condyles moving down the eminence. This record is essential because CR is of vital importance to the success of almost all restorative cases and thus should be the starting point. There are many ways to obtain the CR bite record, including—but not limited to—bimanual manipulation, anterior deprogrammers, leaf gauges, and central bearing points.
Another essential record is the maximum intercuspation bite, used to verify the termination of the slide from CR to MI. Also the ability to view the full dentition in MI allows one to determine whether tooth wear is occlusally generated or other factors have contributed to the worn dentition.
The final pieces needed to complete the picture are the diagnostic photographs: these are invaluable. Diagnostic photographs break down incrementally the various aspects that make up the patient’s current physical and esthetic design. While there are many views that can comprise a complete photographic record, the ones that are essential for diagnostic purposes are:
- Full-face smile—shows the relationship of the smile to the face
- Close-up smile—captures relationship of upper smile line to lower lip
- Close-up profile—shows the upper incisal edge position to inner vermillion border of lower lip
- Close-up high smile line—provides information on embrasures, symmetry of gingival heights, and margin placement
- Close-up “E” position—shows relationship of upper incisors to upper lip
- Close-up MI occlusion (retracted)—shows front to back progression
- Close-up rest position—shows display relationship of incisal plane of lower teeth to lower lip
- Smile with teeth apart (close-up)—displays the silhouette of upper and lower incisal plane
- Smile, head tipped down (close-up, shot from the tip of the nose)—shows the relationship of arch form to lower lip
Once all the records are taken and consolidated, the pieces of the puzzle are together, and the integration and assimilation process begins. Using the diagnostic waxing method, the visualization of a treatment begins to unfold. Various determinations can be made: Whether or not additive or subtractive equilibration is necessary, possibly a combination of the two; Whether the plane of occlusion is in need of correction so that the fundamentals of occlusion can be achieved; Whether there are sufficient stable centric stops both posterior and anterior for occlusal stability; Whether or not anterior guidance functions can be maximized or even obtained. These are only a few examples of observations to be analyzed. After the integration of data and analysis phase is complete, reducing or adding to the teeth on the mounted models with wax can begin. In effect, the technician is restoring the patient without touching the patient at all. These restorations on the diagnostic models are the trial run of the treatment plan: it is better to make changes in the treatment plan at this stage than with a hastily made decision at the chair. Upon completion, this diagnostic wax-up becomes the blueprint of the treatment plan.
Types of Diagnostic Wax-Ups
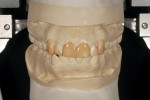
Generally, there are four types of diagnostic wax-ups commonly requested by restorative dentists: the basic diagnostic wax-up, the full contour wax-up, case presentation wax-up, and the orthodontic wax-up. The basic diagnostic wax-up (Figure 1) aids in developing an overall game plan for the restorative procedures. Minimal waxing is used and placed in deficient areas only. Models can be marked to depict necessary gingival crown lengthening. Wax can then be flowed down or up in those areas to provide a good visual of the improvement. Cusp tips can be added to improve centric stop areas, lingual contours added to improve anterior guidance functions, and incisal length added to achieve the desired length or position. Many times it is necessary to reduce areas with a handpiece and bur to eliminate areas that are detrimental to the overall goal of proper plane of occlusion, stable centric stops, and maximized anterior guidance function. The basic diagnostic wax-up is the tool of choice—along with the other study records—to communicate with the laboratory technician or laboratory assistant as to the direction the case will be developed. Of all the wax-ups, the basic diagnostic wax-up is the least costly in both time and money. However, it is the best tool for the visualization process.
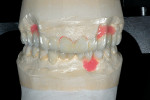
As the name implies, the full-contour wax-up (Figure 2) is used when improved esthetics and contours are included in the treatment plan. It incorporates the same visualization process as the basic wax-up but uses more wax. The full-contour wax-up is also used if missing teeth are involved and implant placement determinants are necessary. Teeth are reduced enough to allow the technician or laboratory assistant to establish proper tooth form and function. In many instances, this is the wax-up of choice for large rehabilitation cases. Judgment calls can be made during the analysis phase of the full-contour wax-up when it is determined that finer details of the current situation are of less value in the overall end result. Another advantage of the full-contour wax-up is the ability to create functionally correct provisionals for the patient.
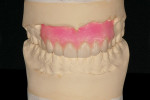
The case presentation wax-up (Figure 3) is generally requested to show the patient the end result of the personalized treatment plan: when done well, this wax-up is very impressive. In order to create this type of wax-up, the teeth are prepared on the model as they would be in the mouth. Then wax is built-up to proper contour and function. Often pink baseplate wax is added to the tissue areas to complete the visual effect for the patient. The case presentation wax-up is the least diagnostic of all wax-ups, unless done in tandem with a basic diagnostic wax-up. It is as the name implies—for case presentation and therefore patient acceptance. Although not common, provisionals can also be generated from this type of wax-up, provided the pink wax has not been added to the tissue areas. The case presentation wax-up requires much more skill and time from the technician or laboratory assistant, which is reflected in the cost.
The orthodontic wax-up (Figure 4) helps the practitioner visualize the possibilities available when repositioning is an integral part of obtaining optimal results on a given case. The orthodontic wax-up can help determine whether interproximal reduction will be necessary, and if so, how much. Reductions can be measured and documented throughout the diagnostic wax-up. Teeth can be placed in the proper position so that the fundamentals of occlusal stability can be achieved. Many times after going through this process, it is discovered that the restorative requirements are significantly reduced (ie, veneers versus crowns). The orthodontic wax-up is a great communication tool between restorative dentists and their orthodontist or orthodontic laboratory. The more information supplied in conjunction with the wax-up (x-rays, periodontal information, age of patient), the more accurate the orthodontic wax-up will be. Many times, removable orthodontic appliances can be made to accomplish tooth repositioning goals. It is through this type of wax-up that these types of determinations can be made. The orthodontic wax-up requires greater knowledge and skill, and a moderate amount of time is required to perform this wax-up and document the tooth dimension changes. The cost of this type of wax-up is often well worth the time and money spent.
American polymath Walter Russell was a world-renowned sculptor, painter, architect, scientist, philosopher, and world skating champion. While watching Dr. Russell sculpt a bust of George Washington, a student asked how he could sculpt with such speed, accuracy, and perfection. Dr. Russell replied, “I have already visualized the end result.”1 Through observing, analyzing, and planning, the visualization process was achieved—all that was left was to do it. So it is with the diagnostic wax-up process: it is the secret of many successful dentists and technicians worldwide.
Reference
1. Kulhawick J. The Russell Years at Swannanoa. https://www.philosophy.org/index.php?option=com_content&task=view&id=43&Itemid=76. Accessed June 23, 2009.
About the Author
Walter Richardson, CDT, TE
Bay View Dental Laboratory
Chesapeake, Virginia