The Three Pillars of Successful Implant Planning
The use of digital planning software facilitates precision, communication, and treatment acceptance
Melissa Seibert, DMD, MS
Implant treatment planning is rarely perfectly straightforward. For example, it would be uncommon for a clinician to treatment plan a partially edentulous space at the site of tooth No. 30 that was unaffected by a hard- or soft-tissue defect or a super-erupted opposing tooth. Oftentimes, clinicians have to consider the use of hard- and/or soft-tissue grafting procedures, limited or comprehensive orthodontics, treatment to manage a marginal ridge discrepancy, etc, during the treatment planning process. This can make treatment planning complex, particularly if multiple practitioners are involved. The three pillars of successful implant treatment planning are precision, communication, and case acceptance.
Precision
Both the surgeon and restorative dentist, which in some case may be the same person, should endeavor to ensure that an implant can actually be placed exactly where it was treatment planned to be placed. This goal may appear obvious, but clinicians commonly fail to achieve it. For example, a patient may present with an edentulous space at the site of tooth No. 8 for which an implant is treatment planned to be positioned far enough apically to achieve the optimal emergence profile. However, if the planning was imprecise or failed to account for the needs of the hard and soft tissues at the site, the implant can end up being placed too coronally, and not only will the optimal emergence profile not be achieved but also an idealized papilla will not form. In effect, it does not matter how well an implant's position and angulation are planned if there is not a means or capability to deliver precisely what was planned.
Communication
With implant treatment planning, as with all treatment planning, either a multidisciplinary approach or an interdisciplinary approach can be utilized. In a multidisciplinary approach, practitioners from multiple disciplines are involved but they are not intercommunicating during the process. Such implant planning may involve a surgeon and a restorative dentist, but if these providers have not discussed their individual goals for the case, they cannot ensure that they align with one another in the plan. This approach may result in implant planning that is purely restoratively driven or purely surgically driven, which can cause problems. For example, the restorative dentist may design a case and request that an implant be placed in a way that is surgically impractical. If the restorative dentist designs a screw-retained implant crown at the edentulous site of tooth No. 8, but to accomplish it, the implant may be positioned outside of the alveolar housing, then the surgeon has to make adjustments that may compromise the position of the final restoration. In the multidisciplinary approach, because the clinicians involved in implant treatment planning do not communicate with one another, they may be unaware of the variables that the other party needs to be optimized for implant placement to be successful.
The antidote to this scenario is interdisciplinary treatment planning. In interdisciplinary treatment planning, all of the parties involved thoroughly communicate with one another to develop a plan that is in alignment with each other's goals. The challenges involved in interdisciplinary treatment planning are that it is time-intensive and that it requires resources for the participants to effectively communicate. Effectively communicating may require setting up an in-person meeting with mounted stone models on an articulator or finding a HIPAA-compliant digital platform to send cone-beam computed tomography (CBCT) DICOM files back and forth, among other actions.
Case Acceptance
The final pillar of successful implant treatment planning, which cannot be overlooked, is achieving case acceptance. Challenging cases may require extensive treatment planning to accomplish, but ultimately, patients have to accept these treatment plans for them to move forward. This itself can pose a challenge because some of these cases are expensive and have lengthy timelines. There are many variables involved in achieving case acceptance. It is important that each patient fully understands his or her needs and how a proposed treatment plan will accomplish them. Engaging patients in the treatment planning process and incorporating their feedback can help in achieving acceptance, but this can be difficult to do when using analog methods.
The Advantages of Digital Implant Planning
Digital implant planning provides a means by which clinicians can optimize precision, facilitate interdisciplinary communication, and achieve case acceptance. When an implant is treatment planned using digital software that incorporates the patient's intraoral scans and CBCT images, the dental team can ensure that it is positioned and angulated with the upmost accuracy because both the models and the CBCT can be visualized in the process. Digital implant planning can also help to facilitate interdisciplinary communication because a digital workflow enables team members to send files back and forth to one another. In this manner, the restorative dentist can digitally design a case and place the prospective implant in a location that best accommodates his or her restorative plan. From there, the proposed plan can be sent to the surgeon for confirmation or modification. This workflow ensures that there is no guesswork by any dental team members regarding where the implant should be placed. Prior to digital planning software, dental team members may have had to make assumptions. Finally, digital implant planning may help in achieving case acceptance because patients can be further engaged in the treatment planning process and are able to visualize their needs. When patients can be present for the digital design process, their input can be provided in real time rather than when their wax-up comes back from the laboratory. This helps them to feel that they have agency in the design process and that their opinions are being heard.
Case Report
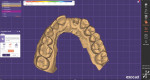
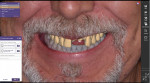
A 50-year-old male patient was referred to the dental clinic for the treatment of a fractured left lateral incisor (tooth No. 10), which had been previously treated, and an edentulous space at the site of tooth No. 9 (Figure 1). The patient, who had been missing tooth No. 9 for multiple years due to trauma, originally had a crown on tooth No. 10 with a pontic cantilevered off of it to replace tooth No. 9. As a result of the fracture, it was determined that tooth No. 10 was non-restorable and required extraction. The patient requested implants at the sites of teeth Nos. 9 and 10. In this case, digital treatment planning software (DentalCAD, exocad) and implant planning software (exoplan, exocad) were utilized to accomplish precision, facilitate communication, and achieve case acceptance.
Acquiring Records
The first step in this case involved acquiring high-resolution patient portrait photographs with a DSLR camera (EOS 80D, Canon), taking full-arch digital impressions/scans (Primescan®, Dentsply Sirona), and performing a full-arch maxillary CBCT scan (Planmeca ProMax 3D®, Planmeca). Next, the digital impression scans were converted into a stereolithography (STL) file and uploaded into the treatment planning software. STL is a file format used to transmit the geometric makeup of a 3D design.1 STL files can also be referred to as standard tessellation language files.2 A triangle is to an STL file what a pixel is to a PNG or JPEG file. A JPEG or PNG file is used to store an image and is composed of thousands of small pixels. Likewise, an STL file is used to store a 3D design and is composed of thousands of small triangles.
Smile Design
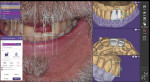
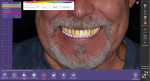
In the treatment planning software, the two-dimensional patient portrait photograph was overlayed over the scan of the patient's dentition (Figure 2). Incorporating a patient portrait into the digital design process provides the clinician with critical information about the patient's smile and how the proposed dentition should fit into the lips (Figure 3 and Figure 4). Historically, one challenge associated with designing an esthetic case that was mounted on an articulator was designing the edges of the maxillary incisors so that they were consonant with the curvature of the lower lip.3 This could be problematic because clinicians had to predict the position of the lips relative to the mounted stone models. The lips provide information that is essential to smile design. Ideally, 2 to 4 mm of the central incisors should be displayed when the patient is in repose; however, less will show as patients age or if they receive lip filler injections.4,5
An additional advantage of the smile design software used in this case, or any other digital smile design module that is lifelike, is that it may facilitate better communication with patients and improve the likelihood of case acceptance. With digital design, the practitioner and patient can sit together and review the patient's existing smile as well as what a proposed smile will look like in the patient's face. Patients can point things out on the screen and show practitioners what they may or may not like about their smile or a proposed smile design. This can facilitate a process of "co-diagnosis" in which the patient can become a partner in his or her own health and the practitioner and patient can arrive at conclusions together. Although there are other means of accomplishing this goal, the use of digital treatment planning software can really help to engage patients and secure their buy-in.
When involving patients in digital treatment planning, they can be present while clinicians are designing their smiles, or they can return when the designs are complete to provide feedback and give final approval prior to moving forward with the workflow. If a laboratory technician is the one designing a patient's smile, the patient can still be included in the process when the practitioner reviews the design and request any changes prior to ultimately approving it. Allowing patients to be present during the design process can be beneficial because it can make them feel like they are more intricately involved and have more agency in their treatment plans. It also allows them to communicate how they would like the design to be modified earlier on in the treatment planning process. Furthermore, when an analog treatment planning process is used and modifications are needed, clinicians have to return the case back to the laboratory by mail, and the time required for the design process is significantly extended. But with digital treatment planning, patients can provide feedback in real time, and whoever is designing the case can quickly make any necessary modifications to the design.
Implant Planning
In this case, it needed to be determined if two implants could be placed in the available space or if it would only accommodate one. One of the challenges of implant planning in the esthetic zone is obtaining a suitable peri-implant papilla.6 Papilla fill is influenced by the vertical distance between the interproximal contact and the alveolar crest and the horizontal distance between the adjacent structures. Generally, implants should be placed 1.5 mm to 2 mm from adjacent teeth and 3 mm to 4 mm from adjacent implants.7-9 This distance is critical because clinical trials have demonstrated that there is a lateral element to bone loss around implants. In Tarnow and Cho's classic study, adjacent implants displayed a lateral bone loss of 1.34 mm from the medial implant shoulder and 1.40 mm from the distal implant shoulder.9 The data indicated that crestal bone loss was mitigated when implants were appropriately placed far enough from one another.
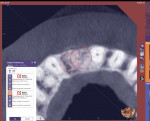
A clinician can quickly determine if enough horizontal space is available for an implant by calculating the horizontal width intraorally, on a cast, or by using CBCT software or digital implant planning software. Arguably, utilizing CBCT software or digital implant planning software is more accurate because it permits visualization of the roots. In this case, different permutations of implant widths and positions were attempted at site Nos. 9 and 10 in the pre-planning module to determine if two implants could be reasonably accommodated, but ultimately, there was inadequate horizontal space. In the software used, proposed implants turn red to indicate a lack of space, which helped to facilitate patient communication and case acceptance (Figure 5). Although the patient presented with the hopes of receiving two implants, the software functioned as a tool to explain to the patient why that was not a possibility. Alternatively, the edentulous site was treatment planned for an implant-supported restoration at the site of tooth No. 9 with a pontic at site No. 10 that would be cantilevered off of No. 9.
The crown and pontic for site Nos. 9 and 10 were designed using the CAD software, and once the patient was satisfied with the design, it was carried over into the implant planning software for implant planning. A screw-retained implant crown was chosen because it would permit easier retrievability if necessary.10
Hard-Tissue Grafting
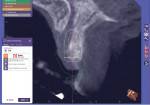
In the implant planning software, it was determined that if the implant were to be placed in the most ideal position, about 25% of it would be positioned in the incisive canal (Figure 6). This presented a challenge because it would also be ideal to have the implant entirely surrounded by hard tissue. It is not uncommon for this situation to be encountered when the maxillary arch is devoid of an anterior incisor for an extended period of time. The size of the incisive canal has been shown to increase with partial edentulism and ridge atrophy.11
To develop the site for implant placement, treatment to remove the contents of the canal and fill it with allograft was proposed to the patient. Magennis and colleagues demonstrated that patients who have their nasopalatine nerve sectioned will experience immediate revascularization and eventually achieve reinnervation of the anterior palate due to additional supply from the greater palatine nerve.12 Furthermore, Scher, Rosenquist, and Penarrocha have all demonstrated that the contents of the incisive canal can be successfully removed and the space grafted without patient reports of sensory disturbance or subsequent implant failure.13-15 Using the implant planning software, the patient in this case was shown the proposed implant placement and how it would encroach on the incisive canal. By providing visuals, a thorough informed consent conversation was facilitated, and the patient agreed to treatment. Ultimately, a portion of the contents of his nasopalatine canal was obliterated, and the space was filled with an allograft material.
Implant Placement
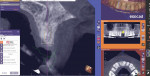
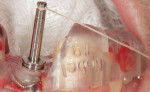
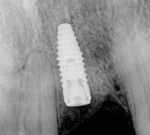
Once the patient had healed and the site was ready for implant placement, a new CBCT scan was acquired because the bony architecture of the site had changed. The digital design was then aligned with the CBCT scan once more (Figure 7) and a guide was fabricated (Figure 8). An implant (NobelReplace® CC, Nobel Biocare) was placed at site No. 9 using a fully guided surgical approach (Figure 9). An immediate provisional was not placed at the time of implant placement because an insertion torque of 35 Ncm or greater was not achieved.16,17 If adequate primary stability had been achieved, a provisional restoration could have been delivered, without the need for adjustment, at the time of placement of the implant. A postoperative radiograph confirmed that the implant had been placed in the most ideal position possible (Figure 10), which was critical because the patient's peripatetic lifestyle as a veteran precluded interdisciplinary treatment planning with the restorative dentist who would complete the case.
Conclusion
Precision, communication, and case acceptance are critical variables for success in implant treatment planning. Once case acceptance has been achieved, leveraging digital design software and following a guided surgical approach to placement can help to facilitate an idealized outcome.
About the Author
Melissa Seibert, DMD, MS
Creator and Host
Dental Digest Podcast
US Air Force Dentist
Deputy AEGD Program Director
Langley Air Force Base
Hampton, Virginia
Clinical Instructor
Creighton University
School of Dentistry
Omaha, Nebraska
References
1. Kamio T, Suzuki M, Asaumi R, Kawai T. DICOM segmentation and STL creation for 3D printing: a process and software package comparison for osseous anatomy. 3D Print Med. 2020;6:17.
2. Brünler R, Hausmann R, von Münchow M, et al. Design of complexly graded structures inside three-dimensional surface models by assigning volumetric structures. J Healthc Eng. 2019;2019:6074272.
3. Manjula WS, Sukumar MR, Kishorekumar S, et al. Smile: a review. J Pharm Bioallied Sci. 2015;7(Suppl 1):S271-S275.
4. Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning. Part I. Am J Orthod Dentofacial Orthop. 1993;103(4):299-312.
5. Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning. Part II. Am J Orthod Dentofacial Orthop. 1993;103(5):395-411.
6. Pradeep AR, Karthikeyan BV. Peri-implant papilla reconstruction: realities and limitations. J Periodontol. 2006;77(3):534-544.
7. Van Oosterwyck H, Duyck J, Vander Sloten J, et al. The influence of bone mechanical properties and implant fixation upon bone loading around oral implants. Clin Oral Implants Res.1998;9(6):407-418.
8. Esposito M, Ekestubbe A, Gröndahl K. Radiological evaluation of marginal bone loss at tooth surfaces facing single Brånemark implants. Clin Oral Implants Res. 1993;4(3):151-157.
9. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
10. Assaf M, Gharbyeh AZA. Screw-retained crown restorations of single implants: a step-by-step clinical guide. Eur J Dent. 2014;8(4):563-570.
11. Mardinger O, Namani-Sadan N, Chaushu G, Schwartz-Arad D. Morphologic changes of the nasopalatine canal related to dental implantation: a radiologic study in different degrees of absorbed maxillae. J Periodontol. 2008;79(9):1659-1662.
12. Magennis P. Sensory morbidity after palatal flap surgery-fact or fiction? J Ir Dent Assoc. 1990;36(2):60-61.
13. Rosenquist JB, Nyström E. Occlusion of the incisal canal with bone chips. A procedure to facilitate insertion of implants in the anterior maxilla. Int J Oral Maxillofac Surg. 1992;21(4):210-211.
14. Peñarrocha M, Carrillo C, Uribe R, García B. The nasopalatine canal as an anatomic buttress for implant placement in the severely atrophic maxilla: a pilot study. Int J Oral Maxillofac Implants. 2009;24(5):936-942.
15. Scher EL. Use of the incisive canal as a recipient site for root form implants: preliminary clinical reports. Implant Dent. 1994;3(1):38-41.
16. Bhekare A, Elghannam M, Somji SH, et al. Case selection criteria for predictable immediate implant placement and immediate provisionalization. J Oral Biol. 2018;5(1):6.
17. Schwartz-Arad D, Chaushu G. Placement of implants into fresh extraction sites: 4 to 7 years retrospective evaluation of 95 immediate implants. J Periodontol. 1997;68(11):1110-1116.
Disclaimer: the views expressed in this article are those of the author or product manufacturers and do not reflect the official views or policy of the US Department of the Air Force, the US Department of Defense, or the US Government. No federal endorsement of a manufacturer is intended.