Selecting a Dental Light Curing Unit
Essential properties and considerations to ensure restorative success and avoid complications
Richard Bengt Price, BDS, DDS, MS, PhD | Braden Sullivan
Most dental offices use dental light curing units (LCUs) every day to photopolymerize (ie, harden) materials such as bonding agents, composites, cements, and sealants.1-5 Some LCUs can even help clinicians visualize cracks in teeth and detect the presence of resins. Consequently, LCUs have become indispensable to the practice of dentistry.
The Basics
LCUs with halogen light bulbs have been used in dentistry for more than 50 years; however, the halogen bulb has a short lifespan (50 to 100 hours), is inefficient, and produces a significant amount of heat.1 To provide a faster and deeper cure, plasma arc LCUs were developed, but these devices are expensive, large, and also produce a considerable amount of heat. Therefore, most LCUs now use light emitting diodes (LEDs). These LCUs are small, efficient, and do not require bandpass filters. They can also be battery operated, and LEDs last for thousands of hours, which is significantly longer than halogen bulbs.6-8 Figure 1 illustrates some of the wide range of smaller and more ergonomic LED LCUs available for dentists to choose from.
Traditionally, dentists have focused on the irradiance, curing speed, and cost of LCUs.9 This article examines some of the other properties of LCUs to highlight the unseen value of using a quality device for dental procedures. A quality LCU has a relatively low one-time cost when compared with other dental equipment, but it must be correctly used and maintained to avoid unwanted negative impacts on a practice.
Light-cure dental resins must receive sufficient light energy delivered in the correct wavelengths to fully photopolymerize.1,3 This can prevent issues such as staining, leakage, pain, fracture, low bond strengths, loss of the restoration, and color changes1,2,5,10,11 as well as reduce the leaching of unwanted chemicals into the oral cavity.1,3,12,13 This minimizes the need for repairs or replacements, saving clinicians chair time and money in the long run. Properly cured dental materials also provide more durable and esthetically pleasing restorations, which improves patient satisfaction and increases the likelihood of return visits and referrals.
Most dental manufacturers14-17 recommend exposing resin-based composites to a minimum irradiance of 500 to 700 mW/cm2 for 20 seconds, thus delivering 10 to 14 J/cm2 to the material. In the authors' opinion, the ideal curing light should provide approximately 1,200 to 1,500 mW/cm2 over a broad spectrum of blue light (400 to 500 nm), have a long battery life, have an ergonomic shape, and be durable enough to withstand frequent use. For example, if such an LCU was used for 10 seconds, it would deliver 12 to 15 J/cm2. This is slightly more than the minimum amount of energy recommended by some manufacturers but less than the minimum amount (eg, 20 to 40 J/cm2) recommended by others for some of their darker or more opaque dentin shades.18,19 Therefore, it is important to follow the manufacturer's instructions for each material and adjust the exposure time accordingly. There are many popular LCUs that meet these criteria (eg, Elipar™ DeepCure-S, 3M; SmartLite® Pro, Dentsply Sirona; Valo™ Grand and Valo™ X, Ultradent; Bluephase® G4, Ivoclar) (Figure 2). When selecting a curing light, it's important to use the correct terminology, which includes the following:
• Radiant flux. This describes the power from the LCU in watts.
• Energy. This equals power × time and is measured in joules.
• Irradiance. This is the light that the resin receives in mW/cm2.
• Radiant exitance. This is a measure of power/light tip area and is the same as the irradiance measured at the light tip (mW/cm2).
• Radiant exposure. This equals irradiance × time and is measured in J/cm2.
• Emission spectrum. These are the wavelengths of light from the curing light in nanometers (nm).
Manufacturers' advertising brochures and some publications often use terms such as intensity, strength, power density, or brightness, but these are imprecise and should be avoided.
Light Guide Size and Shape
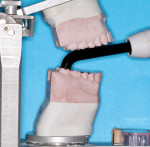
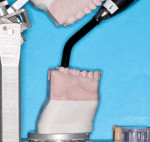
LCUs use one of two methods to aim the light from the source to the target: either light guides that are comprised of fiber-optic bundles or the LED is at the light tip. The fiber-optic bundles consist of hundreds of individual glass fibers that have been packed closely together to enable the light to travel from its source in the body of the LCU to the end of the light tip. These light guides come in a variety of fixed-diameter sizes and shapes. They are brand-dependent, fragile, and easily chipped, and they can be costly to replace. Furthermore, the size and shape of the light guide affects the LCU's ability to access all areas in the mouth.3,5,20-23 The LCU shown in Figure 3 has a low-profile light guide that permits better access to the molar teeth than the LCU shown in Figure 4. If the LCU shown in Figure 4 is used to light cure resin restorations placed in posterior teeth, they will be cured with the LCU tip at an angle, and the resin will likely be suboptimally polymerized at the bottom.21,24 To overcome this problem, as can be seen in Figures 1 and 2, many LCUs now place the LED emitter in the head of the device, and a lens is usually used to focus the light. This eliminates the need for a light guide and makes the LCU more durable.
The size of the LCU tip and its position over the resin are critical factors because they can impact the amount of energy and, in some cases, the wavelengths of light delivered to the resin from the LED emitters in the LCU. These factors may affect the photopolymerization of the resin.21,24-26 Obviously, the high power or irradiance values measured on the laboratory bench are meaningless clinically if the light tip cannot be positioned correctly over the resin (Figure 4). Therefore, when purchasing an LCU, it is important to consider that the average mouth opening is only 43 mm for men and 41 mm for women.27 Children and some adults will have much smaller openings. Therefore, before purchasing a new LCU, clinicians should always check that they can fully access the posterior restorations of the patients that they treat in their offices.3,20-26,28-32 The ease of use and the intuitiveness of its controls are also important factors to consider in order to avoid accidents, such as using it on too low or high of an output setting during a procedure. It would be very unfortunate to find out at the end of a procedure that the resin was light cured with the LCU on a low output setting.
Power Output
Values such as irradiance or intensity do not indicate how powerful an LCU is. Only the power in watts can accurately describe how powerful an LCU is. Reducing the diameter of the light tip will increase the irradiance from a low-power LCU (Figure 5). For example, reducing the diameter of a light tip from 10 mm to 7 mm will roughly halve its area (78.5 mm2 to 38.5 mm2). If the same power is delivered from two LCUs with tips of these diameters, this reduction in the tip diameter would double the irradiance, making the LCU with the smaller tip appear more "powerful." However, it is not, and because its smaller tip now covers less of the restoration, more exposures will be required.
The effect of distance on irradiance is another issue. Depending on their design, some LED LCUs deliver only 25% of the irradiance measured at the tip when the tip is held 8 mm away from the resin surface.33,34 This reduction can negatively affect how well the resin is cured.35 In contrast, by their very nature, laser LCUs demonstrate almost no reduction in the irradiance they deliver over clinically relevant distances.
To prevent patient harm as well as detrimental effects on the mechanical properties of resins due to rapid polymerization, the ISO 10650 standard36 limits how high the radiant exitance can be from LCUs.2,37-45The radiant exitance in the 380 nm to 515 nm wavelength region should be no greater than 4,000 mW/cm2. Below 380 nm, the radiant exitance should not be greater than 200 mW/cm2, and above 515 nm, it should not be greater than 100 mW/cm2. Because the chemistry of a resin is what limits its reaction rate and not the LCU used, if clinicians want to cure fast, they need to use resins that have been designed to cure fast44 (eg, Tetric® PowerFill and Tetric® PowerFlow, Ivoclar); otherwise, they should adhere to the resin manufacturer's recommendations regarding the exposure time and level of irradiance that should be used. If the resin manufacturer recommends a 10- or 20-second exposure time using 1,000 mW/cm2, do not try to light cure the resin in 1 second. Moreover, even if a dentist wanted to deliver the minimum 10 to 20 J/cm2 recommended by the resin manufacturer in 1 second, the irradiance from the light would have to be 10,000 to 20,000 mW/cm2. No LCU delivers an irradiance that high because it would cause unwanted thermal damage to the oral tissues.46
Emission Spectrum
Depending on their design, LCUs emit different wavelengths of light, which affects their capability to light cure resins. Light-curable resin materials contain photoinitiator molecules with specific bonds that only absorb certain wavelengths of light. A photoinitiator's ability to react with electromagnetic energy (ie, light) depends on the electron configuration of the molecule and the photon's wavelength. To produce translucent and bleach-white shades of restorative resins, manufacturers have incorporated co-initiators or alternative photoinitiators.2,3 However, most of these alternative photoinitiators are activated by shorter wavelengths of light, such as violet light, which has a wavelength less than 420 nm. Although the resins that contain these alternative photoinitiators could be photopolymerized using the broad emission spectrum delivered by older halogen LCUs, the first- and second-generation LED LCUs only emit light in the blue wavelength (ie, greater than 420 nm); therefore, even though they deliver more than 1,000 mW/cm2, they cannot activate the additional photoinitiators within these resins.3,5 They can only activate camphorquinone.
By incorporating more than one LED color emitter into the curing light, third-generation LCUs are able to emit both the shorter wavelength of violet light (390 nm to 430 nm) as well as blue light (440 nm to 500 nm).2,3,5,8,47 These LCUs can activate all of the photoinitiators that are currently used in dental resin systems. Third-generation LCUs are also referred to as "multi-wave" or "multi-peak" LCUs, indicating that they emit light that has more than one wavelength peak. The internal optics of broad-spectrum, multiple-peak LED LCUs must be carefully designed to produce a light output that has a high irradiance and is spectrally uniform over the entire LCU tip.3,48-50 Otherwise, one part of the tip may be emitting light that is less than 420 nm while another part is emitting light that is greater than 420 nm.
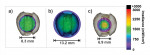
Figure 6 illustrates the range in wavelength outputs from four contemporary LCUs (SmartLite® Pro, Dentsply Sirona; Valo™ X, Ultradent; Pinkwave™ Quadwave™, Vista Apex; Monet® Laser Curing Light, AMD Lasers). Typically, the wavelength range in which the greatest light output occurs is described using the full width at half maximum. For blue LED LCUs, this value is usually between 20 nm and 24 nm (Figure 6a). Figure 6b and Figure 6c illustrate how some LCUs use multiple LED emitters to produce a broader range of wavelengths. Figure 6d illustrates the wavelength produced by a battery-operated, high irradiance diode laser LCU.51 However, because it is a laser, the full width at half maximum is only about 2 nm.
The LCU shown in Figure 6c has four distinct wavelength bands that deliver red (625 nm to 750 nm) and infrared (800 nm to 900 nm) in addition to blue and violet light. The manufacturer claims that this "quad-wave" light can reduce polymerization shrinkage stress52 by using multiple wavelengths. However, the absorbance spectra of the four most common photoinitiators used in dental resins (ie, camphorquinone, phenylbis [2,4,6-trimethylbenzoyl]-phosphine oxide [BAPO], Ivocerin, and Lucirin TPO)3,49,53 suggest that light above 500 nm will not activate these photoinitiators. Therefore, the benefit of the additional wavelengths remains uncertain.54,55 Many researchers are looking at how these different types of LCUs perform clinically.
Light Beam Profile
Because LCU light beams are not visible to the human eye, specialized equipment is required to detect the subtle differences in their uniformity. If the light beam is not uniform, it can result in uneven photopolymerization of the resin.56-60 Therefore, it is important for LCUs to provide both a uniform spectrum and irradiance across their light beams. Figure 7 illustrates the differences in the beam profiles from the aforementioned four curing lights.3-5,20,56 When the irradiance is multiplied by the exposure time used, the beam profiles show how much radiant energy is delivered. Because these energy images depict the amount of light that the resin receives during the designated exposure time as well as the area of the resin that receives it, beam profiles can provide an extra indication of the light curing effectiveness of LCUs when compared with averaged power or irradiance values. Beam profile images can also illustrate the effect of distance on the light delivered. Figure 8 demonstrates the excellent beam uniformity from one LCU (Valo X, Ultradent) at distances of 0 mm, 4 mm, and 8 mm from the light tip. This LCU still delivers about 60% of the irradiance at 8 mm from the light tip.
Figure 9 depicts the beam profiles of three LCUs (Bluephase® PowerCure, Ivoclar; Valo X, Ultradent; LED-B, Woodpecker) superimposed over an average-sized mandibular first molar tooth with a mesial-occlusal-distal preparation. This image illustrates how the first LCU, with its wide-diameter tip, completely covers the tooth with a uniform amount of light. In contrast, the third LCU, with a smaller diameter light guide, covers a much smaller area with an uneven amount of light. Although the first LCU covers less area than the second, its light distribution is very uniform. As this figure illustrates, the LCUs with smaller diameter light guides will require multiple exposures to fully cover the tooth with light. Dentists should consider this fact and assess the tip diameters of LCUs when choosing which one to buy. A larger diameter light tip is beneficial when light curing bulk-fill resins or cementing crowns, veneers, or onlays; however, a smaller diameter tip is ideal when light curing brackets, Class V restorations, or restorations in small teeth.
Battery Life
Cordless LCUs are the most popular, but when choosing between models, it is essential to compare their battery life and cost of replacement batteries. Some replacement batteries for LCUs cost more than $200. All things considered, it may be better to opt for an LCU that can be both battery powered and wired to avoid any inconvenience in case the battery drains during a procedure (eg, Bluephase G4, Ivoclar; Bluephase PowerCure, Ivoclar; Valo X, Ultradent).
Cheaper battery-operated curing lights may not offer both options. Moreover, cheaper LCUs may not compensate for the decrease in output or the effects of temperature changes on the LED, which could result in unstable light output without warning. Investing in a high-quality curing light from an established manufacturer is recommended to avoid such problems.22,61-66
Durability and Warranty
When choosing a curing light, it is worth considering its durability, including whether or not it can withstand accidental drops or impacts. Fiber-optic light guides are easily broken. In addition, a strong warranty from the seller can protect clinicians from any potential defects or malfunctions. When buying an LCU online, there's a risk of receiving counterfeit or low-quality products that may not meet safety standards for dental use. Buying from unverified retailers could lead to poor curing performance, malfunction, a fire, or even harm to the patient, with no means of support or option for repair or replacement from the seller. To avoid such issues, it is advisable to only purchase an LCU from authorized dealers who offer manufacturer warranties and customer support.
Regulatory Compliance
In the United States and Europe, dental curing lights are considered Class II medical devices and are regulated by government agencies such as the US Food and Drug Administration.67-69 When purchasing LCUs from unestablished manufacturers or unauthorized online sellers, there's no way to verify that the product has undergone proper testing and validation for safe use on patients. Some online retailers may sell LCUs that do not meet the necessary regulatory standards, putting clinicians and dental offices at risk of adverse legal or ethical consequences. One aspect of this concern involves the lithium-ion batteries that are used to power cordless LCUs. All lithium-ion batteries use flammable materials, and a chain reaction can occur that results in a fire or even a catastrophic explosion. This is another reason that dentists should only purchase certified products from reputable retailers.69
Proper Use and Maintenance
Many dentists are unaware of the importance of properly using and maintaining the LCUs in their offices.6,70-75This is critical to the success of restorative procedures. LCUs should be used and cleaned according to the manufacturer's instructions.29,31,32 To ensure proper curing, the tip of the LCU should be positioned as close as possible and perpendicular to the restoration.4,5Some research6,70,71has shown that many of the LED LCUs used in dental offices often deliver less than 300 to 500 mW/cm2, even though the manufacturers claim that these devices deliver more than 1,000 mW/cm2. The fact that so many of the LCUs used in dental offices deliver such a low irradiance and that many of the dentists will still use a 10 to 20 second exposure time for everything is concerning because this can lead to undercured restorations, reduced bond strength, and leaching of undesirable chemicals into the mouth.10-13
It is also important to note that even when the top surface of a resin restoration appears fully cured, if insufficient energy is delivered, the bottom of the restoration will be undercured. This may result in adverse effects. To avoid these issues, dentists should regularly use accurate dental radiometers (eg, Bluephase® Meter II, Ivoclar; Bluelight CheckUp, Bluelight) to measure the irradiance from their LCUs (Figure 10).76-80In addition to providing the irradiance, The Bluephase Meter II indicates how powerful the light is in mW, and the CheckUp provides information on the recommended exposure times for the specific resins that dentists use and alerts them about possible temperature concerns.
Safety Concerns
In humans, the cornea, aqueous humour, lens, and vitreous humour of the eye are not able to block blue light. There are increasing concerns that prolonged exposure to artificial blue light can disrupt sleep patterns,5,81-84 accelerate retinal aging, and cause age-related macular degeneration.85 Artificial blue light can also cause immediate and irreversible retinal burning.3,86,87 This risk is highest between 415 nm and 480 nm, with the hazard peaking at 440 nm.3,86,87 Unfortunately, this range matches the peak emission spectra from most dental LCUs. Most countries follow internationally accepted guidelines regarding safe levels of exposure to blue light in all workplaces, not just dental offices.86,88 It is important to note that the maximum recommended exposure times in the workplace are developed for individuals with normal photosensitivity; however, children as well as adults who have had cataract surgery or are taking photosensitizing medications may be more susceptible to retinal damage.86,88 LCU manufacturers recommend using protective blue light blocking orange shields and glasses to protect the eyes of patients and practitioners from the bright blue light (Figure 11).1,3,89,90 In particular, appropriate eye protection is essential when using the Class 4 diode laser LCU. This laser can cause blindness to the patient or user, and OSHA guidelines91 must be followed when using any laser in the dental office. In addition to adverse effects from blue light, high power LCUs can also generate heat, which can be uncomfortable for patients. Therefore, care should be taken to avoid direct contact between the light guide and patients' tissues.
Future Developments and Innovations
Advancements in curing light technology are continually being made, with manufacturers improving the power output, irradiance, spectrum, battery life, and durability of their LCUs. Using a diode laser as the light source appears to be a promising innovation because it is difficult to collimate the incoherent light from LEDs. Conversely, a diode laser emitter is a point source of coherent light, which makes it much easier to collimate or refocus with an optical lens. Diode lasers are also more efficient at converting electrical energy into radiant energy than LEDs. However, due to the nature of a diode laser LCU, its full width at half maximum output is less and the diameter of its light beam is much smaller (2 nm) when compared with halogen or LED curing lights. This necessitates the delivery of multiple overlapping exposures to cover a larger restoration, which negates some of the possible time savings associated with using a diode laser LCU. Finally, diode laser LCUs are currently more expensive than LED LCUs, and this has limited their widespread use in dentistry.
Conclusion
The dental LCU has become an essential instrument in modern dentistry. It should be comfortable to hold, be easy to operate, and use intuitive controls that don't require excessive effort or attention. However, just because an LCU delivers a high irradiance on the laboratory bench does not mean that it can light cure a resin in the mouth. Clinicians should confirm that the LCU can deliver sufficient energy at the correct wavelengths to the resin. In addition, they must use the LCU correctly and determine how many exposures are required to cover the restoration with light. Considering the potential risks associated with lack of quality assurance, fires, warranty support, calibration and accuracy issues, regulatory compliance, and lack of testing and verification, dentists should exercise caution when shopping for LCUs online and only purchase certified models from reputable retailers.
About the Authors
Richard Bengt Price, BDS, DDS, MS, PHD
Professor
Department of Dental Clinical Sciences
Faculty of Dentistry
Dalhousie University
Halifax, Nova Scotia, Canada
Braden Sullivan
DDS Student
Faculty of Dentistry
Dalhousie University
Halifax, Nova
Scotia, Canada
References
1. Rueggeberg FA, Giannini M, Arrais CAG, Price RBT. Light curing in dentistry and clinical implications: a literature review. Braz Oral Res. 2017;31(suppl 1):e61.
2. Watts DC. Light-curing dental resin-based composites: how it works and how you can make it work. Front Dent Med. 2023;4:1108316.
3. Price RB, Ferracane JL, Hickel R, Sullivan B. The light-curing unit: an essential piece of dental equipment. Int Dent J. 2020;70(6):407-417.
4. Price RB, Shortall AC. Essentials of light curing. Dent Update. 2018;45(5):400-406.
5. Price RB, Rueggeberg FA. Chapter 6: Light curing of restorative materials. In: Ritter AV, Boushell LW, Walter R, eds. Sturdevant's Art and Science of Operative Dentistry. 7th ed. Elsevier; 2019:170-199.
6. Ernst CP, Price RB, Callaway A, et al. Visible light curing devices - irradiance and use in 302 German dental offices. J Adhes Dent. 2018;20(1):41-55.
7. Algamaiah H, Watts DC. Chapter 5: How do I select and deploy light curing units for BFC? In: Sabbagh J, McConnell R, eds. Bulk Fill Resin Composites in Dentistry Springer Cham; 2023;51-65.
8. Jandt KD, Mills RW. A brief history of LED photopolymerization. Dent Mater. 2013;29(6):605-617.
9. Korner P, Wegehaupt FJ, Attin T. Einschätzung von Zahnärzten zu vermuteten Gründen für das Scheitern von Kompositfüllungen mittels Adhäsivtechnik [Assessment of dentists' opinions on the cause of failure of adhesive composite restorations]. Swiss Dent J. 2021;131(1):45-52.
10. Xu X, Sandras DA, Burgess JO. Shear bond strength with increasing light-guide distance from dentin. J Esthet Restor Dent. 2006;18(1):19-27; discussion 28.
11. Hass V, Dobrovolski M, Zander-Grande C, et al Correlation between degree of conversion, resin-dentin bond strength and nanoleakage of simplified etch-and-rinse adhesives. Dent Mater. 2013;29(9):921-928.
12. Fujioka-Kobayashi M, Miron RJ, Lussi A, et al. Effect of the degree of conversion of resin-based composites on cytotoxicity, cell attachment, and gene expression. Dent Mater. 2019;35(8):1173-1193.
13. Maktabi H, Ibrahim MS, Balhaddad AA, et al. Improper light curing of bulkfill composite drives surface changes and increases S. mutansbiofilm growth as a pathway for higher risk of recurrent caries around restorations. Dent J (Basel). 2021;9(8):83.
14. TetricPowerFill: Instructions for Use. Ivoclar Vivadent AG, Schaan/Liechtenstein 2021.
15. SDR+: Instructions for Use. Dentsply Sirona Charlotte, NC,USA. 2018.
16. SonicFill 3: Directions for Use. Kerr Corporation Orange, CA, USA.2018.
17. G-ænial Sculpt: Instructions for Use. GC AMERICA, Alsip, IL. USA. 2015.
18. Filtek One Bulk Fill Restorative: Instructions for Use. 3M Dental, St. Paul, MN. USA.
19. Filtek Supreme Ultra: Instructions for Use. 3M Dental, St. Paul, MN. USA. 2016.
20. Osseiran A, Price RB, Dunn K, et al. Buyer beware: the lowdown on 8 budget curing lights. Dent Econ. 2022;112(2):18-22.
21. Moreira RJ, de Deus RA, Ribeiro MTH, et al. Effect of light-curing unit design and mouth opening on the polymerization of bulk-fill resin-based composite restorations in molars. J Adhes Dent. 2021;23(2):121-131.
22. Soares CJ, Rodrigues MdP, Oliveira LRS, et al. An evaluation of the light output from 22 contemporary light curing units. Braz Dent J. 2017;28(3):362-371.
23. André CB, Nima G, Sebold M, et al. Stability of the light output, oral cavity tip Accessibility in posterior region and emission spectrum of light-curing units. Oper Dent. 2018;43(4):398-407.
24. Konerding KL, Heyder M, Kranz S, et al. Study of energy transfer by different light curing units into a Class III restoration as a function of tilt angle and distance, using a MARC Patient Simulator (PS). Dent Mater. 2016;32(5):676-686.
25. Price RB, McLeod ME, Felix CM. Quantifying light energy delivered to a Class I restoration. J Can Dent Assoc. 2010;76(2):a23.
26. Kojic DD, El-Mowafy O, Falenchuk O, et al. Radiant-exposure attenuation through Class-2 proximal slots. Am J Dent. 2021;34(2):116-119.
27. Gallagher C, Gallagher V, Whelton H, Cronin M. The normal range of mouth opening in an Irish population. J Oral Rehabil. 2004;31(2):110-116.
28. Soares CJ, Bragança GF, Pereira RADS, et al. Irradiance and radiant exposures delivered by LED light-curing units used by a left and right-handed operator. Braz Dent J. 2018;29(3):282-289.
29. Samaha S, Bhatt S, Finkelman M, et al. Effect of instruction, light curing unit, and location in the mouth on the energy delivered to simulated restorations. Am J Dent. 2017;30(6):343-349.
30. Balhaddad AA, Marghalani AA, Raderman MA, et al. Hands-on training based on quantifying radiant exposure improves how dental students cure composites: skill retention at 2-year follow-up. Eur J Dent Educ. 2021;25(3):582-591.
31. Suliman AA, Abdo AA, Elmasmari HA. Training and experience effect on light-curing efficiency by dental practitioners. J Dent Educ. 2020;84(6):652-659.
32. Price RB, Strassler HE, Price HLet al. The effectiveness of using a patient simulator to teach light-curing skills. J Am Dent Assoc. 2014;145(1):32-43.
33. Price RB, Labrie D, Whalen JM, Felix CM. Effect of distance on irradiance and beam homogeneity from 4 light-emitting diode curing units. J Can Dent Assoc. 2011;77:b9.
34. Corciolani G, Vichi A, Davidson CL, Ferrari M. The influence of tip geometry and distance on light-curing efficacy. Oper Dent. 2008;33(3):325-331.
35. Al Nahedh H, Al-Senan DF, Alayad AS. The effect of different light-curing units and tip distances on the polymerization efficiency of bulk-fill materials. Oper Dent. 2022;47(4):E197-E210.
36. International Standards Organization. ISO 10650:2018 Dentistry-powered polymerization activators. ISO website. https://www.iso.org/standard/73302.html. Published August 2018. Accessed June 29, 2023.
37. Wydra JW, Cramer NB, Stansbury JW, Bowman CN. The reciprocity law concerning light dose relationships applied to BisGMA/TEGDMA photopolymers: theoretical analysis and experimental characterization. Dent Mater. 2014;30(6):605-612.
38. Musanje L, Darvell BW. Polymerization of resin composite restorative materials: exposure reciprocity. Dent Mater. 2003;19(6):531-541.
39. Tichy A, Bradna P. Applicability of exposure reciprocity law for fast polymerization of restorative composites containing various photoinitiating systems. Oper Dent. 2021;46(4):406-418.
40. Sadeghyar A, Watts DC, Schedle A. Limited reciprocity in curing efficiency of bulk-fill resin-composites. Dent Mater. 2020;36(8):997-1008.
41. Leprince JG, Hadis M, Shortall AC, et al. Photoinitiator type and applicability of exposure reciprocity law in filled and unfilled photoactive resins. Dent Mater. 2011;27(2):157-164.
42. Selig D, Haenel T, Hausnerová B, et al. Examining exposure reciprocity in a resin based composite using high irradiance levels and real-time degree of conversion values. Dent Mater. 2015;31(5):583-593.
43. Feng L, Carvalho R, Suh BI. Insufficient cure under the condition of high irradiance and short irradiation time. Dent Mater. 2009;25(3):283-289.
44. Par M, Marovic D, Attin T, et al. Effect of rapid high-intensity light-curing on polymerization shrinkage properties of conventional and bulk-fill composites. J Dent. 2020;101:103448.
45. Besegato JF, Jussiani EI, Andrello AC, et al. Effect of light-curing protocols on the mechanical behavior of bulk-fill resin composites. J Mech Behav Biomed Mater. 2019;90:381-387.
46. Spranley TJ, Winkler M, Dagate J, et al. Curing light burns. Gen Dent. 2012;60(4):e210-214.
47. Varshney I, Jha P, Nikhil V. Effect of monowave and polywave light curing on the degree of conversion and microhardness of composites with different photoinitiators: an in vitro study. J Conserv Dent. 2022;25(6):661-665.
48. Michaud PL, Price RB, Labrie D, et al. Localised irradiance distribution found in dental light curing units. J Dent. 2014;42(2):129-139.
49. Price RB, Ferracane JL, Shortall AC. Light-curing units: a review of what we need to know. J Dent Res. 2015;94(9):1179-1186.
50. Price RB, Labrie D, Rueggeberg FA, et al. Irradiance differences in the violet (405 nm) and blue (460 nm) spectral ranges among dental light-curing units. J Esthet Restor Dent. 2010;22(6):363-377.
51. AMD Lasers. Monet Laser Curing Light. The 1 second revolution. West Jordan, UT; 2021.
52. Vista Apex. Pinkwave Instructions for Use. Inter-Med, Inc. Racine, WI; 2021.
53. Meereis CTW, Leal FB, Lima GS, et al. BAPO as an alternative photoinitiator for the radical polymerization of dental resins. Dent Mater. 2014;30(9):945-953.
54. Maucoski C, Price RB, Arrais CAG. Temperature changes and hardness of resin-based composites light-cured with laser diode or light-emitting diode curing lights. Odontology. 2023;111(2):387-400.
55. Adams KR, Savett DA, Lien W, et al. Evaluation of a novel "quad" wavelength light curing unit. J Clin Exp Dent. 2022;14(10):e815-e821.
56. Soares CJ, Braga S, Price RB. Relationship between the cost of 12 light-curing units and their radiant power, emission spectrum, radiant exitance, and beam profile. Oper Dent. 2021;46(3):283-292.
57. Price RB, Labrie D, Rueggeberg FA, et al. Correlation between the beam profile from a curing light and the microhardness of four resins. Dent Mater. 2014;30(12):1345-1357.
58. Issa Y, Watts DC, Boyd D, et al. Effect of curing light emission spectrum on the nanohardness and elastic modulus of two bulk-fill resin composites. Dent Mater. 2016;32(4):535-550.
59. Magalhaes Filho TR, Weig KM, Costa MF, et al. Effect of LED-LCU light irradiance distribution on mechanical properties of resin based materials. Mater Sci Eng C Mater Biol Appl. 2016;63:301-307.
60. Shimokawa C, Turbino ML, Giannini M, et al. Effect of curing light and exposure time on the polymerization of bulk-fill resin-based composites in molar teeth. Oper Dent. 2020;45(3):E141-E155.
61. AlShaafi MM, Harlow JE, Price HL, et al. Emission characteristics and effect of battery drain in "budget" curing lights. Oper Dent. 2016;41(4):397-408.
62. Shimokawa CA, Turbino ML, Harlow JE, et al. Light output from six battery operated dental curing lights. Mater Sci Eng C Mater Biol Appl. 2016; 69:1036-1042.
63. Al-Zain AO, Alshehri IM, Jamalellail HMH, et al. Effect of battery discharge on the output from budget light-curing units. Eur J Gen Dent. 2022;11(02):123-131.
64. Maucoski C, Balzer AH, Kudrek de Souza A. Influence of a budget single-peak light-curing unit on the microhardness and bond strength of bulk-fill resin composites to the gingival floor of proximal class II cavity preparations. International Journal of Adhesion and Adhesives. 2022;118:103239.
65.Ozkan S, Gollerli YY. Effects of declining battery voltage on light intensity and power consumption of light-curing. J Clin Orthod. 2017;51(7):411-418.
66. Prochnow FHO, Kunz PVM, Correr GM, et al. Relationship between battery level and irradiance of light-curing units and their effects on the hardness of a bulk-fill composite resin. Restor Dent Endod. 2022;47(4):e45.
67. U.S. Food and Drug Administration. Guidance for Industry and FDA Staff Dental Curing Lights - Premarket Notification [510(k)] Submissions. FDA website. Issued March 27, 2006. Accessed June 29, 2023. https://www.fda.gov/media/74206/download.
68. European Commission. MDCG 2021-24 - Guidance on classification of medical devices. Published October 4, 2021. Accessed June 29, 2023. https://health.ec.europa.eu/latest-updates/mdcg-2021-24-guidance-classification-medical-devices-2021-10-04_en
69. Price RB, Ferracane JL, Darvell BW, et al. Caveat emptor when purchasing dental products online. J Am Dent Assoc. 2022;153(3):196-199.
70. Morimoto S, Zanini RA, Meira JB, et al. Influence of physical assessment of different light-curing units on irradiance and composite microhardness top/bottom ratio. Odontology. 2016;104(3):298-304.
71. Altaie A, Hadis MA, Wilson V, et al. An evaluation of the efficacy of LED light curing units in primary and secondary dental settings in the United Kingdom. Oper Dent. 2021;46(3):271-282.
72. Kopperud SE, Rukke HV, Kopperud HM, et al. Light curing procedures - performance, knowledge level and safety awareness among dentists. J Dent. 2017;58:67-73.
73. Frazier K, Bedran-Russo AK, Lawson NC, et al. Dental light-curing units: An American Dental Association clinical evaluators panel survey. J Am Dent Assoc. 2020;151(7):544-545 e542.
74. Kojic DD, El-Mowafy O, Price R, et al. Efficacy of light-emitting diode light polymerization units used in private practices in Toronto, Ontario, Canada. J Am Dent Assoc. 2019;150(9):802-808.
75. Kojic DD, El-Mowafy O, Price R, et al. The ability of dental practitioners to light-cure simulated restorations. Oper Dent. 2021;46(2):160-172.
76. Maucoski C, Price RB, Arrais CA, et al. Power output from 12 brands of contemporary LED light-curing units measured using 2 brands of radiometers. PLoS One. 2022;17(7):e0267359.
77. Shortall AC, Hadis MA, Palin WM. On the inaccuracies of dental radiometers. PLoS One. 2021;16(1):e0245830.
78. Shimokawa CA, Harlow JE, Turbino ML, et al. Ability of four dental radiometers to measure the light output from nine curing lights. J Dent. 2016;54:48-55.
79. Imbery TA, Bergeron SY, Boyle J. Radiant exitance of old, new, and damaged LED light curing units. Oper Dent. 2022;47(6):693-700.
80. Holmes DC, Lien W, Raimondi CJ, et al. Novel chairside spectrometer-trained system for measuring the irradiance of light-curing units. Gen Dent. 2023;71(2):59-63.
81. Nagai N, Ayaki M, Yanagawa T, et al. Suppression of blue light at night ameliorates metabolic abnormalities by controlling circadian rhythms. Invest Ophthalmol Vis Sci. 2019;60(12):3786-3793.
82. Tosini G, Ferguson I, Tsubota K. Effects of blue light on the circadian system and eye physiology. Mol Vis. 2016;22:61-72.
83. Zhao ZC, Zhou Y, Tan G, et al. Research progress about the effect and prevention of blue light on eyes. Int J Ophthalmol. 2018;11(12):1999-2003.
84. Effets sur la santé humaine et sur l'environnement (faune et flore) des diodes électroluminescentes (LED): ANSES. 2019. https://www.anses.fr/en/system/files/AP2014SA0253Ra.pdf
85. Wielgus AR, Roberts JE. Retinal photodamage by endogenous and xenobiotic agents. Photochem Photobiol. 2012;88(6):1320-1345.
86. TLVS and Beis: Based on the documentation of the Threshold Limit Values for chemical substances and Physical Agents & Biological Exposure indices. Cincinnati, OH: ACGIH Publications; 2023.
87. Price RB, Labrie D, Bruzell EM, et al. The dental curing light: A potential health risk. J Occup Environ Hyg. 2016;13(8):639-646.
88. ICNIRP. Guidelines on limits of exposure to incoherent visible and infrared radiation. Health Phys. 2013;105(1):74-96.
89. Bruzell EM, Johnsen B, Aalerud TN, et al. Evaluation of eye protection filters for use with dental curing and bleaching lamps. J Occup Environ Hyg. 2007;4(6):432-439.
90. Soares CJ, Rodrigues MdP, Vilela ABF, et al. Evaluation of eye protection filters used with broad-spectrum and conventional LED curing lights. Braz Dent J. 2017;28(1):9-15.
91. Occupational Safety and Health Administration. Laser Hazards. OSHA website. Accessed June 29, 2023. https://www.osha.gov/laser-hazards/hazards.







![Figure 7 (7.) Examples of the energy delivered in 10 seconds from three LED LCUs ([a.] SmartLite Pro, Dentsply Sirona; [b.] Valo X, Ultradent; and
[c.] Pinkwave Quadwave, Vista Apex) and in 1 second from the laser LCU ([d.] Monet Laser Curing Light, AMD Lasers). Note the differences in beam uniformity, tip diameters, and the wide range of radiant exposure values delivered
in the 10-second and 1-second exposure time.](/media/thumbnail/102291/150x150)