Restoration of a Class I Malocclusion Case
Clear aligner therapy and minimally invasive veneers deliver a conservative yet highly esthetic outcome
Dimple Desai, DDS
Today's patients are often well informed about restorative dental procedures and may express concerns about treatments that require the removal of healthy tooth structure. Using the latest digital tools, materials, and techniques, it is possible for practitioners to help a significant number of patients achieve their stated goals of improving their smiles using minimally invasive treatments that do not require or require only a minimal amount of enamel contouring—even in cases involving malocclusion. Optimal esthetics can be successfully achieved with conservative techniques in cases involving underlying factors such as Class I deep bite malocclusion with proper case selection and occlusal management.
Healthy young adults who wish to improve their smiles often don't realize that the physical problems that they see in the mirror, such as chipped maxillary incisors, may be indicative of one or more underlying conditions. In order to treat a patient's cosmetic concerns, a full analysis of the relationship between form and function must be conducted and oftentimes addressed before esthetic issues can be tackled.1 Promoting and protecting the health and well-being of the patient must always be the primary consideration in any cosmetic case.
When considering treatment options for young adults, the preservation of tooth structure is of the utmost importance.2 Cosmetic treatment in the anterior region often involves the placement of porcelain veneers using conventional approaches that remove healthy tooth structure in order to achieve highly esthetic outcomes. Although conventional approaches to porcelain veneer treatment are still prescribed for the majority of the patients who receive cosmetic care, improvements in restorative materials and the development of conservative techniques allow clinicians to deliver highly esthetic outcomes using minimally invasive or no-preparation veneers in cases in which clear aligner therapy is used to correct a deep bite and straighten misaligned teeth.3,4
In the case presented in this article, the function and esthetics of a young female adult who wished to improve her smile are managed using clear aligner therapy to reposition her teeth in both arches followed by treatment with minimally invasive veneers to address her esthetic concerns.
Case Report
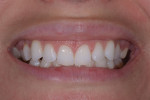
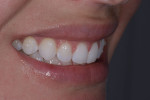
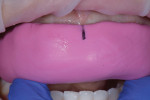
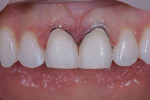
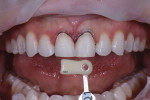
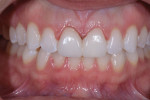
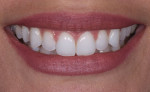
A 24-year-old female business professional who was very concerned with the esthetics of her smile was referred to the practice for consultation. Her primary concerns were the chipping of her maxillary central incisors and the crowding of her lower anterior teeth (Figure 1). Prior to her appointment, she had researched restorative treatments for chipped anterior teeth online, and when she presented, she expressed anxiety about receiving any treatment that would "grind her teeth down to pegs" as she had seen in an online video. The patient also expressed that she wanted her restored teeth to appear "natural." To put her at ease, she was assured that highly esthetic treatment options existed that didn't require the removal of significant amounts of tooth structure if her existing teeth were deemed sound.
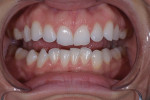
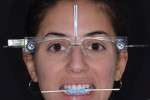
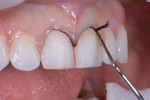
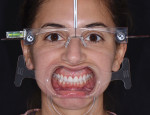
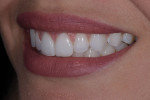
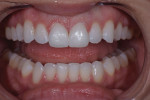
A full mouth series of radiographs was acquired, which revealed that her dentition was healthy and unrestored, and her periodontium was deemed healthy upon probing. Although an evaluation of her temporomandibular joints was deemed negative for dysfunction, the teeth in the anterior region of her mandibular arch showed moderate crowding and were misaligned (Figure 2), and her maxillary arch exhibited a deep bite in excess of 3 mm in a Class I malocclusion relationship with her mandibular arch. Her constricted chewing pattern was causing her upper anterior teeth to improperly occlude with her lower teeth, resulting in the chipping of her maxillary central incisors. Clinical photographs were acquired, which revealed high lip dynamics in the 11th percentile that resulted in the display of a slight gingival disharmony between teeth Nos. 8 and 9. In addition, it was evident that tooth No. 9 was approximately 0.1 mm narrower than tooth No. 8. The patient's canine edge position at rest was deemed reasonable for determining the incisal lengths of the restorations for teeth Nos. 8 and 9 in that position.
Evaluation and Treatment Plan
The patient's esthetic goals could only be predictably realized by first addressing her deep bite and constricted envelope of function. Opening her bite and removing any occlusal interferences would permit the restoration of teeth Nos. 8 and 9 with minimally invasive veneers.5 The treatment plan proposed to the patient involved the use of clear aligner therapy to both straighten her lower dentition and open her maxillary overbite by 1.5 mm, while maintaining an appropriate posterior occlusal relationship, followed by restoration of her central incisors with minimally invasive porcelain veneers.6 To create gingival harmony between teeth Nos. 8 and 9, gingival recontouring would also be performed.
For patients who are anxious about their esthetic concerns being addressed immediately, it is important to help them understand that treatment sequencing to address the causative factors behind their esthetic problems is vital. Doing so not only helps to achieve treatment acceptance but also helps to ensure adherence to the treatment plan. To demonstrate the need for the patient's teeth to be repositioned before addressing her esthetic concerns, intraoral scans of her upper and lower arches were acquired (iTero Element®, Align Technology) and uploaded into simulation software. The patient was visually shown how her current occlusal relationship was causing the chipping of her maxillary incisors—a condition that needed to be addressed before restoring her smile to prevent future issues. The use of software simulation (Invisalign® Outcome Simulator Pro, Align Technology) helped her to visualize how clear aligner therapy could straighten her lower anterior teeth and open her bite and also offered her a preview of what her newly restored smile could look like. Once the patient understood the value of addressing her malocclusion to ensure the longevity of the minimally invasive restorative measures that would be used to improve her smile, she accepted the treatment protocol.
Deep Bite Therapy
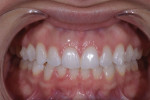
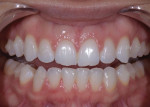
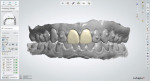
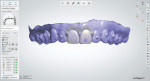
The patient's clear aligner therapy involved a 22-week protocol of upper and lower aligners that were changed each week. Using aligner software (ClinCheck® Pro, Align Technology), a series of aligners was designed that corrected the crowding and supraeruption of her lower incisors7 as well as corrected her deep bite by leveling her mandibular arch and slightly opening up her anterior bite without flattening her smile arc (Figure 3 through Figure 5). By intruding teeth Nos. 8 and 9, their gingival architecture would be more in symmetry with that of teeth Nos. 6 and 11.
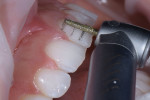
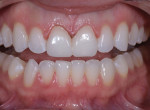
The patient was instructed to wear the aligners all day except for when she was eating or flossing and brushing. Research has found that patients who require moderate dental realignment are very receptive to this method and compliant with the strict protocol.8 When the patient returned to the practice after her last week of aligner therapy, her occlusal contacts and bite were checked and photographed (Figure 6 and Figure 7), and the relationship of her upper to lower arch was scanned and sent along with the photographs to the laboratory for the digital design of two minimally invasive veneers for teeth Nos. 8 and 9 (Figure 8 and Figure 9).
Gingival Recontouring and Temporization
Due to the young age of the patient and her desire to conserve tooth structure, the treatment plan involved only the most minimal preparation of teeth Nos. 8 and 9 in order to restore their harmony, symmetry, and length.9-12 The patient's high lip dynamics also required consideration of her gingival architecture. In this case, the gingival zenith of tooth No. 8 was not in harmony with that of tooth No. 9. When compared with tooth No. 9, the gingival height of tooth No. 8 was more incisal by approximately 0.75 mm.
Bone sounding was performed on tooth No. 8 with a periodontal probe. After confirming that the patient had a low crestal bone that measured 2 mm from line angle to line angle, it was determined that crown lengthening would be required. A No. 67 mini blade was used to align the gingival height of tooth No. 8 with that of tooth No. 9 and to correct the gingival zenith. Using a bone chisel (KB-1 Chisel, Brasseler USA), the crestal bone of tooth No. 8 was reshaped to be 3 mm from line angle to line angle. Once the reshaping was completed and gingival hemostasis was accomplished, a periodontal probe was used to confirm that the correct bone height had been achieved.
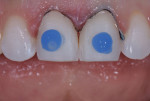
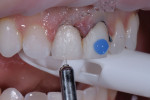
To ensure a proper emergence profile for the minimal preparation veneers on teeth Nos. 8 and 9, as well as to minimize over/under preparation, a putty matrix provided by the laboratory that replicated the diagnostic wax-up was used to create a facial reduction preparation guide. A self-curing temporary material (Telio® CS C&B, Ivoclar) was injected into the putty matrix and placed onto the unprepared teeth (Figure 10). Once set, the matrix was removed, and a depth cutting diamond (Depth Cutters, Brasseler USA) was used to make minimal preparation depth cuts into the temporary material and onto the tooth.11,12 Next, a graphite pencil was used to demarcate the depth grooves on the teeth, and the tooth surfaces were reduced equally with a diamond bur from the cervical third to the incisal third (Figure 11).
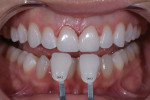
Following the minimal preparation of teeth Nos. 8 and 9, a preparation stent was used to confirm that there was adequate space for the final porcelain veneers. Two gingival retraction cords (sizes 0 and 1) were then inserted into the gingival sulcus (Figure 12 and Figure 13). After natural die shade tabs (IPS® Natural Die Material Shade Guide, Ivoclar) were used to determine the shade of the preparations, the appropriate tab (ND1) was photographed to communicate the shade to the ceramist (Figure 14), and impressions were made using vinyl polysiloxane impression materials (Virtual® XD heavy and light body, Ivoclar). Once the impressions were set, a bite registration was acquired to confirm the occlusion with the opposing arch and photographed to send to the ceramist.
To place the temporary restorations, each preparation was first spot etched (Figure 15) and thoroughly rinsed (Figure 16). A bonding agent (Adhese® Universal, Ivoclar) was then applied and air-dried for 5 seconds. After the retraction cords were removed, the self-curing temporary material was loaded into the putty matrix and placed onto the teeth. The temporary restorations were then trimmed, and the occlusion was verified (Figure 17 and Figure 18). The patient immediately approved the shade and shape of the temporary restorations. To communicate the shape and contours to the laboratory, a retracted photograph was taken of the patient with the temporary restorations in place (Figure 19). In addition, a series of photographs was taken with facial reference glasses (Kois Facial Reference Glasses, Kois Center) to help determine the correct midline, shade of the existing temporary veneers, and shade of the proposed final ceramic veneers (Figure 20 and Figure 21).
In collaboration with the ceramist, it was determined that shade OM2 (VITA Toothguide 3D-MASTER®, VITA North America) with a blend of OM3 and slight translucency would best match the shade of the patient's adjacent teeth. To provide her with the esthetics she desired, the case required a material that could be pressed to the minimal thickness while still delivering excellent strength, so the decision was made to use lithium disilicate (IPS e.max® Press, Ivoclar). Final communication with the ceramist was accomplished by uploading an intraoral scan of the temporary restorations along with a 1:2 retracted photograph and shade tab photograph (Figure 22 and Figure 23).
Final Restorations
Three weeks later, the patient returned for seating of the final restorations. After the temporary restorations were gently removed, the lithium disilicate veneers were tried in using three different cement variations and photographed for analysis. Variation one was a neutral try-in paste (Variolink® Esthetic Try-in [Neutral], Ivoclar), variation two was an extra light try-in paste (Variolink Esthetic Try-in [Light+], Ivoclar), and variation three was a 50/50 blend of the neutral and extra light try-in pastes. All three photographs were evaluated for their esthetics, and variation two was selected for final cementation.
Following try-in, the final veneers were removed, disinfected, etched with a 5% hydrofluoric acid solution for 20 seconds, rinsed, air-dried, and inspected to confirm the presence of an internal frosty appearance. Next, they were etched with a 37% solution of phosphoric acid for 60 seconds, rinsed, and air-dried again. And lastly, the veneers were silanated for 60 seconds and then given a final air-drying.
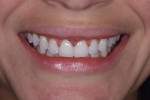
To ready teeth Nos. 8 and 9 for placement of the veneers, they were air abraded with aluminum oxide at 40 psi, thoroughly rinsed, etched with phosphoric acid for 15 seconds, rinsed again, and air-dried. A self-etching adhesive (OptiBond™ Universal, Kerr Corporation) was then applied, and after the solvent was air-dried, the adhesive was cured. Next, the dual-cure cement that was selected (Variolink® Esthetic Light+, Ivoclar) was placed onto the veneers, and they were seated onto their respective teeth and tack cured.13 Any excess cement was then removed using a curette and fine burs. After removal of the excess cement interproximally, final curing was completed. A glycerin gel (Liquid Strip, Ivoclar) was applied over the margins of the veneers, and each was cured for 20 seconds. The retraction cord was removed, the contacts and occlusion were checked and verified, and final radiographs were acquired to confirm the seat and verify that no excess cement remained. The patient expressed that she was thrilled with the final outcome (Figure 24 through Figure 26).
The patient returned one week later for final occlusal verification and portraits (Figure 27). An intraoral scan was performed and sent to the laboratory for the fabrication of final upper and lower retainers that she was instructed to wear each night to maintain tooth alignment.
Conclusion
With careful case selection and knowledge regarding proper tooth preparation, material selection, and adhesive protocols, many patients can be successfully restored with minimally invasive or no-preparation veneers. This case demonstrates that highly esthetic outcomes can be achieved even in cases where malocclusion is present and clear aligner therapy is required.14,15
About the Author
Dimple Desai, DDS
Accredited Member
American Academy of Cosmetic Dentistry
Private Practice
Newport Beach, California
References
1. Bhuvaneswaran M. Principles of smile design. J Conserv Dent. 2010;13(4):225-232.
2. Pikus-Katz E. Maximizing esthetics while preserving bone and tooth structure in a young patient utilizing digital technologies. Compend Contin Educ Dent. 2022;43(4):232-236.
3. Morita RK, Hayashida MF, Pupo YM, et al. Minimally invasive laminate veneers: clinical aspects in treatment planning and cementation procedures. Case Rep Dent. 2016;2016:1839793.
4. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 26 years of success. Dent Clin North Am. 2007;51(2):399-417.
5. Sondhi A. Anterior interferences: their impact on anterior inclination and orthodontic finishing procedures. Semin Orthod. 2003;9(3):204-215.
6. Giancotti A, Mampieri G, Greco M. Correction of deep bite in adults using the Invisalign system. J Clin Orthod. 2008;42(12):719-726.
7. Ko HC, Liu W, Hou D, et al. Recommendations for clear aligner therapy using digital or plaster study casts. Prog Orthod. 2018;19(1):22.
8. Linjawi AI, Abushal AM. Young adults' preferences and willingness to pay for invasive and non-invasive accelerated orthodontic treatment: a comparative study. Inquiry. 2020;57:46958020963595.
9. Vanlıoğlu BA, Kulak-Özkan Y. Minimally invasive veneers: current state of the art. Clin Cosmet Investig Dent. 2014;6:101-107.
10. LeSage B. Establishing a classification system and criteria for veneer preparations. Compend Contin Educ Dent. 2013;34(2):104-112, 114-115; quiz 116-117.
11. Gao J, He J, Fan L. Accuracy of reduction depths of tooth preparation for porcelain laminate veneers assisted by different tooth preparation guides: an in vitro study. J Prosthodont. 2021. doi: 10.1111/jopr.13456.
12. Sisler ZS. Preparation guides: 10 steps to maximize success for veneer preparation. J Cosmet Dent. 2020;35(4):26-33.
13. Hikita K, Van Meerbeek B, De Munck J, et al. Bonding effectiveness of adhesive luting agents to enamel and dentin. Dent Mater. 2007;23(1):71-80.
14. Smielak B, Armata O, Bojar W. A prospective comparative analysis of the survival rates of conventional vs no-prep/minimally invasive veneers over a mean period of 9 years. Clin Oral Investig. 2022;26(3):3049-3059.
15. Gurel G, Morimoto S, Calamita MA, et al. Clinical performance of porcelain laminate veneers: outcomes of the aesthetic pre-evaluative temporary (APT) technique. Int J Periodontics Restorative Dent. 2012;32(6):625-635.