Re-treatment of Failing Class V Restorations With Gingival Recession
Blendable gingival-shade composite system facilitates natural esthetics, symmetry
Paiman Lalla, DDS
Gingival recession, which is common among the adult population and affects almost all middle-aged to elderly individuals to some degree, is characterized by the apical migration of the gingival margin toward the cementoenamel junction (CEJ).1 The level or severity of recession is determined by the distance between the CEJ and the gingival margin. Among other factors, gingival recession can be caused by periodontal disease, plaque accumulation, inflammation, improper flossing, aggressive tooth brushing, malocclusion, and dominant roots.2
On the island of Trinidad, one of the unique challenges involved in treating patients with gingival recession is the ethnic variation of the population, which results in a myriad of gingival color tones.3 The population is 35.4% East Indian, 34.2% African, 15.3% mixed ethnicity (African/East Indian), 7.7% other, and 1.3% unspecified.4
Until a few years ago, recession cases had to be treated with traditional tooth-shade composite because the variation in gingival shade resulting from the population's ethnic mix made it difficult to find acceptable gum shades for many patients. Unfortunately, this caused an esthetic dilemma because it failed to maintain gingival symmetry, and some patients were unsatisfied with the results due to the disproportionate appearance of their teeth.
However, the introduction of a universal composite with a unique gingival shade system presented a solution to this problem. The universal composite used in the following case report is available in five gingival shades that can be blended and layered to produce custom shades to treat gingival recession in patients of any ethnicity.
Case Report
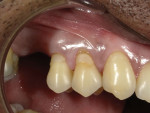
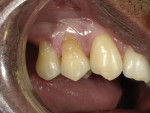
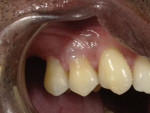
A 53-year-old male patient of Indian descent who had previously received Class V restorations on teeth Nos. 4 and 5 (Figure 1) presented to the practice complaining of mild cold sensitivity associated with tooth No. 4 and severe cold sensitivity associated with tooth No. 5. To improve the process of treatment planning and shade matching, all clinical photography for the case was performed with a digital dental camera (EyeSpecial, Shofu). A thorough examination revealed damage to the restorations in the buccogingival region of both teeth. After discussing possible treatment options, the patient chose to have the existing composite restorations replaced. The Miller Class I gingival recession exhibited by tooth No. 5 would offer the opportunity to use a blend of gingival shade universal composites to maintain the appearance of gingival symmetry.5 In addition to the obvious esthetic benefits, these gingival shade composites were selected because they contain Shofu's bioactive Giomer Technology, which has been clinically proven to facilitate long-term ion exchange for antibacterial and acid-neutralizing effects that can help to minimize problems caused by plaque and biofilm and reduce the occurrence of secondary decay.6,7
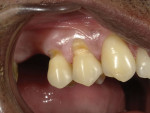
After an anesthetic was administered, coarse and fine diamond burs (Maxima®, Henry Schein) were used to remove the old composite restorations and to slightly bevel the enamel margin of the preparations (Figure 2). The enamel surfaces of the preparations were then selectively etched with a 38% phosphoric acid solution (Etch-Rite™, Pulpdent) to avoid the occurrence of sensitivity if any of the exposed dentin was also etched (Figure 3). Next, a universal bonding agent (BeautiBond®, Shofu) was applied to all surfaces of the preparations in one generous coat, left undisturbed for 10 seconds, air-dried for 3 to 5 seconds, and then light cured for 5 seconds (VALO™ curing light, Ultradent) (Figure 4). This universal bonding agent was chosen because of its unique dual adhesive monomers, which deliver equal bond strength to enamel and dentin with an extremely low film thickness of 5 µm that helps to eliminate marginal stain lines.
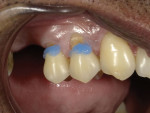
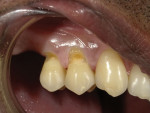
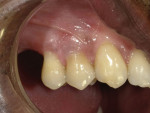
After the bonding agent was placed and cured, the first step of the restorative process was to place a flowable nanohybrid composite (Beautifil Flow Plus® X F00 [A4], Shofu) into the bonded preparations in layers no thicker than 2 mm, each of which was light cured (Figure 5). Once the tooth structure was restored, the next step was to add the gingival shade universal composite (Beautifil® II Gingiva [G-V, G-DP], Shofu) to tooth No. 5 to improve the gingival symmetry. For this case, the violet and dark pink shades were mixed in a 3:1 proportion (Figure 6). An ultra-fine diamond bur and a 16-fluted carbide bur were then used to complete the contouring and finishing. The final polishing was accomplished with a 32 fluted carbide bur and an 8-mm polishing disc system (Super-Snap®, Shofu). The shade of the gingival composite achieved in the final result closely matched the natural gingival shade of the patient (Figure 7).
About the Author
Paiman Lalla, DDS
Master
International Congress of Oral Implantologists
Private Practice
San Fernando, Trinidad and Tobago
References
1. Paryag AA, Rafeek RN, Mankee MS, Lowe J. Exploring the versatility of gingiva-colored composite. Clin Cosmet Investig Dent. 2016;8:63-69.
2. Pradeep K, Rajababu P, Satyanarayana D, Sagar V. Gingival recession: review and strategies in treatment of recession. Case Rep Dent. 2012;2012:563421.
3. Ho DK, Ghinea R, Herrera LJ, et al. Color range and color distribution of healthy human gingiva: a prospective clinical study. Sci Rep. 2015;5:18498.
4. Central Intelligence Agency. The CIA World Factbook 2021-2022. Skyhorse; 2021.
5. Miller PD Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
6. Gordan VV, Mondragon E, Watson RE, et al. A clinical evaluation of a self-etching primer and a giomer restorative material: results at eight years. J Am Dent Assoc. 2007;138(5):621-627.
7. Najma Hajira NSW, Meena N. GIOMER- the intelligent particle (new generation glass ionomer cement). Int J Dent Oral Health. 2015;2(4):http://dx.doi.org/10.16966/2378-7090.166.
MANUFACTURER INFORMATION
Shofu
shofu.com
800-827-4638