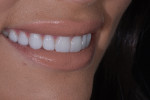
Prepless Veneers for Fractured and Worn Maxillary Teeth
Lithium disilicate provides a highly esthetic and strong long-term result
Dimple Desai, DDS
Among teenagers and young adults, social media has become one of the most common forms of communication, and it is impacting the perception of smile esthetics.1,2 Facebook, Instagram, Snapchat, TikTok, and other social media platforms provide young digital natives with meaningful tools with which they can communicate and interact with friends across geographic barriers, build online social and professional networks, and seek out entertainment or information about current events.
Taking digital photographs of oneself, or "selfies," and posting them on social media platforms for others to view is a popular practice. Focusing primarily on the face, selfies have made social media users more aware of the role that their teeth and smiles play in portraying a healthy lifestyle, significantly amplifying their consciousness of smile esthetics.3 In addition, the impact of the COVID-19 pandemic and social distancing requirements has given rise to online video meetings with friends, family, and co-workers using platforms such as Zoom. The increased frequency at which individuals are seeing their own faces has also added pressure to personal appearance awareness. As a result, young adults have become increasingly self-conscious about minor flaws in the appearance of their teeth. For issues such as tooth discoloration, gaps in the esthetic zone, and chipped, worn, or misshapen teeth, young consumers are turning to their dentists for solutions to improve the esthetics of their compromised smiles.
Many of these young patients present to the practice already educated about possible restorative solutions based on information that they gathered from Internet sources. Some also appear to be more aware of the benefits of preserving natural tooth structure.4 For dentists who work with young adults and are faced with these demands, finding the most conservative solutions to restore their smiles is important to maintaining their long-term dental health. From orthodontic treatment to tooth whitening and minimal- or no-preparation veneers, clinicians need to be prepared to consider all of the treatment options and offer those that focus on enamel preservation to achieve the best outcomes for these patients.5
Case Report
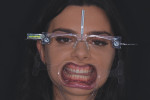
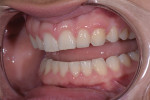
A healthy 22-year-old female patient presented to the practice unhappy with the appearance and quality of her smile (Figure 1). During the initial examination, she indicated that her maxillary central incisors had become chipped as a result of trauma that occurred during a soccer game. The remainder of her maxillary anterior teeth exhibited edge-to-edge wear from a parafunctional lateral grinding habit, which had significantly shortened her teeth and impaired the esthetics of her smile. The patient was adamant that she wanted veneers to fix her teeth and broaden her smile and that she did not want her natural teeth filed down. She also expressed a desire for very bright, white teeth.
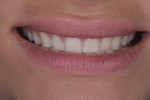
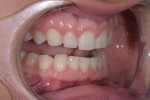
The initial in-office record-taking appointment was important in evaluating and assessing the viability of restoring her smile with no-preparation veneers. At this appointment, unretracted and retracted digital clinical photographs of the patient's teeth were acquired while the patient was fitted with facial reference glasses (Kois Facial Reference Glasses 2.0, Kois Center) and standing in front of a black poster board (Figure 2 and Figure 3). The unretracted photograph of the patient wearing the glasses aligned her horizontal and vertical planes and would aid the dental laboratory in creating a precise diagnostic wax-up prototype of the restorative solution. The retracted view was digitally imported into presentation software (Keynote, Apple Inc.) and used to measure the length and width of each tooth.
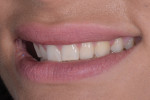
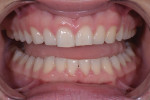
The patient exhibited a low-lip smile line with retroclined maxillary teeth, so there was adequate room to add length to teeth Nos. 4 through 13, fill the frame of her smile, and fill her upper lip and flange area (Figure 4 through Figure 6). Retracted close-up images of her smile revealed gingival symmetry that was within normal levels (Figure 7 through Figure 9). Although slight gingival contouring was suggested for tooth No. 8 to bring it into harmony with tooth No. 9, this procedure was rejected by the patient.
A main goal of the restorative treatment was to create central dominance in the patient's smile. In an analysis of the digital photographs, tooth No. 8 measured approximately 6 mm in width and 6.5 mm in length, and tooth No. 9 measured 6 mm in width and 5.5 mm in length—both well off the golden standard of 8.5 mm in width and 10 mm in length. Based on those measurements, it was determined that the lateral restorations would need to be 2-mm less in width than the centrals and that the canines would need to be 1-mm less.
Given the reality of the patient's parafunctional grinding habit, the most critical decision in achieving her stated goals was the selection of a restorative material that was not only highly esthetic but also strong. It was decided that lithium disilicate (IPS e.max® Press, Ivoclar Vivadent) no-preparation veneers with cut-backs for layering would provide the most esthetic, functional, and long-term solution. During the treatment planning, the patient was advised that wearing a nightguard would be essential to preserving the veneers.
Laboratory Communication
An intraoral scan (iTero, Align Technology) of the anterior arch was acquired and uploaded to the dental laboratory for the creation of a diagnostic wax-up of the proposed outcome. The full template of record-taking photographs and a description outlining the exact goals of the case were sent along with the intraoral scan, including instructions regarding the final shape of the teeth, which the patient wanted to be more oval than her naturally square teeth.
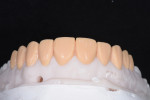
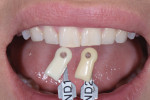
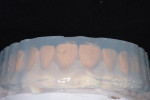
The laboratory-created diagnostic wax-up of the final case was delivered to the practice for patient approval (Figure 10). Once the patient approved the proposed treatment plan, her teeth were photographed with shade tabs (IPS Natural Die Material Shade Guide [ND1 and ND2], Ivoclar Vivadent) to provide the laboratory with the base shade of her natural teeth so that the technician could achieve the bleach shade that she desired (Figure 11).
Provisionalization
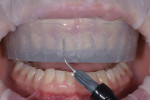
To facilitate the placement of temporary restorations using a precise composite injection molding technique, a silicone matrix was fabricated from the diagnostic wax-up (Figure 12). Every other tooth was isolated and spot-etched for 15 seconds (Total Etch, Ivoclar Vivadent), and then a self-etching bonding agent (Adhese® Universal, Ivoclar Vivadent) was applied to the etched areas to seal the enamel surface and create a bond. Next, the clear matrix was seated on the patient's maxillary arch, and a bleach shade composite (G-ænial™ Universal Flo, GC America) was injected into the matrix in the locations of the etched teeth and then light cured for 3 seconds (Bluephase® PowerCure, Ivoclar Vivadent) (Figure 13). This etching, bonding, and composite injection molding protocol was then repeated for the remaining teeth.
Once the temporary restorations were placed, they were further refined and polished (Figure 14 through Figure 16). The function, phonetics, and esthetics were then checked and verified. After the patient approved the esthetics of the provisional restorations, the occlusion was adjusted to prevent further wear. Traditional impressions of the maxillary and mandibular arches were then made to create models for the in-office fabrication of interim night guards from bleaching tray material (Essix® TRAY RITE® Plastic, Dentsply Sirona). The patient was instructed to wear the nightguards for a 2-month period to ensure the integrity of the temporary restorations until the final restorations could be seated.
Final Delivery
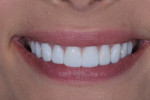
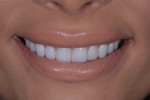
After the final restorations were received from the laboratory, each was carefully inspected for overall integrity, length, and final contours. The patient was retracted, and the provisional restorations were carefully removed, taking special care to ensure that any remnants of the composite were eliminated. Next, each tooth was individually isolated, air abraded, and acid etched for 20 seconds. Prior to seating, each veneer was etched with hydrofluoric acid for 20 seconds, rinsed, and air-dried, then etched with phosphoric acid for 60 seconds, rinsed, and air-dried, and then silanated for 60 seconds and air-dried again. The veneers were bonded to the teeth with an esthetic luting composite (Variolink® Esthetic LC, Ivoclar Vivadent) and light cured for 3 seconds. After bonding, each tooth was cleaned, and the patient's bite was confirmed both laterally and protrusively. The patient returned in 1 week so the integrity of the veneers could be checked (Figure 17 through Figure 20) and an intraoral scan could be acquired for laboratory fabrication of her final maxillary and mandibular nightguards.
Conclusion
Although not ideal for every case, no-preparation veneers can provide patients with a highly conservative and natural appearing result. Studies have demonstrated excellent long-term success rates of porcelain veneers when the preparation is confined to the enamel.6-9 With the advent of new and improved materials and techniques, these restorations can rival the results obtained by traditionally prepared veneers while meeting the demands of patients who understand the benefits of minimally invasive dentistry.10
Acknowledgement
The author would like to thank Juan Rego, CDT, FAACD, of Smile Designs by Rego for his work on this case.
About the Author
Dimple Desai, DDS
Accreditation Candidate
American Academy of Cosmetic Dentistry
Luminous Smiles
Newport Beach, California
References
1. Rana S, Kelleher M. The dangers of social media and young dental patients' body image. Dental Update. 2018;45(10):902-910.
2. Theobald AH, Wong BK, Quick AN, Thomson WM. The impact of the popular media on cosmetic dentistry. N Z Dent J. 2006;102(3):58-63.
3. McMahon S, Zwickel J. Selfie culture driving more cosmetic dentistry: a case report of conservative, responsible veneers: delivering the smile. OralHealth website. https://www.oralhealthgroup.com/features/selfie-culture-driving-more-cosmetic-dentistry-a-case-report-of-conservative-responsible-veneers-delivering-the-smile. Published April 7, 2020. Accessed December 8, 2021.
4. Wells D. "No-prep" veneers: demand and desire for more conservative preparations begins to drive this new area of esthetic dentistry. Inside Dentistry. 2010;6(8):56-60.
5. Vanlıoğlu BA, Kulak-Özkan Y. Minimally invasive veneers: current state of the art. Clin Cosmet Investig Dent. 2014;6:101-107.
6. Karagözoğlu İ, Toksavul S, Toman M. 3D quantification of clinical marginal and internal gap of porcelain laminate veneers with minimal and without tooth preparation and 2-year clinical evaluation. Quintessence Int. 2016;47(6):461-471.
7. Gurel G, Sesma N, Calamita MA, et al. Influence of enamel preservation on failure rates of porcelain laminate veneers. Int J Periodontics Restorative Dent. 2013;33(1):31-39.
8. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2):399-417.
9. Calamia JR. Etched porcelain facial veneers: A new treatment modality based on scientific and clinical evidence. NY J Dent. 1983;53(6):255-259.
10. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing Co.; 2002.