Chairside Brush-On Composite Veneers
Treating enamel imperfections with a therapeutic flowable composite
Payam Ataii, DMD, MBA
Enamel is the hardest biologic substance in the human body. Approximately 95% to 96% of its composition is made up of calcium phosphate salts in the form of hydroxyapatite, and the remainder is made up of water and organic materials that help with binding the hydroxyapatite.1,2 In addition to protecting the teeth from decay, the enamel enables them to withstand heavy masticatory forces.2
This article presents a case that involves the reaction of enamel surfaces under stress (eg, mastication forces, abfractions) and the use of a reactive treatment plan to avoid early-stage enamel penetration of caries. This treatment plan, which employs a bioactive flowable composite to deliver chairside "brush-on" veneers, can provide patients with a quick and affordable option to gain a more esthetic smile with therapeutic benefits.
Product selection is an important factor in rebuilding the demineralized enamel layer. According to in vitro and in vivo assessments, dental resin composite materials form more plaque biofilm on their surfaces when compared with other types of dental restorative materials.3 Biofilm and plaque formation occurs within the first 24 hours of restorative material placement, leading to an increase in the number of gram-positive bacteria present in the human oral environment, including Streptococcus mutans, Actinomyces naeslundii, and Lactobacillus casei, which will increase the chances of secondary decay.4 However, the use of a bioactive composite restorative material can aid in remineralizing and strengthening the tooth structure through fluoride release and promote the formation of an apatite-like layer that can potentially lead to the formation of a fluoridated apatite, resulting in improved clinical effectiveness and durability.
Case Report
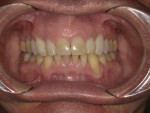
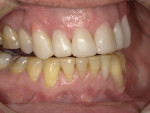
An adult male patient presented with enamel deformity in the anterior region, enamel demineralization from previous bonding, intrinsic staining, and slight anterior gingival recession-all of which were contributing to his esthetic concerns, specifically for teeth Nos. 6 through 11 (Figure 1). The patient did not want to have extensive treatment performed; however, he asked if there was a way to have his upper anterior teeth appear "more refreshed and whiter" without spending too much money or time in the chair. Various treatment options were reviewed with the patient, and the decision was made to address his concerns with a direct brush-on restorative technique using a bioactive injectable composite (Beautifil Flow Plus® X, Shofu). This material was selected because it is fast setting, provides fluoride release, and demonstrates low polymerization shrinkage and the ability to bond to enamel and dentin. Additional benefits include a reduction in microleakage, elimination of sensitivity, and the ability to immediately finish and polish the restoration.5 Restoratives with Giomer technology possess the beneficial characteristics of glass ionomers but clinically demonstrate excellent esthetics, effortless polishing, protection from surface acidity that causes enamel demineralization, restoration longevity, and ease of use for direct composite chairside procedures.6-8
Regarding the patient's gingival recession, both surgical and nonsurgical treatment options were discussed during the initial consultation. The patient chose a nonsurgical approach utilizing a bioactive resin composite in a gingival shade (Beautifil® II Gingiva, Shofu).
Gingival Restoration
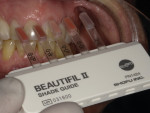
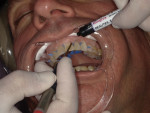
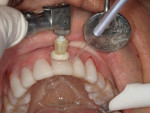
The bioactive gingiva-colored composite was placed prior to the brush-on composite veneers. First, the correct shades (G-OR and G-LP) were selected using a shade guide (Figure 2). Isolation is always best achieved using a rubber dam; however, in this case, the clear 0.002-µm thick matrix strips (Matrix Strips, Crosstex) that were used interproximally to separate teeth Nos. 6 through 11 were sufficient. After the teeth were wedged and isolated, the areas of recession were restored by sandblasting the dentogingival collars with a 27-μm aluminum oxide powder (MicroEtcher™, Zest Dental Solutions), etching them with a 35% phosphoric acid solution, applying a bonding agent (BeautiBond®, Shofu), and placing the pink composite at the gumline (Figure 3). The pink composite was light cured for 15 seconds and then lightly polished with a fine finishing stone (Dura-White®, Shofu) at the margins.
Brush-On Veneers
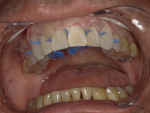
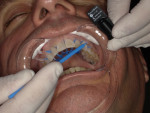
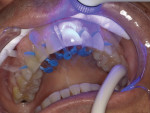
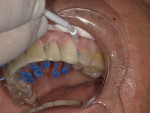
The patient was now ready for the enamel brush-on composite veneer technique. To prevent the removal of healthy enamel, no drills or burs were used. First, the facial surfaces of the maxillary anterior teeth from cuspid to cuspid (teeth Nos. 6 through 11) were prepared by gently sandblasting them with a 27-μm aluminum oxide powder, then they were etched with a 35% phosphoric acid solution for 20 seconds. (Figure 4). Next, the enamel was air-dried, and the bonding agent was placed on the facial surface of each tooth using a microbrush and scrubbed for 10 seconds (Figure 5). The facial surfaces of the teeth were each air-dried for 3 seconds and exposed to an LED curing light for 5 seconds (Figure 6), then the bioactive flowable composite (Beautifil Flow Plus® X F00 [shade A0.5], Shofu) was brushed onto each facial surface (Figure 7) and light cured for 15 seconds.
Finishing and Polishing
Final finishing was accomplished with a flame-shaped stone (Dura-White®, Shofu) at the gingival margins to remove any flash. The next step was to achieve a high polish. First, slow-speed polishing disks (Super-Snap® Polishing Disks, Shofu) were used, and then the final polish was completed with paste-impregnated disks that, when exposed to water, release a high quality polishing paste made of aluminum oxide (Super-Snap® SuperBuff Disks, Shofu) (Figure 8).
Conclusion
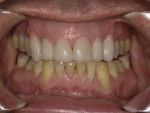
The patient expressed his satisfaction with the esthetics of the final restorations (Figure 9 and Figure 10), and the biocompatible restorative material used will help to maintain the luster and polish as he returns to his daily routine of flossing and brushing (Figure 10).
About the Author
Payam Ataii, DMD, MBA
Private Practice
Laguna Hills, California
References
1. Mann AB, Dickinson ME. Nanomechanics, chemistry and structure at the enamel surface. Monogr Oral Sci. 2006;19:105-131.
2. Higham S, Hope C, Valappil S, et al. Caries process and prevention strategies: the host. Dentalcare.com website. https://www.dentalcare.com/en-us/professional-education/ce-courses/ce370/. Revised August 27, 2021. Accessed September 3, 2021.
3. Aminoroaya A, Neisiany RE, Khorasani SN, et al. A review of dental composites: methods of characterizations. ACS Biomater Sci Eng. 2020;6(7):3713-3744.
4. Kidd EA, Joyston-Bechal S, Beighton D. Microbiological validation of assessments of caries activity during cavity preparation. Caries Res. 1993;27(5):402-408.
5. Graham L. Advances in tooth-colored restoratives. Dental Academy of Continuing Education website. https://dentalacademyofce.com/courses/2003/pdf/1012cei_glass_ionomer_web.pdf. Published December 1, 2010. Accessed September 3, 2021.
6. Gordan VV, Blaser Pk, Mjor I, et al. Clinical evaluation of a giomer restorative system: thirteen-year recall. Presented at: IADR General Session; March 23, 2013; Seattle, Washington.
7. Margolis HC, Zhang YP, Lee CY, et al. Kinetics of enamel demineralization in vitro. J Dent Res. 1999;78(7):1326-1335.
8. Gordan VV, Mondragon E, Watson RE, et al. A clinical evaluation of a self-etching primer and a giomer restorative material: results at eight years. J Am Dent Assoc. 2007;138(5):621-627.
For more information, contact:
Shofu
shofu.com
800-827-4638