Chairside Processing of Attachments for Implant-Retained Overdentures
Improving accuracy, stability, and retention
Timothy Kosinski, DDS | Stephanie Tilley, DMD
For patients who suffer from complaints related to their conventional full dentures, implant-retained overdentures are an outstanding and cost-effective means to reestablish quality of life. These appliances can be fabricated in a horseshoe shape with no significant palatal coverage; therefore, the patient's gag reflex is eliminated, and the taste buds present in the palate are exposed. Maintenance becomes rather routine because the patient is able to remove the overdenture with finger pressure, and the intraoral environment can be cleaned with soft brushes, irrigators, or a simple washcloth. Although there is much promotion of full arch, implant-retained fixed bridgework, the implant-retained overdenture offers a viable alternative in these times when many patients are facing economic difficulties.1
The strategic surgical placement of dental implants to retain maxillary overdentures is accomplished in many ways. Cone-beam computed tomography (CBCT) analysis allows practitioners to visualize precise positioning within the arch of the maxilla, and guided surgical procedures provide a means to visualize and accurately angle the implants during delivery, maximizing stability and function. The positioning of these implants is key. According to Misch,2 stability is achieved by placing the implants around the arch with as much spread as the available anatomy will allow. Implant-retained prostheses can cantilever up to one and a half times the distance between a line drawn through the most anterior implants and a line drawn through the most posterior implants (ie, A-P spread). However, implant retained overdentures are a bit distinctive in that they are supported by both implants and the soft tissue. The implant attachments are solid, but the tissue itself is resilient to varying degrees, depending on the thickness. Oftentimes, practitioners make an implant level impression of the internal design of the fixture and the residual ridge. This is then used by a laboratory technician to choose the correct abutment height and to cure the attachments into the tissue side of the prosthesis.3,4 This process may produce inaccuracies due to improper fit on the soft tissue. Excessive wear of the attachment devices during function and rocking of the overdenture may result, and subsequent breakdown of the bone surrounding the fixtures could occur, frustrating both the patient and the practitioner.5
The negative effects of wearing conventional dentures can be significant, but any method that increases chewing function is valuable to the overall health of the patient because the digestive process and nutrition are improved. As teeth are lost in the maxillary arch, the bone will shrink apically and palatally. Teeth lost in the posterior region of the maxilla can result in the enlargement of the sinuses, making implant placement challenging without grafting procedures to increase the available hard tissue. When properly placed, dental implants may help in preserving residual hard tissue over time.6 Certainly, dental implants have become a viable alternative to conventional techniques, and patients have become aware that these procedures are provided by both general dentists and dental specialists though the internet and other marketing efforts. The charge of dental professionals is to educate and instruct patients about the benefits and risks of these treatments and to provide options that work for them financially to meet their ultimate goals and desires.
Critical to successful overdenture construction is the proper positioning and angulation of the implants within the edentulous arch. When available hard tissue allows, anteriorly-posteriorly spacing the implants will help reduce rocking of the prosthesis during mastication, providing a more stable prosthesis. There are many different methods that can be employed to attach an overdenture to the integrated fixtures, including cast bars, which connect the implants and provide a solid foundation for various attachment devices (eg, o-rings; Ceka Attachments, Preci-Line; Stern ERA®, Sterngold; Hader clips).7, 8 Bar-retained overdentures are expensive to fabricate, making them cost-prohibitive for some patients. In addition, any loss of an implant under a cast bar may result in the need for re-fabrication of the bar.9 Therefore, simplicity in creation of the final prosthesis for the dentist and cost to the patient are two very important factors in the ultimate determination of the design. This article will describe the chairside curing of an implant attachment system to retain a palateless implant-retained overdenture.
Rationale and Attachment Selection
Relying on a dental laboratory technician to create the underlying retention for implant-retained overdentures sometimes results in small discrepancies that can affect patient comfort and ideal function. Because overdentures are supported by implants and soft tissue, chairside intraoral seating of the attachments can accommodate any micromovement of the soft tissue, which is difficult to do in hard model dental laboratory processing. Cold curing attachments chairside is a rather simple process and the most predictable means of ensuring stability and retention. This can be done during the initial fabrication of an appliance or in situations when laboratory processed attachments are not working well.
The attachments used in the following case (LOCATOR®, Zest Dental Solutions) can be freestanding and are easily replaced. Freestanding attachments are indicated when there is adequate vestibular and palatal depth to limit or prevent lateral displacement of the denture. Loss of an implant will not necessarily require re-fabrication of the entire prosthesis, and the vertical height of the available bone is not critical because they are low profile. The self-locking design facilitates easy seating by the patient. Retention is provided both on the inside and outside of the device, which involves a nylon component that is fitted into a metal denture cap housing. This design allows for ready changeability.10,11
Although these components are said to last for approximately 60,000 cycles of use when they are completely snapped onto the implant attachment cuff,10 any irregularities may result in improper fit, loss of retention, or the need for frequent replacement. The nylon retentive males are evaluated yearly and may need to be changed. The standard males, which offer various levels of retention (eg, clear [5 lb], pink [3 lb], blue [1.5 lb]), can be used effectively to restore an implant with up to 10° of angulation or non-parallel implants with 20° of divergence between them. In addition, there are extended range males (eg, green [4 lb], orange [2 lb], red [1 lb]) that can be used when implant angulation increases to up to 20°, accommodating 40° of divergence between implants.12
The final palateless overdenture is created using conventional denture techniques, including a preliminary impression, fabrication of a stable record base and occlusal rims, and a tooth evaluation in wax. An occlusal record is made, and the esthetics and phonetics are verified with the patient.
Case Report
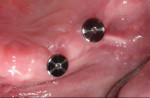
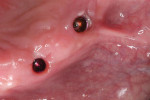
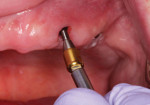
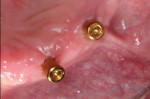
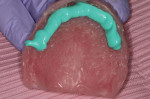
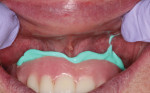
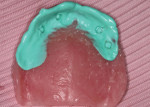
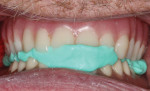
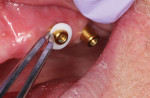
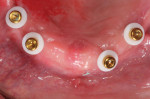
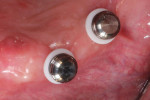
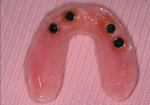
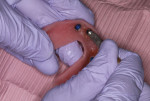
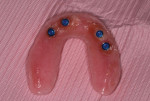
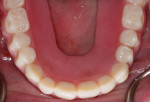
In this sample case involving a male patient, four implants (Hahn™ Tapered Implant System, Glidewell) were surgically placed into the available bone around the maxillary arch. Healing abutments were used to allow for a healthy tissue cuff to be created (Figure 1 and Figure 2). After an adequate healing period to allow for osseointegration, the healing abutments were removed, and the predetermined attachment system abutments were threaded into place and torqued to 30 Ncm using an abutment driver (Figure 3). The attachments rest approximately 1.5 mm above the crest of the soft tissue (Figure 4).
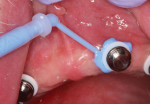
Next, a stable record base with denture teeth waxed into place was relieved, bite registration material (FUTAR® Kettenbach) was placed into the setup (Figure 5), and it was passively seated onto the attachments intraorally (Figure 6). This material serves as a guide to the abutment positions and ensures that the inside of the denture is completely relieved in the locations necessary to allow for a cold cure pickup impression of the nylon retention males. An evaluation of the material revealed that there were no interferences, and the precise position of the attachments was easy to demonstrate (Figure 7).
A bite registration was used to verify the patient's occlusion (Figure 8). This is critical to the success of curing the retentive females into the denture. Maximum intercuspation should be verified prior to curing. Block out spacers were placed over the attachments and set to the tissue level (Figure 9 and Figure 10). They help to ensure that the hard reline material will not lock onto the attachments during curing, which is one of the major concerns that dentists have when doing a chairside pickup impression. Intraoral locking of appliances can be particularly stressful.
After the black nylon laboratory males and denture caps were placed on the attachments (Figure 11), a flowable addition-curing silicone material (Quick Up Blue [Fit Test C & B], VOCO) was placed between the block out rings and the soft tissue for extra insurance that none of the hard reline material would lock onto the underside of the laboratory males when the denture caps were picked up (Figure 12). An adhesive (Quick Up Adhesive, VOCO) was placed into the relieved areas of the overdenture, and then, a flowable reline material (Quick Up Self-Curing Luting Material, VOCO) was injected until they were about two-thirds full. The overdenture was then seated onto the attachments intraorally. After a few minutes, the self-curing acrylic hardened, picking up the denture caps, and because the black laboratory males have little retention, the denture could be easily removed from the mouth. Any voids were filled with a light-cured correction material (Quick UP LC, VOCO) (Figure 13).
Using the removal tool (a simple sharp scaler may also be used), the black processing males were removed, and then, attachments with greater retention were easily inserted into the metal receptacles using the seating tool (Figure 14). The final horseshoe shaped overdenture demonstrated excellent retention and stability, providing form, function, and improved comfort for the patient (Figure 15 and Figure 16).
Conclusion
With dental implants, dentists provide an outstanding service for their patients. Although there are several approaches available to restore form and function to edentulous patients, implant-retained overdentures remain an excellent, financially achievable solution to increase quality of life for many individuals. Positive results occur by creating retention and stability and at the same time removing the palate that is present in conventional maxillary dentures; however, the dental laboratory is oftentimes relied on to process the retentive components based on an implant-level impression of the edentulous arch. Because overdentures are supported by both implants and soft tissue, processing the attachments on hard, laboratory-created models can potentially result in discrepancies and incomplete seating, which can subsequently lead to increased wear of the nylon components, rocking, and food entrapment. Chairside relining of these attachments is still the most accurate way to ensure a complete seat.
About the Author
Timothy Kosinski, DDS
Master
Academy of General Dentistry
Adjunct Associate Clinical Professor
University of Detroit Mercy
School of Dentistry
Detroit, Michigan
Private Practice
Bingham Farms, Michigan
Stephanie Tilley, DMD
Fellow
International College of Dentists
Fellow
International College of Oral Implantologists
Private Practice
Pensacola, Florida
References
1. Douglas CW, Shih A, Ostry L. Will there be a need for complete dentures in the United States in 2020? J Prosth Dent. 2002;87(1):5-8.
2. Misch CE. Contemporary Implant Dentistry. 3rd ed. St. Louis, MO: Mosby Elsevier; 2008.
3. Alsiyavi AS, Felton DA, Cooper LF. The role of abutment-attachment selection in resolving inadequate interach distance: a clinical report. J Prosthodont. 2005;14(3):184-189.
4. Trakas T, Michalakis K, Kang K, Hirayama H. Attachment systems for implant retained overdentures: a literature review. Implant Dent. 2006;15(1):24-34.
5. Ghotmi M, Hornsy L, Daou E. The locator: useful attachment for overdentures. Dental News website. https://www.dentalnews.com/2015/07/03/the-locator-useful-attachment-for-overdentures/. Published July 3, 2015. Accessed March 4, 2021.
6. Martínez-Lage-Azorin JF, Segura-Andres G, Faus-Lopes J, Agustín-Panadero R. Rehabilitation with implant supported overdentures in total edentulous patients: a review. J Clin Exp Dent. 2013;5(5):e267-e272.
7. Carvalho ER, Figueiral MH, Fonseca R, et al. In vitro study of the insertion and disinsertion effect on retention of two attachment systems of an overdenture on two implants. Revista Odonto Ciencia. 2014;29(1):1-5.
8. Alqutaibi AY, Kaddah AF. Attachments used with implant supported overdentures. International Dental & Medical Journal of Advanced Research. 2016;1(2):1-5.
9. Mahajan N, Thakkur RK. Overdenture locator attachments for atrophic mandible. Contemp Clin Dent. 2013;4(4):509-511.
10. Kosinski TF. Implant overdentures: a superior, cost-effective alternative to traditional dentures. Chairside. 2015;10(4):30-38.
11. Cha M, Kim D, Park C, Cho L. A literature review on locator attachment for implant overdentures. Journal of Dental Rehabilitation and Applied Science. 2013;29(2):127-140.
12. Miller A, Correia A, Rocha J, et al. Locator® attachment system for implant overdentures: a systematic review. Stomatologija. 2017;19(4):124-129.