The Implant Screw-Retained, Fixed-Detachable Bridge
Improving quality of life for edentulous patients
Timothy Kosinski, DDS | Stephanie Tilley, DMD
The dental profession presents clinicians with unique opportunities to use their skills to improve the dental form and function of each patient and, ultimately, his or her quality of life.
Modern dental implants, which osseointegrate into available hard tissue, can serve as a foundation for both fixed and fixed-detachable prostheses.1 There is much media attention placed on the permanent replacement of missing teeth with full arch implant-retained prostheses. This has provided education to the general public about the improved function and esthetics that can be achieved with dental implant dentistry. As a result, patients often present to practices requesting such therapy.
In the past, full arch implant-retained prostheses, commonly known as "hybrids," employed some type of cast or milled retaining bar with denture teeth and acrylic gingiva cured on top of it. This restoration, which could be screw retained, helped support the facial form.2However, over time, its design often led to acrylic fracture and wear of the denture teeth.
Certainly, losing teeth is a process that can take both an emotional and physical toll on the patient. Conventional dentures and removable partials still have a place in the profession, but to really ameliorate patients' issues, high-quality, reasonably priced, implant-retained restorations with extremely long-term prognoses have become prevalent.
Monolithic Zirconia Appliances
With today's technology, clinicians are able to restore function to a very high degree. Mastication is dramatically improved, and when a solid zirconia construction is selected, periodontal and peri-implant health is maintained because plaque and debris do not readily adhere to the material.3,4 Esthetic solid zirconia is very strong and functional. The phase transformation of zirconia under stress makes it highly resistant to fracture.5 CAD/CAM advancements using milled monolithic zirconia are replacing the more traditional acrylic-based hybrid appliances. Cone-beam computed tomography (CBCT) diagnosis and analysis provides practitioners with the ability to determine the position of vital anatomical structures and use software to virtually place implants in ideal positions. The final implant-retained prosthesis can then be digitally designed to precise specifications.6
Because the material is very resilient and resistant to fracture, a milled monolithic zirconia bridge can be designed to eliminate the palatal coverage that would occur with a traditional denture or implant-retained overdentures.7 However, in order to determine whether such a prosthesis is a possibility for a patient, it is imperative that the dentist create a treatment map. When invading vital anatomy, the risks must be clearly understood and appreciated. The mandibular nerve position and the location of the maxillary sinuses need to be delineated. Once this information is acquired, it is most efficient to design "from the teeth first." This means determining the precise position of the final replacement dentition in a way that the number of dental implants and their placement can be optimized. According to Misch, when considering a full arch fixed prosthesis, it is possible to cantilever distal pontics and crowns approximately 1.5 times the measured distance from a line drawn between the most anterior contralateral implants and the most posterior contralateral implants.8
There are several methods of retaining full arch monolithic zirconia bridges to implants. A common approach is to have the dental laboratory create custom-milled zirconia or titanium abutments that are torqued into place and used as support to cement bridgework. Another popular method is to create screw-retained implant bridges in which the abutment screws thread through the zirconia crowns to provide the retention.9 If angulation problems arise, multiunit angled abutments can be used to allow the access holes to be ideally positioned onto the cingulum or occlusal surfaces of the restoration.
The final function and esthetics of this prosthesis are specifically determined by the available hard tissue that the patient presents with. Sometimes, tooth-colored crowns with an emergence profile can be created. If there is bone loss, it may be necessary to add gingival-shaded material so that the final crowns appear normal in shape; however, the lip support is facilitated by the elongated material that extends into the implants and gingiva. Therefore, interarch measurements need to be made prior to any surgical intervention and laboratory fabrication.
Case Report
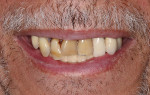
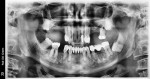
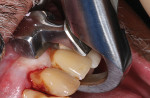
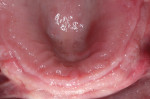
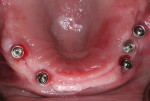
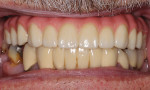
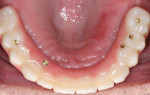
A 72-year-old male patient presented with periodontally involved nonrestorable maxillary teeth (Figure 1 and Figure 2). He had no significant contraindicated medical issues, and the only medication he was taking was for high blood pressure. Several treatment options were discussed, including a conventional maxillary complete denture, implant-retained overdentures, a fixed prosthesis, and an implant-retained bridge. The patient elected to proceed with implant treatment for a screw-retained, fixed-detachable zirconia bridge.
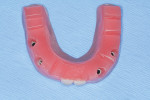
As previously mentioned, simply placing implants in locations with available bone is no longer acceptable; implant sites need to be selected that best support the final prosthesis. The final result should be considered prior to beginning this process. In this case, CBCT analysis (Green CT, VATECH America) was used to help determine the virtual implant positions.4 The process begins with making sure that the patient's existing conventional denture is properly and completely seated on the edentulous ridge. Any discrepancies can distort the surgical guide that will be created. If necessary, the dentist should reline the existing denture to achieve a more positive seat, or if the tooth position is going to change, a new transitional denture should be fabricated. The intaglio surface must be completely in contact. In this case, the patient's properly fitted denture was scanned outside of the mouth with radiographic markers (Suremark® Labels, Suremark). Then, the denture was seated intraorally with the markers still in place, and a second scan was taken. This information, along with a hard edentulous cast, was provided to the implant-planning software company. Alternatively, the dentist can personally design and plan the implant locations. Here, implant-planning software (Implant Planning Software, 3D Diagnostics) was consulted to help design the implant positions and eventually fabricate the final surgical guide. Completing a significant amount of the design of the final prosthesis early in the process helps ensure that the final monolithic zirconia bridge provides a result that the patient will accept and promote.
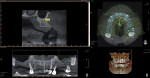
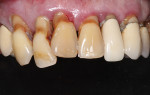
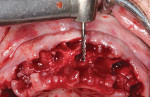
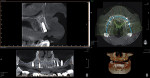
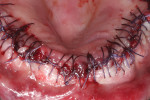
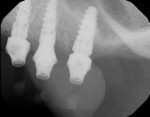
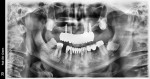
Once the implant positions were designed and the surgical guides were fabricated, the osteotomies for the implants (Hahn™ Tapered Implant System, Glidewell Laboratories) were completed through the surgical guides, and the implants were threaded into place using the implant system's guided surgical kit. The CBCT analysis was useful in the diagnosis and indicated large maxillary sinuses as well as adequate bone height and width in the premaxilla area for dental implants (Figure 3). Although the patient's remaining dentition was failing, adequate hard- and soft-tissue contours remained (Figure 4). An atraumatic extraction system (Physics® Forceps, Directa AB) was used to remove the teeth in a minimally invasive manner and maintain the facial bone (Figure 5). Following reflection of the facial and palatal tissue, a surgical bur was used to contour the sharp crestal edges and smooth down the hard-tissue surfaces (Figure 6). An interocclusal distance of at least 14 mm per arch is required to fabricate the implant screw-retained fixed prosthesis.4 The dental implants were strategically placed in the available hard tissue, and the positions were verified with a postoperative CBCT image (Figure 7). When suturing (Vilet Resorbable Sutures, Implant Direct) the tissue, a band of at least 2 mm of attached gingiva was maintained on the facial aspect of each implant (Figure 8).
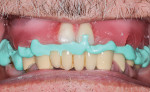
Once the implants had become integrated (Figure 9), they were uncovered in preparation for an implant level impression. Next, a clean impression was taken using vinyl polysiloxane (VPS) materials (Panasil®, Kettenbach), a stone cast was fabricated, and conventional bite relations and a wax setup were created. Denture teeth can be used to help determine the proper vertical dimension of occlusion and overall facial form (Figure 10 and Figure 11). After the patient is given an opportunity to evaluate the esthetics that were created and accept the position of the teeth, it is important to realize that any final prosthesis must be passively seated. Excessive forces cannot be placed upon the implants or abutment screws; therefore, another step was added to the process to improve the passivity of the appliance. Inlay resin jigs (DuraLay Inlay Pattern Resin, Reliance Dental Manufacturing) were created by the dental technician and independently threaded into each individual implant. After the jigs were luted together with a pattern resin (primopattern LC Gel, primotec USA) (Figure 12), a custom tray was filled with the appropriate impression materials, and a pickup impression of the screw-retained jigs was taken. This final impression needs to be very accurate because it will provide the laboratory technician with the best master cast to begin fabrication of the final prosthesis.
Once the master cast is fabricated, the dental laboratory technician will decide if multiunit abutments are needed to adjust the angulation of the retention screws through the access openings in the occlusal and palatal aspects of the prosthesis (Figure 13). If multiunit abutments are not chosen, then it may become necessary to place access holes in the facial aspect of the prosthesis, potentially creating an esthetic concern.
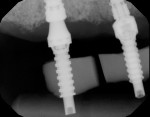
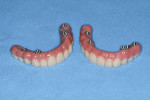
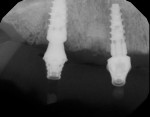
When the bite relation and final impressions were confirmed to be accurate, a polymethylmethacrylate (PMMA) appliance was fabricated (Figure 14). This transitional appliance can be easily modified for occlusal discrepancies and esthetic concerns. This modification process is continued until both form and function are appropriate. The patient may wear this PMMA try-in for 1 to 4 weeks to verify acceptance before the final prosthesis is fabricated. After any adjustments are made and the try-in appliance is finalized, it is returned to the laboratory. Using CAD/CAM, the final solid prosthesis was then milled from a zirconia puck (BruxZir®, Glidewell Laboratories). Figure 15 shows a side-by-side comparison of the PMMA try-in prosthesis and the final zirconia screw-retained prosthesis. Digital periapical radiographs of the multiunit abutments allowed the access holes to be placed on the palatal aspect of the final screw-retained prosthesis (Figure 16 and Figure 17).
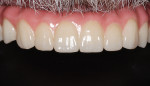
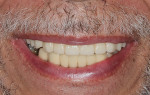
After the final prosthesis was seated and the abutment screws were torqued into place at 35 Ncm (Figure 18), the access holes were obturated with a tooth-colored composite material. The patient returned in approximately 1 week in order to check the occlusion and review proper at-home maintenance. The final postoperative panoramic radiograph indicated that the appliance was functional (Figure 19), and the patient expressed happiness with the esthetics and stability (Figure 20 and Figure 21).
Conclusion
Patients who wear conventional removable appliances are often resigned to a reduced quality of life. Esthetics can be improved with such appliances, and there is also some increased function, but for those who have their natural dentition, it can be difficult to imagine what it is like to wear "plastic teeth." Dentures simply provide the minimal amount of tooth replacement. Of course, edentulous patients may continue to lose bone height and contour over time, requiring relines or replacement throughout the years. And with resorption comes the loss of facial support, lip support, and vertical dimension of occlusion.
In order to stay or become more youthful looking, the public spends millions-if not billions-of dollars each year. Although dentures may be an initially cost-effective treatment modality, they may not serve the long-term interests of patients' physical and psychological needs. Implant-retained removable appliances are certainly an improvement from conventional removable dentures, but oftentimes, there is a request for fixed teeth. The digitally designed and custom-milled monolithic zirconia bridge documented here offers a viable and valuable step up in treatment for these patients. It dramatically improves chewing efficiency, and with the help of skilled dental laboratory technicians, provides beautiful esthetics-two components that can improve the overall quality of life of patients who wear traditional removable appliances.
About the Author
Timothy Kosinski, DDS
Master
Academy of General Dentistry
Adjunct Associate Clinical Professor
University of Detroit Mercy
School of Dentistry
Detroit, Michigan
Private Practice
Bingham Farms, Michigan
Stephanie Tilley, DMD
Private Practice
Pensacola, Florida
References
1. Jayesh RS, Dhinakarsamy V. Osseointegration. J Pharm Bioallied Sci. 2015;7(Suppl 1):S226-S229.
2. Egilmez F, Ergun G, Cekic-Nagas I, Bozkaya S. Implant-supported hybrid prosthesis: conventional treatment method for borderline cases. Eur J Dent. 2015;9(3):442-448.
3. Christensen GJ. BruxZir and e.maxCAD: superior clinical performance at 3+ years. Clinicians Report. 2014;7(6):1-3.
4. Carames J, Tovar Suinaga L, Yu YC, et al. Clinical advantages and limitations of monolithic zirconia restorations full arch implant supported reconstruction: case series. Int J Dent. 2015;2015:392396. doi: 10.1155/2015/392496.
5. Giordano R, Sabrosa CE. Zirconia: material background and clinical application. Compend Contin Educ Dent. 2010;31(9):710-715.
6. Schlesinger CD. CBCT guided surgery: accurate, predictable, and economical. Dentistry Today website. https://www.dentistrytoday.com/implants/10588-cbct-guided-surgery-accurate-predictable-and-economical. Published August 1, 2019. Accessed October 31, 2019.
7. Tischler M. A maxillary fixed bridge supported by dental implants: treatment sequence and soft-tissue considerations. Compend Contin Educ Dent. 2012;33(5):340-344.
8. Misch CE. Contemporary Implant Dentistry. 3rd ed. St. Louis, MO: Mosby Elsevier; 2008.
9. Jacobs R, Salmon B, Codari M, et al. Cone beam computed tomography in implant dentistry: recommendations for clinical use. BMC Oral Health. 2018;18(1):88.