Implant Restoration on Both Sides of the Maxillary Arch
Clark F. Brown Jr, DDS
Dentistry is always seeking to improve patient care. This occurs through education as well as with new materials, techniques, and technologies. The mouth is a difficult place not only to work in but also for materials to properly function in and withstand the stresses of the oral environment over time. The placement of dental implants and implant restorations have proven to be some of the best services that dentists can provide to patients. It is no longer necessary for a patient with missing teeth to wear removeable appliances or sacrifice additional teeth for a fixed bridge.
Although providing dental implants is an exceptional service, it requires training in both placement and restoration. New technology has been developed to improve the quality of this service. With digital integration, the dentist can begin an implant case with the final result in mind. After optical images are taken and a virtual crown is designed, the design can be imported and superimposed onto a cone-beam computed tomography (CBCT) scan, and then a surgical guide can be fabricated.1
For a case that involves implants on each side of an arch, the traditional method of restoring them would include placing impression posts, taking a vinyl polysiloxane (VPS) impression, and sending it to the laboratory. This laboratory would pour the impressions, place the abutments in the analogs, and then fabricate the crowns. Oftentimes, custom abutments are used, which allow for a better emergence profile. This laboratory process is both time-consuming and expensive.
Alternatively, a digital workflow can provide all of the advantages of custom abutments with the added advantages of speed (ie, the restoration can be completed in a single visit), improved accuracy, and lower cost.2
Intraoral scanners can produce full-arch images, but acquiring accurate ones can be challenging. An accurate bite can be easily obtained for a single quadrant, but in full-arch cases, there can be difficulty in obtaining an accurate bite registration. The most accurate way to handle a full-arch case is to open two separate incidences of the software and to do each side individually. Although this is not a difficult or particularly time-consuming task, more advanced intraoral scanners can accurately capture the full arch in a single scan.
When choosing an intraoral scanner, it is important to take into account its trueness (ie, comparison of the digitized model with the original model) and precision (ie, the repeatability of or closeness between test results).
Case Report
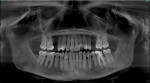
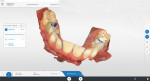
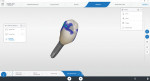
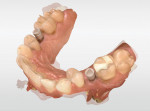
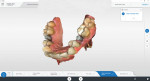
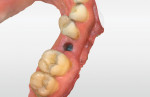
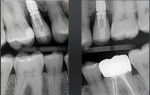
A patient who presented with teeth Nos. 4 and 13 missing desired to have dental implants to replace them (Figure 1). A CBCT scan (Galileos®, Dentsply Sirona) was taken, and it was determined that there was adequate bone volume for dental implants without the need for grafting. A pretreatment scan was taken using an intraoral scanner (CEREC Primescan, Dentsply Sirona), and the crowns were virtually designed (Figure 2 and Figure 3). These designs were then imported into imaging software (Galaxis, Dentsply Sirona). After the implants were virtually placed with the final restorations in mind, the data was exported from the imaging software and imported into the scanning software (CEREC Software 5.0.x, Dentsply Sirona) to produce two surgical guides (CEREC Guide 2, Dentsply Sirona).
The patient was taken to the treatment room, prepared, and anesthetized for the implant placement procedure. Two 3.5 x 10 implants (MegaGen AnyRidge®, ids Integrated Dental Systems) were selected for the sites of teeth Nos. 4 and 13. The surgical guides were tried in and the accuracy of their fit was established. Using a flapless surgical technique, a tissue punch was used to remove a small area of tissue at each site. The osteotomies were created using the surgical guide for all bur diameters. Next, the implants were delivered through the surgical guide, and healing abutments were placed. There was no need for sutures.
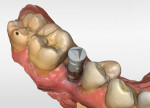
After an adequate healing period, the healing abutments were removed, and the stability of each implant was assessed using the Implant Stability Quotient (ISQ). Both implants had an ISQ of 80. Scan posts (ScanPost, Dentsply Sirona) were placed at fixture level, and full-arch images were obtained (Figure 4 through Figure 9). The complete imaging of the upper arch, lower arch, bite, and gingival mask took less than 5 minutes. The software proposed a design for the crowns, which were screw-retained restorations, and allowed for complete control over any desired changes (Should the dentist desire a cemented restoration, the software allows the proposed restoration to be split into an abutment and crown.). The entire design-to-mill time for both of the restorations was under 10 minutes. The screw-retained crowns were fabricated from abutment blocks (IPS e.max®, Ivoclar Vivadent). The titanium bases (TiBase, Dentsply Sirona) were then cemented to the abutments according to the manufacturer's instructions. The milling, crystallization, and titanium base cementation process took approximately 1 hour.
After the crowns were tried-in and it was determined that no adjustments were required, they were torqued into place at 35 Ncm according to manufacturer's instructions, and polytetrafluoroethylene (PTFE) tape and composite were used to seal the screw-access channels (Figure 10).
The entire procedure was quick, predictable, and accurate. The use of preoperative planning, virtual implant placement, guided surgery, and final screw-retained crowns made the treatment an almost effortless process.
About the Author
Clark F.
Brown Jr, DDS
Diplomate
American Board of Oral Implantology
Private Practice
Melbourne, Florida
For more information, contact:
Dentsply Sirona • dentsplysirona.com • 844-848-0137
References
1. Brown CF Jr. Galileos Cone-Beam & CEREC Integration. Version 1.3. Clark F. Brown, Jr, DDS; 2012. Accessed May 16, 2019.
2. Sannino G, Germano F, Arcuri L, et al. CEREC CAD/CAM chairside system. Oral Implantol (Rome). 2015;7(3):57-70.