Determining Appropriate Fees for Tooth Bleaching
Tips for approaching treatment and coding it in a cost-efficient manner
Van B. Haywood, DMD | Jacqueline Delash, DMD, MPH
Determining appropriate fees for tooth bleaching in a dental office should take into account several considerations, which are based upon the diagnosis of the cause of discoloration and the patient's concerns. The national average cost of tray bleaching is between $260 and $320 per arch, which includes the examination, screening radiographs, impressions, trays, and other needed materials.1 Tooth "bleaching" materials are generally different from tooth "whitening" products that are marketed as toothpaste and other over-the-counter dentifrices. "Whitening" products generally only remove the stains from the external surfaces of the teeth, whereas "bleaching" products penetrate deep within the tooth structure, changing the internal color of the tooth, which resides in the dentin.2,3 When offering tray bleaching to patients, consider the following tips to help determine the most appropriate treatment and the most cost-effective way to code for the treatment rendered.
One Arch at a Time
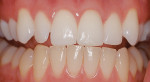
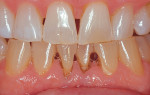
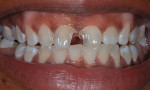
The American Dental Association's (ADA) code for external bleaching for home application is D9975, which is a "per-arch" treatment.4 Surprisingly, the results of early bleaching research indicated that almost 50% of patients who bleached their top arch chose not to bleach their bottom arch, even when it was offered at no cost and they were without previous bleaching problems. Some patients have stated that because no one sees their bottom teeth, they simply have no further interest in pursuing bleaching treatment. Therefore, approximately 50% of patients who are interested and willing to pay for top-arch bleaching find bleaching their bottom arch to be an unnecessary investment in time and money. In addition, bleaching one arch at a time can improve patient compliance because the color contrast between arches is visually evident (Figure 1). Moreover, one-arch bleaching helps with the reduction of generalized sensitivity because there are less teeth involved, and it helps to avoid occlusal issues because only a single tray is worn during the treatment. Lastly, a "one-arch" fee is all that is required if one arch is a denture that opposes a patient's natural teeth. Therefore, dental offices should offer a one-arch fee to patients as a viable treatment plan option.
Single Dark Tooth Bleaching
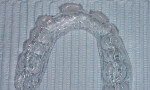
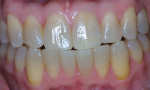
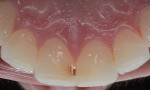
A single dark tooth that is contraindicated for root canal therapy can be bleached externally using a "single-tooth" bleaching tray.5,6 Because peroxide passes through intact enamel and dentin and gets to the pulp in 5 to 15 minutes, it is unnecessary to open the pulp chamber or perform an endodontic therapy to obtain internal access. A vital single tooth can be bleached just as easily from the "outside in" as from the "inside out." The bleaching code for a single dark tooth tray is the same as a "per-arch" full tray (ie, D9975). The difference is in the tray fabrication, which only allows the bleaching material to contact the single dark tooth without changing the shade of the adjacent teeth (Figure 2). This allows the opportunity for the single dark tooth to either match the color of the adjacent teeth or become lighter than the adjacent unbleached teeth. In the latter case, an additional full tray is fabricated on the same cast, and the adjacent teeth are bleached to match the new shade.
Depending on the approach to treatment, a single, dark endodontically-treated tooth presents several options for the fees and codes. A single dark tooth that has received endodontic therapy can be bleached from the inside using the "walking bleach" technique.7 In this technique, the inside of the pulp chamber is cleaned of pulp debris, the gutta-percha is removed to 2 mm below the cementoenamel junction, and a barrier (ie glass ionomer) is placed over the gutta-percha. Next, a bleaching medicament (ie hydrogen peroxide, sodium perborate, carbamide peroxide) is placed into the pulp chamber and the endodontic access is temporarily sealed. The "internal" bleaching material must be changed weekly, from one to six times, depending on the desired tooth color. The ADA code for "internal bleaching per tooth" is D9974. However, this process can lead to multiple dental visits and become time-consuming for both the patient and the provider. Because the process of internal bleaching can take from one to six visits, the amount of "meet, greet, and seat" time for the patient, as well as the treatment and cleanup time, can make it difficult to predict an appropriate fee for the process.
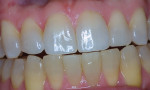
To ameliorate this concern, one approach is to combine both "internal" and "external" bleaching treatment. This time-efficient approach involves accessing the tooth internally to clean the pulp chamber, place the barrier, and add the bleaching medicament, as is done in the walking bleach technique (Figure 3); however, after this initial access, the bleaching process is continued from the outside in using a "single-tooth" bleaching tray. Although the addition of "external" bleaching requires an alginate impression, cast, and tray, the time saved by allowing the patient to continue the treatment for as long as is needed at home without scheduling weekly chairtime to access the tooth and change the material offsets the cost. This allows the practice to be more time- and cost-efficient and allows the patient to spend less time traveling and visiting the office.
The challenge with the dual "inside and outside" bleaching approach is choosing the best procedure code and the most appropriate fee. The dentist should consider selecting "single-tooth internal bleaching" (ie, D9974) for the code and fee because this treatment requires the most chairtime, and then include the cost of making the single-tooth external bleaching tray as a part of that fee without using a separate code. This approach is more time-efficient and profitable for the office than performing internal bleaching only. After the single-tooth bleaching is completed, which may take 8 to 10 weeks, wait 2 weeks for the shade to stabilize and then restore the access opening with a composite in a matching shade. If the single tooth does not fully bleach to match the adjacent teeth, then a lighter-shade composite should be used. Sometimes, a stark white, opaque composite material is placed into the most apical third of the access, followed by a matching shade composite in the anatomical area to close the orifice. This composite restoration requires a different code (ie, D2330) and an additional fee.
In the case of a single dark tooth that was previously endodontically treated but is adequately sealed with a composite, there is no need to reenter the pulp chamber in order to bleach if the cleanliness of the pulp chamber can be verified via a radiograph. The normal, "per-arch" bleaching tray code (ie, D9975) and fee should be applied regardless of whether a single-tooth bleaching tray or full-arch bleaching tray is used to bleach the tooth.
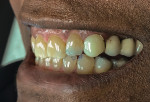
Significant Extrinsic and Intrinsic Staining
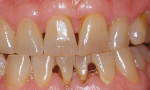
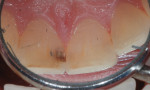
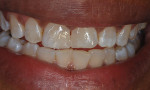
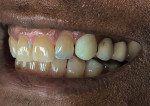
The extended treatment of nicotine- and tetracycline-stained teeth requires an approach involving a modified fee. Nicotine-stained teeth (Figure 4) require 1 to 3 months of nightly treatment with 10% carbamide peroxide to remove the soaked-in nicotine stains (Figure 5). Tetracycline-stained teeth can require 2 to 12 months of nightly treatment (ie, 3 to 4 months on average) for the bleaching material to enter the dentin and remove most of the tetracycline staining (Figure 6 and Figure 7). Due to these unpredictable treatment times, the determination of a fair fee for both the dental office and the patient is best achieved by creating a "pay-as-you-go" process. The patient pays the normal single-arch bleaching fee using code D9975 and is provided with roughly enough material to bleach one arch for 1 month. During this time, the patient uses a form to record their nights of treatment to determine exactly how long the initially dispensed syringes will last, which in turn, determines how often the patient will require a refill. The fee for the extended treatment becomes the cost of the materials used per month plus any chairtime needed until the desired shade is reached. The dental office can charge accordingly for the purchase of subsequent bleaching refill kits. Because the treatment time can vary greatly based on each patient's situation, this method of calculating payment is fair to both the patient and to the dental office. It also allows flexibility for the patient to bleach to the point when the shade stabilizes without further change or to the point when he or she is pleased with the result, tires of the procedure, or no longer wishes to spend further finances on bleaching.
Existing Decay Considerations
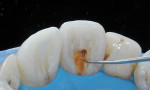
When considering bleaching in cases involving existing decay, the treatment may require two different codes and fees. The final shade achieved and the rate of shade change from bleaching is different for every patient. If the patient is interested in bleaching and presents with existing decay that requires a restoration, the dentist cannot reliably predict the final shade of the restoration prior to bleaching. Fortunately, bleaching with 10% carbamide peroxide stops the progression of decay while the bleaching treatment is in process.8,9 With most small carious lesions, the dentist can bleach over the existing decay (Figure 8 and Figure 9), wait 2 weeks for the shade to stabilize and the bond strengths to return to normal, then restore the lesion with the appropriate shade of composite.
However, if the decay is deep or the tooth is sensitive, the caries needs to be removed prior to bleaching to avoid further pulpal insult (Figure 10). In these cases, the dentist can first place a "protective restoration" (ie, code D2940) with a resin-modified glass ionomer (RMGI), selecting the best possible projection of the final shade (Figure 11). With this protective restoration placed, the patient can then bleach his or her teeth while also minimizing the concern of a pulpal insult or further progression of caries if he or she unexpectedly stops bleaching. If the esthetics of the RMGI need improvement during the bleaching process, a thin layer of resin infiltrate (eg, Optiguard™ Surface Sealant, Kerr™) can be added to the surface of the restoration to create a glossy and natural appearance (Figure 12 and Figure 13). Upon completion of the bleaching treatment, if the shade of the RMGI matches reasonably well, and the patient is satisfied with the appearance, then no further treatment is needed. However, if the final bleaching shade does not match the previously placed RMGI, or the surface gloss is insufficient, then the dentist need only remove the external portion of the RMGI and bond an appropriate shade of composite, leaving the remaining RMGI as a base. Although this additional treatment provides the best esthetics and the safest option for deep decay or sensitive lesions, it requires a separate fee and code for the final resin-based composite restoration (ie, D2332).
Thermoplastic Trays
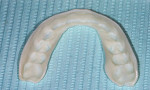
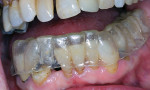
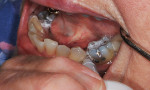
For the maxillary arch, the use of thermoplastic trays10 can facilitate a reduced fee for patients who require only minimal lightening or who have difficulty with the process of making impressions (Figure 14). Teenagers and young adults often have reasonably white teeth but may still have a desire to maximize their tooth shade.11 As opposed to pursuing over-the-counter products,12 it is best for the dentist to provide a proper examination and radiographs to determine a diagnosis for any discoloration.13 Fabrication of a thermoplastic tray can be accomplished in a few minutes and bypasses the need for alginate impressions, casts, and a vacuum former. Although the standard single-arch bleaching code is still used, the associated fee can be reasonably reduced because this approach requires less chairtime, no laboratory work, and no impression material. This can provide an excellent way to help some patients achieve their desired level of esthetics without needing to charge the full fee for the traditional bleaching impression/cast. This approach works best on the maxillary arch due to the tongue's position when swallowing to form the tray. This normal swallowing benefit is not present when attempting a mandibular thermoplastic tray, so the mandibular arch will usually require a traditional impression and tray with a different fee. Just as with traditional, single-arch bleaching, completing one arch at a time is inherently less expensive and can provide the patient with visible results to later determine whether or not bleaching the mandibular arch is desired.
Orthodontic Considerations
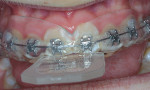
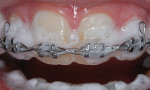
The occurrence of white spot lesions and caries from improper oral hygiene during orthodontic treatment can be significantly reduced by utilizing bleaching materials.14 Although this approach requires adding an additional fee to that of the orthodontic treatment, the benefits of bleaching while the patient is in an orthodontic appliance can greatly reduce the need for and cost of restorative treatment after the completion of orthodontic therapy. This preventive approach is highly effective because in addition to bleaching the teeth, the bleaching material helps to cleanse the teeth and gingiva from bacteria and plaque during orthodontic treatment. Considering the ease of use, cost-effectiveness, and minimal chairtime required, thermoplastic material is ideal for making bleaching trays that fit over orthodontic brackets intraorally (Figure 15). These trays help to fend off white spot lesions and decalcification by elevating the intraoral pH, removing plaque, and killing some of the bacteria that cause tooth decay. As the teeth continue to shift during orthodontic treatment, new trays will need to be fabricated approximately every 2 to 3 months, which can add about $400 to $800 to the total treatment costs over a 2-year treatment period. The attraction of this approach is twofold. First, the young patients undergoing orthodontic therapy are motivated to wear the tray because they are bleaching their teeth, and second, the parents are receiving value in their investment via improved hygiene and a reduction in white spot lesions or caries, which subsequently reduces the potential need for costly future restorations that could range from $175 to $250 per tooth. Furthermore, the thermoplastic trays can be made directly over the orthodontic brackets in the mouth and can also serve as a "sports guard" to minimize bracket damage to the lips and cheeks. The only segment of orthodontics for which this treatment does not apply is when the patient is in cross-elastics. For these patients, injecting 10% carbamide peroxide directly onto the brackets will afford some hygienic benefits, as will using a water pick with a 1:1 ratio of water and 3% hydrogen peroxide (Figure 16). In addition, an over-the-counter, 10% carbamide peroxide oral antiseptic supplementary product (eg, Gly-Oxide®Liquid Antiseptic Oral Cleanser, GlaxoSmithKline) can be injected directly onto the teeth and tongue for a 2- to 3-minute cleaning rinse. This product is also used to disinfect and deodorize bleaching trays and many other appliances (eg, occlusal guards, oral sleep appliances). Moreover, the manufacturer recommends placing it on toothbrushes prior to the toothpaste as an adjunct to improve overall oral hygiene. Although Gly-Oxide was the original bleaching material, it is too runny for tray bleaching and does not stay on teeth for long periods; therefore, thicker, more viscous materials are indicated for tray use to achieve longer lasting benefits.
Caries Control
One adjunct to routine caries control is the use of carbamide peroxide with custom trays. This approach can be especially helpful in elderly patients with dry mouth (Figure 17) or who experience reduced salivary flow from radiation therapy. Treatment to control caries with bleaching products should not be given bleaching codes. The appropriate code to use for the tray would be for a "fluoride gel carrier," which is D5986, and the appropriate code to use for the material is for "drugs or medicaments dispensed in the office for home use," which is D9630. Bleaching products containing urea, such as carbamide peroxide, elevate the pH of the mouth, which stops or slows the process of tooth decay. This change in pH occurs within 5 minutes of tray insertion,15,16 and the pH remains elevated while the trays are in the mouth. In addition, carbamide peroxide has been shown to kill the bacteria that cause caries.17 Accordingly, the bleaching process effectively removes the salivary film and plaque layer from the teeth, leading to environmental control and a reduction in caries. The challenge associated with this approach to caries control is the ongoing cost of the 10% carbamide peroxide. It can be supplied from the dental office in the same manner as it is for the extended treatment approach. Lastly, the patient can pursue over-the-counter 10% carbamide peroxide products for supplemental caries control (Figure 18).
Conclusion
In summary, there are many unique situations related to tooth bleaching that require different approaches to treatment, and these various approaches necessitate the determination of appropriate treatment codes and related fees. Bleaching is best performed by the dental office after a proper examination, radiographs, and a diagnosis of the cause of discoloration.18 The ability to tailor the treatment to the specific needs and conditions of the patient is a major benefit of having the dental team supervising ongoing bleaching treatment.
About the Authors
Van B. Haywood, DMD
Professor
Department of Restorative Sciences
Augusta University
Dental College of Georgia
Augusta, Georgia
Jacqueline Delash, DMD, MPH
Instructor
Department of Restorative Sciences
Augusta University
Dental College of Georgia
Augusta, Georgia
References
1. American Dental Association. 2018 Survey of Dental Fees. ADA Center for Professional Success Page. https://success.ada.org/en/practice-management/finances/survey-of-dental-fees. Accessed January 3, 2019.
2. Haywood V. Tooth whitening is not always tooth bleaching. Inside Dentistry. 2018;14(2):80.
3. Haywood VB, Sword RJ. Bleaching tetracycline stained teeth: considerations and recommendations for treatment. Inside Dentistry. 2018;14(1):38-44.
4. American Dental Association. CDT-2017 Code on Dental Procedures and Nomenclature. Delta Dental Website. https://www.deltadentalco.com/uploadedFiles/ProviderFeeSchedules/DDCO_Par_Provider_Documents/CDT%202017_Code%20on%20Dental%20Proc_Nomenclature%20online.pdf. Accessed January 3, 2019.
5. Haywood VB. Bleaching a retained primary tooth. Dentistry Today. 2018;37(8):74-77.
6. Haywood VB, DiAngelis AJ. Bleaching the single dark tooth. Inside Dentistry. 2010;6(8):42-52.
7. Freccia WF, Peters DD, Lorton L, et al. An in vitro comparison of nonvital bleaching techniques in the discolored tooth. J Endod. 1982;8(2):70-77.
8. Haywood VB. Bleaching and caries control in elderly patients. Aesthetic Dentistry Today. 2007;1(4):42-44.
9. Lazarchik DA, Haywood VB. Use of tray-applied 10 percent carbamide peroxide gels for improving oral health in patients with special-care needs. J Am Dent Assoc. 2010;141(6):639-646.
10. Haywood VB, Caughman WF, Frazier KB, et al. Fabrication of immediate thermoplastic whitening trays. Contemporary Esthetics and Restorative Practice. 2001;5(9):84-86.
11. Greenwall-Cohen J, Greenwall L, Haywood V, et al. Tooth whitening for the under-18-year-old patient. Br Dent J. 2018;225(1):19-26.
12. Haywood VB, Boyleston E. Does "activated charcoal" effectively whiten teeth? Dimensions of Dental Hygiene. 2017;15(12):66.
13. Haywood VB. A pre-bleaching exam is vital for optimum whitening. Inside Dentistry. 2012;8(9):66-68.
14. Haywood VB. Orthodontic caries control and bleaching. Inside Dentistry. 2010;6(4):36-50.
15. Leonard RH Jr, Austin SM, Haywood VB, et al. Change in pH of plaque and 10% carbamide peroxide solution during nightguard vital bleaching treatment. Quintessence Int. 1994;25(12):819-823.
16. Leonard RH Jr, Bentley CD, Haywood VB. Salivary pH changes during 10% carbamide peroxide bleaching. Quintessence Int. 1994;25(8):547-550.
17. Bentley CD, Leonard RH, Crawford JJ. Effect of whitening agents containing carbamide peroxide on cariogenic bacteria. J Esthet Dent. 2000;12(1):33-37.
18. Haywood VB, Bergeron BE. Bleaching and the diagnosis of internal resorption. Decisions in Dentistry. 2018;4(8):20, 22-25.