Fixed Prosthodontics with a Digital Workflow
Enhanced communication between the clinician and ceramist improves efficiency, outcomes
Druthil Belur, BDS, DMD, MS, CDT | Bobby Williams, CDT
Digital dentistry has revo-lutionized the way that we approach restoration. Its inception dates back 30 years to the introduction of the CEREC® 1 System1 and digital radiography.2 Digital dentistry encompasses a wide array of options involving hardware and software in almost every area of the profession.3-9 In the area of restorative dentistry, new workflows are constantly being developed.10-14 Today, almost all dentistry-related journals publish articles that discuss technology.
A comprehensive examination of a patient has always involved the teeth, gingiva, alveolar process, soft tissues, jaws, muscles, temporomandibular joint, and face.15-19 Although dentists visualize symmetry, proportions, contours, and shape during routine examinations, digital smile design has streamlined this process.20 It enables a more efficient dentogingival and facial analysis, improving the ability to plan and execute.21,22
Additive23 and subtractive24 technologies have significantly impacted dental laboratories. There are hundreds of manufacturers that are constantly developing products for use in dentistry. The accuracy of printed models and working casts has improved significantly over the past few years.25,26 It has been shown that crowns fabricated using CAD/CAM have a better fit when compared with those manufactured by conventional methods.27,28 High-translucency yttria-stabilized tetragonal zirconia is a common material used for fixed dental prostheses and crowns that has gained acceptance in recent years.29,30
In the following clinical case, which utilizes a number of digital workflows, the partnership between the prosthodontist and the ceramist was key to the success of the final result. Their interdependency and communication at various stages improved procedural efficiency as well as the outcome for the patient.
Case Report
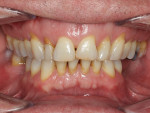
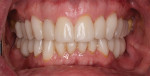
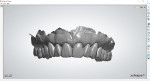
A 62-year-old, male patient presented for dental treatment with a chief complaint regarding the esthetics of his smile. Specifically, his concern involved the undesirable shade and contour of his teeth. He was also concerned about his missing posterior mandibular teeth and the generalized recession of his gums. A clinical examination revealed attrition, generalized recession, partial edentulism, a lack of anterior guidance, and uneven anterior and posterior occlusal planes (Figure 1). A parafunctional habit was also suspected. After a detailed medical and dental history were established, intraoral and extraoral examinations were conducted, and the following were obtained for treatment planning: preliminary maxillary and mandibular impressions, centric relation records, facebow records, a full mouth series of radiographs, a panoramic radiograph, cone-beam computed tomography (CBCT) scans (i-CAT™ FLX, i-CAT) of the mandible, and intra- and extraoral photographs. Diagnostic casts were mounted using an adjustable articulator (SAM® 3 Articulator, Great Lakes Dental Technologies) and analyzed (Figure 2).
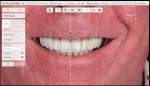
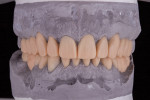
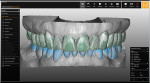
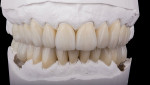
During the patient's first visit, he expressed the need to visualize the proposed plan prior to beginning treatment. Using CAD software (3Shape Dental System, 3Shape), an extraoral smile photograph (Figure 3) and an intraoral retracted photograph (Figure 1) were incorporated to create a 2-dimensional digital smile design (Figure 4). Using the face as a guide, the amount of desired incisal visibility was determined, including better proportions as well as improved anterior and posterior occlusal planes. This design was used in a series of slide presentations with the patient to facilitate a detailed esthetic analysis and discussion. After it was determined that the design met the patient's objectives, the next step was to proceed with a full mouth diagnostic wax-up. Using the 2D digital smile design as a guide, a manual wax-up of both arches was performed (Figure 5). Good communication and a thorough understanding of the objectives enabled both the clinician and ceramist to design the required contours, proportions, shape, excursive guidance, and occlusion.
Following the establishment of a comprehensive diagnosis and treatment plan, the patient's next visit involved the creation of a chairside mock-up. From the diagnostic wax-up, a putty matrix (Aquasil, Dentsply Sirona) was fabricated. Next, a chairside, bis-acrylic provisional material (Integrity® Multi-Cure Temporary Crown and Bridge Material, Dentsply Sirona) was used to produce the mock-up. After it was shown to the patient, he consented to the proposed plan, and treatment was divided into surgical and restorative phases.
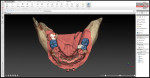
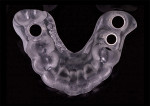
During the surgical phase, four implants were virtually planned for the mandible using treatment planning software (NobelClinician, Nobel Biocare). The diagnostic wax-up of the maxillary arch was scanned with a laboratory scanner (D900 Dental Scanner, 3Shape), and an STL (stereolithography) file was generated. This STL file and the previously obtained CBCT scan were then imported into the treatment planning software and the missing teeth were virtually planned (Figure 6). Because the diagnostic wax-up was used, the size, position, and orientation of the proposed implants were prosthetically driven. Subsequently, a restricted surgical guide (NobelClinician, Nobel Biocare) was designed and fabricated (Figure 7), which facilitated the placement of the four mandibular implants in a single visit.
After confirmation of osseointegration 3 months later, a vinyl polysiloxane (VPS) (Aquasil, Dentsply Sirona) impression using closed tray impression copings (NobelReplace® Conical Connection, Nobel Biocare) was obtained, and a cast with a soft-tissue moulage was fabricated. Indirect, screw-retained provisional restorations were then fabricated in the laboratory and delivered.
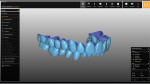
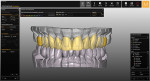
For the restorative phase, the manual diagnostic wax-up was first scanned by the laboratory using a scanner (S600 ARTI Scanner, Zirkonzahn) with a SAM Articulator interface plate/jig (Figure 8). Then, all of the teeth in the manual wax-up were converted into individual 3-dimensional digital versions (Figure 9). In preparation for the first appointment, modeling software (Zirkonzahn.Modellier, Zirkonzahn) was used to digitally design temporary shell crowns for both arches, and they were milled (M4 Wet Heavy Metal Milling Unit, Zirkonzahn) from a poly(methyl methacrylate) puck (Figure 10).
After the maxillary and mandibular teeth were prepared, the milled temporary crown shells were sandblasted, coated with a bonding agent (Prime&Bond®, Dentsply Sirona), relined with the bis-acrylic provisional material, and delivered. The patient was kept in the provisional restorations for about 8 to 10 weeks (Figure 11). This time frame allowed the dentist to refine the occlusion and establish a functional pattern that was harmonious with the envelope of function. Phonetics, esthetics, and incisal visibility with the lip at rest were also evaluated during this period.
Having established a stable occlusion and confirmed the esthetics with the patient, final impressions were taken with custom trays and the VPS material. Facebow records, centric relation records, and extra- and intraoral photographs were sent to the laboratory along with the impressions of the provisional restorations. This not only allowed the dentist to communicate the desired esthetics to the ceramist but also allowed the working models from the final impressions to be cross-mounted. In addition, a detailed prescription was sent to the laboratory with the case.
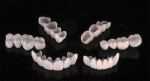
Regarding material selection, high-translucency zirconia crowns with facial cutbacks and feldspathic porcelain layering were chosen for all of the anterior teeth and premolars. For the molars, a monolithic zirconia design with external staining was chosen. The restorations were milled from a zirconia puck (Prettau® Anterior® Zirconia, Zirkonzahn), and the facial layering with feldspathic porcelain was achieved with a natural fine-structure feldspar veneering ceramic (VITA VM®9, VITA North America). Although the provisional implant crowns were screw retained, the final restorations were designed to be cement retained to custom-milled titanium abutments with titanium nitride coatings (Atlantis™ Abutments, Dentsply Sirona).
To prepare the working casts, the impressions were poured with dental stone. Using the models from the provisional restorations, the facebow records, and the interocclusal records for cross-mounting, the final working casts were mounted on the articulator. After the working casts were ditched and the die pins for each tooth placed, the casts were scanned again using the laboratory scanner. Scans were performed both with and without interocclusal records utilizing the SAM Articulator interface jig/plate. The STL files generated from the scanner were then imported into the modeling software for the final restorations to be designed (Figure 12).
Once milled, the crowns were painted with B1 shading liquid (Colour Liquid Prettau® Anterior® Aquarell, Zirkonzahn). Blue and violet incisal shading liquids were subsequently applied to create a polychromatic look (Figure 13). The restorations were then sintered in a programmable oven (VITA ZYRCOMAT® 6000 MS, VITA North America) per the manufacturer's instructions. After sintering, the crowns were placed on the ditched dies to verify their fit and form.
To adjust the color of the restorations, they were layered with chroma stains (VITA AKZENT Plus® CHROMA STAINS, VITA North America), and a fast glaze cycle was performed at 895 °C in a furnace (VITA VACUMAT® 6000, VITA North America). Next, a thin layer of highly fluorescent porcelain (VITA VM9 EFFECT LINER, VITA North America) was applied to the facial cutback and fired at 945 °C. This facilitates a stronger bond between the veneering porcelain and the zirconia substructure. After this firing cycle was completed, the first buildup of porcelain was initiated using a base dentin shade (VITA VM9 [1M2], VITA North America) around the gingival third. Next, a 1M1 base dentin shade was layered in the middle third, followed by a 0M3 base dentin shade on the line angles and a 1M2 base dentin shade in the middle incisal third. These same steps were then repeated with a thinner layer of a TRANSPA dentin shade (VITA VM9 TRANSPA DENTINE, VITA North America) to full contour. The restorations were then minimally cut back for incisal characterization. A blue/gray modifier (VITA VM9 EFFECT ENAMEL [EE9], VITA North America) was placed on the incisal edges of the restorations, and a blue modifier (VITA VM9 EFFECT ENAMEL [EE10], VITA North America) was placed on the distal and mesial aspects of the incisal edges. To create depth and contrast, a small amount of mamelon material (VITA VM 9 MAMELON [MM1], VITA North America) was placed over the more chromatic middle incisal half. Finally, a mixture comprising two-thirds enamel material (VITA VM9 ENAMEL [ENL], VITA North America) and one-third blue/gray modifier was layered in a thin veneer over the facial two-third aspects of the restorations. Once the buildups were complete, they were fired at 910 °C with a 30-second hold time.
The second (and final) buildup was accomplished using a cervical enamel shade (VITA VM9 EFFECT ENAMEL [EE5], VITA North America) at the gingival third, a white opal shade (VITA VM9 EFFECT OPAL [EO2], VITA North America) at the height of contour and line angles, and a neutral, translucent shade (VITA VM9 EFFECT ENAMEL [EE2], VITA North America) in the middle third. Finally, the white opal shade was applied on the incisal edge, and the restorations were fired again at 910 °C with a 30-second hold time.
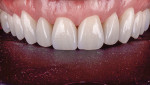
Following the final buildup, the restorations were then glazed and fired at a lower temperature of 895 °C to preserve the anatomy and create an eggshell satin finish that mimicked the patient's natural dentition (Figure 14). A diamond polishing paste was used for the final finishing. After the seating, contours, occlusion, and esthetics were verified, the case was sent back to the clinician's office where the same factors were evaluated.
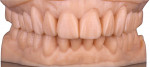
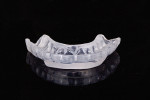
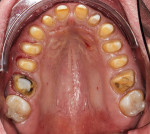
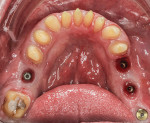
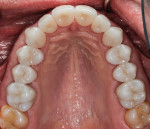
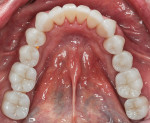
During the delivery appointment, the provisional restorations were removed and the abutments were polished using a fine grit pumice. The final restorations were seated and individually checked for marginal adaptation. Radiographs were taken to verify the seating. The provisional, screw-retained implant crowns were also removed (Figure 15 and Figure 16), and the custom titanium healing abutments were delivered. After copies of the abutments for the implant crowns were made (Figure 17), all of the restorations were tried in together, and the interproximal contacts, occlusal contacts, phonetics, esthetics, centric occlusion, and anterior guidance were verified. Once patient approval was obtained, the implant crowns were luted with temporary resin cement (Retrieve™, Parkell), and the rest of the restorations were luted with resin cement (RelyX™ Unicem Self-Adhesive Universal Resin Cement, 3M). After the excess cement was removed, the occlusion was verified and detailed postoperative instructions were given. Both intra- and extraoral photographs of the completed case were taken, and optical impressions were obtained for the fabrication of an occlusal guard (Figure 18). Intraoral scanning was performed (TRIOS®3 Wireless Cart, 3Shape) on both arches, and conventional interocclusal records were obtained in an open-mouth position. Using the optical scan data, models were created (Figure 19) with a 3D printer (Form 2 3D Printer, FormLabs), and all of the records were sent to the laboratory for fabrication of a digital splint (Figure 20). The prepared and seated lower and upper arches can be seen in Figure 21 through Figure 24.
Conclusion
Excellent communication between the clinician and ceramist is key to clinical success. The process of additive and subtractive manufacturing in dentistry has gained a lot of traction. With improved accuracy, affordability, and established workflows, digital dentistry has significantly improved efficiency and consistency in both the clinical and laboratory environments. However, fundamental concepts in fixed prosthodontics are also critical to success. The value of facebow, occlusal, and centric relation records have been well-documented throughout the years.19,31-33 New algorithms to incorporate these records are constantly being developed in software modules. A thorough understanding of conventional prosthodontic concepts enables a symbiotic workflow incorporating traditional and digital dentistry.
Disclosure
Mr. Williams lectures for VITA North America. He did not receive an honorarium for this contribution to Inside Dentistry.
About the Authors
Druthil Belur, BDS, DMD, MS, CDT
Prosthodontist
San Francisco, California
Owner
Dental Lavelle
Bengaluru, India
Bobby Williams, CDT
Owner
Synergy Ceramics Dental Studio
Plano, Texas
References
1. Mörmann WH, Brandestini M, Lutz F. The Cerec system: computer-assisted preparation of direct ceramic inlays in 1 setting. Quintessenz. 1987;38(3):457-470.
2. Mattoon JS, Smith C. Breakthroughs in radiography: computed radiography. Compend Contin Educ for the Practicing Veternarian. 2004;26(1):58-66.
3. Zaruba M, Mehl A. Chairside systems: a current review. Int J of Comput Dent. 2017;20(2):123-149.
4. Grünheid T, Patel N, De Felippe NL, et al. Accuracy, reproducibility, and time efficiency of dental measurements using different technologies. Am J Orthod Dentofacial Orthop. 2014;145(2):157-164.
5. Nasef AA, El-Beialy AR, Mostafa YA. Virtual techniques for designing and fabricating a retainer. Am J Orthod Dentofacial Orthop. 2014;146(3):394-398.
6. Setzer FC, Hinckley N, Kohli MR, et al. A survey of cone-beam computed tomographic use among endodontic practitioners in the United States. J Endod. 2017;43(5):699-704.
7. Strbac GD, Schnappauf A, Giannis K, et al. Guided modern endodontic surgery: a novel approach for guided osteotomy and root resection. J Endod. 2017;43(3):496-501.
8. Song IS, Lee MR, Ryu JJ, et al. Reconstruction of a severely atrophied alveolar ridge by computer-aided gingival simulation and 3D-printed surgical guide: a case report. Int J Oral Maxillofac Implants. 2018;33(3):e73-e76.
9. Gallucci GO, Khoynezhad S, Yansane AI, et al. Influence of the posterior mandible ridge morphology on virtual implant planning. Int J Oral Maxillofac Implants. 2017;32(4):801-806.
10. Yilmaz B, Azak AN, Alp G, et al. Use of CAD-CAM technology for the fabrication of complete dentures: an alternative technique. J Prosthet Dent. 2017;118(2):140-143.
11. Papadiochou S, Pissiotis AL. Marginal adaptation and CAD-CAM technology: a systematic review of restorative material and fabrication techniques. J Prosthet Dent. 2018;119(4):545-551.
12. Alshhrani WM, Al Amri MD. Customized CAD-CAM healing abutment for delayed loaded implants. J Prosthet Dent. 2016;116(2):176-179.
13. Rutkūnas V, Gečiauskaitė A, Jegelevičius D, et al. Accuracy of digital implant impressions with intraoral scanners. A systematic review. Eur J Oral Implantol. 2017;10(Suppl 1):101-120.
14. Venezia P, Torsello F, D'Amato S, et al. Digital cross-mounting: a new opportunity in prosthetic dentistry. Quintessence Int. 2017;48(9):701-709.
15. Spear FM. Interdisciplinary management of worn anterior teeth. Facially generated treatment planning. Dent Today. 2016;35(5):104-107.
16. Spear FM. Too much tooth, not enough tooth: making decisions about anterior tooth position. J Am Dent Assoc. 2010;141(1):93-96.
17. Ramos V. Facial analysis and treatment planning esthetics. In: Sadan A. Quintessence of Dental Technology 2004. Berlin, Germany. Quintessence Publishing Company; 2004;(27):19-29.
18. Mack MR. Perspective of facial esthetics in dental treatment planning. J Prosthet Dent. 1996;75(2):169-176.
19. Dawson P. Functional Occlusion: From TMJ to Smile Design. 1st ed. St Louis, MO: Mosby; 2007.
20. Coachman C, Calamita M. Digital smile design: a tool for treatment planning and communication in esthetic dentistry. Quintessence Dental Technology. 2012;103-111.
21. Coachman C, Calamita MA, Sesma N. Dynamic documentation of the smile and the 2D/3D digital smile design process. Int J Periodontics Restorative Dent. 2017;37(2):183-193.
22. Tak On T, Kois JC. Digital smile design meets the dento-facial analyzer: optimizing esthetics while preserving tooth structure. Compend Contin Educ Dent. 2016;37(1):46-50.
23. Revilla-León M, Sánchez-Rubio JL, Besné-Torre A, et al. A report on a diagnostic digital workflow for esthetic dental rehabilitation using additive manufacturing technologies. Int J Esthet Dent. 2018;13(2):184-196.
24. Miyazaki T, Hotta Y, Kunii J, et al. A review of dental CAD/CAM: current status and future perspectives from 20 years of experience. Dent Mater J. 2009;28(1):44-56.
25. Barazanchi A, Li KC, Al-Amleh B, et al. Additive technology: update on current materials and applications in dentistry. J Prosthodont. 2017;26(2):156-163.
26. Alharbi N, Wismeijer D, Osman RB. Additive manufacturing techniques in prosthodontics: where do we currently stand? A critical review. Int J Prosthodont. 2017;30(5):474-484.
27. Ng J, Ruse D, Wyatt C. A comparison of the marginal fit of crowns fabricated with digital and conventional methods. J Prosthet Dent. 2014;112(3):555-560.
28. Al-Rabab‘ah MA, Macfarlane TV, McCord JF. Vertical marginal and internal adaptation of all ceramic copings made by CAD/CAM technology. Eur J Prosthodont Restor Dent. 2008;16(3):109-115.
29. Harada K, Raigrodski AJ, Chung KH, et al. A comparative evaluation of the translucency of zirconias and lithium disilicate for monolithic restorations. J Prosthet Dent. 2016;116(2):257-263.
30. Chun EP, Anami LC, Bonfante EA, et al. Micro-structural analysis and reliability of monolithic zirconia after simulated adjustment protocols. Dent Mater. 2017;33(8):934-943.
31. Nagy WW, Goldstein GR. Facebow use in clinical prosthodontic practice. J Prosthodont. 2018. doi: 10.1111/jopr.12944.
32. Nagy WW, Smithy TJ, Wirth CG. Accuracy of a predetermined transverse horizontal mandibular axis point. J Prosthet Dent. 2002;87(4):387-394.
33. Wood GN. Centric relation and the treatment position in rehabilitating occlusions: a physiologic approach. Part II: the treatment position. J Prosthet Dent. 1988;60(1):15-18.