Addressing Sleep-Related Breathing Disorders
Dentistry’s role in a multidisciplinary treatment network
Steven R. Acker, DDS, MS | Nancy Hartrick, DDS
Maintaining health and wellness is an important goal for many people. With an increased understanding of the relationship between oral and systemic health, it has become apparent that the dental profession plays a significant role in this area. A primary responsibility of dental practitioners is to educate patients about treatment in a manner that enables them to make the best choices to improve their quality of life. Relationships between oral and systemic health are multifactorial. Sleep-related breathing disorders (SRBDs) are conditions that are highly influenced by these relationships. SRBD is an inclusive term associated with snoring, breathing-related sleep disorders, upper airway resistance syndrome,1 and obstructive sleep apnea (OSA).2 Although all of these are linked to disruptions in normal breathing patterns, some may lead to chronic illness, and others may affect physical growth as well as cognitive and behavioral development.
Increased Focus on SRBDs
There has been much discussion in the public domain about OSA. During the past few years, it has been given more attention by the mainstream media following the loss of actress Carrie Fisher and former Associate Justice of the Supreme Court Antonin Scalia, whose deaths were both linked to complications related to OSA. The fatal rail accidents in the New York area that occurred on the Metro North in 2013 and in the Hoboken Terminal in 2016 also drew public attention. The engineers of the trains involved in both of these accidents suffered from OSA, and excessive daytime sleepiness is one of the common comorbid medical conditions associated with the diagnosis. Attention deficit hyperactivity disorder (ADHD), allergies, and crowded teeth are among the many modern-day afflictions interfering with the healthy development of children. When left untreated, SRBDs can be closely related to these conditions.3
The Role of Dentistry
Dentists are in a unique position to help people of all ages who have been impacted by this far too common disorder, participating in both the identification and care of affected patients. In October 2017, the American Dental Association (ADA), published their proposed policy statement on the role of dentistry in the treatment of SRBDs.4 The statement established dentistry's critical position in this multidisciplinary field, including outlining the dentist's responsibilities regarding treatment and staying current with related continuing education. From proper clinical screening and the provision of age-appropriate questionnaires for risk assessment and treatment recommendations to the alleviation of symptoms and the management of care, dentists are a key part of the patient healthcare team. In younger, growing patients, dentists have even more opportunity to relieve and even reverse the damage from SRBDs by working with habit correction and aiding in the development of normal airways.
Airway Patency
SRBDs are related to the collapsibility of the upper airway, which can result in decreased air flow. Various intrinsic and extrinsic factors can affect the collapsibility of the airway, including muscle tone, reflex responses, tissue inflammation, and even sleep position. Mechanosensory receptors in the upper airway respond to changes in airway pressure, airflow, temperature, and upper airway muscle tone. When they sense a disruption in airflow or a reduction in breathing accompanied by a decrease in oxygen levels and an increase in carbon dioxide levels, they send a signal to the brain (ie, cerebellum), triggering the sympathetic nervous system to create a protective arousal that disturbs the normal cycles of sleep.5 This protective arousal returns the patient to normal breathing, but it is a compensatory measure, not the sign of a healthy airway.
When airway issues are chronic, the receptors in the cerebellum become exhausted over time, resulting in a reduced response or no response to the reduction in airflow-a situation with potentially dire consequences. When the sympathetic nervous system is triggered, the arousal is accompanied by an increase in cortisol levels via the hypothalamic-pituitary-adrenal axis. Cortisol release increases stress on the heart and other systems, which can also increase levels of inflammation in the body. Chronic heightened cortisol levels increase the risk of heart attack and stroke as well as a host of other comorbid conditions, including cardiac arrhythmias, hypertension, nocturnal bruxism, ADHD, anxiety and depression, and erectile dysfunction.
Screening and Data Collection
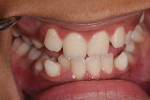
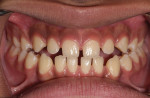
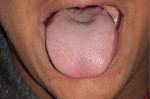
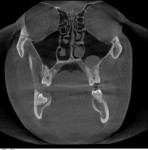
The airway health of patients needs to be maintained while they are both asleep and awake. To achieve this, diagnosis and treatment must be focused on structure (ie, the size of the airway) (Figure 1), function (ie, the stability of the airway) (Figure 2 and Figure 3), and behavior (ie, the mode of breathing). Identifying compromises and developing a mode of action requires a system for screening, data collection, risk assessment, and diagnosis. Screening can be accomplished through the use of pediatric and adult questionnaires in combination with specific clinical evaluations to help identify patients at risk who require further data collection.6
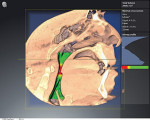
For patients identified as at-risk, data collection with more extensive clinical examination and measurements, including photography, videos, and objective tools, can be utilized. Devices such as cone-beam computed tomography (CBCT) scanners (Figure 4 and Figure 5) and high-resolution pulse oximeters (HRPO) are helpful data collection tools to aid in screening for patients with compromised airways. Once these patients have been identified, the dentist may refer them to a physician for an official diagnosis and, depending on their age and condition, further treatment.
Dentists are in a position to take the lead in an active network of healthcare professionals to help treat and manage this large and growing public health concern. Dental health professionals are at the forefront because they are uniquely trained to assess the oral, perioral, and facial structures as well as to recognize and treat airway issues before the onset of OSA occurs.
Considerations for Treatment
Although a diagnosis of sleep apnea must be made by a physician, dentists and their teams can be trained to manage many of the related structural, functional, and behavioral issues. Following risk assessment and diagnosis, treatment options can be discussed and employed. Some may require the help and teamwork of other healthcare professionals, but others can be initiated within the dental office. Basically, the earlier the intervention, the higher the chances for successful resolution and the lower the chances for serious, life-altering compensations.
As specified in the proposed ADA policy statement, among older patients diagnosed with OSA, oral appliance therapy is appropriate treatment for mild and moderate cases as well as for severe cases when continuous positive airway pressure therapy is not well-tolerated by the patient.4 For younger patients with OSA, there are often more treatment options. Functional appliances can be used in combination with myofunctional therapy to guide the growth of the maxilla and mandible, creating healthy and properly functioning airways.7 Many of these therapies have the potential to prevent or even reverse some of the growth and developmental and/or behavioral and learning challenges that are more often seen among children today. There is considerable literature supporting the idea that many of the cases and symptoms of ADHD in children are associated with breathing and airway issues. Treatment to ensure the proper development and function of the airway can often eliminate the symptoms of ADHD.8 Children must be able to breathe nasally, seal their lips at rest, and maintain proper tongue position and function.
Nasal breathing stimulates the production of nitric oxide. This chemical is produced in the paranasal sinuses and only during nasal breathing. It is a stimulant to the parasympathetic nervous system, which is essential for proper function of both the cardiovascular and central nervous systems. In addition to being a potent vasodilator, it also has antimicrobial properties. Constant mouth breathing causes inflammation to the tonsils, adenoids, and other oral tissues due to a lack of nasal filtration. The nose is the filter for the air during breathing because it helps eliminate the passage of viruses, bacteria, fungi, and environmental irritants into the airway.
From infancy, the proper rest position of the tongue is on the palate. This position leads to proper facial development. The tongue constantly applies light forces on the palate, allowing for the formation of a wide and properly contoured maxilla. The maxilla is the scaffold for the facial structures and affects the width of the nasal passages. Proper development of these structures is integral to airway formation. The mandible has a higher probability of developing normally if the maxillary anatomy develops normally. In clinical screening for airway and breathing disorders, the presence of a high palatal vault from tongue positioning is a red flag potentially indicating abnormal airway development. This can result when the tongue rests too low in the mouth, which may be due to a tongue-tie (ie, ankyloglossia) or compensation. Among children, additional red flags include open mouth posture, dry mouth, chapped lips, nasal congestion, and snoring. Early intervention is critical and may save a child from developing into an unhealthy adult with OSA and other potential comorbidities. Long before reaching the level of airway collapse associated with the development of OSA, a patient goes through a period in which the airway becomes too small, partially collapses, or has turbulent airflow, making breathing and the proper exchange of oxygen and carbon dioxide difficult.
Screening adults and children for airway and breathing disorders should be a primary focus of dental professionals as well as properly treating pediatric patients so they can experience normal breathing and airway development. Dentists have the responsibility to screen for airway and breathing disorders as well as to collect data, assess risk, refer for diagnosis, provide treatment, and develop a means to assess results. After treatment, subjective follow-up assessments (ie, how the patient feels) and objective measurements (eg, HRPO or sleep test) should be used to determine the efficacy of treatment.
A Multidisciplinary Network
Multidisciplinary care from a network of health professionals who possess a full understanding of airway development and breathing is necessary to help minimize the potential of diseases and conditions that can result from improper breathing. Approximately 158 million adults aged 25 years and older suffer from sleep apnea, and more than 10 million US men and women with the disorder currently go untreated.9
There are many health professionals who are qualified to form this network and help our community of patients with breathing and airway issues, including the following:
• Restorative dentists
• Pediatric dentists
• Orthodontists
• Oral Surgeons
• Ear, nose, and throat specialists
• Myofunctional therapists
• Respiratory physiologists
• Pediatricians
• Sleep physicians
• Primary care physicians
• Craniosacral therapists
• Chiropractors
• Lactation consultants
• Neurologists
• Pulmonologists
• Cardiologists
The goal of dental practices and this network at large is to establish an algorithm for the diagnosis, management, and desired resolution of breathing and airway issues for patients. This is a multidisciplinary approach that involves individualized care. In many cases, the restorative or pediatric dentist is in the unique position of being the first healthcare professional to see and evaluate patients for breathing and airway-related issues.
In 2019, the message for the dental profession is that the focus on airway and breathing disorders needs to go far beyond the treatment of OSA. This is a health concern with vast ramifications that are just now becoming well understood. Airway and breathing disorders are a life-changing issue for many patients, and the dental profession has the ability to intervene and improve the health and wellness of our communities and our country.
About the Authors
Steven R. Acker, DDS, MS
Private Practice
Staten Island, New York
Clinical Instructor
Advisory Board Member
Kois Center
Seattle, Washington
Nancy Hartrick, DDS
Private Practice
Royal Oak, Michigan
Clinical Instructor
Advisory Board Member
Kois Center
Seattle, Washington
References
1. Guilleminault C, Stoohs R, Clerk A, et al. A cause of excessive daytime sleepiness. The upper airway resistance syndrome. 1993;104(3):781-787.
2. Park JG, Ramar K, Olson EJ. Updates on definition, consequences, and management of obstructive sleep apnea. Mayo Clin Proc. 2011;86(6):549-555.
3. Courtney R. The importance of correct breathing for raising healthy good looking children. JATMS. 2013;19(1): 20-27.
4. American Dental Association. Proposed Policy Statement on the Role of Dentistry in the Treatment of Sleep-Related Breathing Disorders. ADA Website. https://www.ada.org/~/media/ADA/Member%20Center/FIles/Role_of_Dentistry_in_the_Treatment_of_Sleep_1-5.pdf?la=en. Accessed September 20, 2018.
5. Chandra S, Sica AL, Wang J, et al. Respiratory effort-related arousals contribute to sympathetic modulation of heart rate variability. Sleep Breath. 2013;17(4):1193-1200.
6. Chervin RD, Hedger K, Dillon JE, et al. Pediatric sleep questionnaire (PSQ): validity and reliability of scales for sleep-disordered breathing, snoring, sleepiness, and behavioral problems. Sleep Med. 2000;1(1):21-32.
7. Jefferson Y. Mouth breathing: adverse effects on facial growth, health, academics, and behavior. Gen Dent. 2010;58(1):18-25
8. Murphy K. Attention Problems May Be Sleep Related. New York Times Website. https://well.blogs.nytimes.com/2012/04/16/attention-problems-may-be-sleep-related/. Published April 16, 2012. Accessed September 20, 2018.
9. Garcha P, Aboussouan L, Minai, O. Sleep-Disordered Breathing. Cleveland Clinic Website. https://teachmemedicine.org/cleveland-clinic-sleep-disordered-breathing/. Published January 1, 2013. Accessed November 8, 2018.